Risk Model Performance And Calibration
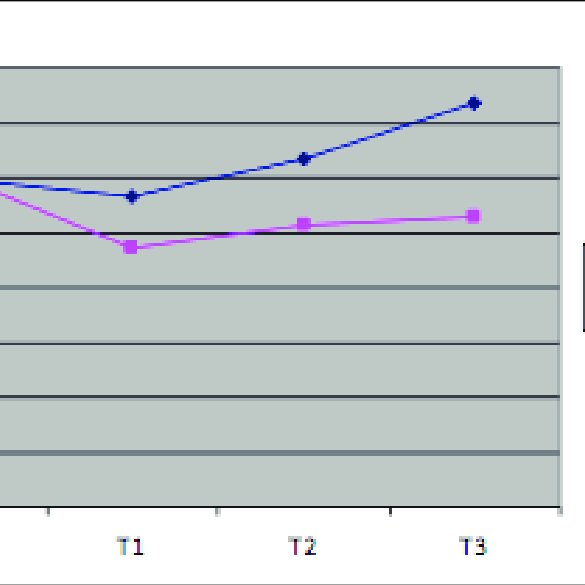
Both risk prediction models had virtually identical C statistics . Despite this similarity, CIHI-predicted mortality was significantly lower than Society of Thoracic Surgeons-predicted mortality, with a mean absolute difference of 1.03% . Using the CIHI model, 77% of patients had lower predicted mortality. In relative terms, the CIHI model underestimated risk of death by a mean of 23.7% . The underestimation was more pronounced among patients who died within 30 days of surgery than among those who did not , which was significant . Underestimation of CIHI-predicted mortality was more pronounced in patients at higher predicted risk, as evidenced by the calibration plots presented in Figure 3.
Calibration plots for mortality predicted by the Society of Thoracic Surgeons and Canadian Institute for Health Information models. Plots show observed and predicted mortality, stratified by decile of risk.
Observed and predicted mortality determined by adjusting risk models for various categories of risk factors not available in administrative data. Note: CIHI = Canadian Institute for Health Information, ESHD = end-stage heart disease, STS = Society of Thoracic Surgeons, UHN = University Hospital Network.
Hospital Or Fixed Interval Mortality
Hospital mortality rates depend on the postoperative transfer policy of patients to other health care facilities or back to the referring hospitals. A hospital with a policy of relatively early discharge or transfer will have lower in-hospital mortality rates than a similar hospital with a policy of late discharge or transfer. The fact that the moment of transfer is at the discretion of providers leaves room for gaming of results: mortality rates can be kept low by early transfer of patients to other health-care facilities . Carey et al. investigated the exact impact of discharge to other healthcare facilities on in-hospital mortality. They concluded that a substantial percentage of in-hospital deaths occur after discharge from the primary institution and that the reported in-hospital death rate might therefore be an underestimation of the true in-hospital death rate. Other studies have also shown the discrepancies between hospital mortality and 30-day mortality and similarly concluded that the former relates to institution-specific discharge policy rather than outcomes useful for benchmarking . These problems relating to in-hospital mortality can be avoided by using mortality rates at a fixed period after surgery, independent of the place of death.
Benchmarking Using Different Outcome Measures
The effect of using different outcome measures on the benchmarking procedure is shown in Fig. . When in-hospital mortality is used as outcome, one low mortality outlier and two high mortality outliers are found . However, by using 30-day mortality as outcome measure, two other centres are identified as outliers as well: Centre B as a low mortality outlier and Centre E as a high mortality outlier. Prolonging follow-up from 30 days to 1 year leads to changes in outlier status in four hospitals . When the same is done for a subset of isolated CABG procedures, benchmarking results remain unchanged with the different follow-up periods. This is shown in Fig. .
Benchmarking of isolated CABG in 10 hospitals using different mortality measures. Interventions from 2007 until 2010 were included. Benchmarking results are unaffected by the choice of the follow-up period.
Also Check: When Do Heart Attacks Occur
Read Also: What Are The Signs Of Heart Failure
Risk Factor Analysis With Survival And Changes In Cardiac Symptoms And Lvef
Post op NYHA class 34 was the only factor associated with 10-year all-cause mortality with OR of 6.3 and P value =0.012. The mean survival of patients in post op NYHA class 34 was 89.7±11.7 months , versus 120.3±8.5 months in patients with NYHA class 12 symptoms . Improvement in LVEF 5% post CABG showed a tendency to improve 10-year survival, but the effect was not statistically significant . The presence of diabetes mellitus showed a trend towards worsened 10-year all cause survival , but the difference was not statistically significant . All patients with insulin dependent diabetes died at 10 years, but analysis was not possible as the at-risk population was only 4.
Figure 5
Post op NYHA class 34 was also associated with worsened 10 year cardiac-event related mortality, with mean cardiac-related event free survival of 99.3±11.8 months in the NYHA class 34 group & 135.7±6.6 months in the class 12 group .
Figure 6
Complete revascularization and presence of all viable segments was not associated with all cause or cardiac-event related mortality. Neither of the two factors had association with post op LVEF improvement or post op NYHA class.
What Do We Do If The Bypasses Close Off
So far we have said that while LIMA-LAD grafts are an excellent option with great long term results, vein grafts are unfortunately no so good, and have an almost 1 in 2 chance of going down within several years of surgery. The good news is that the LIMA-LAD graft is the most important. And although the vein grafts may go down more frequently, if they do go down the chance of needing another heart operation is very, very low. If required, treatment can typically be undertaken using minimally invasive methods such as using stents.
The decision to treat blocked bypasses depends on many factors. Often the blockage may be silent and without symptoms, in which case no specific treatment is needed. Some bypass graft blockages will present with symptoms such as chest pain, shortness of breath or heart failure, in which case further evaluation can be undertaken and the decision made on the best treatment depending on the results of tests such as stress tests and angiograms. Finally some of these bypass blockages may present as a heart attack in which case often the blockages can be treated through the use of stents and medicines.
You May Like: What Should Heart Rate Be When Running
How Long Does It Take To Recover From Heart Surgery
Recovery depends on the type of surgery and other factors like your overall health. Most people need six to 12 weeks to recover from open-heart surgery. Some people need even more time.
Follow your care teams instructions on when you can drive, go back to work, lift heavy objects or do other activities. Your care team will also offer advice on how to care for your incision. Its important to take things slow and give your body time to heal.
As you recover, you may feel:
- A clicking sensation in your chest. This should go away after a week or two. If it doesnt, call your surgeon.
- Bruising or minor swelling at your incision site.
- Difficulty falling asleep or staying asleep.
- Less hungry. You may even feel nauseated around food for a couple of weeks. This is normal and common.
- Pain or tightness in your shoulders and upper back.
- Sad, depressed or moody.
These are normal responses to surgery. But that doesnt mean you have to face them alone. Tell your family or friends how youre feeling. If the pain feels severe or medication doesnt help, call your care team.
What Happens After Heart Surgery
After your heart surgery is done, youll be moved to the intensive care unit . Youll recover in the ICU for at least one day. Youll then move to a regular hospital room for continued rest and care.
How long you stay in the hospital depends on the surgery you had and how your body responds to it. Each persons recovery is different. Your hospital team will keep a close eye on you and make sure youre healing as you should. Theyre also prepared to notice and respond to any problems that come up.
Read Also: How Long Do Heart Attacks Usually Last
You May Experience Sleep Issues
Many people complain of having trouble sleeping for some time after heart surgery. You may experience insomnia because of:
-
Effects of anesthesia
-
Changes in your daily routine
-
Stress from personal concerns
Normal sleeping patterns typically return in two to three weeks. Until then, try these tips:
-
Take enough rest breaks in between your normal daily activities but avoid a daytime nap longer than 20 minutes.
-
If you have pain, take your pain medication about 30 minutes before bedtime.
-
Arrange the pillows so you can maintain a comfortable position and decrease muscle strain.
-
If you feel anxious or nervous, talk to your spouse, partner or a trusted friend. Get your troubles off your mind.
-
Avoid caffeine in the evenings.
-
Listen to relaxing music or a guided imagery audio program.
-
Ask your partner to give you a back rub.
-
Take a relaxing shower.
-
Follow a bedtime routine to let your body know its time to relax and get to sleep.
-
Its OK to sleep on your back, side or stomach. You will not hurt your incisions.
Recommended Reading: What Does Heart Failure Feel Like
Risk Adjustment And Benchmarking
For the benchmarking procedure, risk adjustment was performed using the logistic EuroSCORE. This model is the most commonly used risk-adjustment method in Europe and its definitions are used in the NVT database. The logistic EuroSCORE was calculated for each patient. Subsequently, benchmarking was performed using each early mortality measure. A random effects model was fitted with one of the mortality measures as the outcome variable and including the logistic EuroSCORE as covariate. A random effects model accounts for within-hospital variability and between-hospital variability and is the preferred type of regression model used for comparison between centres . This regression model thus assumes that mortality is partly explained by patient characteristics and partly by a centre effect, which is specific to each centre and can be compared across centres .
Recommended Reading: How Long Does Heart Valve Surgery Take
Description Of Study Population
Our initial data extract included almost 6 00 000 patient records. From these, 54 767 patients undergoing in-hospital CABG for whom the dates of surgery were available comprised the study cohort . The risk profile of the patient population steadily increased over time, with significant increases noted in age, proportion of males, cardiac comorbidities, diabetes and chronic kidney disease . A primary admission diagnosis of AMI among patients undergoing CABG increased during the study period. Concomitant valve surgery at the time of CABG more than doubled over the time period .
To further control for differing follow-up durations among patients having their surgery performed at different times, a series of analyses were performed limited to patient cohorts for whom there was complete follow-up. Mortality at 6 months was consistent with the longer-term result: . Two-year follow-up data were available for patients operated on up to 2012 and again a benefit was apparent for this cohort relative to those operated on earlier in the study period . Complete 5-year follow-up was limited to the cohort of patients undergoing surgery earlier during the study period and the benefit in mortality was attenuated in this cohort when compared with those undergoing CABG earlier:2000/2001 vs 2006/2007 .
Overall Mortality Rates And Survival
In total data on 33 094 interventions were extracted from the NVT national database. The study population is described in Table . The total follow-up time after intervention was 90 386.6 years and the mean follow-up time was 996.9 days. Early mortality rates using the different measures are presented in Fig. . Mortality after discharge from the primary hospital was doubled after 1 year: from 972 deaths to 2052 deaths . In-hospital and 30-day mortalities were nearly identical. However, in Table the difference between these outcome measures is shown. Approximately 20% of all deaths during admission occur after 30 days. The other way around holds true as well: 20% of all deaths within 30 days occur at home or at another care facility.
KaplanMeier survival curve with 95% CI after cardiac surgery. The green line represents the survival rate of the age-matched general population in The Netherlands. The survival rate of the cardiac surgery population equals that of the general population from approximately 120 days after surgery onwards. The hazard after cardiac continues to decline well after 30 days postoperatively. The constant phase of the hazard seems to start after 120 days.
Recommended Reading: Alternative To Open Heart Surgery
What Happens Before Heart Surgery
Preparation for your surgery can take weeks or months. Before your heart surgery is scheduled, your medical care team will evaluate your condition. Your care team will likely include your primary care doctor and cardiologist. Youll also consult with a cardiothoracic surgeon .
Your care team will give you a medical evaluation. This includes:
- Talking about your symptoms and how long theyve been going on.
- Talking about your medical history and your biological familys medical history.
- Blood tests to check your cholesterol and other important numbers.
Your team will also run some diagnostic tests. These tests provide a detailed picture of your heart function and any problems. They also help you and your care team decide if you need surgery and what type you need.
If you need surgery, your care team will tell you exactly how to prepare and what to expect. Its important to follow their recommendations about:
- When to stop taking any medications.
- When to begin fasting the day before your surgery.
- Quitting smoking or tobacco use and reducing alcohol consumption to lower your risk of complications.
Be sure to ask any questions you have, even if they seem small or you think you asked them already. Its better to double-check to make sure youre as prepared as possible for your surgery.
What to expect after youre admitted to the hospital
- Tests like an EKG or chest X-ray.
- Hair shaved from the spot where youll have your incision.
- Glasses and contact lenses.
Recovery After Open Heart Surgery

Open heart surgery is a serious procedure that necessitates constant monitoring and post-operative care. After the procedure, a person may need to stay in the intensive care unit for a few days to receive further treatment. A breathing tube will be left in place for a while after the operation to help with breathing. In addition, a line is left in the vein to provide pain treatment. A person could be connected up to a variety of various monitoring devices. A person will most likely stay in the hospital for roughly a week after exiting ICU. After leaving the hospital, it normally takes 4 to 6 weeks to recover at home. Take your time and be patient. Returning to normal levels of activity can take weeks or months. As part of a specific cardiac rehabilitation programme, some doctors may provide specialist support for daily activities and other aspects of recovery. Blood tests, heart scans, and stress testing may be part of the aftercare for each patient. During a treadmill activity, the heart is monitored as part of a stress test.
Donât Miss: Does Pain Increase Heart Rate
You May Like: What Is Normal Blood Pressure And Heart Rate
When Do You Need Heart Valve Replacement Surgery
A heart valve disease develops when the valve becomes either stiff, narrow , or leaky . These two disease states of the valve disrupt the flow of blood in and out of the heart.
Heart valve diseases can be present by birth or occur as a complication of other health conditions, such as rheumatic heart disease.
Many people who have heart valve disease may never experience any symptoms. Sometimes, the valve disease is diagnosed when a woman is pregnant. Doctors may still recommend heart valve replacement surgery to prevent the worsening of the heart condition.
With a diseased valve, heart valve replacement surgery becomes an emergency if you experience:
When Should I See My Healthcare Provider
- Signs of infection by your incision, like oozing or redness.
- Slurred speech or other signs of a stroke.
It may be hard to know when a symptom is just a part of recovery, or when its a sign of a complication. When in doubt, pick up the phone and call your care team. Its better to get checked out and learn nothings wrong than to ignore a problem that needs medical care.
A note from Cleveland Clinic
Heart surgery is a life-changing event for you and your loved ones. Take the time to learn more about your condition and the surgery that you need. Talk with your healthcare provider and ask any question that comes to mind. Keep your support system close during this journey, and dont be afraid to ask for help when you need it. If you dont have family and friends nearby, talk with your provider about available resources and support groups.
Read Also: What Is The Main Cause Of Heart Attacks
Read Also: Heart Attack And Arm Pain
Minimally Invasive Aortic Valve Replacement
Aortic Stenosis is a heart disease affecting the aortic valve. This valve is responsible for pumping oxygenated blood to all parts of the body. With AS, the aortic valve is too narrow, causing a very high internal pressure due to the heart working extra hard to pump blood through it. This pressure triggers the cardiac muscle to thicken to increase its strength, and eventually tires out and results in a life-threatening condition.
The majority of patients with AS, with or without symptoms present, need to have minimally invasive aortic valve replacement to replace the defective valve with a new mechanical or biological heart valve prosthesis. If there has been a diagnosis of severe AS, even if symptoms are not present, patients should be evaluated as soon as possible for surgical intervention. Clinical evidence shows that delaying surgery is dangerous.
Severe symptomatic aortic valve stenosis is a lethal condition that requires effective aortic valve replacement. No other medical treatment exists for this condition and, without surgery, 75% of patients will die within 3 years of being symptomatic.
Read Also: What Does A Heart Attack Look Like On An Ecg
What Are Stat Categories
STAT categories classify heart surgeries into groups based on how risky or complex they are. The STAT 1 category indicates surgeries with the lowest risk of death, while the STAT 5 category indicates the surgeries with the highest risk of death. A hospital that has a high survival rate for STAT 5 cases indicates success at handling unpredictable situations during the operation and during recovery.
What we measure:
STAT 5 neonatal survival measures the percentage of babies with the most complex heart defects who survive their surgery and have been discharged from the hospital.
What it means:
At Childrens Colorado, our surgical team specializes in some of the most complex cardiovascular procedures, with special expertise in surgical repair during the newborn period. Having a high STAT 5 survival rate means that the newborn babies we treat are more likely to survive their operation than the national average, even though we accept many more complex patients.
Recommended Reading: How To Lower Heart Rate During Exercise
Read Also: What Is My Resting Heart Rate
