How Is Congestive Heart Failure Diagnosed
Congestive heart failure happens when the heart muscles are pumping inefficiently due to fluid buildup around the heart. Its best to get tested, especially if you are at high risk for the condition or have a family history of it. Coronary artery disease, high blood pressure, and a history of heart attacks are all signs that you may be at a higher risk for congestive heart failure. If you smoke, drink excessively, have diabetes, or kidney disease, you are also at a higher risk.
Heart failure doesnt necessarily happen suddenly. It can be chronic, in which case you wont necessarily know whats going on unless you monitor yourself for signs and symptoms. These include:
- Shortness of breath, even when resting
- Reduced ability to exercise, perform regular chores, and move around
- A rapid or irregular heartbeat
- Persistent coughing or wheezing
- Weight gain as a result from fluid retention
- Chest pain
If you notice these symptoms, see a doctor immediately. You will need to get examined and tested for the possible underlying cause of your symptoms. So, how is congestive heart failure diagnosed? Here are a few examples of the tests a doctor can perform to diagnose you. You will not need all of them to get diagnosed. Your doctor will determine which combination of tests are best to get accurate results.
The Earliest Symptoms Of Heart Failure Are Often Very Subtle But It’s Dangerous To Ignore Them
It’s an unfortunate truth that your body slows down in your sixth and seventh decades. Climbing a flight of stairs that you once took two at a time can now feel as daunting as scaling Mount Everest. While some degree of vitality loss can be attributed to natural aging, fatigue and breathlessness may also be signals that your heart is not functioning as well as it should. “There is a general tendency for people to ignore heart failure symptoms and attribute them to just getting older. Therefore, it was very important for us to create an easy way to identify those symptoms,” says Dr. Mandeep R. Mehra, medical director of the Heart and Vascular Center at Harvard-affiliated Brigham and Women’s Hospital.
FACES of heart failure
Heart failure occurs when something damages the heart muscle or reduces the heart’s ability to pump effectively. Most often, the damage stems from coronary artery disease or heart attack. But faulty heart valves, longstanding high blood pressure, or genetic disease may also be to blame. No matter what the cause, the failing heart can no longer pump well enough to keep up with the body’s demand for oxygen-rich blood.
To help both doctors and patients quickly spot a possible combination of heart failure symptoms, the Heart Failure Society of America developed a handy tool that goes by the acronym FACES.
F = Fatigue. When the heart can’t pump enough oxygen-rich blood to meet the body’s energy needs, a general feeling of tiredness or fatigue sets in.
How Can I Improve My Quality Of Life With Heart Failure
There are several things you can do to improve your quality of life if you have heart failure. Among them:
- Eat a healthy diet. Limit your consumption of sodium to less than 1,500 milligrams each day. Eat foods high in fiber. Limit foods high in trans fat, cholesterol, and sugar. Reduce total daily intake of calories to lose weight if necessary.
- Exercise regularly. A regular cardiovascular exercise program, prescribed by your doctor, will help improve your strength and make you feel better. It may also decrease heart failure progression.
- Don’t overdo it. Plan your activities and include rest periods during the day. Certain activities, such as pushing or pulling heavy objects and shoveling may worsen heart failure and its symptoms.
- Prevent respiratory infections. Ask your doctor about flu and pneumonia vaccines.
- Take your medications as prescribed. Do not stop taking them without first contacting your doctor.
- Get emotional or psychological support if needed. Heart failure can be difficult for your whole family. If you have questions, ask your doctor or nurse. If you need emotional support, social workers, psychologists, clergy, and heart failure support groups are a phone call away. Ask your doctor or nurse to point you in the right direction.
Recommended Reading: Does Acetaminophen Increase Blood Pressure
What Is Congestive Heart Failure
Heart failure describes the inability or failure of the heart to meet the needs of organs and tissues for oxygen and nutrients. This decrease in cardiac output, the amount of blood that the heart pumps, is not adequate to circulate the blood returning to the heart from the body and lungs, causing the fluid to leak from capillary blood vessels. This leads to symptoms that may include shortness of breath, weakness, and swelling.
Understanding blood flow in the heart and body
The right side of the heart pumps blood to the lungs while the left side pumps blood to the rest of the body. Blood from the body enters the right atrium through the vena cava. It then flows into the right ventricle where it is pumped to the lungs through the pulmonary artery, which carries deoxygenated blood to the lungs. In the lungs, oxygen is loaded onto red blood cells and returns to the left atrium of the heart via the pulmonary veins. Blood then flows into the left ventricle where it is pumped to the organs and tissues of the body. Oxygen is downloaded from red blood cells into the various organs while carbon dioxide, a waste product of metabolism, is added to be removed in the lungs. Blood then returns to the right atrium to start the cycle again. The pulmonary veins are unusual in that they carry oxygenated blood, while the pulmonary artery carries deoxygenated blood. This is a reversal of duties versus the roles of veins and arteries in the rest of the body.
How Do You Get Congestive Heart Failure
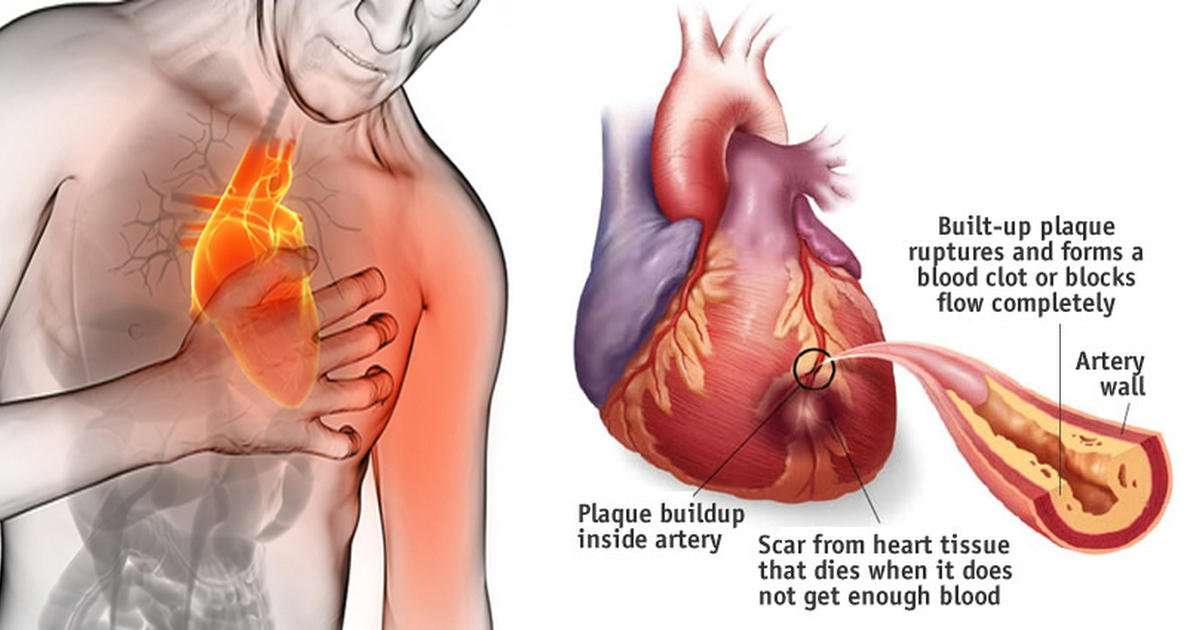
One of the key roles of the human heart is to pump blood throughout the body. Congestive heart failure is a condition in which the heart does not pump enough blood to meet the needs of our body. Before we try to understand what congestive heart failure really is, lets see how the heart handles blood circulation:
Don’t Miss: Dehydration Increased Heart Rate
Atrial Natriuretic Peptide And B
ANP and BNP are endogenously generated peptides activated in response to atrial and ventricular volume/pressure expansion. ANP and BNP are released from the atria and ventricles, respectively, and both promote vasodilation and natriuresis. Their hemodynamic effects are mediated by decreases in ventricular filling pressures, owing to reductions in cardiac preload and afterload. BNP, in particular, produces selective afferent arteriolar vasodilation and inhibits sodium reabsorption in the proximal convoluted tubule. It also inhibits renin and aldosterone release and, therefore, adrenergic activation. ANP and BNP are elevated in chronic heart failure. BNP especially has potentially important diagnostic, therapeutic, and prognostic implications.
For more information, see the Medscape Drugs & Diseases article Natriuretic Peptides in Congestive Heart Failure.
Understanding Congestive Heart Failure
A classification system devised by the American College of Cardiology and the American Heart Association categorizes congestive heart failure patients into four stages, from A to D .
At the earliest stage, someone may not even notice their heart failure, or it may seem to disappear once they start taking medication. Their heart failure might never progress past this point, especially if they take good care of themself. Or at later stages, they may have difficulty with everyday activities, like walking up stairs or carrying groceries. They may feel more fatigued than usual because their cells arent getting the nutrients they need. Fluid in their lungs can cause shortness of breath especially when lying down or it might accumulate in the legs or ankles, causing painful swelling.
Read Also: How Fast Should Your Heart Rate Be
When To Get Medical Advice
See a GP if you experience persistent or gradually worsening symptoms of heart failure.
Call 999 for an ambulance or go to your nearest A& E department as soon as possible if you have sudden or very severe symptoms.
A number of tests can be used to help check how well your heart is working, including blood tests, an ECG and an echocardiogram.
Manage Depression And Anxiety
Depression and anxiety are common in people with congestive heart failure. Feeling unwell, being unable to do some of the things they once enjoyed, and uncertainty about the future can all contribute to feelings of sadness. But if the person youre caring for seems consistently unhappy, they may be depressed. Look out for these signs of depression, and if you notice any, notify their doctor:
- Frequent crying episodes
- Feelings of hopelessness or worthlessness
- Poor appetite or increased appetite
- Sleeping too much or not enough
- Increased agitation and restlessness
- Loss of interest in life
- Expressing thoughts of dying or suicide
Depression is a serious problem that requires evaluation and treatment. But you may be able to help manage your loved ones moods with these activities:
Don’t Miss: Damaged Left Ventricle
What You Can Do For Your Loved One
In addition to symptom management, its important for the family caregiver to learn how to recognize the end-of-life signs for CHF, and when they should contact hospice. Hospice care will be able to address the specific needs of CHF patients in their final days, and help them to get the most out of what time they have left.
Make The Most Of Doctors Appointments
Most patients have a lot of visits to different doctors. To get the most out of appointments, bring a notebook. One of the most important aspects of managing congestive heart failure is keeping track of symptoms, medication side effects, and other concerns. Writing down this information in a notebook will help you and the person in your care stay on top of any changes in their condition.
Other tips to get the most out of appointments include:
- Prepare a list of questions before each visit. Leave spaces for the answers.
- Take notes during the appointment. If either of you doesnt understand something, dont be afraid to ask for an explanation.
- If the person youre caring for isnt following treatment or lifestyle recommendations, make sure the doctor knows it. Trying to protect them isnt in their best interest.
- Do your best to understand all the doctors instructions before you leave, but dont hesitate to call the office if you have questions later.
Read Also: Tylenol Increase Blood Pressure
Tips For Managing Congestive Heart Failure End
You may be asking, How can I provide comfort to my loved one as they experience the end-of-life signs of congestive heart failure? Its only natural that you as a loved one and/or caregiver will want to be as helpful as possible, and ensure that your loved one is experiencing as little pain as possible. Heres some ways you can help:
- Communicate with the doctors and healthcare professionals: Your loved one may be too weak, or simply forget, to communicate their symptoms to the doctors and nurses. You can help by sharing this information with them in order to make sure your loved one gets what they need.
- Provide comfort: Sometimes it is just as simple as spending time with your loved one while watching a TV show, or talking about things they love. These conversations can help in alleviating some of their depression and anxiety.
- Help them remember to take their medicine: There will likely be various pills and medications that your loved one needs to take. You can help by assisting your loved one in staying on schedule.
What Are The Symptoms Of Heart Disease

Sometimes heart disease may be silent and not diagnosed until a person experiences signs or symptoms of a heart attack, heart failure, or an arrhythmia. When these events happen, symptoms may include1
- Heart attack: Chest pain or discomfort, upper back or neck pain, indigestion, heartburn, nausea or vomiting, extreme fatigue, upper body discomfort, dizziness, and shortness of breath.
- Arrhythmia: Fluttering feelings in the chest .
- Heart failure: Shortness of breath, fatigue, or swelling of the feet, ankles, legs, abdomen, or neck veins.
Learn the Facts About Heart Disease
- About 659,000 people in the United States die from heart disease each yearthats 1 in every 4 deaths.1,2
Also Check: Tylenol Effect On Blood Pressure
What Are The Symptoms Of End
Heart Failure: Quick Facts
1. More than 6 million U.S. adults have heart failure.
2. About half of people who develop heart failure die within 5 years of diagnosis.
3. Most people with end-stage heart failure have a life expectancy of less than 1 year.
4. The leading causes of heart failure are diseases that damage the heart, such as heart disease, high blood pressure, and diabetes.
Heart failure worsens over time, so symptoms are most severe during the final stages. It causes fluid to build up in the body, which produces many of these symptoms:
- Shortness of breath . In the final stages of heart failure, people feel breathless both during activity and at rest.
- Persistent coughing or wheezing. This may produce white or pink mucus. The cough may be worse at night or when lying down.
- Weight gain or swelling of the feet, ankles, legs, abdomen, or neck veins.
- Tiredness, weakness.
In addition, people in the final stages of heart failure may suffer from:
- depression, fear, insomnia, and isolation
- anxiety about their future
- trouble navigating the health care system
Women And Heart Failure
Women are just as likely as men to develop heart failure, but there are some differences:
- Women tend to develop heart failure later in life compared with men.
- Women tend to have heart failure caused by high blood pressure and have a normal EF .
- Women may have more shortness of breath than men do. There are no differences in treatment for men and women with heart failure.
You May Like: Coronary Insufficiency Symptoms
What Makes Yale Medicines Approach To Treating Congestive Heart Failure Unique
We have a very patient-focused team at Yale Medicine, says Dr. Jacoby. Every person seen here, we treat as an individual, rather than offering a simple cookie-cutter treatment plan.
Yale Medicines multidisciplinary team comprises of heart failure cardiologists and cardiac surgeons, dedicated advanced-practice, registered nurses and nurse coordinators, dietitians, exercise physiologists, financial counselors, immunologists specializing in transplants, psychologists, and specialists in palliative care.
In our multidisciplinary approach, we include the patients desires as well as input from the family, Dr. Jacoby says. We develop a plan for social work support and take into account all of their financial and emotional stresses in addition to their physical treatment needs.
What You Can Do
Some risk factors of heart failure, like age, cant be modified. Still, people with CHF can take steps to improve the long-term prognosis. The first thing to do is to be familiar with any family history of heart disease. You’ll also want to learn about all the possible symptoms. Don’t ignore any symptom that you think is cause for concern. Tell your healthcare provider about them right away.
Regular exercise, along with managing any other health issues you may have, can also help to keep CHF under control.
Recommended Reading: Heart Rate Vs Blood Pressure
What Is The Outlook For People With Heart Failure
With the right care, heart failure may not stop you from doing the things you enjoy. Your prognosis or outlook for the future will depend on how well your heart muscle is functioning, your symptoms, and how well you respond to and follow your treatment plan.
Everyone with a long-term illness, such as heart failure, should discuss their desires for extended medical care with their doctor and family. An “advance directive” or “living will” is one way to let everyone know your wishes. A living will expresses your desires about the use of medical treatments to prolong your life. This document is prepared while you are fully competent in case you are unable to make these decisions at a later time.
Show Sources
Diagnostic Tests And Procedures
This animation discusses some of the tests used to diagnose heart failure. These tests may include an electrocardiogram to look at your hearts electrical activity, an echocardiogram to measure how well your heart is working and look at the structure, and a chest X-ray to see if your heart is enlarged or there is fluid in your lungs. Other tests may include blood tests and an exercise, or stress test. .
Blood tests
Your doctor may order to check the levels of certain molecules, such as brain natriuretic peptide . These levels rise during heart failure. Blood tests can also show how well your liver and your kidneys are working.
Tests to measure your ejection fraction
Your doctor may order an echocardiography or other imaging tests to measure your ejection fraction. Your ejection fraction is the percent of the blood in the lower left chamber of your heart that is pumped out of your heart with each heartbeat. Ejection fraction tells your doctor how well your heart pumps. This helps your doctor diagnose the type of heart failure you have and guide your treatment.
- If 40% or less of the blood in your left ventricle is pumped out in one beat, you have heart failure with reduced ejection fraction.
- If 50% or more of the blood in your left ventricle is pumped out in one beat, you have heart failure with preserved ejection fraction.
If your ejection fraction is somewhere in between , you may be diagnosed with heart failure with borderline ejection fraction.
Other tests
You May Like: Esophageal Palpitations
Is There A Treatment For Heart Failure
There are more treatment options available for heart failure than ever before. Tight control over your medications and lifestyle, coupled with careful monitoring, are the first steps. As the condition progresses, doctors specializing in the treatment of heart failure can offer more advanced treatment options.
The goals of treating heart failure are to try to keep it from getting worse , to ease symptoms, and to improve quality of life.
Some common types of medicines used to treat it are:
- ACE inhibitors
- Aldosterone antagonists
- ARBs
- ARNIs
- Selective sinus node inhibitors
- Soluble guanylate cyclase stimulator
Your doctor may also recommend a program called cardiac rehabilitation to help you exercise safely and keep up a heart-healthy lifestyle. It usually includes workouts that are designed just for you, education, and tips to lower your chance of heart trouble, like quitting smoking or changing your diet.
Cardiac rehab also offers emotional support. You can meet people like you who can help you stay on track.
