Heart Failure: The Most Important Preventable And Treatable Cardiovascular Complication Of Type 2 Diabetes
Diabetes Care
Milton Packer Heart Failure: The Most Important, Preventable, and Treatable Cardiovascular Complication of Type 2 Diabetes. Diabetes Care 1 January 2018 41 : 1113.
Concerns about cardiovascular disease in type 2 diabetes have traditionally focused on atherosclerotic vasculo-occlusive events, such as myocardial infarction, stroke, and limb ischemia. However, one of the earliest, most common, and most serious cardiovascular disorders in patients with diabetes is heart failure . Following its onset, patients experience a striking deterioration in their clinical course, which is marked by frequent hospitalizations and eventually death. Many sudden deaths in diabetes are related to underlying ventricular dysfunction rather than a new ischemic event. As effective treatments for heart failure have emerged, the risk of sudden death has declined, even in the absence of an implantable cardioverter-defibrillator .
See accompanying articles, pp. 14, 136, 143, 150, and 156.
Stage 3 Of Congestive Heart Failure
Its not uncommon for congestive heart failure to be accompanied by other heart conditions. If you are diagnosed with stage three CHF, along with another heart condition, its likely that youll have difficulty performing regular tasks. Small bouts of exercise or minimal doses of physical activity will cause the same symptoms mentioned in stage two fatigue, shortness of breath, and heart palpitations. In stage three, lifestyle changes are not as effective, and a surgical procedure may be necessary. However, its never too late to talk to a doctor about your heart condition and what the future may look like.
When To Get Medical Advice
See a GP if you experience persistent or gradually worsening symptoms of heart failure.
Call 999 for an ambulance or go to your nearest A& E department as soon as possible if you have sudden or very severe symptoms.
A number of tests can be used to help check how well your heart is working, including blood tests, an ECG and an echocardiogram.
Also Check: Weakening Heart Symptoms
Stages Of Heart Failure
In 2001, the American Heart Association and American College of Cardiology described the “Stages of Heart Failure.” These stages, which were updated in 2005, will help you understand that heart failure is often a progressive condition and can worsen over time. They will also help you understand why a new medication was added to your treatment plan and may help you understand why lifestyle changes and other treatments are needed.
The stages classified by the AHA and ACC are different than the New York Heart Association clinical classifications of heart failure that rank patients as class I-II-III-IV, according to the degree of symptoms or functional limits. Ask your doctor what stage of heart failure you are in.
Check the table below to see if your therapy matches what the AHA and ACC recommend. Note that you cannot go backward in stage, only forward.
The table below outlines a basic plan of care that may or may not apply to you, based on the cause of your heart failure and your special needs. Ask your doctor to explain therapies that are listed if you do not understand why you are or are not receiving them.
The New York Heart Association clinical classifications of heart failure rank people as class I-II-III-IV, according to the degree of symptoms or functional limits. You can ask your doctor if you want to know what stage of heart failure youâre in.
Congestive Heart Failure & Coughing: What To Do When Experiencing Cardiac Cough
Medically reviewed by Dr. Kenneth Knowles, MD on February 21, 2020
You have a bad cough so what? Its probably just a little cold, or so you keep telling yourself and anyone who comments. While most people associate coughing as a common symptom that accompanies lung or respiratory issues, its connection to heart failure often goes unnoticed. This is called a cardiac cough, and it often happens to those with congestive heart failure . In fact, a bad cough and CHF can actually be a warning that your treatment for heart failure is, well, failing or, at the very least, reacting poorly with your body. Stick around as we dive deeper into the relationship between congestive heart failure and coughing, and how you should treat your cardiac cough when experiencing exacerbated symptoms.
Recommended Reading: Left Ventricular Congestive Heart Failure
Providence Cardiology Specialist Scott Werden Says Treatment Options Include Medication And Lifestyle Changes
Like so many diagnoses, the words pack an emotional wallop: Congestive heart failure.
While the phrase may sound like a death sentence, the good news is that many people whose hearts are considered to be failing can make a virtually complete recovery.
The phrase congestive heart failure is not a pronouncement of imminent death, but a clinical term to describe poor functioning of the mechanics of the heart. As the American College of Cardiology puts it, it is a problem with how your heart pumps.
It is a scary term, agrees Scott Werden, D.O., a cardiology specialist who practices in Olympia and Shelton, Washington, with Providence Medical Group Cardiology Associates. But, he says, You can have an absolutely complete recovery from heart failure.
Dr. Werden says full recovery depends on a variety of things, such as how well a patient responds to medication. A minority of people with congestive heart failure require surgery, and some will never enjoy the high quality of life they did before their hearts failed. But many others will return to very nearly normal life and levels of activity, he says.
What Are The Symptoms Of Heart Failure
You may not have any symptoms of heart failure, or the symptoms may be mild to severe. Symptoms can be constant or can come and go. The symptoms can include:
- Congested lungs. Fluid backup in the lungs can cause shortness of breath with exercise or difficulty breathing at rest or when lying flat in bed. Lung congestion can also cause a dry, hacking cough or wheezing.
- Fluid and water retention. Less blood to your kidneys causes fluid and water retention, resulting in swollen ankles, legs, abdomen , and weight gain. Symptoms may cause an increased need to urinate during the night. Bloating in your stomach may cause a loss of appetite or nausea.
- Dizziness, fatigue, and weakness. Less blood to your major organs and muscles makes you feel tired and weak. Less blood to the brain can cause dizziness or confusion.
- Rapid or irregular heartbeats. The heart beats faster to pump enough blood to the body. This can cause a rapid orirregular heartbeat.
If you have heart failure, you may have one or all of these symptoms or you may have none of them. They may or may not indicate a weakened heart.
You May Like: Claritin Heart Racing
What Is The Treatment For Congestive Heart Failure
The treatment of heart failure depends on the exact cause, but it can usually be treated effectively. The overall goals are to correct underlying causes, to relieve symptoms, and to prevent worsening of the condition. Symptoms are relieved by removing excess fluid from the body, improving blood flow, improving heart muscle function, and increasing delivery of oxygen to the body tissues. This can be done by the various congestive heart failure treatments listed in this sections.
If the underlying cause of heart failure is not correctable by surgery or catheterization procedures, medical treatment is composed of lifestyle changes and medications.
Congestive Heart Failure 101
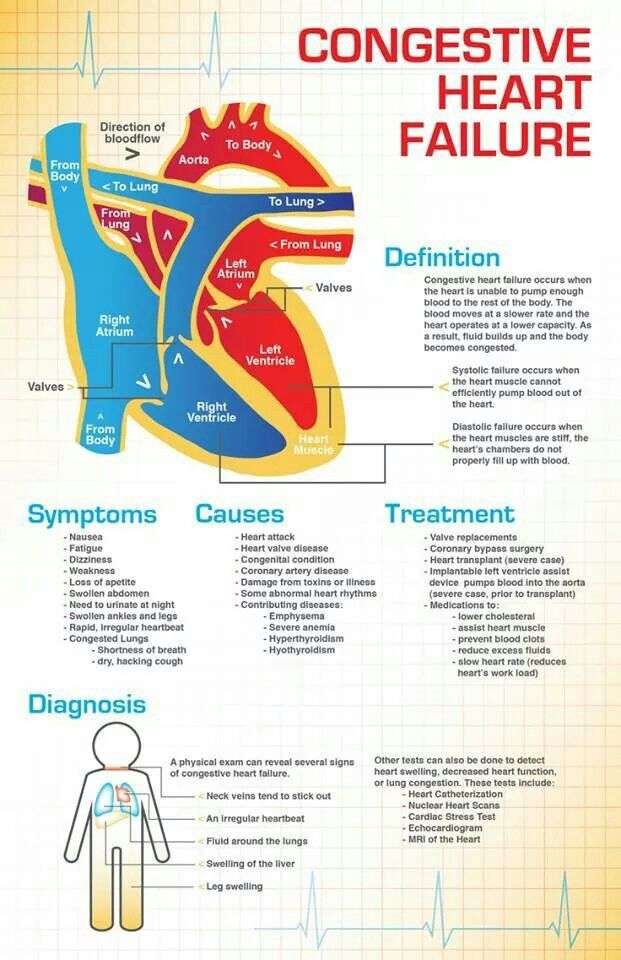
Congestive heart failure occurs when the heart cant pump enough blood to meet the demands of your body. This impairment can result from a number of preexisting cardiac disorders, which can lead to the following symptoms:
- Fatigue and weakness
- Edema
- Wheezing or chronic coughing
Due to the hearts inability to effectively pump blood, any returning circulation from the heart to the lungs can get backed up. This can lead to pulmonary congestion hence, the name congestive heart failure. Its also the primary reason behind chronic coughing.
Recommended Reading: Fitbit Charge 2 Accuracy Heart Rate
Treating The Underlying Causes
A number of conditions can contribute to heart failure. Treatment of these other factors may range from surgery or angioplasty to open clogged blood vessels in patients with coronary artery disease to medications prescribed to control high blood pressure, diabetes, anemia or thyroid disease. In addition, it’s particularly important to treat abnormal heart rhythms called arrhythmias in patients with heart failure.
Congestive Heart Failure: Symptoms Treatment And Prognosis
Congestive heart failure is a condition that may develop when the heart cant pump enough blood through to the body.
Heart failure doesnt mean the heart has stopped, but it has been weakened or damaged by coronary artery disease, high blood pressure, or infections.
Heart failure can gradually develop and worsen over time, or come about very quickly, depending on the cause.
Most of those living with CHF control their condition, with a healthy heart patient diet and regular exercise.
Recommended Reading: Can Tylenol Cause Heart Attack
Symptoms Of Congestive Heart Failure In Dogs
Here are some common signs that your dog might be suffering from congestive heart failure, according to Pet Health Network®:
- Coughing
- Breathing at a fast rate, especially when in a resting state
- Reluctance or refusal to exercise
- Getting tired more easily on walks or during play
- Fatigue
- Coughing up blood
- Collapsing
If you notice any of these symptoms, you should have your dog checked by your vet without delay.
Can Surgery Be Used To Treat Heart Failure

In heart failure, surgery may sometimes prevent further damage to the heart and improve the heart’s function. Procedures used include:
- Coronary artery bypass grafting surgery. The most common surgery for heart failure caused by coronary artery disease is . Although surgery is more risky for people with heart failure, new strategies before, during, and after surgery have reduced the risks and improved outcomes.
- Heart valve surgery. Diseased heart valves can be treated both surgically and non-surgically .
- Implantable left ventricular assist device . The LVAD is known as the “bridge to transplantation” for patients who haven’t responded to other treatments and are hospitalized with severe systolic heart failure. This device helps your heart pump blood throughout your body. It allows you to be mobile, sometimes returning home to await a heart transplant. It may also be used as destination therapy for long-term support in patients who are not eligible for transplant.
- Heart transplant. A heart transplant is considered when heart failure is so severe that it doesn’t respond to all other therapies, but the person’s health is otherwise good.
Also Check: Can Tylenol Lower Heart Rate
The Ticker Tapes Podcast
Claire Berouche’s life changed in ways she could never have imagined following a family afternoon at the cinema. Claire was given the shock news that she had suffered a heart attack and subsequently heart failure which is irreversible. Hear her story and other real experiences from people living with heart and circulatory diseases.
Why Its Important To Know Your Ef
If you have a heart condition, it is important for you and your doctor to know your EF. Your EF can help your doctor determine the best course of treatment for you. Measuring your EF also helps your healthcare team check how well our treatment is working.
Ask your doctor how often you should have your EF checked. In general, you should have your EF measured when you are first diagnosed with a heart condition, and as needed when your condition changes.
Read Also: Does Acetaminophen Raise Your Blood Pressure
Stages C And D With Preserved Ef
Treatment for patients with Stage C and Stage D heart failure and reserved EF includes:
- Treatments listed in Stages A and B.
- Medications for the treatment of medical conditions that can cause heart failure or make the condition worse, such as atrial fibrillation, high blood pressure, diabetes, obesity, coronary artery disease, chronic lung disease, high cholesterol and kidney disease.
- Diuretic to reduce or relieve symptoms.
YOU ARE THE MOST IMPORTANT PART OF YOUR TREATMENT PLAN!
It is up to you to take steps to improve your heart health. Take your medications as instructed, follow a low-sodium diet, stay active or become physically active, take notice of sudden changes in your weight, live a healthy lifestyle, keep your follow-up appointments, and track your symptoms. Talk to your healthcare team about questions or concerns you have about your medications, lifestyle changes or any other part of your treatment plan.
Symptoms Of Congestive Heart Failure
The symptoms of congestive heart failure are also associated with other diseases and ailments.
In the early stages of congestive heart failure, there is a possibility that you might not feel any changes or symptoms. But as the disease progresses, symptoms appear.
Following symptoms would indicate a person has congestive heart failure:
Recommended Reading: How Does Heart Rate Affect Blood Pressure
Teamwork Exercise And Diet
Treatment of CHF may be the best example in medicine where optimal outcomes are achieved by the patient and physician working together.
The patients role in this partnership is crucial. Heres what patients can do to feel better and make sure their treatment is as effective as possible:
- The single most critical thing is to avoid dietary salt . Sodium consumption directly relates to fluid retention, which can tax a weakened heart.
- Weigh themselves daily to monitor their fluid status and weight, and report changes as soon as possible to their care team.
- Take medications as directed and see their doctor for regular checkups to stay on top of the disease.
- Get cardiac rehabilitation early and exercise regularly thereafter. Exercise has clearly been shown to decrease symptoms, optimize physical conditioning around an imperfect heart and prolong life.
- Lose weight, maintain an optimal weight and maintain a healthy diet and lifestyle. All are critically important to long-term symptom relief and survival.
Congestive Heart Failure Treatment
While congestive heart failure is a chronic, long-term condition, you can live a longer and healthier life with proper management. Treatment depends on the individual patient and their current stage of heart failure, but typical management plans include drugs and medication, surgery and lifestyle changes. Talk to your health care provider about your particular options.
You May Like: Tylenol Heart Rate
Stage 1 Of Congestive Heart Failure
If youve been diagnosed with stage one of congestive heart failure, it is because a doctor has noticed a weakness in your heart. This news may be surprising, as stage one of CHF does not exhibit any symptoms. Although CHF cannot be cured, you can make healthy lifestyle changes and take certain medication to manage this condition.
Complications Of Acute Heart Failure
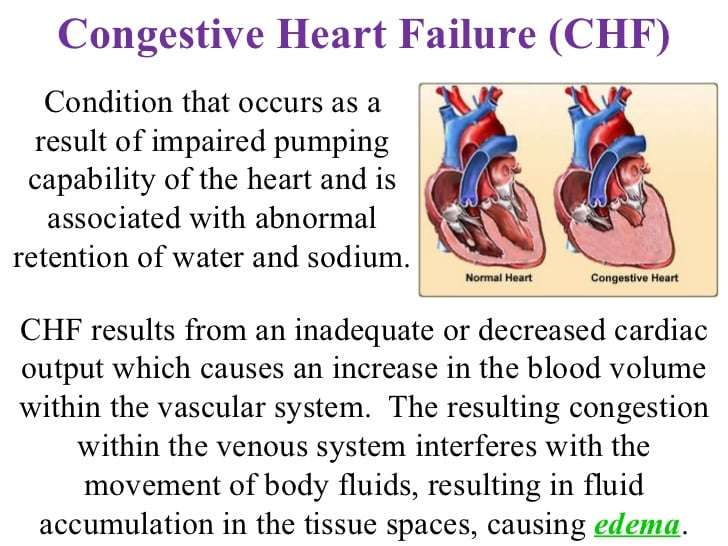
Acute heart failure can cause other conditions, often as a consequence of fluid building up in different parts of the body.
Pulmonary edema
If fluid builds up in the lungs, this causes a very serious condition called pulmonary edema. Fluid is pushed into air sacs which reduces the lungsâ ability to transfer oxygen into the blood. This leads to shortness of breath, particularly when lying down. Other symptoms can include:
- Coughing or, in some cases, coughing up blood
- Wheezing
- Anxiety
- Swelling in the legs or abdomen
Pulmonary edema can be life-threatening. Anyone showing signs of pulmonary edema should see a doctor immediately.
Ascites
Acute heart failure can cause a buildup of fluid in the abdominal cavity. This is called ascites and can cause pain in the abdomen, bloating and shortness of breath.
Cardiorenal syndrome
Around one in four people who have acute heart failure also experience a significant worsening of kidney function, known as cardiorenal syndrome. The older a person is, the higher their risk of developing cardiorenal syndrome. The risk is increased if the person also has:
Cardiohepatic syndrome
Acute heart failure can lead to a worsening of liver function. Liver cells can be destroyed through pressure building up due to blood slowing down before entering the heart, which is a very serious condition. It can cause:
Read Also: Beta Blockers Congestive Heart Failure
What Are The Stages Of Heart Failure
Heart failure is a chronic long-term condition that gets worse with time. There are four stages of heart failure . The stages range from “high risk of developing heart failure” to “advanced heart failure,” and provide treatment plans. Ask your healthcare provider what stage of heart failure you are in. These stages are different from the New York Heart Association clinical classifications of heart failure that reflect the severity of symptoms or functional limits due to heart failure.
As the condition gets worse, your heart muscle pumps less blood to your organs, and you move toward the next stage of heart failure. You cannot go backwards through the stages. For example, if you are in Stage B, you cannot be in Stage A again. The goal of treatment is to keep you from progressing through the stages or to slow down the progression.
Treatment at each stage of heart failure may involve changes to medications, lifestyle behaviors and cardiac devices. You can compare your treatment plan with those listed for each stage of heart failure. The treatments listed are based on current treatment guidelines. The table outlines a basic plan of care that may apply to you. If you have any questions about any part of your treatment plan, ask a member of your healthcare team.
Nitrates Apresoline Beta Blockers And Inotropes Drugs For Congestive Heart Failure
Nitrates are venous vasodilators that include isosorbide mononitrate and isosorbide dinitrate . They are commonly used in combination with an arterial vasodilator, such as hydralazine .
- Nitroglycerin is a nitrate preparation that is administered to treat acute chest pain, or angina.
Hydralazine is a smooth muscle arterial vasodilator that may be used for congestive heart failure. Clinical trial data has shown hydralazine plus nitrates to be especially effective in African-Americans with heart failure, when used in addition to ACE inhibitors or ARBs.
- Isosorbide dinitrate and hydralazine is a fixed dose combination of isosorbide dinitrate and hydralazine . This drug is indicated for heart failure in African-Americans based in part on results of the African American Heart Failure Trial .
- Hydralazine is also especially valuable in patients who have poor kidney function and/or are intolerant to ACE inhibitors and ARBs.
Beta-blockers: These drugs slow down the heart rate, lower blood pressure, and have a direct effect on the heart muscle to lessen the workload of the heart. Specific beta-blockers, such as carvedilol and long-acting metoprolol , have been shown to decrease symptoms, hospitalization due to congestive heart failure, and deaths. Other beta-blockers include bispropolol , atenolol , propranolol , and , but they are generally not used with significant congestive heart failure.
Getting the most out of congestive heart failure medications involves the following:
You May Like: Each Square On Ecg
