Tac Operation And Echocardiography
Transverse aortic constriction operation was performed to 812-week-old male mice. Transgenic mice were all backcrossed in C57BL/6 strain for more than ten generations and age-matched pairs of mice were used in the study. We also used littermates to minimize the age differences. The transverse aorta was ligated with a 7-0 silk suture paralleled with a 26 or 27-gauge blunt needle, which was removed after the ligation. Sham-operated animals were subjected to similar surgical procedure without aortic constriction and used as control. TAC operation was performed to the mice weighing 2227g at the age of 812-week old. Surgeon was not informed about the genotype of the mice. The mice that died within 1 week after the operation were excluded from the analysis. Transthoracic echocardiography was performed to conscious mice with a Vevo 2100 imaging system . M-mode echocardiographic images were obtained from a longitudinal view to analyze the LV size and LV contraction.
Adenoviral Overexpression Of D1r
Recombinant adenovirus vectors were generated for overexpression of D1R in CMs using AdEasy Adenoviral Vector System according to the manufacturers instruction. Complementary DNA clone for Drd1 was purchased from TransOMIC Technologies and fused with FLAG-tag. Genetic Ca2+ indicator GCaMP8 was coexpressed with D1R by using inserting internal ribosomal entry site. LacZ was used as a control for D1R overexpression . The titer of the adenovirus was determined by AdEasy viral titer kit according to the manufacturers instructions. Adenovirus was infected to CMs at 3 days after the isolation at 25 m.o.i. for 6h. Cells were stained with commercially available anti-Tag antibody,, to confirm the overexpression of tagged D1R .
Selection Of Patients For Home Inotropes
Long-term inotropic therapy should be offered in selected patients. A detailed conversation with the patient and family shall be held, including a discussion on the risks and benefits of use of inotropes. Inotropes at home can be managed with the help of a home infusion program and a visiting nurse. Chronic heart failure patients awaiting heart transplants are candidates for intravenous inotropic support until the donor heart becomes available . This helps to maintain hemodynamic stability and keep the fluid status and pulmonary pressures optimized prior to the surgery. On the other hand, in patients with severe heart failure who are not candidates for advanced heart failure therapies, such as transplant and mechanical circulatory support, inotropic agents can be used for palliative therapy . In such a situation, the patient and family should be informed of the risks and benefits of this therapy. Inotropes can help reduce frequency of hospitalizations and improve symptoms in these patients.
Don’t Miss: What Causes Slow Heart Rate
Human Sample Collection And Rna
All experiments undergone at the University of Colorado Hospital were approved by the Colorado Multiple Institutional Review Board , and written consent had been obtained from all participants. The protocols of sample collection and RNA-seq analysis of whole heart tissue were previously described. The history of ICD implantation or sustained ventricular tachycardia events in 12 months prior to heart transplantation was collected. These clinical histories were obtained by independent operator who was blinded to the result of RNA-seq analysis about DRD1.
Isolation Of Cms And Single
Single-CM transcriptomes were obtained using mice model of pressure overload-induced heart failure. CMs were isolated from the heart of adult mice using the Langendorff perfusion apparatus,,. Briefly, the heart was quickly excised and retrogradely perfused through the aorta with Ca2+-free buffer for 2min at 4mL/min, then with collagenase solution , 0.05mg/mL protease type 14 , and 100µM CaCl2 in 0-Ca2+ buffer) for 10min at 3mL/min. The whole system was maintained at 39°C. Following perfusion, hearts were placed in 35-mm dish containing 100µM Ca2+ buffer with 2mg/mL bovine serum albumin and gently minced with microscissors. The cell suspension was filtered through 200µm mesh to remove undigested tissue and CMs were collected by centrifugation at 100×g for 2min. The supernatant was discarded and CMs were resuspended in medium containing a low concentration of Ca2+ . Rod-shaped living CMs were collected immediately after isolation and incubated in lysis buffer. Smart-seq2 protocol generated the single-cell RNA-seq libraries. A total of 280 single-CM transcriptomes of sham-operated, 1, 2, and 4 weeks after TAC-operated mice were analyzed. RPKM values were calculated with reads mapped to the nuclear genome using DEGseq .
Also Check: Steps In Dying From Congestive Heart Failure
Deletion Of Cardiac D1r Ameliorates Ventricular Arrhythmia
Fig. 2: Deletion of cardiac D1R ameliorates heart failure-associated ventricular arrhythmia.
a Generation of cardiac-specific D1R-deficient mice and the design of the PCR primer. KO knockout. b Representative results of the genotyping PCR from both tail and heart tissues. Genomic DNA was extracted from the mice with indicated genotypes. c Bar graph showing the expression of Drd1 in TAC-operated hearts of MHC-Cre or MHC-Cre/Drd1fl/fl mice assessed by qPCR . Data are shown as mean and s.e.m. Statistical significance was determined by MannWhitney U test *p=0.036 versus control. d Left: representative surface electrocardiogram recordings of the normal sinus rhythm and the premature ventricular contraction . Right: bar graph showing the frequency of drug-induced PVC in MHC-Cre and MHC-Cre/Drd1fl/fl mice under anesthesia. The frequency of PVC in MHC-Cre mice before TAC operation is shown as a control , n=7 and MHC-Cre/Drd1fl/fl , n=5). Data are shown as mean and s.e.m. Statistical significance was determined by KruskalWallis test followed by Dunns multiple comparisons test *p=0.023 MHC-Cre versus MHC-Cre/Drd1fl/fl . e Survival curves comparing post-TAC survival of MHC-Cre and MHC-Cre/Drd1fl/fl mice . Statistical analysis was performed by GehanBreslowWilcoxon test *p=0.030.
Isolation Of Neonatal Rat Cms
Neonatal rat CMs were prepared from the ventricles of newborn Wistar rats. The ventricular part of the heart was quickly excised and washed in ice-cold PBS. Digestion of the ventricles was performed seven times with 0.05% trypsin-EDTA at 37°C for 10min. Supernatant from the first digestion was discarded, and those from the other digestion steps containing CMs were collected. Non-CMs were separated from CMs by plating the cells to a culture dish in Dulbeccos modified Eagles medium containing 10% fetal bovine serum and the cells were cultured at 37°C for 50min. Nonattached cells were collected and used as CMs. CMs were cultured in DMEM containing 10% FBS and 25µM cytosine -D-arabinofuranoside hydrochloride was added to inhibit the proliferation of non-CMs.
Don’t Miss: Life Expectancy With Heart Failure
Dopamine And Dobutamine For Congestive Heart Failure
Acute dopamine infusion increases renal plasma flow, urinary sodium excretion rate, glomerular filtration rate, and the functional status of patients with moderate to severe congestive heart failure. These effects result from stimulation of dopamine receptors as well as f3 adrenergic receptors. Beregovich and co-workers studied the dose-related hemodynamic and renal effects of dopamine in patients with classes III and IV congestive heart failure . Cardiac output and urinary sodium excretion rates rose progressively as dopamine infusion was increased from 1 to 5 and 10 /¿g/kg/min. Stroke volume and urinary flow rate, however, tended to plateau above 5 /xg/ kg/min and several patients developed sinus tachycardia or striking increases in systemic vascular resistance at the highest infused dose. These workers concluded that a dose of 5 /¿g/kg/min was optimal in terms of overall hemodynamic response in patients with congestive heart failure. While the effects of dopamine infusion on renal sodium excretion and cardiac hemodynamics are often dramatic, the natriuretic effects typically wane after 12-24 hr .
Dopmamine, /^kg/minute Dopamine, fig/kg/minute
FIGURE 5. Effects of dopamine on cardiac output , systemic vascular resistance , urinary sodium excretion , and urine flow rate in patients with congestive heart failure. Data from Beregovich, et al. Am. Heart J. 87:550-557,1974.
50 100 150 200 250 300
FUROSEMIDE EXCRETION RATE
50 100 150 200 250 300
Phosphodiesterase Type 3 Inhibitors
Milrinone
Milrinone, a PDE3 inhibitor, is a commonly used inotropic agent in patients with severe HF or cardiogenic shock. It inhibits PDE3, which physiologically degrades intracellular cyclic adenosine monophosphate . Through this inhibition, cAMP accumulates in the cell, causing protein kinase A activation. This facilitates more calcium ions to enter the myocardial cell, thus potentiating the actin-myosin cross-bridging leading to increased cardiac contractility. This mechanism is independent of the beta-adrenergic pathway. As a result, the use of PDE3 inhibitors, and milrinone in particular, is suitable for patients with chronic HF under beta-blockade who present with AHF or cardiogenic shock compared with other inotropes.
Another feature of the mechanism of action of milrinone is that the same intracellular processes is activated in smooth muscle cells of the peripheral and pulmonary vasculature, leading to a net vasodilatory effect in addition to its positive inotropic effect. This combination of actions classifies milrinone as an inodilator.
Recommended Reading: Is Heart Rate The Same As Blood Pressure
Human Sample Collection And Single
All experiments were approved by the ethics committee of the University of Tokyo . All procedures were conducted according to the Declaration of Helsinki, and written informed consent was obtained from all participants. Heart tissue was obtained immediately after death due to noncardiac cause or during LV assist device surgery or heart transplantation . The history of sustained ventricular tachycardia was collected from clinical records of our hospital, patient referral document from other hospitals, or cardiac monitoring records of implantation device. These clinical histories were obtained by independent operator who was blinded to the result of single-cell RNA-seq analysis. Demographics and characteristics of each patient were shown in Supplementary Table . Immediately after the collection of the heart tissue, rod-shaped living CMs were isolated, and then incubated in lysis buffer. The method of single-cell RNA-seq analysis using the Smart-seq2 protocol was previously described. Single-CM RNA-seq data has been deposited in the Gene Expression Omnibus with the accession code GSE 95143.
Dopamine: Clinical Applications Iii Cardiovascular
- Barry P. McGrath, Xhi Qin Wang
- Aust Prescr 1994 17:44-5
SummaryDopamine is an endogenous catecholamine with an important role in the regulation of renal function, sodium homeostasis and blood pressure. D1 receptors on vascular smooth muscle mediate vasodilatation, while stimulation of D1 receptors in the renal proximal tubules leads to natriuresis and diuresis. D2 receptors on presynaptic sympathetic nerve endings inhibit noradrenaline release. Dopamine infusions are used widely for the management of cardiovascular disorders and renal dysfunction in intensive care units. The ability of dopamine to `protect’ the kidney against ischaemic or toxic insults requires proper evaluation in controlled trials. A number of dopaminergic prodrugs, selective dopamine agonists and dopamine congeners with additional actions on other adrenoceptors have been developed. These drugs are undergoing clinical trials in the management of cardiovascular disorders such as hypertension, heart failure and shock.
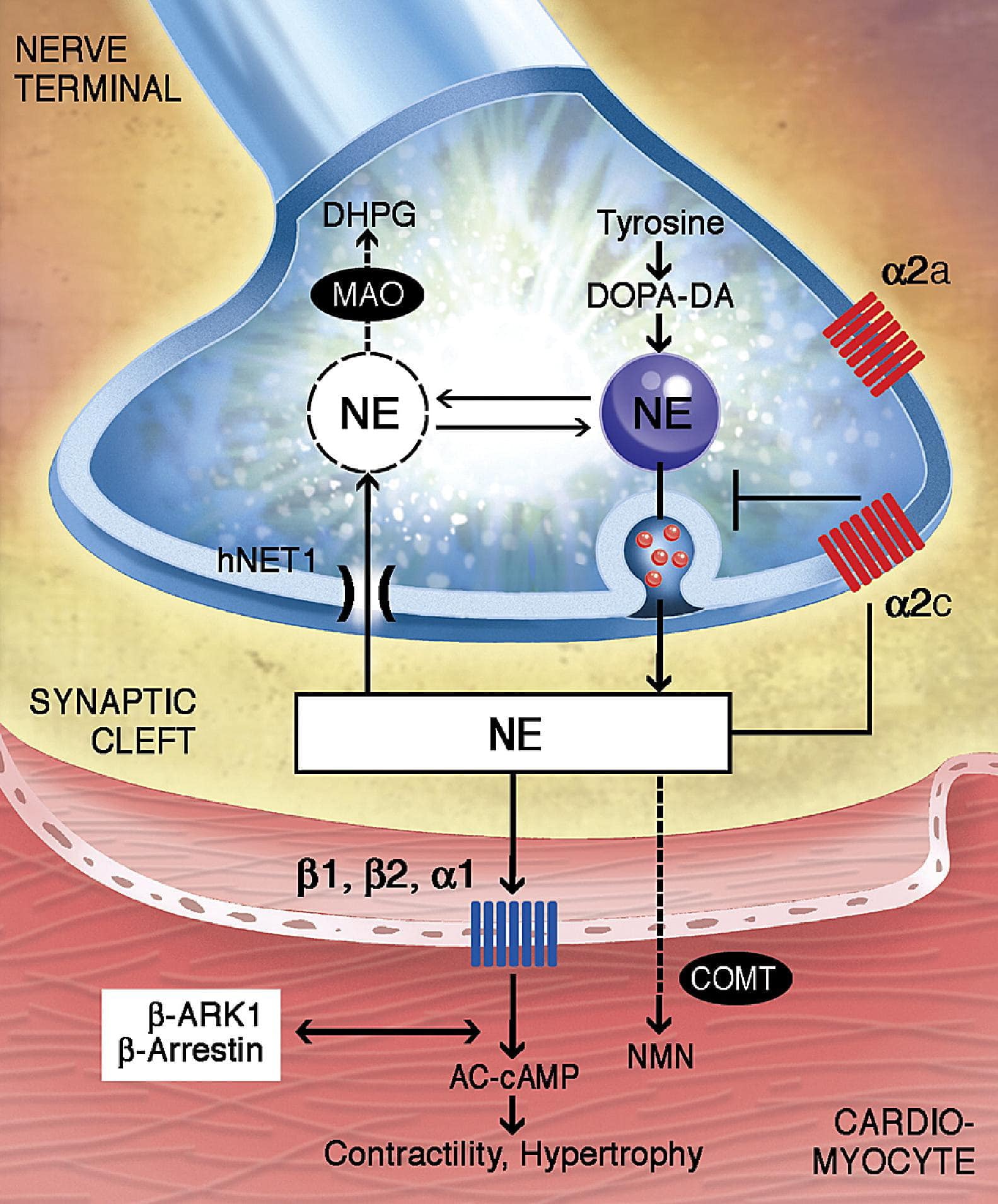
Endogenous dopamine and dopamine receptors Dopamine is an endogenous catecholamine which modulates many physiological functions. These include peripheral cardiovascular control and central nervous system actions. Central dopamine receptors and pathways are likely to be involved in the control of cardiovascular function, but this has been a rather neglected area of research. Most studies have focused on the peripheral actions of dopamine.
Further reading
Also Check: How Long Should Heart Palpitations Last
Complementary And Alternative Medicine
Some complementary therapies have been proven helpful in managing heart failure. These approaches do not cure or improve the condition, and they have not been proven to prolong life. However, they may improve symptoms and help prevent heart failure from worsening.
- Mind-body interventions: Techniques such as yoga, tai-chi, acupuncture, biofeedback, and reflexology are generally done with the guidance and supervision of a trained expert. Studies have shown that these interventions can provide small to moderate benefits for people with heart failure.
- Stress reduction: Stress management techniques such as meditation, counseling, mindfulness, and lifestyle adjustment have produced moderate benefits in heart failure. There are various stress management techniques, and selecting the approach that best fits your personality is important.
- Curcumin: A natural spice derived from turmeric, curcumin has shown some preliminary promise in heart failure in animals. Its effectiveness in preventing or treating heart failure in humans is unknown.
Complementary therapies should never be used in place of medical treatments recommended by your healthcare provider. Always tell your practitioner about any alternative or complementary treatments you’re using.
Recommendations On The Optimal Administration Of Inotropes In Acute Heart Failure
Approximately 10% of all hospitalised HF patients also have hypotension, decreased cardiac output and signs of peripheral hypoperfusion. In this considerable subgroup of patients, inotropes are recommended as part of their management . In refractory cases, circulatory support devices can be used in selected patients to maintain perfusion and haemodynamic stability for short periods of time. However, due to the sparsity of these devices compared with the large number of AHF patients, their use is reserved as bridge-to-transplant or other treatment decisions, while inotrope infusions as initial short-term support remain very common in everyday clinical practice.
Practical Recommendations on the Use of Inotropes in Patients with Acute Heart Failure and Hypoperfusion
AHF = acute heart failure CHF = chronic heart failure SBP = systolic blood pressure.
The general principle that applies for the use of inotropes is to use them for the shortest amount of time possible and in the lower effective dose until the therapeutic goal of haemodynamic stabilisation and restoration of vital organ perfusion and function is achieved.
You May Like: Can Ecg Tell Heart Attack
Left Ventricular Assistive Device
LVADs are battery-operated pumps implanted in the body to assist the heart with pumping. They were initially considered a way to support the heart function for people who were waiting for heart transplants, but they are effective and can be used as a more long-term plan.
Placement of these devices requires general anesthesia and a recovery period of several days. You should also expect your medical team to test the effectiveness of the device shortly after the procedure and periodically for the long term.
Increased Expression Of Cardiac D1r In Patients With Heart Failure
We finally assessed the expression of D1R in patients with heart failure. RNA-seq analyses of whole heart tissues from patients with cardiomyopathy of various etiology, showed that D1R expression was upregulated in human failing hearts . Furthermore, our ad hoc analysis on previous cohort demonstrated that among patients with cardiomyopathy, the expression levels of cardiac D1R tended to be higher in patients with a history of ventricular tachycardia and/or with an implantable cardioverter defibrillator device . We next analyzed the transcriptome of the CMs from the patients by single-cell RNA-seq. There was no CM that expressed D1R among the 72 CMs examined in the patient with normal cardiac function. In contrast, D1R-expressing CMs were identified in 9 out of 11 patients with heart failure . Moreover, the number of D1R-expressing CMs tended to be higher in the heart failure patients with a clinical history of ventricular tachycardia . These observations support our findings in animal models and suggest a role for D1R-expressing CMs in the pathogenesis of ventricular arrhythmias in patients with heart failure. These findings in human patients may also explain the result of the previous clinical study showing that dopamine analogs worsened the prognosis of the patients, with chronic heart failure by increasing the incidence of cardiac sudden death related with arrhythmia.
You May Like: How Blood Travels Through The Heart
How Is Dopamine Injection Given
Dopamine is injected into a vein through an IV. A healthcare provider will give you this injection.
Tell your caregivers if you feel any burning, pain, or swelling around the IV needle when dopamine injection is injected.
Your breathing, blood pressure, oxygen levels, kidney function, and other vital signs will be watched closely while you are receiving dopamine injection.
Recommendations On The Optimal Weaning Of Inotropes In Acute Heart Failure
As soon as congestion is alleviated and renal function improves, shown by an increase in urinary output and a decrease in blood urea nitrogen and creatinine levels, inotropic support should be tapered with the goal of complete weaning. During this time, standard oral HF treatment should be reinstated, and target doses should be reached after inotropic support is completely withdrawn. Unfortunately, there is a subset of patients who are unable to maintain adequate BP and perfusion without inotropic support despite multiple attempts to discontinue them. These patients, often referred to as inotrope-dependent, are usually supported with inotropes for prolonged periods of time either as a bridge or as part of a broader palliative strategy aimed at symptomatic relief.
You May Like: Workout Heart Rates
Enhancing Healthcare Team Outcomes
Dopamine administration affects the cardiovascular system, as well as other organs, including the kidneys and the brain. Contraindications include specific pharmaceutical agents, lifestyle, and nutrition factors that can impact similar organs with DA treatment. These factors and medications include psychopharmacological agents, neuroleptics, general anesthetics, and even physical therapy-induced cardiac challenges. Communication among all interprofessional healthcare team members, including clinicians, mid-level practitioners, nurses, pharmacists, and therapists, is critical to ensuring proper application of DA to mitigate potentially harmful or chronic adverse effects while considering a holistic healthcare approach along with specific outcome objectives. By engaging in interprofessional teamwork and communication, dopamine therapy can achieve its best possible outcomes with the fewest adverse events.
Overexpression Of Cardiac D1r Triggers Ventricular Arrythmia
We next investigated whether the overexpression of Drd1 gene is sufficient to trigger ventricular arrhythmia in vivo. We crossed MHC-tTA knock-in mice and TRE-D1R/lacZ transgenic mice to create MHC-tTA/TRE-D1R mice. In this transgenic mouse, D1R was overexpressed specifically in CMs, but the overexpression is silenced by treatment with doxycycline . The frequency of drug -induced PVC was significantly higher in MHC-tTA/TRE-D1R mice compared with control mice . Furthermore, PVC frequency in MHC-tTA/TRE-D1R mice was decreased by addition of doxycycline that reduces D1R expression, while doxycycline administration to wild mice didnt affect the frequency of PVCs in wild-type mice . In addition, cardiac function was not altered with overexpression of D1R in CMs . These results collectively suggest that the upregulation of cardiac D1R is both necessary and sufficient for triggering life-threatening ventricular arrhythmia during heart failure independent of cardiac function.
Fig. 3: D1R overexpression in cardiomyocytes triggers aberrant calcium handling.
Also Check: What Is Heart Failure With Preserved Ejection Fraction
