How Do I Manage My Heart Failure
Its important to follow the advice from your doctor and take the medicines youre prescribed. Making changes to your lifestyle is another way to improve your health. Changes you could try are:
- keeping active which has been proven to boost energy and improve sleep and quality of life
- keeping to a healthy weight and diet this will help your overall health and prevent extra strain on your heart
- limiting how much alcohol you drink – lowering your chance of getting abnormal heart rhythms, high blood pressure and diseases such as stroke, liver problems and some cancers
- stopping smoking and using other tobacco products – reducing your risk of developing heart and circulatory diseases
- watching the amount of fluid you have each day if advised by your medical team
- weighing yourself regularly sudden weight gain may mean too much fluid is building up in your body and will need treated.
Living a healthier lifestyle can be hard at first, but its important for your overall quality of life. Visit our healthy living hub to start eating healthier and manage things like smoking and stress today.
Can Heart Failure Be Prevented
You may be able to prevent or delay heart failure if you:
- Work with your provider to manage any health conditions that increase your risk of developing heart failure
- Make healthy changes in your eating, exercise, and other daily habits to help prevent heart disease
NIH: National Heart, Lung, and Blood Institute
Heart Valve Disease Can Be Deadly If Not Treated
Dr. Bargout explains, “If a heart valve has severe stenosis or regurgitation that is left untreated, heart failure can progress leading to significant morbidity, hospitalization or even death. Untreated symptomatic severe aortic valve stenosis is a known cause of sudden death. Recognizing valvular heart disease early on, appropriate follow up with an Echocardiogram and timely intervention are essential in preventing progression where irreversible damage to the heart muscle can occur or even death.”
According to Dr. Sethi, “Untreated valve disease can lead not just to unexpected death but also debilitating symptoms. In cases where there is acute congestive heart failure patients run the risk of needing temporary life support measures such as breathing machines known as ventilators.”
Dr. Sinha says, “Degenerative valvular disease is progressive, and if not treated when it becomes severe, the hemodynamic effects and symptoms will worsen for aortic stenosis and mitral regurgitation. Individuals will have lifestyle limiting symptoms from shortness of breath and fatigue. Eventually, the individual will develop heart failure and die from untreated valvular disease.”
Also Check: How Fatal Are Heart Attacks
How Does Heart Failure Affect The Quality Of Life And Lifestyle
With the right care and treatment plan, many adults still enjoy life even though heart failure limits their activities. How well you feel depends on:
- How well your heart muscle is working.
- How well you respond to your treatment plan.
- How well you follow your treatment plan.
This includes caring for yourself by:
- Taking your medications.
Treatments For Heart Failure
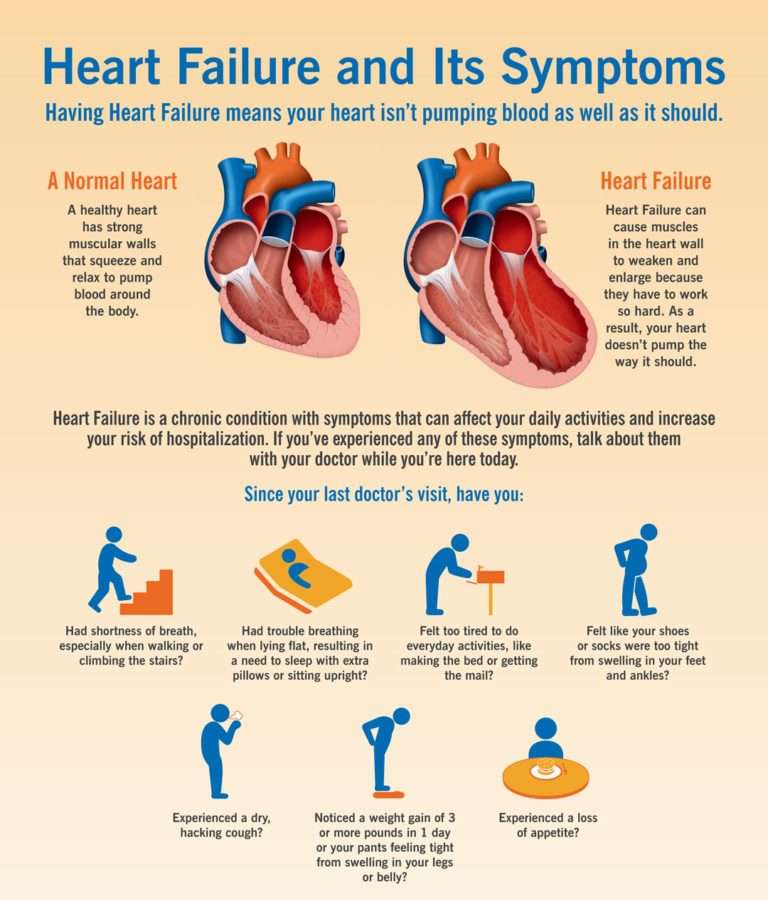
Treatment for heart failure usually aims to control the symptoms for as long as possible and slow down the progression of the condition.
How you’re treated will depend on what is causing your heart failure.
Common treatments include:
- lifestyle changes including eating a healthy diet, exercising regularly and stopping smoking
- medicine a range of medicines can help many people need to take 2 or 3 different types
- devices implanted in your chest these can help control your heart rhythm
- surgery such as a or a heart transplant
Treatment will usually be needed for life.
A cure may be possible when heart failure has a treatable cause. For example, if your heart valves are damaged, replacing or repairing them may cure the condition.
Recommended Reading: How To Improve Ejection Fraction After Heart Attack
When Should I Get Emergency Care
Go to the ER or call 911 if you have:
- New, unexplained, and severe chest pain that comes with shortness of breath, sweating, nausea, or weakness
- Fast heart rate , especially if you are short of breath
- Shortness of breath that doesn’t get better if you rest
- Sudden weakness, or you can’t move your arms or legs
- Sudden, severe headache
- Fainting spells
What Is Heart Failure
Heart failure doesnât mean the heart has stopped working. Rather, it means that the heart works less efficiently than normal. Due to various possible causes, blood moves through the heart and body at a slower rate, and pressure in the heart increases. As a result, the heart canât pump enough oxygen and nutrients to meet the body’s needs.
The chambers of the heart may respond by stretching to hold more blood to pump through the body or by becoming stiff and thickened. This helps to keep the blood moving, but the heart muscle walls may eventually weaken and become unable to pump as efficiently. The kidneys may respond by causing the body to retain fluid and salt. If fluid builds up in the arms, legs, ankles, feet, lungs, or other organs, the body becomes congested. Congestive heart failure is the term used to describe the condition.
You May Like: Did John Legend Have Heart Surgery
What Are The Signs And Symptoms Of Congestive Heart Failure
Shortness of breath
The hallmark and most common symptom of left heart failure is shortness of breath and may occur:
Chest Pain
Right heart failure, left heart failure, or both
Causes Of Low Blood Pressure
Low blood pressure typically results from one or more of the following:
-
Dilation of small arteries
Dilation of arterioles can be caused by
-
Spinal cord injuries, in which the nerves that cause the arterioles to constrict are impaired
Low blood pressure also occurs when the nerves that conduct signals between the brain and the heart and blood vessels are impaired by neurologic disorders called autonomic neuropathies Autonomic Neuropathies Autonomic neuropathies are disorders affecting the peripheral nerves that automatically regulate body processes . Causes include diabetes, amyloidosis⦠read more .
When a person quickly moves from a sitting position to a standing position, blood pressure in the blood vessels to the brain decreases, resulting in a temporary sensation of light-headedness or faintness. This is called orthostatic hypotension Dizziness or Light-Headedness When Standing Up In some people, particularly older people, blood pressure drops excessively when they sit or stand up . Symptoms of faintness, light-headedness⦠read more . It can be more pronounced in people who are dehydrated or warm , have certain illnesses, or have been lying down or sitting for prolonged periods of time. Orthostatic hypotension can even cause people to faint. In most people, the body quickly acts to increase blood pressure and prevent the person from fainting.
Recommended Reading: How To Measure Your Heart Rate
Don’t Miss: Meds For Heart Failure
Heart Failure With Preserved Ejection Fraction
Just under half of people with heart failure have a preserved left ventricular ejection fraction . This means that your heart is contracting well but the heart muscle is stiff so the left ventricle does not relax properly between beats. Heart failure with a preserved ejection fraction is particularly common in people with high blood pressure, and those with raised cholesterol, diabetes, obstructive sleep apnea, and in those who smoke.
How Can I Prevent Heart Failure
You can prevent heart failure by preventing coronary heart disease and heart attack. The best way to do this is to reduce or eliminate the risk factors that lead to heart failure. You could:
- drink alcohol in moderation
- reduce stress and look after your mental wellbeing
If you have had a heart attack, its even more important to manage your risk factors and follow your treatment plan. Make sure you check in frequently with your healthcare team.
Some risk factors such as your age, whether you have other health conditions, or your genes may be outside your control. Speak with your doctor if you have concerns about developing heart failure, and how you can manage it.
You May Like: Lung Problems After Open Heart Surgery
What Causes Heart Failure
Heart failure is caused by many conditions that damage the heart muscle, including:
- Coronary artery disease.Coronary artery disease , a disease of the arteries that supply blood and oxygen to the heart, causes decreased blood flow to the heart muscle. If the arteries become blocked or severely narrowed, the heart becomes starved for oxygen and nutrients.
- Heart attack. A heart attack happens when a coronary artery becomes suddenly blocked, stopping the flow of blood to the heart muscle. A heart attack damages the heart muscle, resulting in a scarred area that doesnât work the way it should.
- Cardiomyopathy. Damage to the heart muscle from causes other than artery or blood flow problems, such as from infections or alcohol or drug abuse.
- Conditions that overwork the heart. Conditions including high blood pressure, valve disease, thyroid disease, kidney disease, diabetes, or heart defects present at birth can all cause heart failure. In addition, heart failure can happen when several diseases or conditions are present at once.
What To Know About Heart Valve Disease
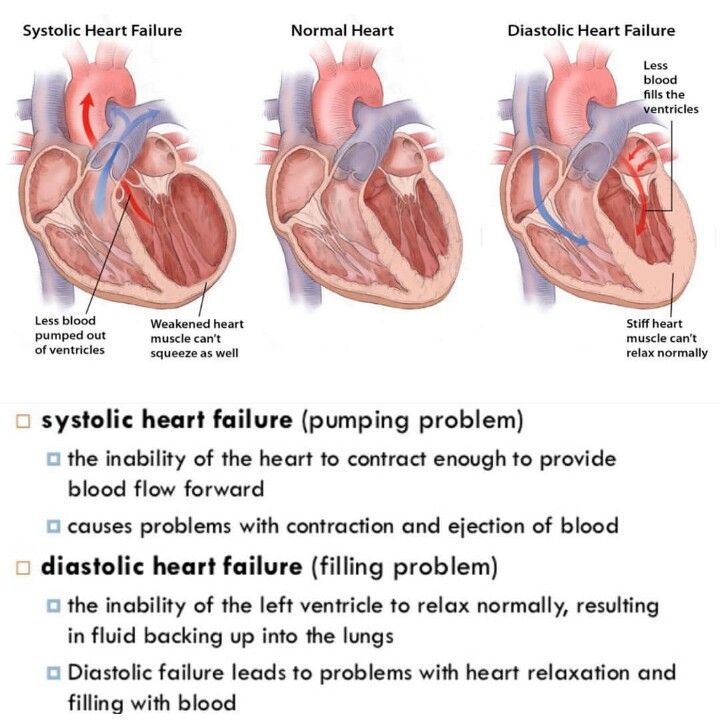
Raed Bargout, MD, Chief of Cardiovascular Disease at Dignity Health Glendale Memorial Hospital says, “The heart is a muscle, the size of a hand fist composed of four chambers pumping blood in both the Aorta and pulmonary artery. Heart valves separate those four chambers and hence there are four valves, The Aortic, Mitral, Tricuspid and pulmonic valve. Valves function to control and regulate blood flowing from one chamber to the other. Healthy heart valves are able to fully open and close during the cardiac cycle while diseased valves might not fully open or fully close and hence leads to a variety of symptoms and diseases.”
Dr. Sinha explains, “The heart has four chambers and four valves. On the right side of the heart , there is the tricuspid and pulmonic valve. On the left side , there is the mitral valve and aortic valve. There is a wide variety of valvular disease, and it is difficult to summarize all of them in a short amount of time. For simplicity, valvular disease can be broadly categorized into two forms: 1. Stenosis which is when blood has difficulty passing through a valve usually because of thickening of the valve leaflets and 2. Regurgitation when the valve leaflets do not shut tightly and blood leaks backwards into the preceding chamber. Valvular disease typically would not have a hemodynamic effect and causes symptoms unless it becomes severe.
Recommended Reading: Why Do Av Nodal Cells Not Determine The Heart Rate
Blood Pressure And Heart Failure Prevention
Two issues arise regarding HF when treating HTN. The first is strictly controlling high BP to prevent structural remodeling and the development of HF. The presence of a J-curve association between BP and CV outcomes have been long debated, but evidence has been controversial . The current consensus is that strict control is mostly beneficial for hypertensive patients with low CV risk, while the risk of CV outcome increases in patients with high risk for coronary heart disease . Recently, the findings from the Systolic Blood Pressure Intervention Trial , which assessed the role of intensive HTN treatment on a composite outcome that included HF, showed that a target SBP< 120mmHg was associated with a 38% relative risk reduction in HF . BP lowering in patients with ventricular hypertrophy can delay further remodeling and reduce the incidence of HF . The LV hypertrophy induced by HTN is not unidirectional, and a regression of LV mass has been observed after the pharmacological treatment of elevated BP . Improvements in LV hypertrophy have also been associated with reduced risks of CV events, including CV death, myocardial infarction, and stroke .
Stage A Treatment Options
Treatment options in stage A mainly focus on promoting your overall health and disease prevention. If you meet the stage A criteria, your doctor will recommend lifestyle changes to slow or stop disease progression.
Heart Failure Doctor Discussion Guide
Recommended Reading: Good Heart Rate Woman
Strengths And Limitations Of This Study
-
We have analysed hypotension incidence and risk factors in a large real-world cohort of patients with incident heart failure in UK primary care.
-
Data are from The Health Improvement Network database, which has been extensively validated for use in pharmacoepidemiology.
-
Since blood pressure is not systematically tested in routine clinical practice, we cannot rule out some detection bias.
-
Due to the nature of data collection during routine clinical practice, we were unable to identify reliably the subgroup of cases with orthostatic hypotension, it was unclear if diagnoses of heart failure were made according to guidelines, and data on heart failure severity and ejection fraction were not complete for all patients.
Stage B Treatment Options
While stage A CHF is managed with lifestyle changes, the treatment plan for stage B typically includes taking medications regularly. People at this stage should still make the same lifestyle changes as those appropriate for stage A. However, your doctor may also prescribe additional treatments such as:
- Angiotensin-converting enzyme inhibitors or angiotensin II receptor blockers, if you arent taking any as part of your stage A treatment plan
- Beta blockers if youve had a heart attack and your EF is 40% or lower, if you arent taking any as part of your stage A treatment plan
- Possible surgery or intervention as a treatment for coronary artery blockage, heart attack, valve disease, or congenital heart disease
Read Also: Recovering From Open Heart Surgery
The Ticker Tapes Podcast
Anne Dixon’s life changed after discovering she had a problem with her heart when she was a student. After an operation, she went back to her normal life, but there was more in store for her. Hear her story and other real experiences from people living with her and circulatory diseases.
What Is An Ejection Fraction
An ejection fraction is a measurement of the blood pumped out of your heart with each beat, expressed in a percentage. It can be measured using an echocardiogram , multigated acquisition scan, nuclear stress test, magnetic resonance imaging , or during a cardiac catheterization. A normal ejection fraction is between 50% and 70%.
Read Also: Fat Burning Heart Rate Chart
What Is Cardiac Arrest
Cardiac arrest results from electrical disturbances that cause the heart to suddenly stop beating properly.
In cardiac arrest, death can result quickly if steps aren’t taken immediately. “Cardiac arrest may be reversed if CPR is performed and a defibrillator shocks the heart and restores a normal heart rhythm within a few minutes,” according to the American Heart Association.
More than 350,000 cardiac arrests occur outside a hospital in the United States each year, the AHA said.
A sudden, unexpected loss of heart function also results in a sudden loss of breathing and consciousness.
Cardiac arrest is not the same as a heart attack, although almost any known heart condition, including heart attack, can cause cardiac arrest.
Another emergency that can lead to cardiac arrest, commotio cordis, is a disruption of heart rhythm after a blow to the area directly over the heart at a key time during a heartbeat cycle.
It’s rare, but it mostly occurs in boys and young men during sports. The American Heart Association says it’s the leading cause of deaths in youth baseball in the United States, typically two to three per year. Automated external defibrillators have helped increase the survival rate.
Stages Of Heart Failure
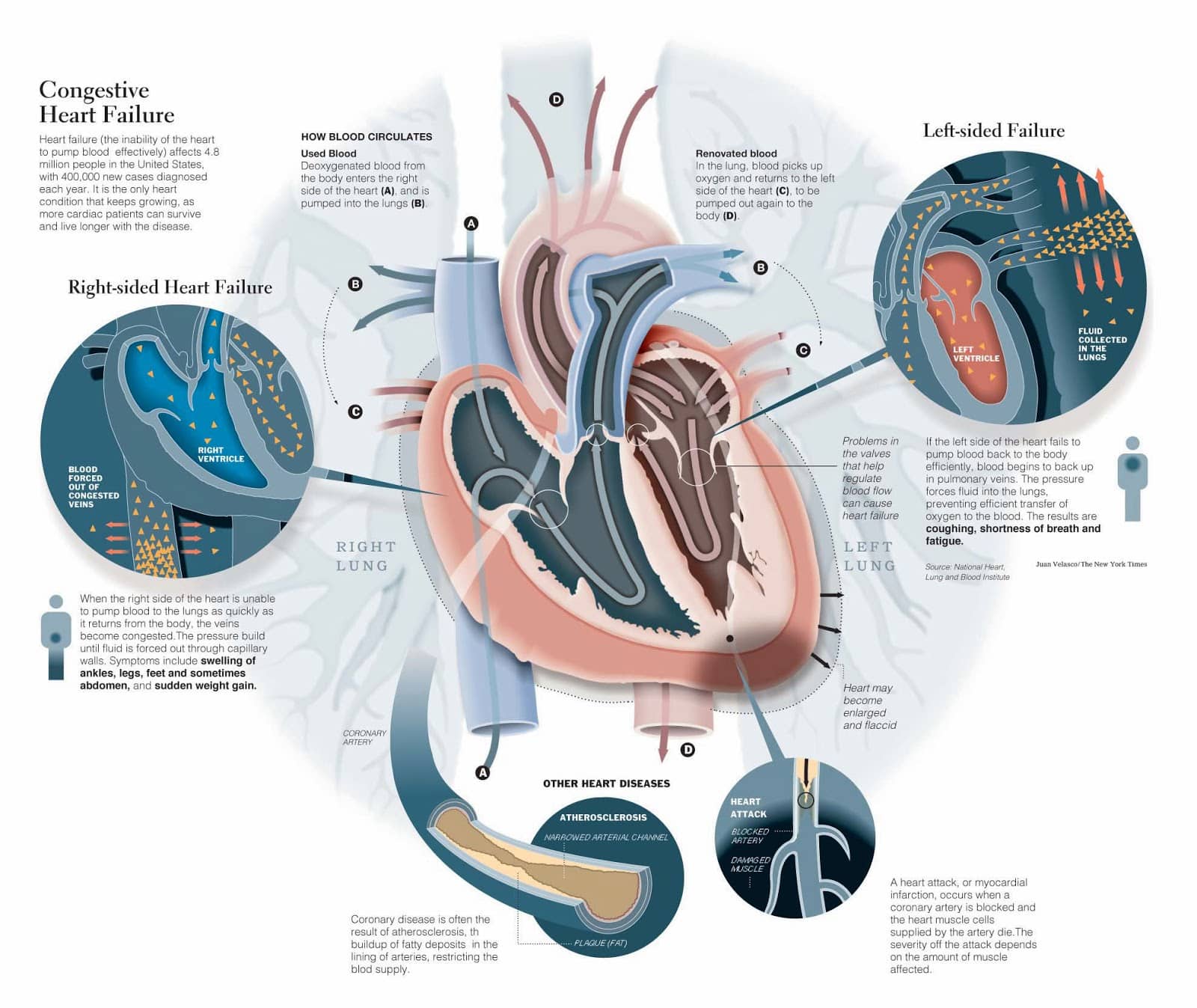
In 2001, the American Heart Association and American College of Cardiology described the “Stages of Heart Failure.” These stages, which were updated in 2005, will help you understand that heart failure is often a progressive condition and can worsen over time. They will also help you understand why a new medication was added to your treatment plan and may help you understand why lifestyle changes and other treatments are needed.
The stages classified by the AHA and ACC are different than the New York Heart Association clinical classifications of heart failure that rank patients as class I-II-III-IV, according to the degree of symptoms or functional limits. Ask your doctor what stage of heart failure you are in.
Check the table below to see if your therapy matches what the AHA and ACC recommend. Note that you cannot go backward in stage, only forward.
The table below outlines a basic plan of care that may or may not apply to you, based on the cause of your heart failure and your special needs. Ask your doctor to explain therapies that are listed if you do not understand why you are or are not receiving them.
The New York Heart Association clinical classifications of heart failure rank people as class I-II-III-IV, according to the degree of symptoms or functional limits. You can ask your doctor if you want to know what stage of heart failure youâre in.
Also Check: What Is An Average Resting Heart Rate
