Blood Thinners: What You Should Know
Blood thinners are medications used to treat and prevent blood clots. Blood travels through blood vessels in a liquid form to bring oxygen and nutrients to tissues throughout the body. When blood clots form in the body, they block normal blood flow from reaching tissues, and can cause tissue death, such as in heart attack, stroke, and pulmonary embolism.
While blood thinners can be lifesaving medications, they carry a risk of bleeding. This article discusses the types of blood thinners, their medical uses, and side effects.
Daniel Grill / Getty Images
What Are The Risk Factors For Atrial Fibrillation
The older we get, the greater our risk for atrial fibrillation. When we hit 65, our risk especially increases. Besides increasing age, high blood pressure is a huge risk factor. High blood pressure causes 1 in 5 cases of Afib. You also have a higher risk of developing Afib if you have any of the following conditions:
In addition, certain lifestyle factors like smoking, alcohol consumption and recreational drug use can raise your risk.
While exercise strengthens your heart, some athletes who exercise intensely for long periods of time could have a higher risk of Afib. In such cases, reducing the exercise intensity usually helps.
An estimated 1 in 3 people with Afib dont know they have it. Thats why its important to know the risk factors and talk with your healthcare provider. If youre at risk, you should have your heart and pulse checked regularly so you can catch problems early.
How Do They Work
Blood thinners do not actually thin the blood. Instead, they help blood flow smoothly through blood vessels and work to reduce a persons risk of forming blood clots.
Blood thinners do not dissolve or break up existing clots. But they can prevent existing clots from getting larger.
Blood thinners work in different ways. Some act by blocking or weakening vitamin K and its blood clotting effects. Others block proteins or enzymes that bind blood cells and platelets.
One type of blood thinner also works to keep platelets from sticking together or to the walls of blood vessels.
Read Also: Chronic Systolic Congestive Heart Failure
Blood Thinners Have Risks And Benefits
Many people with AFib are prescribed blood-thinning medication to help prevent the formation of blood clots. Before 2010, warfarin was the only drug available for AFib patients.
Newer anticoagulant drugs such as dabigatran , rivaroxaban , apixaban , and edoxaban have come on the market since then. However, there has been some concern about the bleeding risk of these medications.
All blood thinners can cause bleeding because they reduce the clotting effects of the blood. Multiple studies have examined the bleeding risks associated with Pradaxa, Xarelto, and other new blood thinners, and research is continuing.
Pradaxa carries a higher risk of gastrointestinal bleeding than warfarin for people over age 65, but it also is more effective at reducing the risk of stroke and death, according to a 2014 study from the U.S. Food and Drug Administration . The FDA determined that Pradaxa has a favorable benefit to risk profile and made no changes to usage recommendations. There is, likewise, a concern that Xarelto may be associated with an increased risk of gastrointestinal bleeding.
In addition to the effects of medication, we also know that age plays a role in your risk for bleeding. A 2015 study found that the risk of gastrointestinal bleeding was similar when comparing warfarin to newer blood thinners in patients 65 and younger. However, the study also found that the bleeding risk increases after age 65 and especially after age 75.
Watch Vitamin K In Your Diet When Taking A Blood Thinner
Your body makes clots and prevents bleeding by using vitamin K, and blood thinners work by blocking vitamin Kdependent clotting factors. That means a diet rich in vitamin K, which is found in leafy green vegetables, like spinach and kale, will diminish the effect of an anticoagulant blood thinner such as warfarin. You can reduce the amount of vitamin K you get in your diet by choosing iceberg lettuce over baby spinach in salads, but you dont have to completely avoid it, Garcia says. Rather, aim to get about the same amount of vitamin K every day to avoid fluctuations in the effectiveness of your blood thinner and avoid side effects.
Also Check: Can Flying Cause Heart Attacks
Vitamins And Nutrients: Find Out What Youre Missing
While you may try your best to get the vitamins you need through a diet of whole foods and complex carbs, you might still be low on a few of them. This can be caused by a variety of normal circumstances, ranging from quantities of the nutrient youre providing your body, as well as your bodys ability to absorb it when it is provided with it.
The most common nutrient deficiencies that tend to cause fatigue or low energy are that of iron, coenzyme Q10, and vitamins B12 and D. If you suspect a deficiency, ask your doctor to test your levels of these nutrients to see whether or not they are low. If they are, this is an easier fix than most simply ask your doctor for dosage suggestions on whatever youre low on, and begin taking a daily supplement. You should notice your energy levels rise as you get more of the missing nutrient in your system, if a nutrient deficiency is the underlying cause of your fatigue.
Stroke Is A Possible Complication Of Af
More persistent types of AF are associated with an increased risk of stroke. A stroke can occur when an artery in the brain is blocked by a blood clot . People with AF are at increased risk of stroke because the irregularly beating atria are prone to developing blood clots. The incomplete contraction of the atria allows blood to pool, stagnate and congeal into a clot.A blood clot can break free from the atria and circulate in the bloodstream until it reaches a blood vessel in the brain. Untreated, the risk of stroke is quite high. Other risk factors further increase the risk of stroke in people with AF.The risk of heart problems, such as heart attack and particularly heart failure, is also increased in people with AF.
Don’t Miss: Is 140 Heart Rate Bad
How Is Atrial Fibrillation Diagnosed
To diagnose atrial fibrillation, your healthcare provider will first ask you some questions. Youll share information about your diet and physical activity, family history, any symptoms youve noticed and risk factors. Its OK if you dont know all the answers but share as much as you can. Your experiences and knowledge are essential tools to help your provider make a diagnosis. Your provider will then give you a physical exam that includes:
- Listening to your heart rhythm with a stethoscope.
- Checking your pulse and blood pressure.
- Checking the size of your thyroid gland to identify thyroid problems.
- Looking for swelling in your feet or legs to identify heart failure.
- Listening to your lungs to detect heart failure or infection.
This exam will help your provider understand your baseline health and how your body is functioning.
Tests to diagnose atrial fibrillation
In addition to the physical exam, your provider may run some tests to make an atrial fibrillation diagnosis. These tests include:
In some cases, your provider may want to check how your heart works in your daily life. If so, youll be asked to wear a Holter monitor or a portable event monitor to record your hearts activity.
An EKG records your hearts electrical impulses and can show if you have atrial fibrillation.
How Can I Take Blood Thinners Safely
When you take a blood thinner, follow the directions carefully. Blood thinners may interact with certain foods, medicines, vitamins, and alcohol. Make sure that your health care provider knows all of the medicines and supplements you are using.
You may need regular blood tests to check how well your blood is clotting. It is important to make sure that you’re taking enough medicine to prevent clots, but not so much that it causes bleeding.
Recommended Reading: Acute On Chronic Congestive Heart Failure
Types Of Blood Thinners
There are a variety of blood thinners, both new and old, that fall under two categories. The first group of blood thinner medications is called anticoagulants. Anti means against and coagulant means to thicken into a gel or solid. Coagulation is the process of blood clotting.
Warfarin is an anticoagulant blood thinner that has been around since the 1950s. Despite the fact that newer blood thinners are now on the market, the U.S. Food and Drug Administration has estimated that approximately two million people still take warfarin.
But even with the continued popularity of this tried-and-true anticoagulant, a newer class of blood thinners has been introduced in recent years. Pradaxa, Xarelto, Eliquis and Savaysa are among the blood thinners approved by the FDA since 2010.
Medications To Reduce The Risk Of Stroke
The use of anticoagulation medications is the most important aspect of the treatment of AF. These medications significantly reduce the risk of stroke in people with AF and are the only therapies that have been shown to prevent serious medical events and to prolong life.The term blood thinners is often used for medications including aspirin and clopidogrel but these medications are completely ineffective in reducing the risk of stroke in AF and should not be prescribed for this reason alone.The effective anticoagulant treatments for AF are warfarin and the newer warfarin-like medications called NOACS . These include dabigatran, apixaban and rivaroxaban. There is little difference between these medications in terms of effectiveness and the small differences in each can be discussed with your doctor.The use of all anticoagulants comes with a risk of bleeding . Consequently, these medications can cause strokes as well as prevent them, although the benefits most often outweigh the risks.Careful attention should be given to the decision as to whether the benefits of anticoagulation outweigh the risks. Factors can be used to estimate the risk of stroke including previous stroke, heart failure, high blood pressure, age, gender, diabetes and vascular disease.
Read Also: Can Acid Reflux Cause Heart Palpitations
Anticoagulants And Gi Procedures
If you plan to have a GI procedure such as a colonoscopy or upper endoscopy, tell the doctor performing it if you are on blood-thinning medications. Its now considered safe to undergo most GI procedures without stopping aspirin. But if you take warfarin, you will need to tell the doctor who prescribes it that you are having a procedure. He or she will instruct you on when to stop warfarin and if you need to take other medication in its place.
Patients usually need to stop taking other blood thinners two to seven days prior to a GI procedure. You should ask your doctor for specific instructions on when to stop your medications.
Ways To Prevent Bleeding Risks
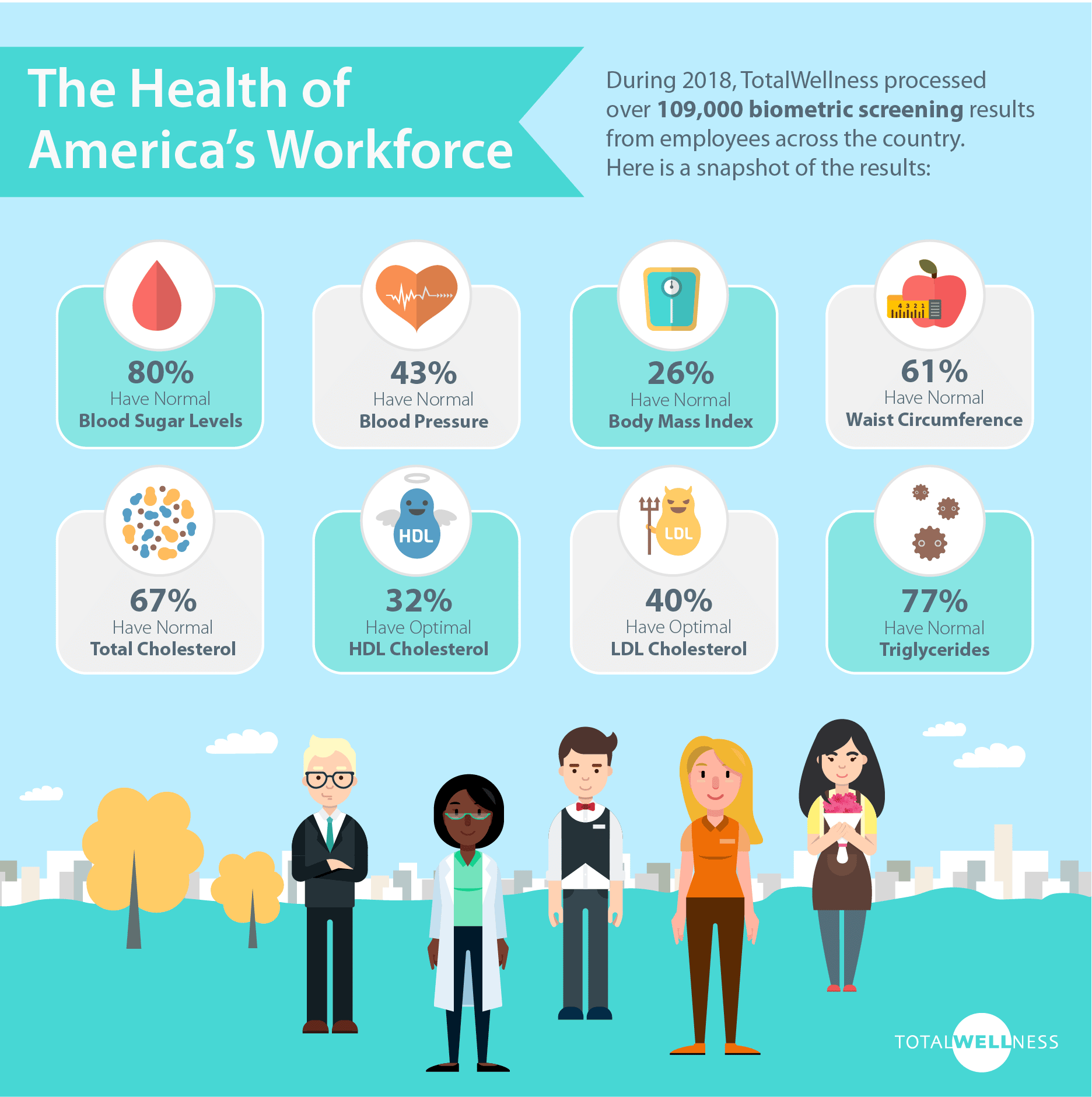
If youre taking blood thinners, following these steps can reduce your risk for potentially serious bleeding:
1. Follow your treatment plan to a T. Be sure you’re taking your medication exactly as directed by your doctor. If you dont take enough of the blood thinner, it might not be able to prevent a clot. But if you take too much, it can increase your risk for bleeding even further, according to the American Heart Association . Typically, the AHA recommends that people on blood thinners should have their blood monitored on a monthly basis.
2. Avoid taking drugs that can increase your risk of heavy bleeding. That includes non-steroidal anti-inflammatory drugs like Advil and Motrin , and Aleve , says , associate staff member in the section of vascular medicine at the Robert and Suzanne Tomsich Department of Cardiovascular Medicine at the Sydell and Arnold Miller Family Heart & Vascular Institute of the Cleveland Clinic in Ohio. Some supplements also can increase your risk of bleeding, says Dr. Gomes. St. Johns wort is one theres also some concern that high doses of omega-3 supplements can make blood thinners more potent, according to the Cleveland Clinic. If you haven’t done so already, tell your doctor about every dietary supplement you are currently using and consult with him or her before taking any new ones even if those products are labeled as safe or all natural.
RELATED: The Best Diet to Prevent a Stroke
Also Check: Heart Transplant Surgery Time
Talk To Your Swedish Physician If You Have Any Of The Listed Warning Signs
Anticoagulants and antithrombotics, commonly known as blood thinners, are used for a variety of medical conditions. They are particularly useful in preventing strokes and heart attacks in many people. But they also can cause bleeding in the gastrointestinal tract, which can be life-threatening in rare cases.
If you take blood thinners regularly or have cardiovascular disease and may be prescribed thinners in the future, here are some important facts about these commonly prescribed medications and how they can affect your gastrointestinal tract.
Aspirin and NSAIDs: Aspirin is used to prevent strokes and heart attacks. Many people with heart disease take a daily dose of “baby” aspirin, about 81 milligrams. Most patients generally tolerate aspirin well, but even in small doses aspirin can irritate the intestinal lining and lead to bleeding. If you have a history of gastrointestinal bleeding, such as an ulcer, you should confirm with your doctor that it is safe to take aspirin. Non-steroidal anti-inflammatory drugs, or NSAIDs, also can damage the GI tract and lead to bleeding. NSAIDs are commonly found in over-the-counter pain relievers and even cold medicine. Let your doctor know if you take any of these medicines.
If you are taking a blood thinner, call your doctor right away or seek emergency treatment if you have these symptoms:
- Blood in stools
- Very dark stools that look like tar or shoe polish
Blood Thinner Drug Xarelto Tied To Higher Rate Of Major Side Effects
Dec 21 – Older adults taking Bayer AG’s blockbuster blood thinner pill Xarelto for a common type of irregular heart rhythm had significantly higher rates of serious bleeding and stroke compared to those taking rival pill Eliquis, a U.S. study showed.
Xarelto, also known as rivaroxaban, is sold in the United States by Johnson & Johnson arm Janssen Pharmaceuticals. Eliquis, also known as apixaban, was co-developed by Pfizer Inc and Bristol Myers Squibb .
The findings are drawn from Medicare claims data on 581,451 adults age 65 or older with atrial fibrillation. Among every 1,000 individuals, the combined rate of major bleeding events and strokes due to clogged arteries or hemorrhage was roughly 16 per year with Xarelto versus about 13 per year with Eliquis, researchers reported on Tuesday in JAMA.
After taking participants’ other risk factors into account, the overall rate of these events was 18% higher with Xarelto, they said. Xarelto was tied to a 12% higher rate of clot-related stroke, a 26% higher rate of bleeding-related stroke, a 41% higher rate of fatal non-stroke bleeding, and a roughly doubled rate of non-fatal non-stroke bleeding.
Blood thinners are used in patients with atrial fibrillation to prevent the rhythm disorder from causing small clots in the heart that can cause strokes if dislodged.
Xarelto was approved by the U.S. Food and Drug Administration in 2011 and Eliquis was approved in 2012. Both drugs are protected by patents.
Don’t Miss: How To Take Your Heart Rate
Things To Know About Taking Blood Thinners Safely
- Atrial Fibrillation
- 7 Things to Know About Taking Blood Thinners Safely
If youve been diagnosed with an abnormal heart rhythm, such as atrial fibrillation or afib, your doctor may recommend taking blood thinners, also called anticoagulants. These medications reduce the bloods ability to clot, lowering your risk of stroke.
Your body creates clots to stop you from bleeding. If you fall or bump your head while taking a blood thinner, you may have internal bleeding even if theres no external sign youve been hurt.
Mercy Clinic Cardiology has 7 things you should know about blood thinners:
How Do Blood Thinners Work
In general, all blood thinners work by either blocking or inactivating part of the system that forms blood clots. These medications work by binding to proteins that are involved in either the coagulation cascade or to proteins on platelet surfaces.
Anticoagulant medications target the coagulation cascade, whereas antiplatelet medications target platelet activation.
You May Like: Good Heart Rate Woman
Pain With Breathing Or Other Chest Pains
Most people immediately consider that they may be having a heart attack when chest pain strikes. However, they do not know that a blood clot might have caused the heart trouble. For that reason, any chest pains you may experience could indicate that you have a blood clot. If you are sweating, and it is painful to breathe deeply, these are additional warning signs. Experts say that a blood clot that causes a pulmonary embolism feels like sharp pains in your chest. However, if your chest feels like it is holding a heavy weight, that is likely a heart problem. You should remember that both of these feelings can be a threat to your life.
