Neurological Complications After Cardiopulmonary Bypass: An Update
Log in to MyKarger to check if you already have access to this content.
Buy a Karger Article Bundle and profit from a discount!
If you would like to redeem your KAB credit, please log in.
Save over 20%
- Unlimited fulltext viewing Of this article
- Organize, annotate And mark up articles
- Printing And downloading restrictions apply
- Access to all articles of the subscribed year guaranteed for 5 years
- Unlimited re-access via Subscriber Login or MyKarger
- Unrestricted printing, no saving restrictions for personal use
The final prices may differ from the prices shown due to specifics of VAT rules.
Ica Doppler Us And Analysis
ICA Doppler US was done as part of preoperative imaging work-up within three months before cardiac surgery. Doppler US was done by experienced radiologists using Logiq7 or Logiq9 technology and a 9MHz sound linear transducer. Doppler images were retrospectively reviewed, and the degree of ICA stenosis was classified according to the Society of Radiologists in Ultrasound Consensus Conference criteria . ICA stenosis was graded as absent less than 125cm/sec and no visible plaque or intima-media thickness) or present with < 50% stenosis 5069% stenosis 70% stenosis to near occlusion near occlusion and total occlusion . ICA stenosis side was also classified as right, left, or bilateral.
Table 2 Internal carotid artery ultrasound findings
Sub Analysis Of Octogenarians
We further analysed the operative outcome in octogenarians. Four patients were 90 years of age. The operations performed in majority of octogenarians were CABG and AVR either as isolated or concomitant procedures, or combined with MVR. One patient underwent CABG and AVR combined with MVR and tricuspid valve repair.
3.3.1 Operative mortality and morbidity
The operative mortality rates were 8.6% for CABG, 5.1% for AVR, 7.9% for combined AVR and CABG, 15% for MVR, and 57% for combined MVR and CABG. Cardiac causes including failure to wean from cardiopulmonary bypass machine, ventricular arrhythmia and myocardial infarction accounted for majority of operative deaths.
Cardiac complications such as arrhythmia and low cardiac output state were the predominant causes of postoperative morbidity. About half of the patients received blood and/or blood product transfusion. Wound infection was observed in 37 patients and debridement was necessary for 10 . Two patients had mediastinitis.
3.3.2 Neurological complications
Neurological complications were observed in 49 patients and in the vast majority neurological impairment was reversible only 5 patients had residual neurological deficit at the time of hospital discharge. Confusion/agitation/seizure was observed in 31 patients and TIA/RIND in 13 . The predictors of early postoperative neurological complications in octogenarians were transfusion of blood and/or blood products and NYHA class III/IV .
Read Also: What Does It Mean When Your Heart Rate Is High
I Managing Perioperative Risk For Ischemic Stroke
a. Assessing risk for perioperative stroke
Ischemic stroke related to perioperative cerebral thromboembolic or hypoperfusion injury is a well-recognized complication of cardiovascular surgery. However, advances in perioperative medical and surgical care have progressively reduced stroke rates following primary CABG.6 Recent studies report post-CABG stroke rates of 1% 5%.79 Diabetic patients have higher post-CABG stroke risk .8 Valvular surgery carries an even higher risk for perioperative stroke, potentially due to particulate and air embolization.10 In a prospective series of > 16,000 cardiac surgery patients, stroke risk was 4.8% after isolated aortic valve replacement, 8.8% after mitral valve replacement, and 9.7% after multi-valve surgery.10 In this study, CABG was associated with a 3.8% stroke risk, and CABG + valve had a 7.4% stroke risk.10 The lack of standardized care across surgeons or institutions may explain the differential neurologic complication rates and risk factors.
b. Planning interventions for coronary artery disease: CABG vs PCI
c. Off-pump surgery vs cardiopulmonary bypass
d. Pharmacologic therapies to reduce risk
e. Atrial fibrillation and stroke
f. Occlusive cerebrovascular disease
f. Aortic valve surgery: transcatheter aortic valve implantation vs. open replacement
What Causes Cognitive Impairment After Bypass Surgery
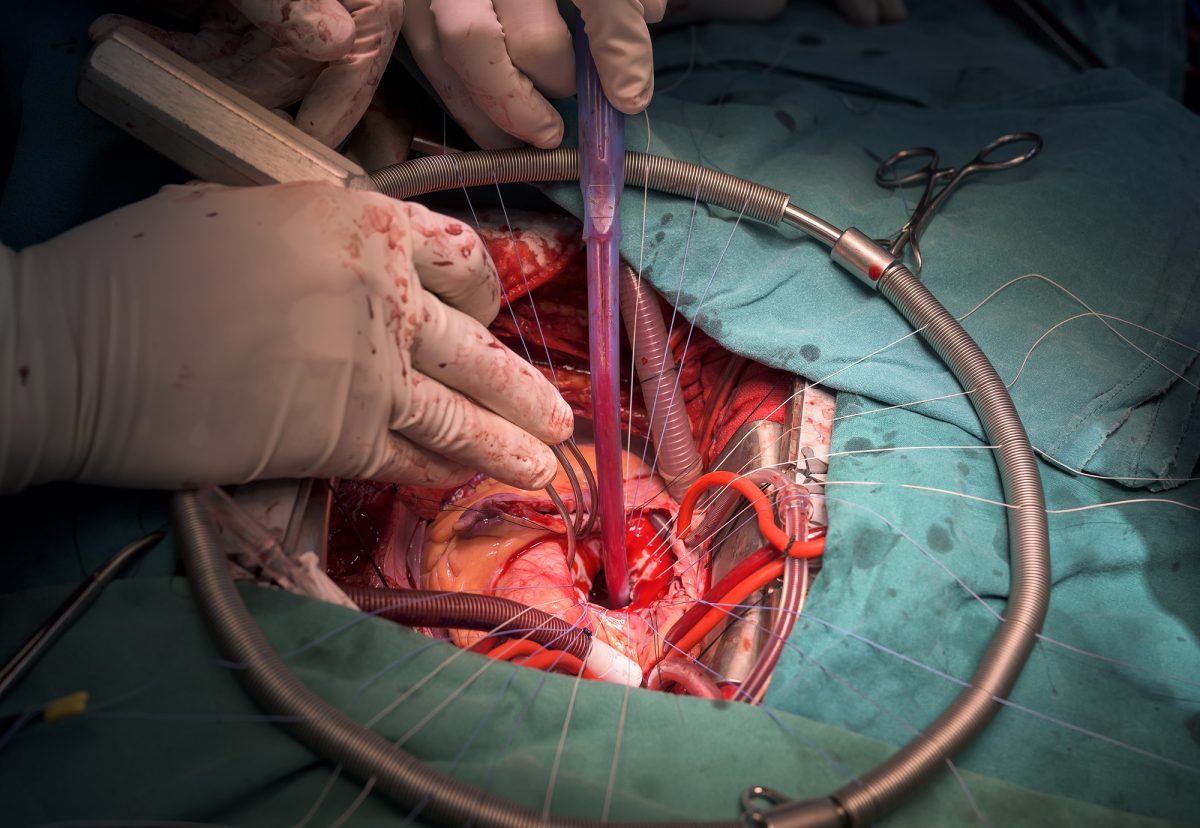
The exact cause of cognitive impairment following bypass surgery is unknown. There are probably several factors that can bring it about.
Originally it was presumed to be caused by small blood clots to the brain associated with usage of the heart-lung bypass pump. However, more recent studies have shown that employing more modern, off-pump bypass surgery has not reduced the incidence of cognitive impairment.
The theory that has the most traction today is that the manipulation of the heart and aorta can generate tiny blood clots, called microemboli, that can travel to the brain and cause damage there . Intraoperative studies using transcranial Doppler techniques have confirmed that showers of microemboli to the brain are common during bypass surgery, and other studies using pre-and-post-operative MRI scans have shown tiny ischemic lesions in the brains of people who experience cognitive decline. However, even these studies have yielded mixed results, and the causative role of microemboli is not yet proven.
Other potential causes, such as drops in blood pressure, hyperthermia , and a prolonged reduction of oxygen levels in the blood, all of which can occur during heart surgery or immediately postoperatively, may also play a role.
You May Like: Does Blood Pressure Increase During Heart Attack
Cognitive Problems After Heart Bypass Linked To Long
May 2001, Vol 32, No. 5
Print version: page 19
3 min read
Monitor on Psychology32
More than half of people who undergo cardiac bypass surgery experience memory problems and other cognitive deficits immediately after surgery. Usually, such problems fade within weeks or months. But recent research indicates heart-bypass patients who show significant cognitive decline immediately after surgery are more likely to show similar decline five years later–even when cognitive function had returned to normal within six months of surgery.
In the study, published in the Feb. 8 New England Journal of Medicine , a team of Duke University researchers led by cardiothoracic anesthesiologist Mark F. Newman, MD, examined 261 patients who had elective coronary-artery bypass grafting . The patients’ average age was 61.
Before surgery and on several later occasions, the researchers gave patients a battery of cognitive tests, measuring their verbal and visual memory, language comprehension, spatial ability, attention and concentration abilities. Results showed that 53 percent of patients experienced significant cognitive declines shortly after surgery. Six weeks later, 36 percent were impaired, and after six months, 24 percent.
Five years after surgery, however, the incidence of cognitive decline had risen again, to 42 percent. Long-term decline was more common for patients who were older, were less educated or experienced cognitive decline immediately after surgery.
–S. CARPENTER
How To Prepare For Open
Tell your doctor about any drugs you are taking, even over-the-counter medications, vitamins, and herbs. Inform them of any illnesses you have, including herpes outbreak, cold, flu, or fever.
In the two weeks before the surgery, your doctor may ask you to quit smoking and stop taking blood-thinning medications, such as aspirin, ibuprofen, or naproxen.
Its important to talk to your doctor about your alcohol consumption before you prepare for the surgery. If you typically have three or more drinks a day and stop right before you go into surgery, you may go into alcohol withdrawal. This may cause life-threatening complications after open-heart surgery, including seizures or tremors. Your doctor can help you with alcohol withdrawal to reduce the likelihood of these complications.
The day before the surgery, you may be asked to wash yourself with a special soap. This soap is used to kill bacteria on your skin and will lessen the chance of an infection after surgery. You may also be asked not to eat or drink anything after midnight.
Your healthcare provider will give you more detailed instructions when you arrive at the hospital for surgery.
Read Also: Rapid Heart Rate While Sleeping
Brain Imaging Protocol And Analysis
MRI was done on a 1.5 Tesla scan . MRI protocol included an axial T2-weighted fluid attenuation inversion recovery sequence an axial T2-weighted fast spin echo sequence an axial T2-weighted gradient echo sequence an axial diffusion-weighted sequence using b values of 0 and 1000s/mm2 a sagittal T1-weighted spin echo sequence a three-dimensional T1-weighted spoiled gradient echo sequence . CT was done on a 64-section CT scan and, again, contrast dye was not routinely used. Patients with stroke underwent emergent CT or MRI as soon as symptoms occurred and the diagnostic tool used were repeated 24h after symptoms or whenever clinical changes occurred. In patients received brain CT scan, the 24h re-evaluation allowed the detection of the vascular territory involved corresponding to the clinical neurological features. Brain images were independently evaluated by two experienced radiologists. Both readers were blinded to clinical information. Diagnosis of stroke was made using previously published criteria . Strokes were classified into ischemic and hemorrhagic. Ischemic strokes were further classified into the following categories: 1) small stroke 2) not small stroke 3) coexisting small and not small strokes. Small strokes were less than 5mm in diameter. Not small strokes included strokes greater than 5mm in diameter. Stroke arterial distribution and number were recorded.
V Neurocognitive Complications: Delirium And Cognitive Decline
Ever since Bedfords seminal case series in 1955,87 we have known that some patients experience neurocognitive difficulties after anesthesia and surgery. Although perioperative outcomes have clearly improved since that time, neurocognitive sequelae of cardiac surgery, including delirium and POCD, remain common and may affect over half of patients,88, 89 although spontaneously resolving in as many as 50% of those affected.89, 90 Whether delirium and POCD are on a pathophysiologic continuum or represent distinct cerebral injuries is unclear however, immediate post-operative delirium has been associated with longer term decreases in cognition.89 It is difficult to understand the relationship between delirium and POCD in part because we do not fully understand the pathophysiology of either condition.
a. Post-operative delirium
As highlighted above, traditional risk factors for POD in cardiac surgery patients include depression, stroke or TIA history, decreased baseline MMSE score, increased baseline serum creatinine, and abnormal serum albumin.94, 96 Despite the identification of these risk factors, the pathophysiology of POD remains unclear. Numerous biomarkers have been correlated with delirium,97 including inflammatory markers,98 markers of brain injury,99 and serum creatinine.94 Neuroimaging findings can also correlate with delirium.100 The challenge will be determining whether these correlations can lead us to mechanisms underlying the pathophysiology of POD.
You May Like: Does High Blood Pressure Make Your Heart Beat Faster
Iv Theraeputic Hypothermia For Global Hypoxic
Hypoxic cerebral injury from dysrhythmias, mechanical injury to the heart, or other complications leading to cardiac arrest can occur during cardiac surgery. While therapeutic hypothermia remains unproven in CPB and AIS, strong evidence supports its use after out-of-hospital cardiac arrest.81 Comatose survivors of out-of-hospital cardiac arrest with return of spontaneous circulation, benefit from rapid induction of TH.82 Target temperature is 32°C 34°C, and duration of TH is 24 hours in most centers. Furthermore, an increasing number of in-hospital cardiac arrest survivors are undergoing TH,83 although outcome data are limited.
In general, TH is well tolerated and the only viable treatment option after cardiac arrest, but there is only evidence regarding feasibility,86 not safety or efficacy, after cardiac surgery. Coagulopathy and immunosuppression are both risks of TH, although these risks may be small compared to a potentially devastating neurologic injury.81
Iii Treating Acute Ischemic Stroke In The Perioperative Setting
Current stroke guidelines recommend avoiding systemic thrombolysis within 14 days of major surgery,75 thus precluding the use of intravenous alteplase in most cases of stroke after cardiovascular surgery. Localized intra-arterial thrombolysis has been described with acceptable safety in this setting in one small case series.76
a. Clot/embolus extraction
Clot retrieval devices hold promise for acute ischemic stroke therapy after cardiac surgery. Currently, 4 clot extraction devices are FDA-approved for use in the United States: the Merci Retriever, Penumbra System, Trevo Pro, and the Solitaire Device . Neurointerventionalists also use aspiration and microcatheter disruption techniques77 to treat AIS, although any of these therapies must be performed within 8 hours of stroke ictus. Patients with AIS can undergo CT or MR angiography to identify large vessel occlusion, or may go directly to catheter angiography, depending on institutional protocols.
You May Like: Can Teenagers Get Heart Attacks
Brain May Suffer Long After Heart Bypass
Thought Impairment Lingers Post-Surgery
July 15, 2002 — Having surgery to save your heart may put your brain at risk. Two studies add new evidence that heart bypass surgery may have lasting effects on the mind.
More than 500,000 heart bypass surgeries are performed each year in the U.S. to restore blood flow to the heart. And although previous studies have suggested that many of these patients suffer from some type of thought impairment or impaired brain function up to six months after surgery, those effects have been hard to measure.
But by examining scans of patients’ brains before and after heart bypass surgery, researchers say these studies offer new evidence that the procedure can affect the brain in both the short and long term.
In the first study, published in the July 2002 issue of The Archives of Neurology, a team of German researchers studied 35 patients under age 70 who had a heart bypass. Brain scans were taken before and after the surgery — along with a series of tests to measure concentration, attention, short-term memory, and hand-eye coordination.
Researchers found new areas in the brain with reduced blood flow after the bypass in 26% of the patients. But having these lesions wasn’t associated with any particular type of impairment, according to the skills tests.
In a second study, a research team from the University of North Carolina at Wilmington, found that these negative effects on the brain can last weeks after surgery.
Show Sources
Peripheral Nerve Disorders After Cardiac Surgery
Professor of Clinical Neurology, Weill Cornell Medical College
Dr. Rubin reports no financial relationships relevant to this field of study.
SYNOPSIS:Following cardiac surgery, about 6% of patients will suffer a peripheral nerve injury, mostly due to compression, traction,or nerve ischemia. Proper patient positioning can prevent most of these injuries.
Gavazzi A, et al. Prevalence of peripheral nervous system complications after major heart surgery. Neurol Sci 2016 37:205-209.
Following cardiac surgery, up to 30% of patients may experience diaphragmatic paralysis due to phrenic nerve injury, while up to 15% of patients sustain peripheral nerve injury affecting the arm, usually demyelinating in nature and resolving within weeks. What is the complete spectrum of neuropathy following open-heart surgery, what are the risk factors, and what is its prevalence?
Recommended Reading: What Should Heart Rate Be When Walking
Heart Surgeries Can Trigger Strokes Seizures And Other Neurological Complications
- Date:
- Loyola University Health System
- Summary:
- Strokes, seizures and other neurological complications related to heart surgery account for “considerable morbidity and mortality,” researchers report.
Strokes, seizures and other neurological complications related to heart surgery account for “considerable morbidity and mortality,” Loyola University Health System neurologists report in the November issue of the journal Hospital Practice.
Other complications include delirium, central nervous system infections, pituitary gland problems, spinal cord or peripheral nerve injuries, residual effects of anesthesia and medication toxicity.
Complications can involve any part of the central and peripheral nervous systems. “Neurologic complications are always a risk with cardiac surgery, especially in older patients who have other health problems,” said Dr. José Biller, first author of the article and chairman of the Department of Neurology at Loyola University Chicago Stritch School of Medicine.
Strokes are the most common neurologic complication after cardiac surgery in adults. In children, seizures are the most common neurologic complication.
However, Biller said patients should not be afraid to undergo cardiac procedures. Many complications are rare. And despite the risks, cardiac surgeries generally “are highly beneficial and life-saving,” he said.
Story Source:
Changes In Cardiac Surgery Techniques
Several techniques or treatments have been developed in recent years in an attempt to improve neurological and other outcomes following cardiac surgery. As stated previously, these have not led to population-wide decreases in procedure-associated mortality and morbidity, most likely because the population undergoing surgery is older, sicker, and has more comorbidities.
Most of the technologies developed for cardiac surgery patients have been aimed at decreasing the extent of embolization to the brain. The use of epi-aortic ultrasound, as described above, is one technology that may allow for changes in operative management that could reduce cerebral embolization. Various arterial filters have been tested in an attempt to reduce distal embolization, with promising results, but unclear direct evidence for reduction in stroke and other neurological complications.91â93
Also Check: Left Sided Heart Failure Treatment
Ii Intraoperative Management To Minimize Stroke
a. Optimizing blood pressure during cardiac surgery
b. Intraoperative cerebral monitoring to prevent neurologic complications
Continuous global cerebral blood flow monitoring is not routinely available in the operating room therefore, various surrogates for cerebral blood flow have been utilized in cardiac surgery. Continuous electroencephalographic monitoring, used to detect ischemia-induced changes in brain electrical activity, can monitor large areas of cortex but cannot detect focal cerebral ischemia and is confounded by temperature effects during intraoperative hypothermia.49 However, cEEG use in critical care is expanding and may prove to be a beneficial tool for ongoing monitoring of cerebral perfusion or subclinical seizures after cardiac surgery.
Near-infrared spectroscopy , based on the differential absorption of light by oxygenated vs deoxygenated hemoglobin, is an attractive option for intraoperative cerebral perfusion monitoring.50, 51 Cerebral desaturation events measured by NIRS have correlated with cognitive decline after cardiac surgery.52 Another study randomized CABG patients to receive cerebral oximetry monitoring with an active treatment protocol for desaturation events, or a control group with blinded monitors.53 A decreased incidence in the composite endpoint of major morbidity or mortality was seen in the active treatment arm. A non-significant trend toward stroke reduction was also noted.
c. Hypothermic vs. normothermic CPB
g. Glycemic control
