The Effects Of Exercise On Hrv And Its Regulation By The Ans
To assess HRV changes with exercise we performed Fourier transforms of the inter-beat-intervals on sequences of R-R intervals . Crude inspection of the results in Figure 3B suggests that both exercise groups possess greater spectral densities, and therefore greater HRV, compared to sedentary mice. To quantify the HRV further, the HRV spectral density was integrated over several frequency ranges . The total power of the HRV was calculated as the sum of the LF and HF components. Since the magnitude HRV depends on HR, irrespective of autonomic activity changes , we corrected for differences in basal HR between the groups by multiplying HRV by the HR2 . Figure 3C shows that LF, HF, and TP were not different between swimming and free-wheel running mice but were elevated in the exercised groups compared with sedentary mice. Unless stated otherwise, all subsequent HRV results were corrected for HR.
Vyvanse And The Central Nervous System
Vyvanse works by altering the balance of chemicals in your brain and increasing norepinephrine and dopamine levels. Norepinephrine is a stimulant, and dopamine is a naturally occurring substance that stimulates feelings of pleasure and reward.
If you have ADHD, you may notice an improvement in your attention span. It can also help control hyperactivity and impulsiveness and improve concentration. Its also used off label for treatment resistant depression and narcolepsy. It may improve depression, fatigue, sleepiness and wakefulness.
When used to treat binge-eating disorder, Vyvanse may help you binge less frequently.
Common side effects in the central nervous system include:
- trouble sleeping
- feelings of paranoia
Tell your doctor if you have a history of drug or alcohol abuse. Vyvanse can be habit-forming, especially if you take it for a long time, and it has a potential for abuse. You should not use this medication without a doctors supervision.
If you become dependent on amphetamines, stopping suddenly can cause you to go through withdrawal. Symptoms of withdrawal include:
- shakiness
- inability to sleep
- excessive sweating
Your doctor can help you lower the dose a little at a time so you can safely stop taking the drug.
Some children may experience a slightly slower rate of growth while taking this medication. Its not usually cause for concern, but your doctor will probably monitor your childs development as a precaution.
Vyvanse And The Circulatory And Respiratory Systems
One of the more common cardiovascular system side effects is a slightly faster heart rate. You may also have a substantial elevation in heart rate or blood pressure, but this is less common. It can also cause cardiac arrhythmias.
Vyvanse can also cause problems with circulation. You may have circulation problems if your fingers and toes feel cold or numb, or if your skin turns blue or red. If that happens, tell your doctor.
Rarely, Vyvanse can cause shortness of breath.
Vyvanse can affect your digestive system. Some of the more common digestive system problems include:
- dry mouth
Don’t Miss: Can Too Much Vitamin D Cause Heart Palpitations
Multiple Sclerosis Has Close Association With Increased Risks Of Heart Failure And Stroke
A few of the research studies have revealed that multiple sclerosis has close association with increased risk related to admission of patients in hospital for heart attack, stroke and heart failure, which suggest that early diagnosis of various cardiovascular impairments is essential to come with the required preventative care in them.
History Of Slow Breathing
The act of controlling ones breath for the purpose of restoring or enhancing ones health has been practiced for thousands of years amongst Eastern cultures. For example, yogic breathing is a well-known ancient practice of controlled breathing, often performed in conjunction with meditation or yoga, for its spiritual and perceived health-enhancing effects . Various forms of pranayama exist, such as nostril breathing , abdominal breathing, forceful breathing and vocalised breathing, which are performed at varying rates and depths . Yoga, and hence pranayama, was first introduced to the West in the late 1800s and its popularity rose in the mid-1900s. Breathing techniques have since become increasingly popular due to a rising interest in holistic and wellness approaches to healthcare. Their claimed health benefits and potential to treat a range of medical conditions has piqued the interest of the medical and scientific communities, and stimulated research into the area.
You May Like: Can Acid Reflux Cause Heart Palpitations
The Effects Of Exercise On Hr And Its Control By The Ans
To examine whether the HR reductions with exercise were associated with ANS remodeling, surface ECGs were recorded in anesthetized mice in the presence and absence of pharmacological blockers of SNA , PNA , or both. Although our analyses compared HRs between the groups, our conclusions were the same when R-R intervals were compared. Consistent with the echocardiographic recordings , Figure 1 shows that baseline HRs were lower by similar amounts in swim and free-wheel exercised mice, compared to sedentary mice . Following PNA blockade, HR increased in sedentary and both exercise groups , with the relative HR increase being greater in both swim- and free wheel-exercised mice compared to sedentary mice . Subsequent SNA blockade with propranolol, in the continued presence of atropine, led to reductions in HR in all three groups with the relative HR reduction being less in exercised than sedentary mice . After complete autonomic blockade , HRs did not differ between exercised and sedentary mice. This interpretation is further supported by the observation that the beating rates in isolated hearts did not differ between groups .
Why Check Heart Rate Variability
- It can identify ANS imbalances. When your system is in fight-or-flight mode, the difference between heartbeats is low as compared to when you are in a relaxed mode where the difference between the heartbeats is high.
- HRV can detect stress levels. People with low HRV can easily experience acute stress while people with high HRV rarely experience stress and their cardiovascular system is in great shape. Checking your HRV can help you understand how to respond to stress in a healthier way.
- May increase awareness of your lifestyle habits. Checking your HRV is one way you can know if your lifestyle habits are healthy or unhealthy for your heart and a great tool to motivate behavioral change.
- It can detect your reaction to the environment, and emotions. Your nervous system can tell you how you are reacting to your environment, feelings, and emotions when you track your HRV.
- Can increase your self-awareness. HRV measurements can help increase your awareness of how you live and think, and how your behavior affects your nervous system and bodily functions.
Recommended Reading: Acid Reflux Cause Palpitations
The Heart As A Hormonal Gland
In addition to its extensive neurological interactions, the heart also communicates with the brain and body biochemically by way of the hormones it produces. Although not typically thought of as an endocrine gland, the heart actually manufactures and secretes a number of hormones and neurotransmitters that have a wide-ranging impact on the body as a whole.
The heart was reclassified as part of the hormonal system in 1983, when a new hormone produced and secreted by the atria of the heart was discovered. This hormone has been called by several different names atrial natriuretic factor , atrial natriuretic peptide and atrial peptide. Nicknamed the balance hormone, it plays an important role in fluid and electrolyte balance and helps regulate the blood vessels, kidneys, adrenal glands and many regulatory centers in the brain. Increased atrial peptide inhibits the release of stress hormones, reduces sympathetic outflow and appears to interact with the immune system. Even more intriguing, experiments suggest atrial peptide can influence motivation and behavior.
Chapters:
Role Of Cardiac Pacemaker
The sinus node is called the cardiac pacemaker as it regulates cardiac contractility and thus, the heart rate. The sinus node is a small ellipsoidal strip of specialized cardiac muscles located in the superior corner of the right atrium.
The cells in the sinus node have automatic electrical rhythmicity. Certain sodium channels are present in these cells that allow the slow diffusion of sodium ions from the extracellular environment into the cells. This inflow of sodium ions causes depolarization in the absence of any electrical stimulus.
The rhythmic cardiac impulses generated in the sinus node are spread to the rest of the cardiac muscles via the conduction system. The rate of impulse generation in the sinus node controls the heart rate. This automatic rhythmicity of the sinus node is controlled by the innervation from the sympathetic and parasympathetic nervous systems.
Recommended Reading: Does Acid Reflux Cause Heart Palpitations
Young Versus Elder Subjects
Comparison between the HR parameter estimates in the YOUNG and ELDER groups showed that healthy older subjects at rest had increased myocardial electrical resistance coefficient , decreased PNS-SNS activity coefficient , a near zero average value of myocardial metabolism leading primarily to a near zero HR slope indicator , and an ultradepressed standard deviation of myocardial metabolism leading primarily to decreased HR amplitude indicator . These results suggested that aging was related to increased myocardial electrical resistance, decreased PNS-SNS activity , and ultradepressed basal metabolism.
The ELDER parameter alterations suggested that ultradepressed basal metabolic rate related to decreased HRV with aging , because decreased PNS-SNS activity led to increased HRV, rather than decreased HRV , according to the HRV amplitude indicator .
Why Does Our Heart Beat Rate Rise When We Get Frightened
D. Janavi, Chennai
Our body responds to stress, worry, anxiety, fear and excitement by activating the fight or flight system. At chemical level, our body releases a series of hormones that makes us hyper-alert, focused, and energised, and this chemical cascade causes increased heart rate, respiratory rate, and perspiration.
From an evolutionary standpoint, this is a system we needed in place for survival.
When a danger is encountered, our brain just sends signals to our entire body warning us that we need to leave the life-threatening situation. The hormones then create adrenaline that will keep us awake and alive while we are fighting or fleeing. Our cells too contribute by keeping everything working and pumping and so that adrenaline can pump through our blood. While the adrenaline is pumping through our blood, so are the fat and sugar. That fat and sugar make our bronchi open wider causing heart beat and breathing rate to accelerate. That is why our heart beats faster when we get frightened.
Normally, heart-rate control is a balance between the two circuits of the Autonomic Nervous System the Parasympathetic Nervous System and the Sympathetic Nervous System. The Sympathetic Nervous System is often referred to as our fight or flight system. The Parasympathetic Nervous System is its counterpart, and can be termed as the rest and digest system. Together, the PSNS and SNS work in all areas of the body to help us act, react, recover and survive.
Read Also: How Much Blood Does The Heart Pump
Examples Of Parasympathetic Responses
An easy acronym to remember how and where the PSNS works is SLUDD. This stands for:
- Salivation: As part of its rest-and-digest function, the PSNS stimulates production of saliva, which contains enzymes to help your food digest.
- Lacrimation: Lacrimation is a fancy word for making tears. Tears keep your eyes lubricated, preserving their delicate tissues.
- Urination: The PSNS contracts the bladder, which squeezes it so urine can come out.
- Digestion: The PSNS stimulates the release of saliva to promote digestion. It also enacts peristalsis, or the movement of the stomach and intestines, to digest food as well as release bile for the body to digest fats.
- Defecation: The PSNS constricts the sphincters in the intestine and moves digested food material down the digestive tract so a person can have a bowel movement.
Keeping these things in mind, you can see why doctors may also call the parasympathetic system the feed and breed system.
How Parkinsons Disease Affects The Autonomic Nervous System And The Heart
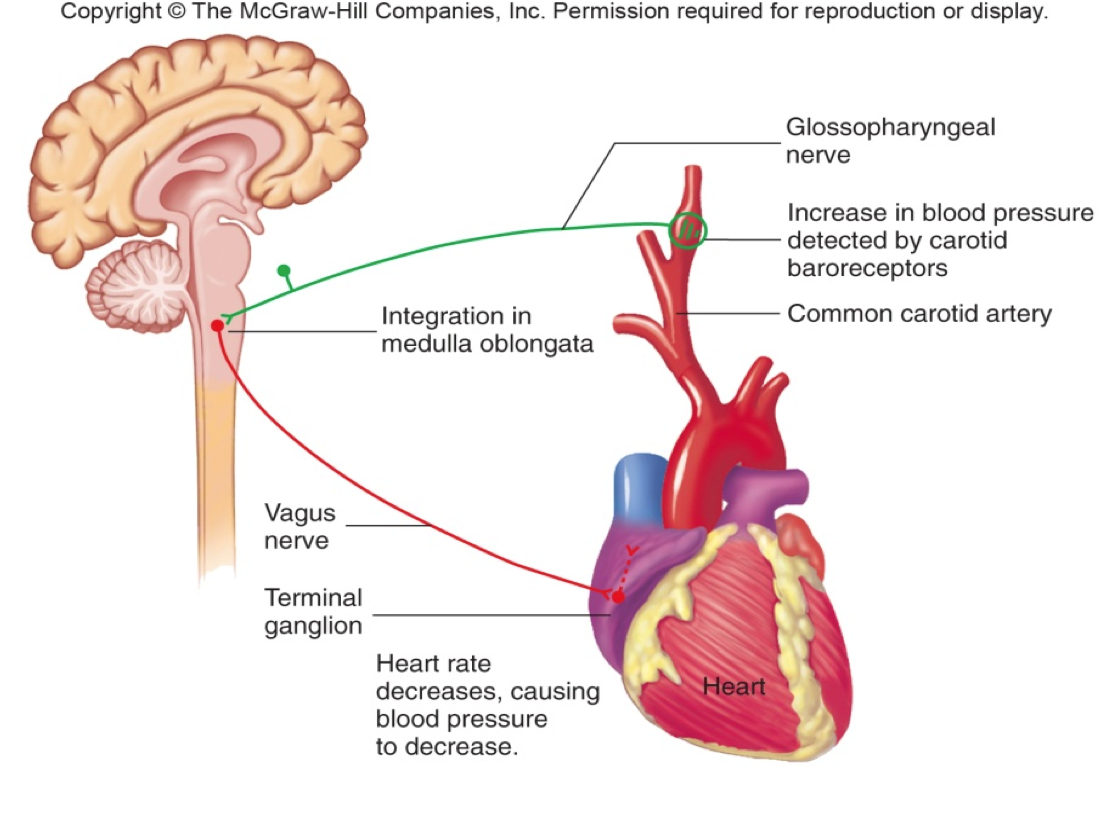
In PD, there are two major reasons why the automatic control of the cardiac system is impaired. First, areas of the brain that control this system often contain Lewy bodies and have undergone neurodegeneration. In addition, the autonomic nervous system itself is directly affected by Lewy body-like accumulations and neurodegeneration. This means, when the baroreceptors in the heart and carotid artery sense a drop in blood pressure and try to generate a signal to the heart and blood vessels to increase the blood pressure, the message may not get through. This results in neurogenic orthostatic hypotension , or drops in blood pressure upon standing due to autonomic nervous system dysfunction. There are no medications that can cure nOH by restoring the autonomic nervous system in PD. nOH however, can be treated. Read more about nOH and its treatments here.
Structural problems of the heart such as coronary artery disease or cardiomyopathy are not thought to be part of the pathology of PD, although of course, could co-exist with PD.
Don’t Miss: Can Reflux Cause Heart Palpitations
How Does Stress Affect My Nervous System
Maybe you have too many deadlines piling up at work. Perhaps your relationship with a loved one is not in the best place. Or like a lot of us, theres a lot of uncertainty in your life right now. Sometimes we find ourselves getting caught up in the details, and this can stress us out. You may know that chronic stress is a big risk factor for heart disease, obesity, and depression. But how exactly does stress interact with our nervous system to enact changes in our body?
Role Of Parasympathetic Dysfunction In Heart Failure
The sensory endings of both vagal and sympathetic afferent fibers in the heart are mechanoreceptors, thereby stimulated by the mechanical stretching associated with cardiac dilatation in HF. In HF with chamber dilatation, both vagal and sympathetic afferent cardiac fibers increase firing, as a result of which the afferent sympathetic excitation leads to tonic and reflex inhibition of cardiac vagal efferent activity. In cases of diastolic dysfunction with no dilatation of heart, the mechanism of reduced vagal activity has not been fully determined.
Also Check: List The Steps Of How To Calculate Your Target Heart Rate Zone
The Autonomic Nervous System And The Heart
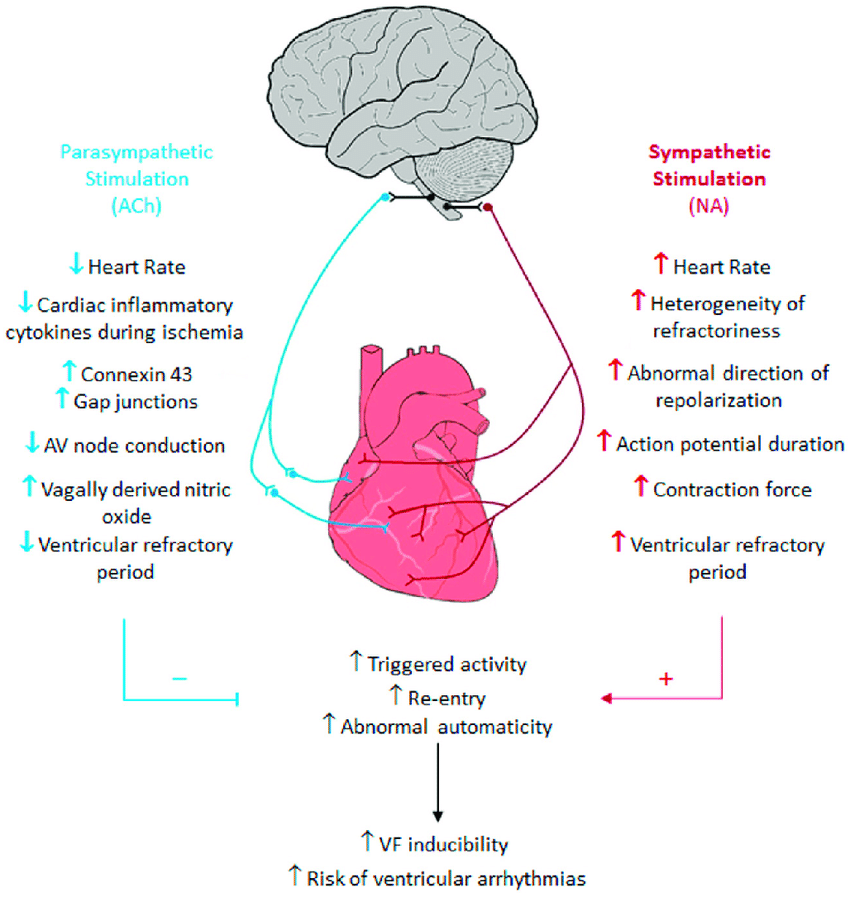
The sympathetic nervous system has a wide variety of cardiovascular effects, including heart-rate acceleration, increased cardiac contractility, reduced venous capacitance, and peripheral vasoconstriction., Conversely, the parasympathetic nervous system affects the cardiovascular system by slowing the heart rate through vagal innervation.
Changes In Heart Rate And Its Regulation By The Autonomic Nervous System Do Not Differ Between Forced And Voluntary Exercise In Mice
- 1Department of Exercise Sciences, University of Toronto, Toronto, ON, Canada
- 2Division of Cardiology, Mount Sinai Hospital, University Health Network, Toronto, ON, Canada
- 3Department of Biology, York University, Toronto, ON, Canada
NEW AND NOTEWORTHY
No previous mouse studies have compared the effects of forced and voluntary exercise on the heart function and its modulation by the autonomic nervous system .
Both voluntary free-wheel running and forced swimming induced similar improvements in ventricular contractile function, reductions in heart rate and enhancements of HR variability .
HR regulation in exercised mice was linked to increased parasympathetic nerve activity and reduced sympathetic nerve activity.
HRV was independent of HR and depended primarily on PNA in both exercised and sedentary mice.
Complete cardiac autonomic blockade eliminated differences in both HR and HRV between exercised and sedentary mice.
Read Also: Does Acid Reflux Cause Heart Palpitations
Fight Or Flight: The Sympathetic Nervous System
09 May 2019
When facing down a ferocious lion, an oncoming car or maybe just an impending deadline, our bodies trigger a physical stress response that prepares us to either fight or flee the scene. This “fight-or-flight” response is driven by the sympathetic nervous system, a normally harmonized network of brain structures, nerves and hormones that, if thrown off balance, can result in serious complications.
Parasympathetic Nervous System And Your Heart
There are a number of special receptors for the PSNS in your heart called muscarinic receptors. These receptors inhibit sympathetic nervous system action. This means theyre responsible for helping you maintain your resting heart rate. For most people, the resting heart rate is between 60 and 100 beats per minute.
On the other hand, the sympathetic nervous system increases heart rate. A faster heart rate pumps more oxygen-rich blood to the brain and lungs. This can give you the energy to run from an attacker or heighten your senses in another scary situation.
According to an article in the journal Circulation from the American Heart Association, a persons resting heart rate can be one indicator of how well a persons PSNS, specifically the vagus nerve, is working. This is usually only the case when a person doesnt take medications that affect heart rate, like beta-blockers, or have medical conditions affecting the heart.
For example, heart failure reduces the response of the parasympathetic nervous system. The results can be an increased heart rate, which is the bodys way of trying to improve the amount of blood it pumps through the body.
Recommended Reading: What Branch Of Medicine Deals With Heart Disease
Cardiac Sympathetic Nervous System
The sympathetic nervous system is the component of the ANS that is responsible for controlling the human bodys reaction to situations of stress or emergency , while the parasympathetic nervous system is generally responsible for basal organ system function.
Cardiac sympathetic preganglionic nerves emerge from the upper thoracic segments of the spinal cord . After traveling a short distance, preganglionic fibers leave the spinal nerves through branches called white rami and enter sympathetic ganglia. The cardiac sympathetic neurons form the sympathetic chain ganglia located along the side of the viscera column . These ganglia comprise the sympatheric trunks with their connecting fibers. The postganglionic fibers, extend to the viscera, such as the heart. In general, sympathetic preganglionic neurons are shorter than sympathetic postganglionic neurons .
Sympathetic receptors: There are two types of adrenergic receptors: and . In the cardiovascular system there are 1, 2, 1, and 2 adrenergic receptors .
