How Does The Heart Beat
The heart gets messages from the body that tell it when to pump more or less blood depending on a person’s needs. For example, when we’re sleeping, it pumps just enough to provide for the lower amounts of oxygen needed by our bodies at rest. But when we’re exercising, the heart pumps faster so that our muscles get more oxygen and can work harder.
How the heart beats is controlled by a system of electrical signals in the heart. The sinus node is a small area of tissue in the wall of the right atrium. It sends out an electrical signal to start the contracting of the heart muscle. This node is called the pacemaker of the heart because it sets the rate of the heartbeat and causes the rest of the heart to contract in its rhythm.
These electrical impulses make the atria contract first. Then the impulses travel down to the atrioventricular node, which acts as a kind of relay station. From here, the electrical signal travels through the right and left ventricles, making them contract.
One complete heartbeat is made up of two phases:
Where Are The Heart And Blood Vessels Found
The heart is a fist-sized organ which lies within the chest behind the breastbone . The heart sits on the main muscle of breathing , which is found beneath the lungs. The heart is considered to have two ‘sides’ – the right side and the left side.
The heart has four chambers – an atrium and a ventricle on each side. The atria are both supplied by large blood vessels that bring blood to the heart . Atria have special valves that open into the ventricles. The ventricles also have valves but, in this case, they open into blood vessels. The walls of the heart chambers are made mainly of special heart muscle. The different sections of the heart have to squeeze in the correct order for the heart to pump blood efficiently with each heartbeat.
Blood Vessels Arteries Capillaries Veins Vena Cava Central Veins
Image 1: Blood Vessels. Arteries carry oxygen rich blood from the left side of the heart to the tissues and organs. After oxygen leaves the blood and moves into the tissues, the level of oxygen in the blood becomes low. The veins carry blood that has a low level of oxygen back to the right side of the heart. Blood from the veins is pumped from the right side of the heart through the blood vessels of the lungs, where new oxygen is picked up. This oxygen rich blood flows from the lungs to the left side of the heart.
Also Check: Does Acid Reflux Cause Heart Palpitations
What Are The Coronary Arteries
Like all organs, your heart is made of tissue that requires a supply of oxygen and nutrients. Although its chambers are full of blood, the heart receives no nourishment from this blood. The heart receives its own supply of blood from a network of arteries, called the coronary arteries.
Two major coronary arteries branch off from the aorta near the point where the aorta and the left ventricle meet:
- Right coronary artery supplies the right atrium and right ventricle with blood. It branches into the posterior descending artery, which supplies the bottom portion of the left ventricle and back of the septum with blood.
- Left main coronary artery branches into the circumflex artery and the left anterior descending artery. The circumflex artery supplies blood to the left atrium, as well as the side and back of the left ventricle. The left anterior descending artery supplies the front and bottom of the left ventricle and the front of the septum with blood.
These arteries and their branches supply all parts of the heart muscle with blood.
When the coronary arteries narrow to the point that blood flow to the heart muscle is limited , a network of tiny blood vessels in the heart that aren’t usually open may enlarge and become active. This allows blood to flow around the blocked artery to the heart muscle, protecting the heart tissue from injury.
Exchange Of Gases Nutrients And Waste Between Blood And Tissue Occurs In The Capillaries
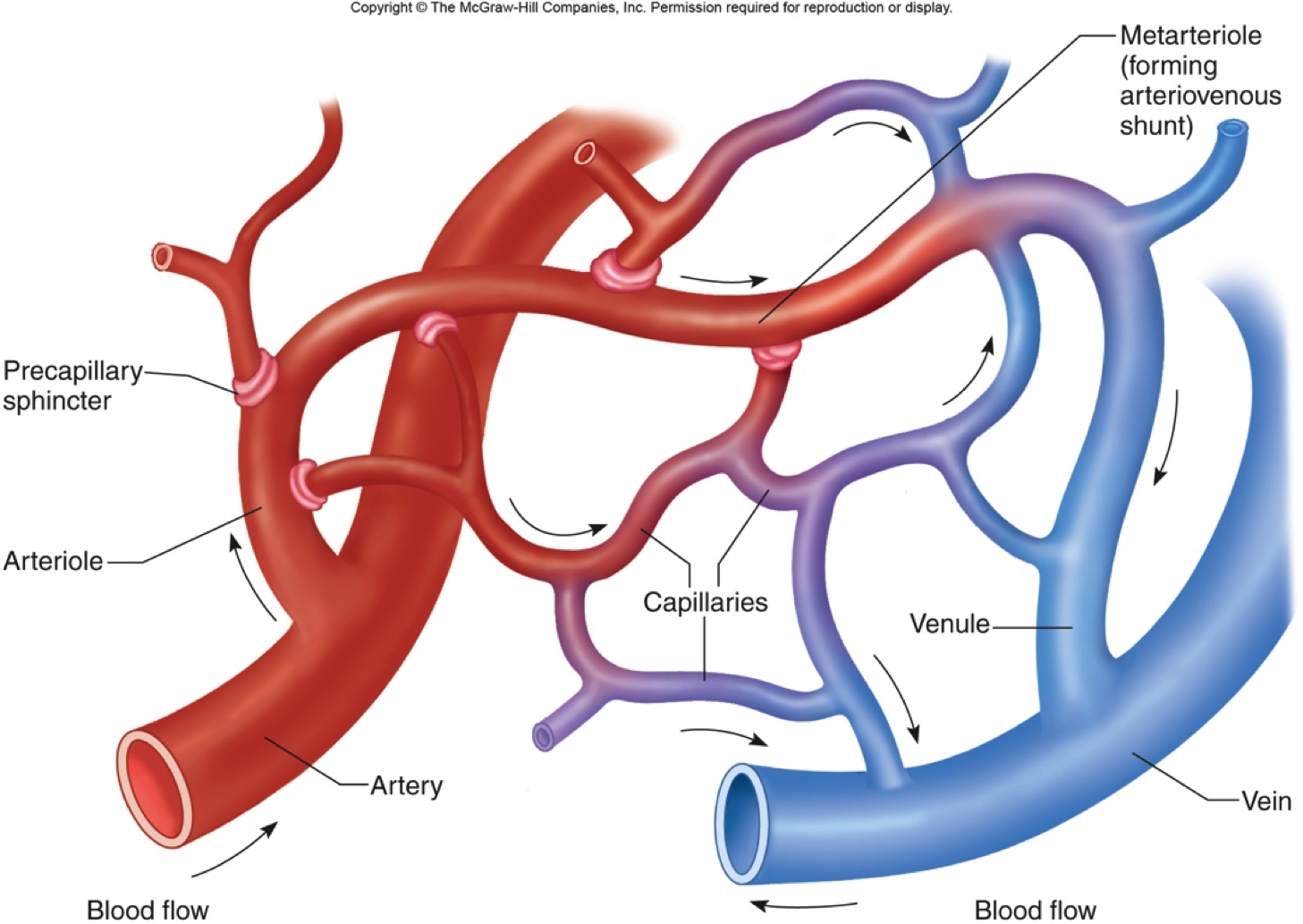
Capillaries are tiny vessels that branch out from arterioles to form networks around body cells. In the lungs, capillaries absorb oxygen from inhaled air into the bloodstream and release carbon dioxide for exhalation. Elsewhere in the body, oxygen and other nutrients diffuse from blood in the capillaries to the tissues they supply. The capillaries absorb carbon dioxide and other waste products from the tissues and then flow the deoxygenated blood into the veins.
Also Check: Acid Reflux Cause Palpitations
Anatomy Of Veins And Arteries
The walls of veins and arteries are both made up of three layers:
- Outer. Tunica adventitia is the outer layer of a blood vessel, including arteries and veins. Its mostly composed of collagen and elastic fibers. These fibers enable the veins and arteries to stretch a limited amount. They stretch enough to be flexible while maintaining stability under the pressure of blood flow.
- Middle. The middle layer of the walls of arteries and veins is called the tunica media. Its made of smooth muscle and elastic fibers. This layer is thicker in arteries and thinner in veins.
- Inner. The inner layer of the blood vessel wall is called tunica intima. This layer is made of elastic fiber and collagen. Its consistency varies based on the type of blood vessel.
Unlike arteries, veins contain valves. Veins need valves to keep the blood flowing toward the heart. Theses valves are particularly important in the legs and arms. They fight gravity to prevent the backflow of blood.
Arteries dont need valves because the pressure from the heart keeps the blood flowing through them in one direction.
Mechanisms To Return Blood
The return of blood to the heart is assisted by the action of the skeletal-muscle pump and by the thoracic pump action of breathing during respiration. As muscles move, they squeeze the veins that run through them. Veins contain a series of one-way valves. As the vein is squeezed, it pushes blood through the valves, which then close to prevent backflow. Standing or sitting for prolonged periods can cause low venous return from venous pooling. In venous pooling, the smooth muscles surrounding the veins become slack and the veins fill with the majority of the blood in the body, keeping blood away from the brain, which can cause unconsciousness.
Venous valve: Venous valves prevent back flow and ensure that blood flows in one direction.
Although most veins take blood back to the heart, portal veins carry blood between capillary beds. For example, the hepatic portal vein takes blood from the capillary beds in the digestive tract and transports it to the capillary beds in the liver. The blood is then drained in the gastrointestinal tract and spleen, where it is taken up by the hepatic veins and blood is taken back into the heart. Since this is an important function in mammals, damage to the hepatic portal vein can be dangerous. Blood clotting in the hepatic portal vein can cause portal hypertension, which results in a decrease of blood fluid to the liver.
Also Check: Does Tylenol Increase Heart Rate
Classification & Structure Of Blood Vessels
Blood vessels are the channels or conduits through which blood is distributed to body tissues. The vessels make up two closed systems of tubes that begin and end at the heart. One system, the pulmonary vessels, transports blood from the right ventricle to the lungs and back to the left atrium. The other system, the systemic vessels, carries blood from the left ventricle to the tissues in all parts of the body and then returns the blood to the right atrium. Based on their structure and function, blood vessels are classified as either arteries, capillaries, or veins.
Summary: Distribution Of Blood Flow
The following list breaks down the blood flow throughout the body:
- Systemic circulation 84%
When blood flow needs to be redistributed to other portions of the body, the vasomotor center located in the medulla oblongata sends sympathetic stimulation to the smooth muscles in the walls of the veins, causing constrictionor in this case, venoconstriction. Less dramatic than the vasoconstriction seen in smaller arteries and arterioles, venoconstriction may be likened to a stiffening of the vessel wall. This increases pressure on the blood within the veins, speeding its return to the heart. As you will note in the image above,;approximately 21 percent of the venous blood is located in venous networks within the liver, bone marrow, and integument. This volume of blood is referred to as venous reserve. Through venoconstriction, this reserve volume of blood can get back to the heart more quickly for redistribution to other parts of the circulation.
Recommended Reading: Reflux And Palpitations
Veins Carry Blood Back Toward The Heart
After the capillaries release oxygen and other substances from blood into body tissues, they feed the blood back toward the veins. First the blood enters microscopic vein branches called venules. The venules conduct the blood into the veins, which transport it back to the heart through the venae cavae. Vein walls are thinner and less elastic than artery walls. The pressure pushing blood through them is not as great. In fact, there are valves within the lumen of veins to prevent the backflow of blood.
Oxygenated Blood Flows Away From The Heart Through Arteries
The left ventricle of the heart pumps oxygenated blood into the aorta. From there, blood passes through major arteries, which branch into muscular arteries and then microscopic arterioles. The arterioles branch into the capillary networks that supply tissues with oxygen and nutrients. The walls of arteries are thicker than the walls of veins, with more smooth muscle and elastic tissue. This structure allows arteries to dilate as blood pumps through them.
Read Also: Thrz Calculator
Anatomy Of The Heart And Blood Vessels
Reviewed byDr Jacqueline Payne
The heart is a muscular pump that pushes blood through blood vessels around the body. The heart beats continuously, pumping the equivalent of more than 14,000 litres of blood every day through five;main types of blood vessels: arteries, arterioles, capillaries, venules and veins.
The Venous Return Curve
If right atrial pressure were changed in steps over the entire range of possible atrial pressures and venous return were measured at each point, plotting the data set would yield a complete venous return curve, which is presented in . As mentioned earlier, such measurements would have to be made during total blockade of the autonomic nervous system so that circulatory reflexes would be normal. Notice that, at the normal right atrial pressure value , venous return is 100%, which is 5 L/min in man. Venous return falls progressively as right atrial pressure increases, until right atrial pressure reaches 7 mm Hg, the normal value for mean systemic pressure. At that point, venous return is 0 because the pressure gradient for venous return is 0. As right atrial pressure falls below 0, the venous return curve increases at a progressively declining rate until flow reaches a plateau at approximately 4 mm Hg. As discussed above, the reason for the curvilinear nature in this portion of the relationship, termed the transition zone, is the progressive increase in vascular resistance due to the collapse of increasing numbers of veins as right atrial pressure becomes more negative.
The complete venous return curve over the range of right atrial pressure from 8 to 8 mm Hg. Venous return values are for humans.
Recommended Reading: Can Reflux Cause Heart Palpitations
You May Like: How Does Anemia Cause Heart Failure
Disorders Of The Cardiovascular System: Edema And Varicose Veins
Despite the presence of valves and the contributions of other anatomical and physiological adaptations we will cover shortly, over the course of a day, some blood will inevitably pool, especially in the lower limbs, due to the pull of gravity. Any blood that accumulates in a vein will increase the pressure within it, which can then be reflected back into the smaller veins, venules, and eventually even the capillaries. Increased pressure will promote the flow of fluids out of the capillaries and into the interstitial fluid. The presence of excess tissue fluid around the cells leads to a condition called edema.
Most people experience a daily accumulation of tissue fluid, especially if they spend much of their work life on their feet . However, clinical edema goes beyond normal swelling and requires medical treatment. Edema has many potential causes, including hypertension and heart failure, severe protein deficiency, renal failure, and many others. In order to treat edema, which is a sign rather than a discrete disorder, the underlying cause must be diagnosed and alleviated.
Figure 7. Varicose veins are commonly found in the lower limbs.
The Constant Pumping Of The Heart Maintains Blood Pressure And Supply Throughout The Body
The blood moving through the circulatory system puts pressure on the walls of the blood vessels. Blood pressure results from the blood flow force generated by the pumping heart and the resistance of the blood vessel walls. When the heart contracts, it pumps blood out through the arteries. The blood pushes against the vessel walls and flows faster under this high pressure. When the ventricles relax, the vessel walls push back against the decreased force. Blood flow slows down under this low pressure.
You May Like: Can Too Much Vitamin D Cause Heart Palpitations
What Kind Of Blood Comes Back Into The Heart & Then Goes To The Lungs
The heart consists of four chambers in which blood flows. Blood enters the right atrium and passes through the right ventricle. The right ventricle pumps the blood to the lungs where it becomes oxygenated. The oxygenated blood is brought back to the heart by the pulmonary veins which enter the left atrium.
Walls Of Arteries And Veins
The walls of both arteries and veins have three layers: the tunica intima, tunica media, and tunica adventitia. You can see the three layers for an artery in Figure \.
Also Check: Fitbit Charge 2 Heart Rate Accuracy
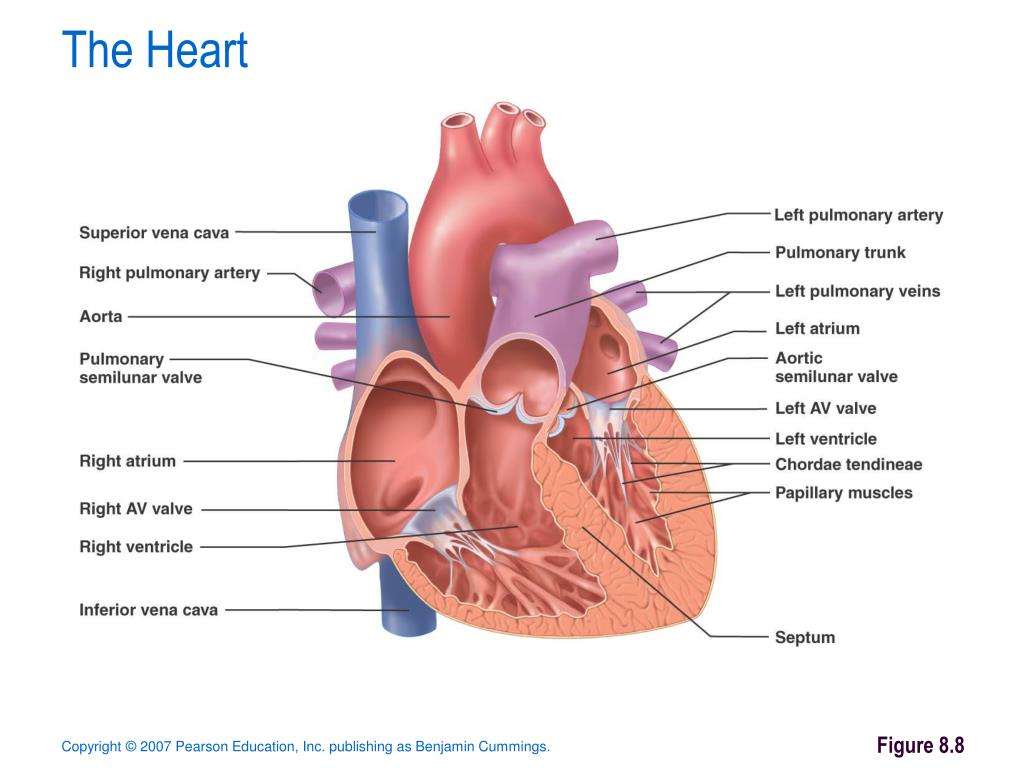
What Are The Parts Of The Heart
The heart has four chambers two on top and two on bottom:
- The two bottom chambers are the right ventricle and the left ventricle. These pump blood out of the heart. A wall called the interventricular septum is between the two ventricles.
- The two top chambers are the right atrium and the left atrium. They receive the blood entering the heart. A wall called the interatrial septum is between the atria.
The atria are separated from the ventricles by the atrioventricular valves:
- The tricuspid valve separates the right atrium from the right ventricle.
- The mitral valve separates the left atrium from the left ventricle.
Two valves also separate the ventricles from the large blood vessels that carry blood leaving the heart:
- The pulmonic valve is between the right ventricle and the pulmonary artery, which carries blood to the lungs.
- The aortic valve is between the left ventricle and the aorta, which carries blood to the body.
How Do The Heart And Blood Vessels Work
The heart works by following a sequence of electrical signals that cause the muscles in the chambers of the heart to contract in a certain order. If these electrical signals change, the heart may not pump as well as it should.
The sequence of each heartbeat is as follows:
- The sinoatrial node in the right atrium is like a tiny in-built ‘timer’. It fires off an electrical impulse at regular intervals. This controls your heart rate. Each impulse spreads across both atria, which causes them to contract. This pumps blood through one-way valves into the ventricles.
- The electrical impulse gets to the atrioventricular node at the lower right atrium. This acts like a ‘junction box’ and the impulse is delayed slightly. Most of the tissue between the atria and ventricles does not conduct the impulse. However, a thin band of conducting fibres called the atrioventricular bundle acts like ‘wires’ and carries the impulse from the AV node to the ventricles.
- The AV bundle splits into two – a right and a left branch. These then split into many tiny fibres which carry the electrical impulse throughout the ventricles. The ventricles contract and pump blood through one-way valves into large arteries:
- The arteries going from the right ventricle take blood to the lungs.
- The arteries going from the left ventricle take blood to the rest of the body.
Don’t Miss: Does Tylenol Increase Heart Rate
Metarterioles And Capillary Beds
A metarteriole is a type of vessel that has structural characteristics of both an arteriole and a capillary. Slightly larger than the typical capillary, the smooth muscle of the tunica media of the metarteriole is not continuous but forms rings of smooth muscle prior to the entrance to the capillaries. Each metarteriole arises from a terminal arteriole and branches to supply blood to a capillary bed that may consist of 10100 capillaries.
Although you might expect blood flow through a capillary bed to be smooth, in reality, it moves with an irregular, pulsating flow. This pattern is called vasomotion and is regulated by chemical signals that are triggered in response to changes in internal conditions, such as oxygen, carbon dioxide, hydrogen ion, and lactic acid levels. For example, during strenuous exercise when oxygen levels decrease and carbon dioxide, hydrogen ion, and lactic acid levels all increase, the capillary beds in skeletal muscle are open, as they would be in the digestive system when nutrients are present in the digestive tract. During sleep or rest periods, vessels in both areas are largely closed; they open only occasionally to allow oxygen and nutrient supplies to travel to the tissues to maintain basic life processes.
