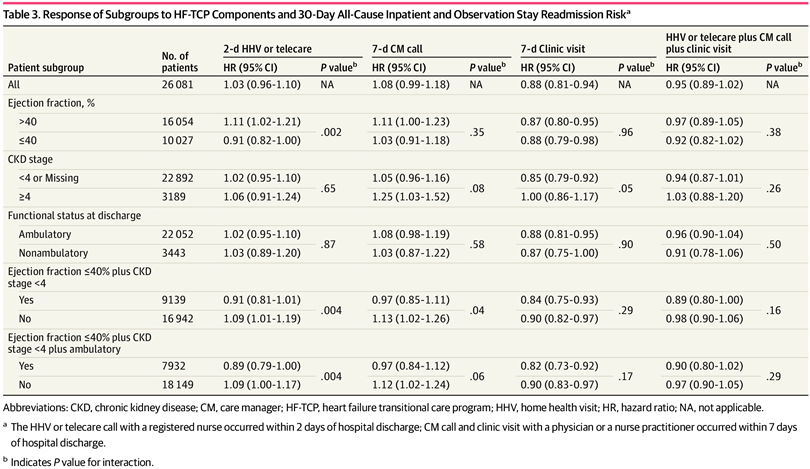
Monitoring Of Clinical Status Of Patients Hospitalized Due To Acute Heart Failure
Recommendations regarding monitoring of clinical status of patients hospitalized due to acute heart failure
| ; |
Patients should be weighed daily and an accurate fluid balance chart should be maintained. Renal function should preferably be monitored with daily measurement of BUN/urea, creatinine and electrolytes. Routine use of a urinary catheter is not recommended.
Renal function is commonly impaired at admission, but may improve or deteriorate with diuresis. Routine monitoring of pulse, respiratory rate and blood pressure should continue. There is no study showing the usefulness of invasive haemodynamic monitoring in patients with AHF excluding those with cardiogenic shock. There is evidence that measuring NPs during the hospital admission may help with discharge planning. Patients whose NP concentrations fall during admission have lower cardiovascular mortality and readmission rates at 6 months.
Study Population And Protocol
Our study population consisted of 152 consecutive patients with CHF confirmed by experienced cardiologists according to the established HF diagnostic criteria from the most recent guidelines of the American College of Cardiology/American Heart Association 11 between October 23, 2019, and January 16, 2020. HF patients with an LV ejection fraction <40%, 40%LVEF<50% and LVEF50% were categorized as HFrEF , HFmrEF and HFpEF , respectively. In addition, 30 patients were excluded because of severe mitral stenosis , constrictive pericarditis , atrial fibrillation , the use of mechanical ventilation, pacemaker implantation , heart valve replacement , gravidity , and a lack of echocardiographic data . In total, 122 patients with CHF were enrolled. The study protocol adhered to the principles of the Declaration of Helsinki and was approved by the Institutional Review Board of the First Affiliated Hospital of Chongqing Medical University. Informed consent was obtained from each patient.
A Failing Heart Imposes A Load On Breathing
Christie and Meakins were the first to document that patients with congestive HF require larger swings in intrathoracic pressures to achieve a similar tidal volume compared with their healthier counterparts; that is, the distensibility or compliance of the lung is markedly reduced in this population. Since then, many investigators have corroborated their findings, reporting that dynamic lung compliance in HF patients is systematically lower compared with healthy individuals, and appears to worsen during physical exertion . This reduced compliance of the lungs has been attributed to the mechanical constraints imposed on lung inflation due to an enlarged heart ; the erectile nature of an engorged pulmonary and/or bronchial vasculature; the development of pulmonary interstitial edema, particularly during exercise; and remodeling of the lung parenchyma due to elevated circulating cytokines and/or chronic hydrostatic insult . The primary consequence of such decreased lung compliance in HF patients is an increased elastic load imposed on the respiratory muscles during inspiration.
Don’t Miss: How Long Do People Live With Congestive Heart Failure
Prevalence Of Augmented Peripheral Chemosensitivity
In clinical studies, PChS is defined as augmented if its numerical value exceeds mean;+;two standard deviations based on data obtained from an age-matched and gender-matched healthy population. This equates to cut-offs between 0.68 and 0.77;l;min1 per peripheral capillary oxygen saturation for the most commonly employed assessment methods. When using the above definition, the prevalence of augmented PChS in HF population is estimated at 4044%. Importantly, the prevalence of elevated PChS has not changed significantly over the last two decades, despite significant advances in the pharmacotherapy of HF and despite introduction of effective coronary and electrophysiological interventions . This underscores the futility of currently available treatment modalities in correcting autonomic imbalances seen in systolic HF.
What Mental Health Disorders Are Related To Heart Disease
Some of the most commonly studied mental health disorders associated with heart disease or related risk factors include the following:*
Mood Disorders: People living with mood disorders, such as major depression or bipolar disorder, find that their mood affects both psychological and mental well-being nearly every day for most of the day.
Anxiety Disorders: People respond to certain objects or situations with fear, dread, or terror. Anxiety disorders include generalized anxiety, social anxiety, panic disorders, and phobias.
Post-Traumatic Stress Disorder : People can experience PTSD after undergoing a traumatic life experience, such as war, natural disaster, or any other serious incident.
Chronic Stress: People are in a state of uncomfortable emotional stressaccompanied by predictable biochemical, physiological, and behavioral changesthat is constant and persists over an extended period of time.
*There may be other behavioral health disorders, such as substance use disorders, that are connected to heart disease.
Read Also: What Does A Slow Heart Rate Mean
A Failing Heart Breathes Too Much
Exercise hyperventilation is a hallmark of the failing heart. Several mechanisms have been proposed as mediators of this excessive ventilatory response, including 1) alveolar ventilation-perfusion mismatching , 2) increased humoral stimuli due to skeletal muscle hypoperfusion and deconditioning , 3) juxta-capillary receptor stimulation consequent to pulmonary vascular congestion and/or hypertension , 4) augmented central and peripheral chemosensitivity , and 5) an inordinately high degree of afferent neural traffic originating from within the locomotor muscles . It is difficult to comment on the relative contributions of these factors to exercise hyperventilation in HF. It is likely that their contributions depend on the clinical status of the patient , and vary with disease severity . Nevertheless, the following is clear: the HF patient breathes too much during exercise. And the problem with breathing too much is straightforward: a higher ventilatory demand begets an increase in the mechanical work expended by respiratory muscles at a given external work rate. However, not only is respiratory muscle work greater in HF patients due to exercise hyperventilation, but the work contributed by the respiratory muscles at a given level of Ve is also inherently higher in this population .
Data And Statistical Analysis
Statistica 10 , LabChart Pro and MATLAB were used to analyse the data. Variables were expressed as the mean and standard error of the mean for repeated measurements before and after CB resection. In cases where repeated data were not available , a baseline value for that particular variable was not taken into account. Thus in some statistical comparisons <10 participants were taken into account . t-test for dependent samples and Wilcoxon matched pairs test were performed depending on the type of distribution to assess differences in measured parameters after CB resection compared with baseline. A P-value <0.05 was considered statistically significant. Due to small sample size, statistical analysis was performed only in combined CBu and CBb groups.
Read Also: How Can I Stop Heart Palpitations At Night
Heart Failure With Reduced Ejection Fraction
In HFrEF , global LV systolic dysfunction predominates. The LV contracts poorly and empties inadequately, leading to
-
Increased diastolic volume and pressure
Many defects in energy utilization, energy supply, electrophysiologic functions, and contractile element interaction occur, with abnormalities in intracellular calcium modulation and cAMP production.
Predominant systolic dysfunction is common in heat failure due to myocardial infarction, myocarditis, and dilated cardiomyopathy. Systolic dysfunction may affect primarily the LV or the right ventricle ; LV failure often leads to RV failure.
Heart Failure With Preserved Ejection Fraction
In HFpEF , LV filling is impaired, resulting in
-
Increased LV end-diastolic pressure at rest or during exertion
-
Usually, normal LV end-diastolic volume
Global contractility and hence ejection fraction remain normal .
However, in some patients, marked restriction to LV filling can cause inappropriately low LV end-diastolic volume and thus cause low CO and systemic symptoms. Elevated left atrial pressures can cause pulmonary hypertension and pulmonary congestion.
Diastolic dysfunction usually results from impaired ventricular relaxation , increased ventricular stiffness, valvular disease, or constrictive pericarditis. Acute myocardial ischemia is also a cause of diastolic dysfunction. Resistance to filling increases with age, reflecting both cardiomyocyte dysfunction and cardiomyocyte loss, and increased interstitial collagen deposition; thus, diastolic dysfunction is particularly common among older adults. Diastolic dysfunction predominates in hypertrophic cardiomyopathy, other disorders with ventricular hypertrophy , and amyloid infiltration of the myocardium. LV filling and function may also be impaired if marked increases in RV pressure shift the interventricular septum to the left.
You May Like: What Should My Active Heart Rate Be
Systemic Inflammatory Consequences Of Chronic Kidney Disease
A pro-inflammatory state is already present in early stages of CKD , and is likely an important risk factor for cardiovascular morbidity and mortality on the long term . In HFpEF, a systemic pro-inflammatory state has been proposed to be a critical causal factor in coronary microvascular dysfunction as inflammatory cytokines can directly induce endothelial cell dysfunction, cause upregulation of adhesion molecules on coronary microvascular endothelial cells, and reduce NO bioavailability, resulting in impaired vasodilation and pro-fibrotic signaling .
Figure 2. A proposed schematic overview of the pathological mechanisms that underlie the progression of CKD to HFpEF. Blue box depicts renal factors; green box depicts coronary microvascular factors; and red box depicts myocardial changes contributing to HFpEF. AGEs, advanced glycation products; CKD, chronic kidney disease; EC, endothelial cell; FGF-23, fibroblast growth factor 23; HFpEF, heart failure with preserved ejection fraction; LV, left ventricle; NO, nitric oxide; RAAS, renin-angiotensin-aldosterone system; ROS, reactive oxygen species; VSMC, vascular smooth muscle cell.
Other Treatments Recommended In Selected Symptomatic Patients With Heart Failure With Reduced Ejection Fraction
7.3.1 Diuretics
Diuretics are recommended to reduce the signs and symptoms of congestion in patients with HFrEF, but their effects on mortality and morbidity have not been studied in RCTs. A Cochrane meta-analysis has shown that in patients with chronic HF, loop and thiazide diuretics appear to reduce the risk of death and worsening HF compared with placebo, and compared with an active control, diuretics appear to improve exercise capacity.,
Loop diuretics produce a more intense and shorter diuresis than thiazides, although they act synergistically and the combination may be used to treat resistant oedema. However, adverse effects are more likely and these combinations should only be used with care. The aim of diuretic therapy is to achieve and maintain euvolaemia with the lowest achievable dose. The dose of the diuretic must be adjusted according to the individual needs over time. In selected asymptomatic euvolaemic/hypovolaemic patients, the use of a diuretic drug might be discontinued. Patients can be trained to self-adjust their diuretic dose based on monitoring of symptoms/signs of congestion and daily weight measurements.
Doses of diuretics commonly used to treat HF are provided in Table;. Practical guidance on how to use diuretics is given in Web Table;7.7.
7.3.2 Angiotensin receptor neprilysin inhibitor
7.3.3 If-channel inhibitor
Practical guidance on how to use ivabradine is given in Web Table;7.8.
Also Check: Does Your Heart Rate Increase When Pregnant
What Can Be Done For People With Mental Health Disorders
Addressing mental health disorders early by providing access to appropriate services and support to increase healthy behaviors can reduce someones risk of experiencing a heart disease event.13,15,17,19,28,38-40
Below are some actions that health care systems, health care professionals, individuals, and researchers can take to promote heart disease prevention and support mental health.
Mechanical Cost Of Breathing With Heart Failure
Fig. 2.The work and power of breathing during graded exercise in patients with heart failure and healthy age-matched control subjects. Data are presented as means±SE *P< 0.05, compared with control group.
HF patients hyperventilate during exercise.
The Wb and Pb are inordinately higher during exercise in HF.
The higher mechanical cost of breathing is primarily due to an increased resistive load to breathing.
Respiratory and limb muscles may compete for an adequate share of cardiac output during exercise in patients with HF.
You May Like: How Long Can Heart Attack Last
Algorithm For The Diagnosis Of Heart Failure
4.3.1 Algorithm for the diagnosis of heart failure in the non-acute setting
An algorithm for the diagnosis of HF in the non-acute setting is shown in Figure;. The diagnosis of HF in the acute setting is discussed in Section 12.
Diagnostic algorithm for a diagnosis of heart failure of non-acute onset
For patients presenting with symptoms or signs for the first time, non-urgently in primary care or in a hospital outpatient clinic , the probability of HF should first be evaluated based on the patient’s prior clinical history , presenting symptoms , physical examination and resting ECG. If all elements are normal, HF is highly unlikely and other diagnoses need to be considered. If at least one element is abnormal, plasma NPs should be measured, if available, to identify those who need echocardiography .,
4.3.2 Diagnosis of heart failure with preserved ejection fraction
The diagnosis of HFpEF remains challenging. LVEF is normal and signs and symptoms for HF are often non-specific and do not discriminate well between HF and other clinical conditions. This section summarizes practical recommendations necessary for proper diagnosis of this clinical entity in clinical practice.
Patients with HFpEF are a heterogeneous group with various underlying aetiologies and pathophysiological abnormalities. Based on specific suspected causes, additional tests can be performed ., However, they can only be recommended if the results might affect management.
What Is The Connection Between Mental Health Disorders And Heart Disease
A large and growing body of research shows that mental health is associated with risk factors for heart disease before a diagnosis of a mental health disorder and during treatment. These effects can arise both directly, through biological pathways, and indirectly, through risky health behaviors.5
People experiencing depression, anxiety, stress, and even PTSD over a long period of time may experience certain physiologic effects on the body, such as increased cardiac reactivity , reduced blood flow to the heart, and heightened levels of cortisol. Over time, these physiologic effects can lead to calcium buildup in the arteries, metabolic disease, and heart disease.1,6-11
Evidence shows that mental health disorderssuch as depression, anxiety, and PTSDcan develop after cardiac events, including heart failure, stroke, and heart attack.5,12-20 These disorders can be brought on after an acute heart disease event from factors including pain, fear of death or disability, and financial problems associated with the event.5,16
Some literature notes the impact of medicines used to treat mental health disorders on cardiometabolic disease risk. The use of some antipsychotic medications has been associated with obesity, insulin resistance, diabetes, heart attacks, atrial fibrillation, stroke, and death.21
Also Check: How Does High Blood Pressure Affect The Heart
Clinical Associations Between Chronic Kidney Disease Coronary Microvascular Dysfunction And Heart Failure With Preserved Ejection Fraction
It should be noted however, that in addition to decreased diastolic function, both hemodialysis and pre-dialysis CKD patients show impaired regional systolic function measured by longitudinal, circumferential, and radial strain while ejection fraction was preserved . Similarly, patients with HFpEF can also display signs of systolic dysfunction defined by decreased global longitudinal strain and Sâ² velocity measured with tissue Doppler. Unger et al. showed in a large group of HFpEF patients that not only diastolic dysfunction, but also the severity of systolic dysfunction and mortality increased in parallel with CKD stage .
Chronic Kidney Disease As A Risk Factor For Heart Failure With Preserved Ejection Fraction: A Focus On Microcirculatory Factors And Therapeutic Targets
- 1Division of Experimental Cardiology, Department of Cardiology, Erasmus MC University Medical Center, Rotterdam, Netherlands
- 2Department of Internal Medicine, Erasmus MC University Medical Center, Rotterdam, Netherlands
- 3Division of Neonatology, Department of Pediatrics, Erasmus MC University Medical Center, Rotterdam, Netherlands
- 4Department of Nephrology and Hypertension, University Medical Center Utrecht, Utrecht, Netherlands
You May Like: What Is A Typical Resting Heart Rate For A Healthy Individual
Atrial Natriuretic Peptide And B
ANP and BNP are endogenously generated peptides activated in response to atrial and ventricular volume/pressure expansion. ANP and BNP are released from the atria and ventricles, respectively, and both promote vasodilation and natriuresis. Their hemodynamic effects are mediated by decreases in ventricular filling pressures, owing to reductions in cardiac preload and afterload. BNP, in particular, produces selective afferent arteriolar vasodilation and inhibits sodium reabsorption in the proximal convoluted tubule. It also inhibits renin and aldosterone release and, therefore, adrenergic activation. ANP and BNP are elevated in chronic heart failure. BNP especially has potentially important diagnostic, therapeutic, and prognostic implications.
For more information, see the Medscape Drugs & Diseases article Natriuretic Peptides in Congestive Heart Failure.
Heart Disease And Mental Health Disorders
Mental health is an important part of overall health and refers to a persons emotional, psychological, and social well-being. Mental health involves how we think, feel, act, and make choices.
Mental health disorders can be short- or long-term and can interfere with a persons mood, behavior, thinking, and ability to relate to others. Various studies have shown the impact of trauma, depression, anxiety, and stress on the body, including stress on the heart.1-3
You May Like: What Causes Your Heart Rate To Drop
Clinical Importance Of Augmented Peripheral Chemosensitivity
Patients with high PChS are characterized by low sensitivity of arterial baroreceptors, which might be the consequence of close anatomical proximity of structures within the central nervous system that are involved in both reflex arcs, such as nucleus tractus solitarii, hypothalamic defence area, reticular formation and ventrolateral medulla oblongata. This relation is reciprocal, as baroreceptor stimulation inhibits chemoreceptor activation and chemoreceptor excitement diminishes baroreflex-mediated inhibition of the sympathetic system . In HF syndrome, low baroreflex sensitivity constitutes a well-established predictor of poor prognosis and haemodynamic instability .
Furthermore, HF patients with augmented level of PChS are prone to ventricular and supraventricular arrhythmias including atrial fibrillation . This may be caused by co-existence of an increased sympathetic tone known to promote cardiac dysrhythmias in the HF population . Alternatively, it may be related to more advanced morphological changes of the myocardium increasing the probability of proarrhythmic substrate formation .
D Physical Examination Findings

Physical examination in Heart Failure
Vital Signs
Pulse: A careful assessment of the arterial pulse rate, rhythm, volume, or character can provide information about the underlying LV pump function, valvular abnormalities, and hemodynamics.
Pulse Rate: Sinus tachycardia is a common feature in patients with acute heart failure and reflects activation of the sympathetic nervous system in response to reduced cardiac output. However, tachycardia may not be prominent in patients who have been adequately beta-blocked.
Chronic tachyarrhythmia in patients with left ventricular dysfunction should raise the suspicion of tachycardia-mediated cardiomyopathy. Bradycardia can result from the use of beta-blockers or may be related to heart block that can occasionally be a precipitating factor for heart failure.
Pulse Rhythm: Sinus arrhythmia is a variation of the pulse rate with breathing and is common in children and adolescents, as well as the physically fit. An irregularly irregular rhythm, often occurring with changing pulse volume, could indicate atrial fibrillation, which is common in patients with heart failure.
Frequent ventricular ectopies are another source of irregular pulse. If they occur frequently as in bigeminy or trigeminy, the pulse can be regularly irregular and the pulse deficit in this setting can be appreciated by simultaneous precordial auscultation and palpation of a peripheral pulse. Rhythm abnormalities, if suspected, need to be confirmed by an electrocardiogram.
You May Like: What Is A Good Resting Heart Rate By Age
