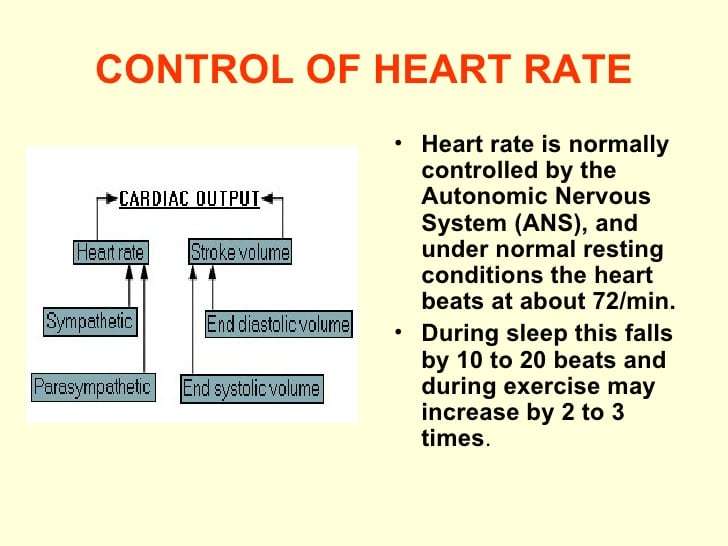
Health And Performance Considerations
Higher heart rates may be an indication of poor heart function and higher than usual stress being placed on the hearts ability to circulate blood. This may further indicate heart disease conditions.
From a performance stand point knowing specific heart rate training zones can optimize our bodys ability to adapt to performance requirements. Determining these zones can be done through many different methods, including VO2 or lactate testing, formulas and general training regimens. It then becomes necessary to monitor intensity in order to optimize your chances for success. To monitor your intensity there are several methods available to you. First is the perceived exertion method in which you rate your perception of how hard you are exerting yourself during a workout. The acronym for this is RPE . The scale on which to base your perceptions range from 1 – 10. See below.
The scale can be broken down as follows:
;;;;;0: Nothing
What Is Heart Failure
Heart failure is a chronic, progressive condition in which the heart muscle is unable to pump enough blood to meet the bodys needs for blood and oxygen. Basically, the heart cant keep up with its workload.
Watch an animation of heart failure.
At first the heart tries to make up for this by:
- Enlarging. The heart stretches to contract more strongly and keep up with the demand to pump more blood. Over time this causes the heart to become enlarged.
- Developing more muscle mass. The increase in muscle mass occurs because the contracting cells of the heart get bigger. This lets the heart pump more strongly, at least initially.
- Pumping faster. This helps increase the hearts output.
The body also tries to compensate in other ways:
- The blood vessels narrow to keep blood pressure up, trying to make up for the hearts loss of power.
- The body diverts blood away from less important tissues and organs , the heart and brain.
These temporary measures mask the problem of heart failure, but they dont solve it. Heart failure continues and worsens until these compensating processes no longer work.
Eventually the heart and body just cant keep up, and the person experiences the fatigue, breathing problems or other symptoms that usually prompt a trip to the doctor.
The bodys compensation mechanisms help explain why some people may not become aware of their condition until years after their heart begins its decline.
Pulmonary Compliance And Volume Shifts Between Systemic And Pulmonary Circuits
So far in this review cardiac function has been considered as one unit starting from the right atrium and exiting from the aortic valve. Pulmonary vessels and independent functions of the right and left ventricle have not been considered. This simplification normally produces a small error because total pulmonary compliance is only one-seventh of total systemic vascular compliance and the pulmonary circuit does not contain a lot of volume that can be shifted to the systemic circulation. It also cannot take up a lot of volume without causing a large increase in pulmonary venous pressure and a major disturbance to pulmonary gas exchange. Even maximal sympathetic stimulation results in only a small shift from the pulmonary circuit to the systemic circulation . However, the small volume reserves in the pulmonary vasculature become important during the variation in pulmonary flow during ventilation, especially during mechanical ventilation and increases in pleural pressure.
Recommended Reading: Does Acid Reflux Cause Heart Palpitations
The Intrinsic Cardiac Ans
In addition to the extrinsic ANS, the heart is also innervated by a complex intrinsic ANS.
Armour et;al. provided a detailed map of the distribution of autonomic nerves in human heart . Throughout the heart, numerous cardiac ganglia, each of which contains 200 to 1000 neurons, form synapses with the sympathetic and parasympathetic fibers that enter the pericardial space . The vast majority of these ganglia are organized into ganglionated plexi on the surface of the atria and ventricles . The intrinsic cardiac ANS is a complex network composed of ganglionated plexi, concentrated within epicardial fat pads, and the interconnecting ganglia and axons . The ganglionated plexi may function as integration centers modulating extrinsic and intrinsic cardiac ANS activities .
In the atria, ganglionated plexi are concentrated in distinct locations on the chamber walls . Specifically, the sinus node is primarily innervated by the right atrial ganglionated plexi, whereas the atrioventricular node is innervated by the inferior vena cavainferior atrial ganglionated plexi .
Another region that is richly innervated by the ANS and has a high density of ganglionated plexi is the pulmonary veinleft atrium junction, which contains closely located adrenergic and cholinergic nerves .
A Brief Overview Of Hrv Metrics
We can describe 24 h, short-term or brief, and ultra-short-term HRV using time-domain, frequency-domain, and non-linear measurements. Since longer recording epochs better represent processes with slower fluctuations and the cardiovascular systems response to a wider range of environment stimuli and workloads, short-term and ultra-short-term values are not interchangeable with 24 h values.
Time-domain indices of HRV quantify the amount of variability in measurements of the interbeat interval , which is the time period between successive heartbeats . These values may be expressed in original units or as the natural logarithm of original units to achieve a more normal distribution .
Table 1. HRV time-domain measures.
Frequency-domain measurements estimate the distribution of absolute or relative power into four frequency bands. The Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology divided heart rate oscillations into ultra-low-frequency , very-low-frequency , low-frequency , and high-frequency bands .
Table 2. HRV frequency-domain measures.
Finally, non-linear measurements allow us to quantify the unpredictability of a time series .
Table 3. HRV non-linear measures.
You May Like: How To Calculate Resting Heart Rate
Assessment In Clinical And Optimal Performance Interventions
The selection of HRV time-domain, frequency-domain, and non-linear measurements and norms to assess progress in clinical and optimal performance interventions should be informed by peer-reviewed studies. Professionals training specialized populations might supplement published norms for the general population with values from their own clients. The rigorous data reporting guidelines proposed by Laborde et al. could guide their efforts to publish their norms to remedy gaps in the literature. The metrics most strongly correlated with clinical improvement and athlete performance gains in these reports could be incorporated in pretreatment/posttreatment, within-session, and across-session assessment. While a full treatment of HRV variables in relation to the HRV biofeedback intervention is beyond the scope of this article, we will briefly touch on the issues that seem to us to be the key ones .
In addition to the primary literature, the Association for Applied Psychophysiology and Biofeedback has published two references that identify metrics associated with clinical and optimal performance outcomes, Evidence-Based Practice in Biofeedback and Neurofeedback and Foundations of Heart Rate Variability Biofeedback: A Book of Readings . Further, readers might consult Gevirtz, Lehrer, and Schwartzs excellent chapter on Cardiorespiratory Biofeedback in Schwartz and Andrasiks Biofeedback: A Practitioners Guide .
Cav31 Subunit: Cacna1g Gene
Cav3.1 channel biophysical properties are very similar to those of the Cav3.2 T-type, although Cav3.1 channels do appear to exhibit a faster recovery from inactivation when membrane potential returns to negative values following depolarization. Cav3.1 subunits are expressed abundantly throughout the brain and the sinoatrial node of the heart, and lower levels are expressed in placenta, lung, and kidney.
Mice in which the Cav3.1 gene is genetically deleted appear anatomically and physiologically normal, although there are several alterations to nervous and cardiovascular system functions. Nervous system-associated defects include an absence of GABAB receptor agonist-induced spike-wave discharges, a lack of thalamic 14 Hz delta waves, a reduction of sleep spindles associated with normal sleep, and an enhanced visceral pain response. Overall, it appears that Cav3.1 channels play a crucial role in thalamocortical burst-firing processes relevant to a number of higher central nervous system functions, including thalamic sensory gating and the control of consciousness. In the heart, Cav3.1 gene deletion is associated with both slowing of the heart rate and atrioventricular dysfunction, indicating that this T-type calcium channel normally contributes to setting the basal heart rate and to atrioventricular conduction.
Alex Y. Tan, Richard L. Verrier, in, 2013
Don’t Miss: Vitamin D3 And Heart Palpitations
Cardiovascular Homeostasis Results Primarily From A Negative Feedback Reflex
A considerable body of evidence suggests that glutamate and -aminobutyric acid play dominant neurotransmitter roles in the baroreceptor reflex. For example, excitatory amino acid antagonists administered directly into the NTS, CVLM, or spinal cord completely eliminate baroreceptor reflex-evoked sympathetic vasomotor responses. Similarly, GABA antagonists injected into the RVLM block such responses. Still, many other inputs and neurotransmitters at these sites have been shown to modulate baroreceptor reflex function.
In addition to the direct autonomic control of the heart and vasculature, afferent inputs from arterial baroreceptors influence other brain outputs relevant to cardiovascular regulation.
M. Ito, in, 2009
Limitations Of The Study
The model was validated with a small complementary set of clinical hemodynamic data of HTxRs and healthy individuals. However, the data contained only a limited number of patient measurements and hemodynamic parameters. Consequently, the model should undergo further validation, based on a more comprehensive dataset.
The often-observed diastolic dysfunction in HTxRs was not explicitly modeled. Thus, the cardiac model represents a properly vascularized, short-term post-HTx condition in which no remodeling has taken place yet. Simulations to investigate the diastolic graft dysfunction and its influence on resting and exercise hemodynamics were not part of this study but certainly interesting for future study, to investigate late HTxR hemodynamic response.
You May Like: How Much Blood Does The Heart Pump
S Sd1 Sd2 And Sd1/sd2
We can analyze a Poincaré plot by fitting an ellipse to the plotted points. After fitting the ellipse, we can derive three non-linear measurements, S, SD1, and SD2. The area of the ellipse which represents total HRV correlates with baroreflex sensitivity , LF and HF power, and RMSSD.
The standard deviation of the distance of each point from the y=x axis , specifies the ellipses width. SD1 measures short-term HRV in ms and correlates with baroreflex sensitivity , which is the change in IBI duration per unit change in BP, and HF power. The RMSSD is identical to the non-linear metric SD1, which reflects short-term HRV . SD1 predicts diastolic BP, HR Max HR Min, RMSSD, pNN50, SDNN, and power in the LF and HF bands, and total power during 5 min recordings .
The standard deviation of each point from the y=x+ average RR interval specifies the ellipses length. SD2 measures short- and long-term HRV in ms and correlates with LF power and BRS . The ratio of SD1/SD2, which measures the unpredictability of the RR time series, is used to measure autonomic balance when the monitoring period is sufficiently long and there is sympathetic activation. SD1/SD2 is correlated with the LF/HF ratio .
Clinical Links Between Coronary Microvascular Disease And Heart Failure With Preserved Ejection Fraction
Cardiovascular risk factors, such as hypertension, diabetes mellitus, hyperlipidaemia, and obesity, lead to a cascade of pro-inflammatory events that eventually lead to eNOS uncoupling and endothelial dysfunction. Hypertension has been implicated in the development of CMD. In addition to causing eNOS dysfunction, it leads to enhanced endothelin production resulting in inappropriate coronary endothelial vasoconstriction. Hypertension is also associated with architectural changes, such as capillary rarefaction, medial hypertrophy, and fibrosis of arteriolar vessels. These result in an inability of the coronary vasculature to augment its blood flow. Insulin resistance and hyperglycaemia, both cardinal features of diabetes mellitus, also alter coronary vascular tone regulation. Coronary microvascular disease is prevalent in patients with T2DM and studies have shown that impaired myocardial flow reserve is strongly associated with the degree of albuminuria in these patients. Coronary microvascular disease and albuminuria may, therefore, share common mechanisms related to the pathogenesis of diabetic micro-vasculopathy.
Recommended Reading: Can Reflux Cause Heart Palpitations
Age Related Structural Changes:
Structural changes with aging involve the myocardium, the cardiac conduction system, and the endocardium. There is a progressive degeneration of the cardiac structures with aging, including a loss of elasticity, fibrotic changes in the valves of the heart, and infiltration with amyloid.The age-associated structural characteristics that have the greatest impact involve the contractility of the heart’s left ventricular wall.;The pumping capacity of the heart is reduced with age due to a variety of changes affecting the structure and function of the heart muscle.For decades, it was thought that the heart undergoes atrophy with advancing age, but evidence suggests that,An age-related increase in the left ventricular posterior wall thickness of approximately 25% has been found between the second and the seventh decade. An increase in heart mass with aging, for the most part, is due to an increase in the average myocyte size, whereas the number of myocardial cells declines.
Valves
An age-related increase in valvular circumference has been;reported in all four cardiac valves ,with the greatest changes occurring in the aortic valve ;Calcific deposits frequently are present .one or more aortic valve cusp.These changes do not usually cause significant dysfunction, although in some older adults, severe aortic valvular stenosis and mitral valvular insufficiency are related to degenerative changes with age. Clinical heart murmurs are detected more frequently.
Cardiac Muscle Compliance
Context Is Crucial When Interpreting Hrv Measurements
Awareness of the context of recording and subject variables can aid interpretation of both 24 h and short-term HRV measurements. Important contextual factors include recording period length, detection or recording method, sampling frequency, removal of artifacts, respiration, and whether or not there is PB. Important subject variables are age, sex, HR, and health status. In addition, influences of position, movement, recency of physical activity, tasks, demand characteristics, and relationship variables can all affect measurements subtly or even greatly by changing ANS activation, breathing mechanics, and emotions.
Don’t Miss: Can Acid Reflux Cause Heart Palpitations
The Hearts Electrical System
The atria and ventricles work together, alternately contracting and relaxing to pump blood through the heart. The electrical system of the heart is the power source that makes this possible. Heres what happens during a normal heartbeat:
Irregular heart rhythms can also occur in normal, healthy hearts. Arrhythmias can also be caused by certain substances or medications, such as caffeine, nicotine, alcohol, cocaine, inhaled aerosols, diet pills, and cough and cold remedies. Emotional states such as shock, fright or stress can also cause irregular heart rhythms.
Arrhythmias that are recurrent or related to an underlying heart condition are more concerning and should always be evaluated by a doctor.
In most cases, treating the underlying condition will take care of the arrhythmia. If not, many medications and procedures are available to eliminate or control the abnormal heart rhythm.
Nsg 5003 2018 Assessment
- 94%88 out of 94 people found this document helpful
This preview shows page 164 – 166 out of 346 pages.
We have textbook solutions for you!
The document you are viewing contains questions related to this textbook.The document you are viewing contains questions related to this textbook.
Nurunnahar Womens College NURSING 101
CH37
Grand Canyon University NURS 6501N
midterm exam.pdf
We have textbook solutions for you!
The document you are viewing contains questions related to this textbook.The document you are viewing contains questions related to this textbook.
Recommended Reading: Acid Reflux Cause Palpitations
Assessment During Hrv Biofeedback Trials
During HRV biofeedback training, adults may be instructed to engage in paced abdominal breathing between 4.5 and 7.5 bpm guided by a real-time display of instantaneous HR and respiration. As clients breathing approaches their resonance frequency, the rate that most strongly stimulates their baroreceptor reflex, RSA will increase . Since respiration rate helps to determine the peak HRV frequency , successful training should produce a lower peak frequency and greater LF power than a resting baseline obtained when clients breathe from 12 to 15 bpm. PB at 6 bpm should result in a spectral peak at 0.1 Hz, while breathing at 7.5 bpm should create a peak at 0.125 Hz. Both 6 and 7.5 bpm rates will also increase power in the LF, which ranges from 0.04 to 0.15 Hz.
How Do I Take My Pulse
You can tell how fast your heart is beating by feeling your pulse. You can feel your pulse on your wrist or neck. Place the tips of your index and middle fingers on the inner wrist of your other arm, just below the base of your thumb. Or, place the tips of your index and middle fingers on your lower neck, on either side of your windpipe. Press lightly with your fingers until you feel the blood pulsing beneath your fingers. You may need to move your fingers around slightly up or down until you feel the pulsing.
You can count the number of beats in 10 seconds and multiply by 6 to determine your heart rate in beats per minute. A normal heart rate, at rest, is 50 to 100 beats per minute.
Your Heart Rate: Pulse in 10 seconds x 6 =_
Recommended Reading: Does Acid Reflux Cause Heart Palpitations
Effector Systems Of Arterial Baroreceptor Reflexes
The term arterial baroreceptor reflex is used to refer to a variety of physiological responses elicited by changes in baroreceptor afferent activity. While the baroreceptor reflex is often used in specific reference to the reflexive change in ABP and heart rate brought about by changing autonomic outflow to the heart and vasculature, there are a large number of physiological responses resulting from changes in baroreceptor afferent input, and they would each appropriately be termed a baroreceptor reflex. For example, decreases in ABP sensed by arterial baroreceptors elicit an increase in vasopressin secretion from the posterior pituitary and an increase in thirst . Thus, baroreceptor reflexes can be viewed as having autonomic, endocrine, and behavioral effectors, all of which interact to promote cardiovascular homeostasis .
Figure 2. Baroreceptor reflex effector systems. Changes in baroreceptor afferent activity reflexively influence many outputs of the brain relevant to cardiovascular regulation. ACTH, adrenocorticotropic hormone.
Figure 3. Relationship between arterial blood pressure, baroreceptor afferent activity, and cardiovascular autonomic outflow. SNS, sympathetic nervous system; PNS, peripheral nervous system; HR, heart rate; CO, cardiac output.
M.C. Andresen, D. Mendelowitz, in, 2009
