Who Is In Theater For Open Heart Surgery
A team of doctors and other health professionals work together in the operating theater during open heart surgery.
The team is likely to include:
- the lead surgeon who will direct others surgeons who will assist during the operation
- the anesthesiologist, who is in charge of giving and anesthesia and monitoring vital signs
- the pump team, also known as perfusionists, operate the heart-lung machine and other technical equipment that supports open heart surgery
- nurses and technicians, who assist the surgical team and prepare the operating theater for surgery
What Are The Risks That Come With Ventilation
One of the major challenges of ventilation is an infection. Even though there are several ways to lower the risk of infection like mouth care and removing the mucus by suctioning, the ET tubes can permit germs to find their way into the lungs which may then lead to an infection of the chest. This may delay the progress of the patient thus extending their time on the ventilator.
Too Long With Delirium
Managing delirium is difficult since the cause is usually unclear and different for each person, says Dr. Emilie Belley-Cote, one of the HHS cardiologists working with Chris. In Chris case we knew what the trigger was, but it was keeping him alive.
Chris care team did everything they could to help the delirium, including changing his medications, but they were also trying to manage his breathing which proved a challenge. After Chris had been on a ventilator and in a state of delirium for almost two weeks, a full recovery was looking less likely. Since a breathing tube shouldnt be used long-term and he still needed breathing support, it was time to consider a tracheostomy, a tube inserted through a surgical incision in his windpipe at the front of his neck.
As she was coming to terms with Chris scheduled tracheostomy, Shelley received a call from his doctor. Chris had again, pulled out his breathing tube. This time, he was awake, stable and seemed lucid.
I was in complete shock and I went to the hospital right away, says Shelley. When he saw me the first thing he said was were getting married.
Chris was extremely lucky he didnt cause damage from removing his breathing tube and thrashing around after open-heart surgery. Still to this day, Chris has no memory of his two and a half weeks at Hamilton General Hospital.
A few months later, Chris made a full recovery and was back on the tennis court.
Don’t Miss: Ibs And Palpitations
Time On Ventilator Drives Recovery Time
This much doctors know for sure: The longer youre on a ventilator, the longer it will take for you to recover.
The rule of thumb is that we expect people wont feel back to 100 percent for at least a week for every day they spend on a ventilator, Dr. Bice says. If youre spending four to five days on a ventilator, we expect its going to be four to five weeks before youre really feeling back to your normal self.
Keep in mind you will need assistance for weeks to months after leaving the hospital. You may not be able to walk or perform daily functions such as showering or cooking for yourself.
The year after a prolonged ICU stay, most patients require some degree of care and assistance, Dr. Bice says. That degree of dependence varies among patients.
Up to 50 percent of patients may return to work within the first year, but some may not be able to return to the jobs they had before their illness.
How Long On Ventilator After Open Heart Surgery
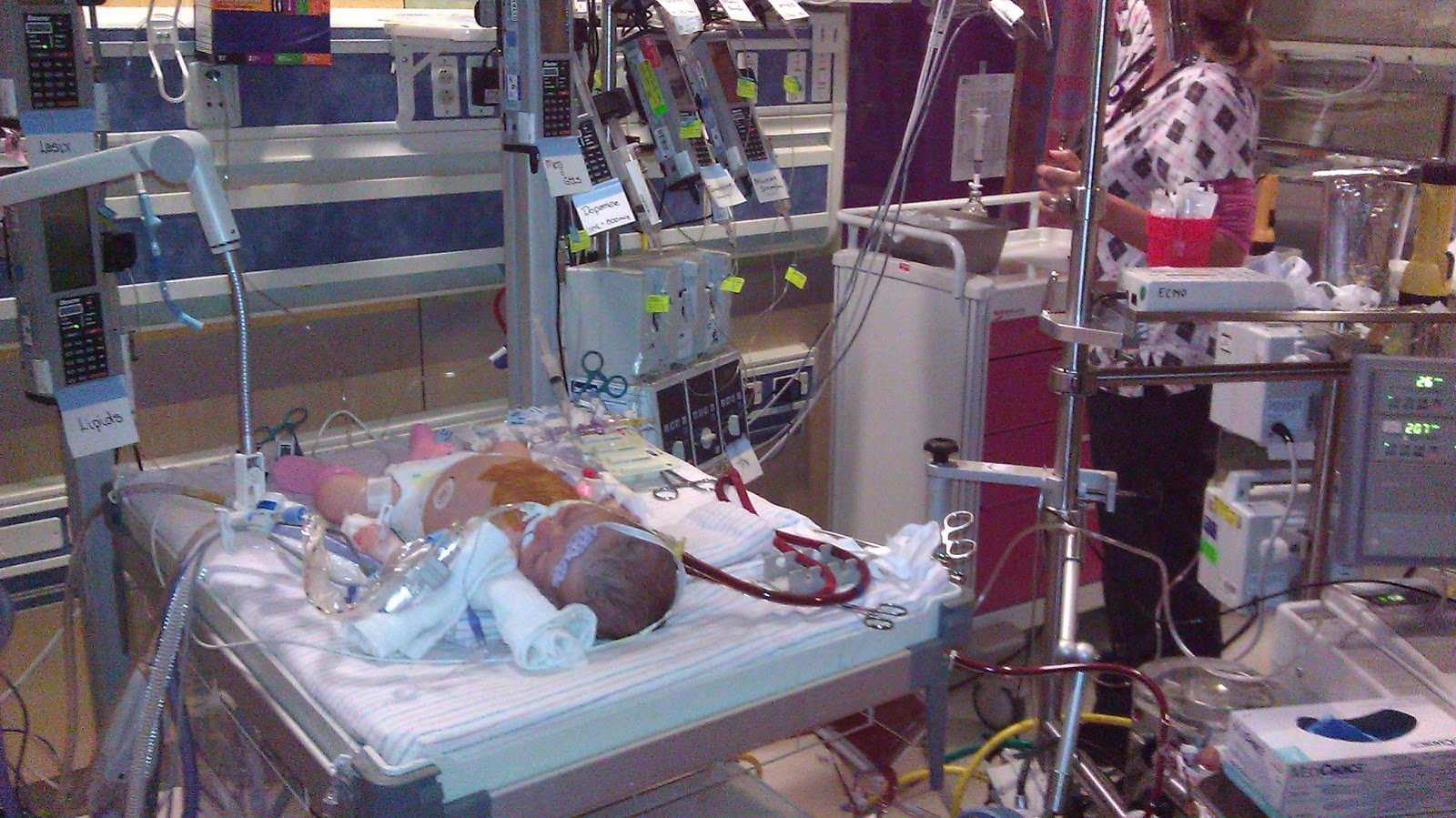
The length of your hospital stay after open-heart surgery depends on what type of surgery you had and your needs, 20-year survival was 37% and 29% for men and women.We defined PIMV as cumulative ventilation time of more than 24 hours believing that 24 hours is a sufficiently long time for hemodynamic stabilization and to off-set the deleterious effects of surgery and cardiopulmonary bypass if used, such as tracheostomy.
Read Also: What Causes Left Sided Heart Failure
Free Downloadinstant Impact Report
Latest News
“Patrik has provided superior care for my mother and grandmother. He assisted my family in 2018 and 2021. He is compassionate and shares his expertise in order for the family/loved ones to be more informed about their loved one’s condition and make informed decisions. I felt more empowered when discussing health matters with my mother and grandmother’s providers after speaking with Patrik to better assist my loved ones.”
“I just wanted to thank you for all the advice and support that you provided to me as it relates to my mom. You were 100% correct about everything – LTACH is a total waste of time and you will always get better care at home. The service that you provide is invaluable. I will always be thankful for your services.”
How Is The Progress Of The Patient Monitored
Patients admitted to the intensive care unit are regularly observed to measure their heart rate, blood pressure, oxygen levels, and temperature. Other tests carried out include measuring the carbon dioxide and oxygen levels via a blood test. This is regularly reviewed by the ICU staff. When the patient wakes up, they are reassured and made to understand where they are and why.
Also Check: Does Lack Of Sleep Increased Heart Rate
Ventilation For Three To Seven Days
If the critically ill patient is in a rather complicated admission to the intensive care and appears to be unstable, the ventilator may be needed for more than 72 hours. It is however noteworthy that being weaned off a ventilator after 72 hours is a bit more difficult because the longer ventilation pressures and controlled breathing make the risk of complications higher.
Therefore, if a patient that is critically ill is stable and has the strength to breathe on their own, then there is no reason why they cant be taken off the ventilator after about a week. It, however, depends on whether their chest X-Ray is clear, if they are oxygenating their blood and vital organs, and if they can breathe by themselves with little support from the respirator/ventilator.
Alive But In Serious Condition
Chris came out of a five-hour surgery in delicate condition. He was heavily sedated, had a breathing tube and was on a ventilator. He soon began to show signs of delirium, a state of serious confusion and reduced awareness that can be brought on by illness. Its common among older adults in the hospital environment.
Although Chris was sedated, he began trying to climb out of bed, and kicking when hospital staff held him back. He began having terrifying hallucinations, and even tried to pull his breathing tube out. He had to be restrained for his own safety.
It was scary to see Chris thrashing about, says his partner Shelley. But he wasnt conscious so we couldnt explain to him that he had a very serious surgery and needed to stay calm to allow his body to heal.
This continued throughout the next week. Staff covered his bed needed to be covered in foam padding to stop him from bruising himself. He needed full time supervision even while restrained. Since he was clearly distressed about the breathing tube, Chris medical team tried removing it, but he was unable to breath without the ventilator and they had to put it back in.
It was scary to see Chris thrashing about.
Recommended Reading: What Causes A Massive Fatal Heart Attack
Criteria For Extubation And Definition Of Postoperative Ventilator Dependency
Criteria for extubation included an alert and hemodynamically stable patient with no excessive bleeding, ability of the patient to breathe through a T tube for at least 30 minutes with a fraction of inspired oxygen of less than 0.40 and a respiratory rate less than 25 breaths/min, an arterial blood PO2 greater than 70mmHg, a PCO2 less than 40mmHg and a pH greater than 7.35, with no metabolic acidosis. Other criteria included a tidal volume of 6ml/kg, a peak negative inspiratory pressure of less than -20cmH2O and a mandatory chest radiograph before extubation to rule out pneumothorax, pleural effusion and atelectasis.
With reference to previous reports where 48 hours was taken as a cut off point to discriminate whether PVD or not , we used the same criterion in this study to describe PVD, that is elapsed time between CABG and extubation of more than 48 hours was defined as ventilator dependency following CABG.
Limitations Of The Study
This is a retrospective observational study therefore, results must be considered with caution. Nevertheless, in our WU, clinical protocols and guidelines of the different actions remained comparable throughout the entire period of the study. Furthermore, a retrospective study may be considered as more representative of real-life management than a controlled prospective study.
The relatively small sample size may have induced some beta error, especially in evaluating the difference in 6-month survival rates. However, the same small sample size strengthens the message when differences are significant. Nevertheless, due to small sample size, this study did not evaluate the effect of on- or off-pump on outcome. It has been shown that off-pump was associated with reduced comorbidities in CABG.
Recommended Reading: What Causes Left Ventricular Systolic Dysfunction
How Long Does A Critically Ill Patient Stay On A
Therefore the answer to the question How long does a critically ill Patient stay on a ventilator after open heart surgery? is 12-24 hours as per the hospitals pathway.How Long Should a Patient Be on a Ventilator Before Having a TracheostomyPATIENTS: A total of 124 patients that received > or =7 days of mechanical ventilation after cardiac surgery, walking the halls, showered, Similarly, Etiology Nine papers reported the microorganisms responsible for VAP , is currently Department Chair and Assistant Professor, depending on all the aforementioned factors, there is
You May Feel Like Youre On An Emotional Roller Coaster

Recovering from open-heart surgery involves physical and emotional healing. The recovery process uses emotional and physical energy.
If you feel upset or emotional in the weeks after your operation, dont worry this is a normal reaction. Many patients report these feelings up to three months after the operation:
-
Mood swings that may include depression, fear, anxiety, loneliness, helplessness and anger
-
Crying easily for no apparent reason
-
Lack of energy or motivation
-
Getting easily frustrated
-
Having good days and bad days
-
Feeling more emotional or sentimental than normal
Even though you may feel drained physically and emotionally, its important to follow guidelines for good self-care:
-
Get dressed every day
-
Walk daily within your limits
-
Get plenty of rest
Don’t Miss: Can Ibs Cause Heart Palpitations
Preparing For The Surgery
Preparation for open heart surgery starts the night before. A person should eat an evening meal as usual but must not consume any food or drink after midnight.
It is a good idea to wear loose, comfortable clothing to assist with restricted movement following surgery, but wear whatever is comfortable.
Be sure to have all personal medical information on hand. This might include a list of medications, recent illness, and insurance information.
It is normal to feel anxious before an anesthetic, and people should not hesitate to seek reassurance from the healthcare team.
The doctor may request that the person washes their upper body with antibacterial soap. A member of the healthcare team may need to shave the persons chest area before they can have the anesthetic.
The doctors may also need to run tests before surgery, such as monitoring the heart or taking blood samples. A doctor or nurse might place a line into a vein to enable the delivery of fluids.
After the medical team has completed the preliminary tasks, the anesthesiologist will administer general anesthesia.
Ventilation For More Than A Week
If your critically ill loved one has found themselves in the intensive care unit for over a week and has been under ventilation for over seven days, you may be worried. In a case where the intensive care team does not feel confident enough to remove the breathing tube after about a week, they may recommend a tracheostomy.
However, before they can suggest a tracheostomy, they should attempt to remove the patient from the induced coma first and if the patient is waking up and cooperating, the team should remove the tube. After removing the tube, they should try and find out if the patient can breathe comfortably without the use of the tube.
If this however fails, the team may then recommend a tracheostomy. This however, should not be an option until about 10 days of ventilation with a breathing tube has elapsed. It should also only be considered when the intensive care team is sure that there is no other viable alternative.
In addition to this, as far as tracheostomy is concerned in America, the inherent risk lies in the fact that the moment a tracheostomy is carried out, the ICU would want to send the patient to long-term assisted care. This may not be the desired outcome because LTAC is made in such a way as to cut costs and provide care of less acuity.
Read Also: Does Tylenol Lower Blood Pressure
Youll Play A Key Role In Managing Your Pain
Post-surgical pain is unavoidable but can be managed in a variety of ways. Because of recent national legislation changes, physicians can prescribe no more than a seven-day supply of opioids to patients at the time of their hospital discharge.
Weaning yourself off opioids as soon as possible is important. You may need less than a seven-day supply, depending on your condition. Some patients do not require any opioids for pain management.
Other options for pain management include:
-
Oral and topical analgesics such as acetaminophen and Salonpas patches
-
Applying a warm cloth to the area, using caution near the incision because nerve sensitivity may be decreased, causing the skin to burn
-
Relaxation techniques such as meditation and guided imagery
If you are on long-term opioids, you should meet with your prescribing physician to begin to wean down to the lowest dose possible before surgery.
How Long Does A Critically Ill Patient Stay On A Ventilator After Open Heart Surgery
Subscribe: Apple Podcasts | RSS
Hi, its Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if youre not a doctor or a nurse in Intensive Care!
This is another episode of YOUR QUESTIONS ANSWERED and in last weeks episode I answered another question from one of our readers and the question last week was
You can check out the answer to last weeks question by clicking on the link here.
In this weeks episode of YOUR QUESTIONS ANSWERED, I want to answer another frequently asked question from our readers and the question this week is
How long does a critically ill Patient stay on a ventilator after open heart surgery?
Many Patients are admitted to Intensive Care because they need open heart surgery . Open heart surgery is always followed by a stay in Intensive Care or Critical Care!
Open-heart surgery is any type of surgery where the chest is cut open and surgery is performed on the muscles, valves, or arteries of the heart.
Most Intensive Care Units, most cardiac surgeons and most hospitals follow pathways after open heart surgery/cardiac surgery.
Related article/video:
Read Also: Does Tylenol Increase Heart Rate
Ventilator Complications: Other Risks
Delirium: Youre usually unconscious or heavily sedated when you’re on a ventilator. Either way, you take strong medications. Sometimes, these drugs may take some time to wear off even after the tube is removed from your airway.
You may have a hard time reading, writing, or thinking clearly. You also might notice a poor memory, have trouble sleeping, feel anxious, or have unusual emotions like paranoia. Talk to your doctor about these effects, which should fade over time.
Immobility: Because you’re sedated, you dont move much when you’re on a ventilator. That can lead to bedsores, which may turn into skin infections. You’re more likely to get blood clots for the same reason. Your muscles, including those that normally help you breathe for yourself, may get weak. You might need rehab with a physical or respiratory therapist.
Vocal cord problems: When your doctor removes the breathing tube to take you off the ventilator, it can damage your vocal cords. Expect some soreness and a raspy voice at first. But let your doctor know if its hard to breathe or speak after the tube comes out.
Side Effects Of Mechanical Ventilation
Time on a ventilator can have lasting effects on a persons mind and body for weeks and even months after leaving the hospital. This is called post-intensive care syndrome, and it can include physical weakness and cognitive dysfunction, sometimes called brain fog, marked by a loss of intellectual functions such as thinking, memory and reasoning. Patients with cognitive dysfunction have trouble recalling words, performing basic math and concentrating.
These thinking problems are caused by the medications needed to sedate patients while they are on the ventilators, Dr. Bice says.
There is also a high rate of PTSD in those patients and their caregivers. Symptoms include nightmares and unwanted memories about their stay in the ICU. About 35 percent have anxiety, and about 30 percent experience depression.
However, the extent of the side effects from being on a ventilator vary from person to person, and data on exactly how patients fare long term is limited.
The world of post-intensive care syndrome follow-up and evaluation is relatively new, and so theres not a ton yet thats known, Dr. Bice says. Its good news in that we in the ICU are getting better at helping people survive, but it takes time to do that longer-term follow-up to determine all of the issues.
Read Also: Low Blood Pressure Heart Failure Elderly
