When To Contact A Doctor
If the rate or rhythm of the heartbeat becomes irregular or is causing distressing symptoms, it is important to seek medical attention.
Even if there does not appear to be any danger, a doctor can provide assistance in reducing the risk of complications.
If a person is experiencing the following symptoms, all of which are symptoms of a heart attack, someone needs to call 911:
- chest pain
Learn The Prevention Measures
Certain measures can be taken to prevent a sudden increase in heartbeat or it becoming a health concern.
Ablation by Radiofrequency Catheter
Catheters are made to enter the heart through blood vessels. Electrodes are present at the catheter ends they are heated and used to damage or ablate the small area of heart that is causing the fast heartbeat.
Medicines
Anti-arrhythmic drugs, if taken regularly can help in preventing tachycardia. Your physician may prescribe other medicines that should be taken along with anti-arrhythmic drugs including channel blockers, such as Cardizem and Calan , or beta-blockers, such as Inderal and Brevibloc .
ICD
It is a device, which monitors your heartbeat continuously. It is implanted surgically into the chest. It detects any abnormality in heartbeat and gives electric shocks to bring back heart rhythm to normal.
Surgery
In some cases surgery is required to remove an area of tissue. This is only done in cases where other therapies are ineffective or if the patient has another disorder of the heart.
Warfarin
Warfarin makes blood clotting difficult and is generally given to persons who have moderate or high risk of having heart attack or stroke. Though, with warfarin the risk of bleeding is raised, it is given to persons, in whom, the risk of heart attack or stroke is greater in comparison to risk of bleeding.
High Resting Heart Rate: Should You Worry
In general, a slower resting heart rate is a sign of good health. Some athletes and people who are very active even have heart rates that dip below 60 when theyre at rest.
A high resting heart rate, on the other hand, can be an indicator of problems such as:
- Poor physical condition.
- Infections.
- Thyroid problems.
Often, a high resting heart rate is a sign that your heart is working harder than it needs to. Like any muscle, the heart doesnt work as well when its out of shape. In people who arent very active, the heart isnt as efficient. It has to work harder to pump blood through your body, Dr. Singh says.
Also Check: Zyrtec And Heart Palpitations
You Have A Heart Arrhythmia
A heart arrhythmia happens when theres some sort of electrical malfunction in your heart, which can cause it to beat irregularly. There are many forms, and they have different causes, but they can often make it feel like your heart is beating quickly or strangely out of nowhere. Although an arrhythmia sounds like a dire diagnosis from Greys Anatomy, they actually arent always serious. Many arrhythmias are not life-threatening, Dr. Mills-Frazier says. Obviously with higher-risk patients, they can be, but theyre often treatable. Arrhythmias often present with side effects like dizziness, nausea, fainting, chest pain, and shortness of breath, according to the American Heart Association.
Causes Of Supraventricular Tachycardia
An episode of supraventricular tachycardia occurs when abnormal electrical impulses suddenly start in the upper chambers of the heart, and override the heart’s natural rhythm.
SVT is sometimes called paroxysmal supraventricular tachycardia . Paroxysm means a sudden temporary disturbance of heart rhythm.
PSVT is usually caused by a short circuit in the electrical system of the heart, which causes an electrical signal to travel rapidly and continuously around in a circle, forcing the heart to beat each time it completes the circuit.
Another type of SVT is called Wolff-Parkinson-White syndrome, where an abnormal electrical connection occurs between the atria and ventricles . People with Wolff-Parkinson-White syndrome are born with a strand of extra muscle tissue between these chambers. This produces a short circuit, which causes the fast heartbeat.
Also Check: Does Tylenol Increase Heart Rate
Increase In Resting Heart Rate Over Time Linked To Heart Disease Death
Study Suggests Regularly Checking Pulse to See Where You Stand
It has been known that a high resting heart rate is a risk for heart disease. Now new research suggests that an increase in resting heart rate over time may actually place a person at greater risk for dying from heart disease and/or other causes in the future. The findings appear in the Dec. 21 issue of the Journal of the American Medical Association.
For adults, a normal resting heart rate is usually between 60 to 100 beats per minute. Athletes tend to have lower resting heart rates.
“A healthy adult is expected to have about 70 beats per minute in resting heart rate and the point is to follow it over time — if it increases more than 10 beats you may talk to your family doctor to get advice about lifestyle changes and/or get a thorough check of your system,” study author Ulrik Wisloff, PhD, tells WebMD in an email.
Curious as to where you stand?
When you wake in the morning, find your pulse on your wrist or neck. Choose the spot that works best for you. Make sure there is a clock nearby. After you find the beat, count how many beats occur within one minute.
What Are The Possible Causes
Tachycardia is usually caused by anything that creates a problem with the electrical impulses, which control rate of the pumping action of the heart. There are multiple things that can disrupt the electrical system of the heart. Some of these are:
- Damage to tissues of the heart due to heart disease
- Anemia
- Congenital disease or abnormality of heart
- Electrical pathways that are not normal and present in the heart at birth
- Exercise
- Low or high blood pressure
- Sudden stress, for instance fright
- Smoking
- Drinking excessive caffeine containing beverages
- Side effects of medicines
- Recreational drug abuse, such as cocaine
- Hyperthyroidism
- Electrolyte imbalance
In certain cases, the cause of sudden increase in heart rate cant exactly be found.
Risk Factors
The risk of getting tachycardia is increased by any condition, which strains the heart or causes damage to the tissues of the heart. Medical treatment or lifestyle changes may lower the risk that is increased by the below mentioned factors:
- High blood pressure
- Underactive or overactive thyroid gland
- Diabetes
- Use of drugs of recreation
Certain other factors, which may raise your risk of getting tachycardia, are:
- Older age: Elderly are at an increased risk of getting tachycardia due to wear and tear of the heart related to age.
- Family: Positive family history of heart rhythm disorders and tachycardia in particular increases your risk.
Medical Tests
Also Check: Can Acid Reflux Cause Heart Palpitations
Increase In Resting Heart Rate Is A Signal Worth Watching
- By Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
When you sit quietly, your heart slips into the slower, steady pace known as your resting heart rate. An increase in your resting heart rate over time may be a signal of heart trouble ahead.
Your heart rate changes from minute to minute. It depends on whether you are standing up or lying down, moving around or sitting still, stressed or relaxed. Your resting heart rate, though, tends to be stable from day to day. The usual range for resting heart rate is anywhere between 60 and 90 beats per minute. Above 90 is considered high.
Many factors influence your resting heart rate. Genes play a role. Aging tends to speed it up. Regular exercise tends to slow your heart rate down. Stress, medications, and medical conditions also influence your resting heart rate.
Results of observational research studies support a link between health and heart rate. Researchers from Norway previously reported the results of a large study looking at changes in resting heart rate over 10 years. They recruited more than 29,000 people without any history or heart disease, high blood pressure, or any other type of cardiovascular disorder, and measured their resting heart rates when they started the study and again 10 years later. This study was published in the Journal of the American Medical Association.
How to lower your resting heart rate
What Are The Common Symptoms
Doctors and scientists are learning new things about this virus every day. So far, we know that COVID-19 may not cause any symptoms for some people.
You may carry the virus for 2 days or up to 2 weeks before you notice symptoms.
Some common symptoms that have been specifically linked to COVID-19 include:
-Shortness of breath
-A cough that gets more severe over time
-A low-grade fever that gradually increases in temperature
Less common symptoms include:
Don’t Miss: What Happens After A Massive Heart Attack
What’s A Normal Heart Rate
“Heart rate is the number of times the heart beats per minute,” explains Sameer Arora, MD, a cardiologist with the University of North Carolina School of Medicine in Chapel Hill.
Your heart rate reflects how fast your heart is contracting or pumping blood through your body, adds , a cardiac electrophysiologist at Henry Ford Health System in Detroit.
The normal range is 60 to 100 beats per minute , but this varies from person to person. One person’s normal may hover at the upper end of the spectrum while another settles in the lower range. Athletes tend to have lower-than-usual heart rates.
Typically, a lower heart rate is better. “The slower it is, the more efficient your heart is working,” says Dr. Steinbaum. “Your arteries and heart are dilating and flexible, so your heart doesn’t have to work as hard.”
Bear in mind that a heart rate that exceeds 100 bpm or drops below 60 bpm doesn’t necessarily indicate that anything is wrong.
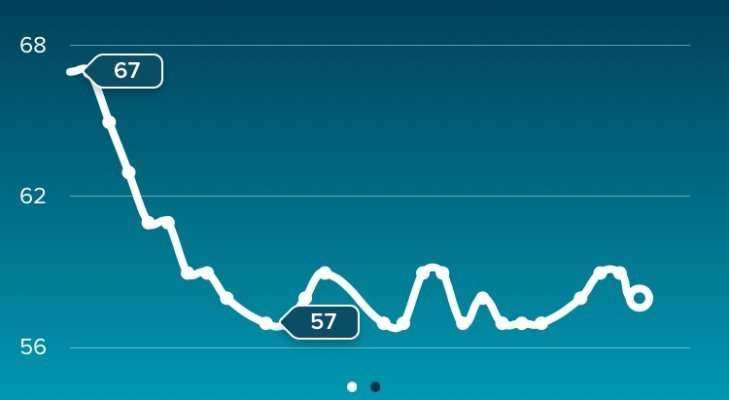
The Hammock: Relaxed In Bed And Ready To Rise
The hammock curve shows an ideal heart rate journey. During your initial sleep stages, your body relaxes and your blood pressure and heart rate begin to drop.
In this scenario, your lowest RHR occurs near the midpoint of your sleep, when the amount of melatonin present reaches a peak. If you are perfectly in sync with the suns patterns, your body temperature drops to its lowest level around 4 a.m.
Your RHR may momentarily rise during REM sleep. This is normal and you can ignore these temporary spikes when looking for the hammock curve during your sleep.
As you wake in the morning, your heart rate begins to rise. The hammock curve is a sign that your body was relaxed during the night and is ready to rise after a quality nights sleep.
Read Also: How Long Does End Stage Heart Failure Last
Ultimately There Are Lots Of Reasons Your Heart May Be Racing
Sometimes its nothing major. Other times, especially when accompanied by symptoms like feeling lightheaded or dizzy, having chest pain, or feeling fatigue, it can be a sign that you should see a doctor. It doesnt matter how healthy you are or how healthy you think you are, Dr. Doshi says. If your heart doesnt feel right for you, its worth getting a checkup.
Related:
Increase In Resting Heart Rate Linked To Death

The study included nearly 30,000 men and women without known heart disease. Researchers measured their resting heart rate twice about 10 years apart. Compared to healthy people whose resting heart rate stayed less than 70 beats per minute during a 10-year period, those whose pulse was less than 70 beats per minute at the first measurement and then greater than 85 at the second were more likely to die from heart disease and other causes after 12 years of follow-up.
Participants whose heart rate was between 70 and 85 at the first measure and then greater than 85 the next time it was measured were also more likely to die from heart disease or other causes.
Further study is needed, but the findings may help identify a group of seemingly healthy people who are at risk for heart disease before they develop any other signs or symptoms, the study authors conclude.
Also Check: Tylenol Heart Palpitations
Medical Causes Of A Fluctuating Heart Rate
Medical issues â many of them easily treated â can also cause a fluctuating pulse, including:
What Are The Best Places To Check Pulse
The best places to check your heart rate are your wrist, the side of your neck, the inside of your elbow, and the top of your foot .
How to Check Your Pulse Video
Watch Emily Reeve, the Senior Cardiac Nurse at the British Heart Foundation, show you how to check your pulse.
Heart Rate Monitors
You can track your heart rate with a wrist monitor like the popular LETSCOM Fitness Tracker .
Or, check out this detailed review of heart rate monitors to help you find the right one for you.
Heart rate monitors make it easier to track your heart rate consistently and learn which activities raise or lower your pulse the most.
You May Like: Mayo Clinic Heart Rate
You Have A Cold Or Fever
If your pounding heart is accompanied by typical signs of a cold or fever, like an elevated temperature, coughing, and sneezing, this is likely the culprit. Battling an infection requires your body to work harder than usual, and that includes making your heart beat faster in order to fight for homeostasis and kick the infection to the curb, Dr. Mills-Frazier says.
Resting Heart Rate During The Night
Nightly average RHR varies widely between individuals. A normal heart rate can range anywhere from 40 to 100 beats per minute and still be considered average. It can also change from day to day, depending on your hydration level, elevation, physical activity, and body temperature. As with many of your bodys signals, its best to compare your RHR with your own baseline. Avoid comparisons to those around you.
When looking at your RHR curve, pay special attention to these three things:
- Your trend: Does your RHR go up, down, or stay level during the night?
- Your lowest point: When is your RHR lowest?
- Your end: Right before you wake up, does your RHR change?
With these questions in mind, here are three patterns you may recognize in the night-time heart rate curves you can see with Oura:
Recommended Reading: Does Ibs Cause Heart Palpitations
Normal Causes Of A Fluctuating Heart Rate
Your resting heart rate is when your heart is doing the least amount of work. That’s measured when you’re sleeping, sitting or lying down and feeling calm and relaxed. Things like your age, sex and physical fitness can affect your resting heart rate.
Plenty of everyday things cause heart rates to fluctuate. You can expect your pulse to change throughout the day as your heart adjusts to different energy needs.
When I Eat Carbs And Sugar My Heart Rate Increases Why Is That
Ive been on a very low carb diet for the past four months. When I eat carbs and sugar, my heart rate increases and I can feel it even when Im not doing anything. Why is that? Can I stop it?
A person is diagnosed with tachycardia when the heart rate is more than 100 beats per minute . The normal resting heart rate for adults is about 60 to 100 BPM and for infants, it is about 110 BPM.
Tachycardia after eating is an uncommon disorder and for the people who experience it, it can create anxiety and stress. Experiencing slightly higher heart rate after having snacks or meals is quite normal, because increased flow of blood is required to digest the food. But, if your heart starts beating rigorously after meals, then it could be a symptom of tachycardia. There is no need to panic as people who experience it can lead a normal life.
The episodes of rapid heartbeat usually begin within 30 to 60 minutes after a meal. The heart rate may go up to 120 beats per minute or even more. Sometimes, it lasts up to 6 hours. An adrenaline rush may be experienced by the person. There can be difficulty in resting, sleeping, or breathing. The person may suffer from bloating and indigestion. If your heart starts beating irregularly or very rapidly after eating, you could have cardiac arrhythmia.
Causes of High Heart Rate after Meals
> > Processed food or food high in oil or food rich in MSG, nitrates and sodium can make your heart beat faster.
Also Check: Can Benadryl Cause Arrhythmias
Youve Had A Lot Of Caffeine
While most people can handle a certain level of caffeine just fine, overdoing it can make your heart speed up. A bunch of patients come to see me with an elevated heart rate, then they tell me they drink multiple highly caffeinated beverages daily, Dr. Mills-Frazier says. Theyre revving themselves up. This is most likely to happen if youve had too much caffeine, but it could also happen in response to small amounts if youre just sensitive to this stimulant.
According to the Mayo Clinic, its safe for adults to have up to 400 milligrams of caffeine a day, or around the amount in four cups of coffee, 10 cans of soda, or two energy drinks . Try cutting back on caffeine gradually to see if it reduces your racing heart. If not, get in touch with your doctor.
