What Makes Yale Medicines Approach To Treating Congestive Heart Failure Unique
We have a very patient-focused team at Yale Medicine, says Dr. Jacoby. Every person seen here, we treat as an individual, rather than offering a simple cookie-cutter treatment plan.
Yale Medicines multidisciplinary team comprises of heart failure cardiologists and cardiac surgeons, dedicated advanced-practice, registered nurses and nurse coordinators, dietitians, exercise physiologists, financial counselors, immunologists specializing in transplants, psychologists, and specialists in palliative care.
In our multidisciplinary approach, we include the patients desires as well as input from the family, Dr. Jacoby says. We develop a plan for social work support and take into account all of their financial and emotional stresses in addition to their physical treatment needs.
Unspecified Systolic Heart Failure
- 2016201720182019202020212022Billable/Specific Code
- I50.20 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
- The 2022 edition of ICD-10-CM I50.20 became effective on October 1, 2021.
- This is the American ICD-10-CM version of I50.20 other international versions of ICD-10 I50.20 may differ.
- Applicable To annotations, or
You May Like: Can Flonase Cause Heart Palpitations
What Causes Congestive Heart Failure
Several factors can cause congestive heart failure. They include:
- Presence of other diseases like diabetes and high blood pressure
- Addictions like smoking and alcohol
Although heart failure is a serious condition, it does not mean that the heart stops functioning altogether. With proper management, persons who have congestive heart failure can lead nearly normal lives, depending on its severity. Besides the required medical and surgical interventions, it is important to eat healthy, stay active as possible, and refrain from alcohol, smoking, and drug abuse. According to the U.S. Centers for Disease Control and Prevention , almost half of the patients with congestive heart failure live beyond five years.
Don’t Miss: How Accurate Is Apple Watch 6 Heart Rate
What You Can Do
Some risk factors of heart failure, like age, cant be modified. Still, people with CHF can take steps to improve the long-term prognosis. The first thing to do is to be familiar with any family history of heart disease. You’ll also want to learn about all the possible symptoms. Don’t ignore any symptom that you think is cause for concern. Tell your healthcare provider about them right away.
Regular exercise, along with managing any other health issues you may have, can also help to keep CHF under control.
What Causes Heart Failure
Heart failure is caused by many conditions that damage the heart muscle, including:
- Coronary artery disease.Coronary artery disease , a disease of the arteries that supply blood and oxygen to the heart, causes decreased blood flow to the heart muscle. If the arteries become blocked or severely narrowed, the heart becomes starved for oxygen and nutrients.
- Heart attack. A heart attack happens when a coronary artery becomes suddenly blocked, stopping the flow of blood to the heart muscle. A heart attack damages the heart muscle, resulting in a scarred area that doesnât work the way it should.
- Cardiomyopathy. Damage to the heart muscle from causes other than artery or blood flow problems, such as from infections or alcohol or drug abuse.
- Conditions that overwork the heart. Conditions including high blood pressure, valve disease, thyroid disease, kidney disease, diabetes, or heart defects present at birth can all cause heart failure. In addition, heart failure can happen when several diseases or conditions are present at once.
Don’t Miss: Coronary Insufficiency Symptoms
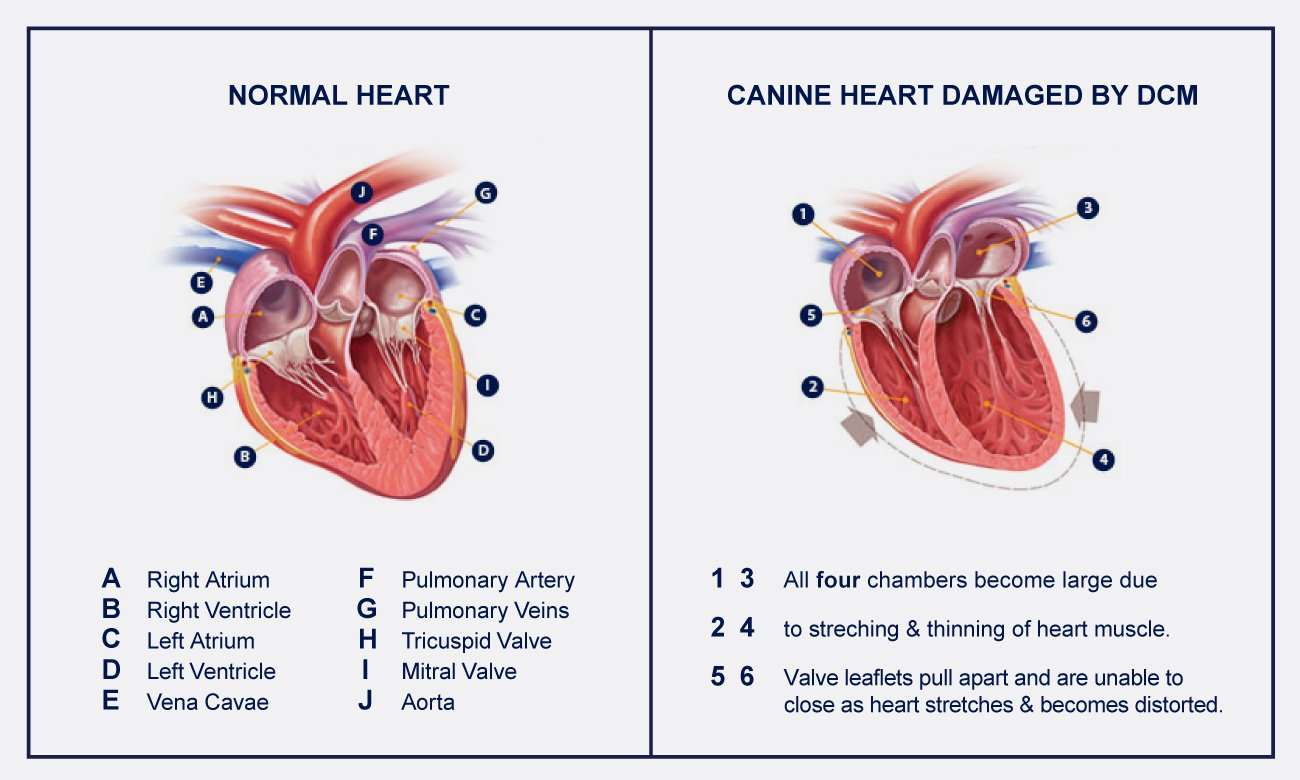
What Is Heart Failure
Heart failure doesnât mean the heart has stopped working. Rather, it means that the heart works less efficiently than normal. Due to various possible causes, blood moves through the heart and body at a slower rate, and pressure in the heart increases. As a result, the heart canât pump enough oxygen and nutrients to meet the body’s needs.
The chambers of the heart may respond by stretching to hold more blood to pump through the body or by becoming stiff and thickened. This helps to keep the blood moving, but the heart muscle walls may eventually weaken and become unable to pump as efficiently. The kidneys may respond by causing the body to retain fluid and salt. If fluid builds up in the arms, legs, ankles, feet, lungs, or other organs, the body becomes congested. Congestive heart failure is the term used to describe the condition.
What Are The Symptoms Of Congestive Heart Failure
Daniel Louis Jacoby, MD, director of Yale Medicines General Heart Failure Programand the Cardiomyopathy Inherited Cardiovascular Disease Program, says that symptoms may be mild or severe and may not always be noticeable.
Most commonly, though, a patient may experience shortness of breath, fatigue, problems with the hearts rhythm called arrhythmias, and edemaor fluid buildupin the legs, he says.
Read Also: Can Tylenol Stop A Heart Attack
What Are The Symptoms Of Chf
What are the symptoms of CHF? What should you be looking for and how do you know if a patient might be suffering from this particular condition?
Well, the first thing to note is that the symptoms of heart failure exist on a spectrum that can run from mild to moderate to severe. Symptoms can come and go and worsen over time, making CHF difficult to diagnose, but here are some of the most common things to look for, according to the American Heart Association.
Treatment And Medication Options For Congestive Heart Failure
Heart failure is a chronic condition and there is no cure. However, once youve been diagnosed, there are several things you can do to treat the condition and manage it so that it does not progress. Chief among them are lifestyle changes. These include exercising and maintaining a heart-healthy diet thats low in saturated fat, trans fats, and cholesterol.
Read Also: What Heart Chamber Pushes Blood Through The Aortic Semilunar Valve
Congestive Heart Failure: Causes Symptoms And Diagnosis
What is chronic heart disease?
Cardiomyopathy is the most common condition that arises as a result of complications from high blood pressure in the pulmonary arteries . It is also known as right heart failure because it occurs inside the right ventricle of the heart. Cardiomyopathy causes the right ventricle to dilate and pump blood less efficiently than normal. The ventricles are then pushed to their limits and eventually fail.
This condition is usually prevented when high blood pressure to the lungs is controlled. However, if left untreated, pulmonary hypertension can eventually lead to cardiopulmonary disease along with other related, life-threatening complications.
Symptoms of chronic heart disease:
Initial symptoms of cardiopulmonary diseasemay go unnoticed because they are similar to the feeling you get after a strenuous activity. These include:
Shortness of breath
Over time, these symptoms will worsen and flare up even at rest
Tell your doctor right away if you have any of the following symptoms:
Chest pain
Tired a lot
Causes of chronic heart disease:
The lungs rely on the heart to transport blood from the body to the lungs. Pulmonary hypertension is a type of increased pressure in the pulmonary artery and the right ventricle of the heart.
Blood clots in the lungs
Chronic obstructive pulmonary disease
Damage to lung tissue
Cystic fibrosis
Diagnosis of chronic heart disease
These tests include:
Right heart catheterization.
How Do I Reduce My Risk For Heart Failure
You can reduce your risk for heart failure by controlling the conditions which can lead to heart failure. Actions such as quitting smoking, eating a healthy diet, and exercising regularly are recommended for all patients. People should have their blood sugar, cholesterol, and blood pressure checked regularly.
Finally, you should meet with an experienced cardiologist if you have risks for heart disease, possible symptoms, or family history.
Recommended Reading: Gerd And Heart Flutters
How To Code If No Cause For Heart Failure Is Documented
If no cause for heart failure is spcified in the note, it is better to code just the heart failure diagnosis alone , even if a secondary diagnosis is present in the note, such as hypertension. In other words, the medical coder does not have the liberty to makes the connection between another condition and heart failure, unless it is already present in the chart. In such a case, the coder should assign separate codes for the two conditions.
Stages Of Congestive Heart Failure:
Stage 1: No symptoms are experienced, and you can easily carry on with your usual physical activities. Lifestyle changes followed by heart medications will be sufficient to manage CHF at this stage.
Stage 2: None to mild symptoms observed at rest. But you may experience palpitation, fatigue, or shortness of breath during physical activity or stress.
Lifestyle changes, heart medications, and preliminary congestive heart failure treatment will help you manage the condition.
Stage 3: None or mild symptoms were observed at rest. But your physical activity gets limited, and even little physical activity may increase your discomfort, fatigue, and breathlessness. At this stage, you should seek Congestive heart failure treatment actively and consult your doctor about the treatment procedure.
Stage 4: Symptoms are present even at rest, and you cannot carry out any physical activity. Though congestive heart failure cannot be cured at this stage, a healthy lifestyle, proper care, and congestive heart failure treatment can achieve some semblance of normalcy.
Read Also: Does Tylenol Increase Heart Rate
Heart Failure Treatment Is A Team Effort
Heart failure management is a team effort, and you are the key player on the team. Your heart doctor will prescribe your medications and manage other medical problems. Other team members — including nurses, dietitians, pharmacists, exercise specialists, and social workers — will help you achieve success. But it is up to YOU to take your medications, make dietary changes, live a healthy lifestyle, keep your follow-up appointments, and be an active member of the team.
If you notice anything unusual, don’t wait until your next appointment to discuss it with your doctor. Call them right away if you have:
- Unexplained weight gain
- Swelling in your ankles, feet, legs, or belly that gets worse
- Shortness of breath that gets worse or happens more often, especially if you wake up feeling that way
- Bloating with a loss of appetite or nausea
- Extreme fatigue or more trouble finishing your daily activities
- A lung infection or a cough that gets worse
- Fast heart rate
- New irregular heartbeat
Uncontrolled High Blood Pressure
Blood pressure that is too high means your heart has to work harder than it should. This is why hypertension that goes untreated for a long period of time raises the risk for heart failure. Excessive high blood pressure weakens the heart, and eventually it becomes unable to pump efficiently. Keeping your blood pressure within a goal range is one of the best ways to reduce the risk of heart conditions.
Also Check: Fitbit Charge 2 Accuracy Heart Rate
Tips For Managing Congestive Heart Failure End
You may be asking, How can I provide comfort to my loved one as they experience the end-of-life signs of congestive heart failure? Its only natural that you as a loved one and/or caregiver will want to be as helpful as possible, and ensure that your loved one is experiencing as little pain as possible. Heres some ways you can help:
- Communicate with the doctors and healthcare professionals: Your loved one may be too weak, or simply forget, to communicate their symptoms to the doctors and nurses. You can help by sharing this information with them in order to make sure your loved one gets what they need.
- Provide comfort: Sometimes it is just as simple as spending time with your loved one while watching a TV show, or talking about things they love. These conversations can help in alleviating some of their depression and anxiety.
- Help them remember to take their medicine: There will likely be various pills and medications that your loved one needs to take. You can help by assisting your loved one in staying on schedule.
Congestive Heart Failure: Prevention Treatment And Research
Congestive heart failure is a serious condition in which the heart doesnt pump blood as efficiently as it should. Despite its name, heart failure doesnt mean that the heart has literally failed or is about to stop working. Rather, it means that the heart muscle has become less able to contract over time or has a mechanical problem that limits its ability to fill with blood. As a result, it cant keep up with the bodys demand, and blood returns to the heart faster than it can be pumped outit becomes congested, or backed up. This pumping problem means that not enough oxygen-rich blood can get to the bodys other organs.
The body tries to compensate in different ways. The heart beats faster to take less time for refilling after it contractsbut over the long run, less blood circulates, and the extra effort can cause heart palpitations. The heart also enlarges a bit to make room for the blood. The lungs fill with fluid, causing shortness of breath. The kidneys, when they dont receive enough blood, begin to retain water and sodium, which can lead to kidney failure. With or without treatment, heart failure is often and typically progressive, meaning it gradually gets worse.
More than 5 million people in the United States have congestive heart failure. Its the most common diagnosis in hospitalized patients over age 65. One in nine deaths has heart failure as a contributing cause.
Also Check: Low Pulse High Blood Pressure Causes
Outlook For Heart Failure
Heart failure is a serious long-term condition that’ll usually continue to get slowly worse over time.
It can severely limit the activities you’re able to do and is often eventually fatal.
But it’s very difficult to tell how the condition will progress on an individual basis.
It’s very unpredictable. Lots of people remain stable for many years, while in some cases it may get worse quickly.
Unspecified Combined Systolic And Diastolic Heart Failure
- 2016201720182019202020212022Billable/Specific Code
- Edema of lung with heart disease NOS
- Edema of lung with heart failure
- Left heart failure
- Pulmonary edema with heart disease NOS
- Pulmonary edema with heart failure
- edema of lung without heart disease or heart failure
- pulmonary edema without heart disease or failure
Recommended Reading: Apple Watch 6 Heart Rate Accuracy
Complications Of Congestive Heart Failure
Heart failure can lead to a number of complications that can influence the chance of survival, including:
- Rapid Weight Loss Severe heart failure can lead to an unintentional rapid loss of weight that can be life-threatening. Heart failure can cause blood to back up into the liver and intestines, causing these organs to swell. This swelling can lead to nausea and loss of appetite, and can prevent the body from absorbing nutrients from food.
- Impaired Kidney Function Congestive heart failure weakens the hearts ability to pump blood, reducing blood flow to the kidneys. This can lead to kidney damage or kidney failure if left untreated.
- Liver Damage Heart failure can cause fluid to build up on the liver, which can lead to scarring. This makes it more difficult for the liver to carry out its day-to-day functions.
- Arrhythmias Heart failure results in damaged heart muscles, which can lead to the development of an arrhythmia, or abnormal heart beat. Arrhythmias can include the heart beating too quickly, beating too slowly, or beating irregularly.
- Heart Valve Problems If the heart is enlarged due to heart failure, the valves of the heart, which ensure appropriate direction of blood flow through the organ, may not function properly.
- Angina and Heart Attack Heart disease is a major contributing factor in many heart failure cases, and people with congestive heart failure are at continued risk of angina and heart attack.
Symptoms Of Congestive Heart Failure
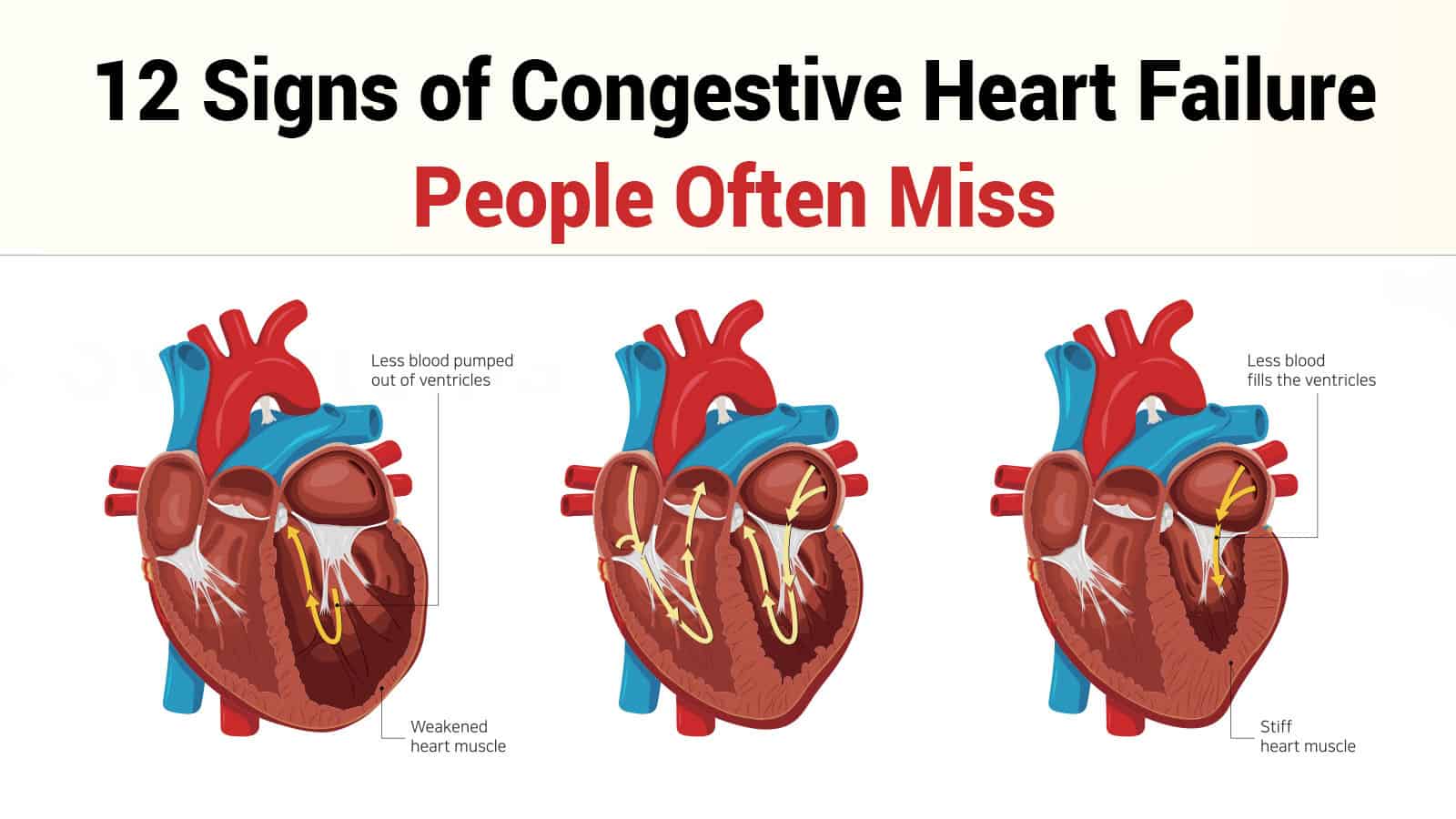
Heart failure can be ongoing , or your condition may start suddenly . Heart failure signs and symptoms may include shortness of breath when you exert yourself or when you lie down, fatigue and weakness, swelling in your legs, rapid or irregular heartbeat, reduced ability to exercise, persistent cough or wheezing with white or pink blood-tinged phlegm, increased need to urinate at night, swelling of your abdomen , very rapid weight gain from fluid retention, lack of appetite and nausea, difficulty concentrating or decreased alertness, sudden or severe shortness of breath and coughing up pink and foamy mucus, and chest pain if your heart failure is caused by a heart attack
Also Check: Massive Heart Attack Prognosis
Chf Icd 10 Codes And Guidelines
Most of the heart failure codes include in chapter 9 of ICD-10 CM manual, diseases of circulatory system, code range I00-I99.
- Combination code If patient has any type of heart failure and hypertension, it should be combined and coded as I11.0 eventhough physician has not linked both. It should not be coded combined if the medical record states the conditions are unrelated.
- Heart failure should be coded additionally when coding I11.0
- Do not code I11.9 when coding I11.0 .
- When coding biventricular heart failure it is necessary to code the type of left heart failure also according to the code also note with I50.82
Go by Failure, Heart to find correct codes for heart failure in ICD-10 CM manual index.
Look at the below scenarios to clearly understand the coding concepts of CHF.
CHF ICD 10 Code Example 1
Elizabeth is a 65 year old female who comes to emergency department for shortness of breath and leg edema from past 2 days. She came to visit doctor as the symptoms are getting worse. She has hypertension and takes Lisinopril for the same. She does not have chest pain or palpitation. She is not a smoker. Her family history includes heart disease for her mother and brother. Vitals showed temperature 97.3 F, heart rate 72 bpm, respiratory rate 25, BP 150/96 mmHg. Physical exam showed pitting edema on both the extremities, shortness of breath and dry skin. Physician ordered for blood tests, EKG and chest X-ray. This case was diagnosed as acute diastolic heart failure.
