How To Live Longer With Heart Failure
Everything you need to know about the various stages of heart failure to live longer with the condition.
A congestive heart failure diagnosis doesnt mean your heart has stopped working, it means that your heart is unable to pump enough blood throughout your body.
Heart failure is a scary term, says , a cardiologist at the Cleveland Clinic in Ohio. The condition can worsen if the proper steps arent taken to slow or halt the problem, but it does not mean your life is over.
Congestive heart failure, more simply known as heart failure, occurs when there’s a reduction in blood flow throughout the body because blood flow from the heart slows down. That means blood returning to the heart through the veins backs up, causing congestion in the body’s tissues. That congestion may cause swelling in the ankles, legs, or stomach, as well as fluid in the lungs that causes trouble breathing.
Life expectancy with congestive heart failure varies depending on the severity of the condition, genetics, age, and other factors. According to the Centers for Disease Control and Prevention , around one-half of all people diagnosed with congestive heart failure will survive beyond five years. Only around 10 percent of people diagnosed with the condition survive at least 10 years, according to a study published in August 2013 in the journal Circulation Research.
What Can Hospice Do For A Patient With Heart Disease
Your hospice team evaluates the patients status and updates the plan of care as symptoms and conditions change, even on a day-to-day basis. The goal of hospice is to manage symptoms and relieve physical/emotional distress so patients can live as fully as possible, retain their dignity and remain comfortable at home.
The hospice plan of care treats a wide range of symptoms, including:
- Shortness of breath
- Functional decline
- Hypertension
When you turn to hospice, you are not alone in your journey your hospice care team is educated and experienced in advanced cardiac care:
- Monitor and manage your symptoms
- Communicate with your cardiologists office to intervene early and stabilize worsening conditions
- Provide medication, oxygen and other medical equipment related to your heart disease
- Provide services to reduce acute symptoms and avoid re-hospitalization
- Provide an average of 5 home visits per week and proactive phone calls
Hospice offers comprehensive services for patients with heart disease:
How Long Can You Live With Severe Congestive Heart Failure
The life expectancy for congestive heart failure depends on the cause of heart failure, its severity, and other underlying medical conditions. In general, about half of all people diagnosed with congestive heart failure will survive five years. About 30% will survive for 10 years.
Don’t Miss: Does Benadryl Lower Heart Rate
Why Its Important To Know Your Ef
If you have a heart condition, it is important for you and your doctor to know your EF. Your EF can help your doctor determine the best course of treatment for you. Measuring your EF also helps your healthcare team check how well our treatment is working.
Ask your doctor how often you should have your EF checked. In general, you should have your EF measured when you are first diagnosed with a heart condition, and as needed when your condition changes.
Tips For Managing Congestive Heart Failure End

You may be asking, How can I provide comfort to my loved one as they experience the end-of-life signs of congestive heart failure? Its only natural that you as a loved one and/or caregiver will want to be as helpful as possible, and ensure that your loved one is experiencing as little pain as possible. Heres some ways you can help:
- Communicate with the doctors and healthcare professionals: Your loved one may be too weak, or simply forget, to communicate their symptoms to the doctors and nurses. You can help by sharing this information with them in order to make sure your loved one gets what they need.
- Provide comfort: Sometimes it is just as simple as spending time with your loved one while watching a TV show, or talking about things they love. These conversations can help in alleviating some of their depression and anxiety.
- Help them remember to take their medicine: There will likely be various pills and medications that your loved one needs to take. You can help by assisting your loved one in staying on schedule.
Read Also: Does Benadryl Lower Heart Rate
Weight Loss Diabetes And Obesity
A 2018 study published in the Canadian Journal of Diabetes suggests that a sustained weight loss of more than 5% of body weight will lead to an improvement in glycemic control and cardiovascular risk factors. By employing healthy lifestyle choices such as exercise, eating a better diet, and other behavior interventions, both weight loss and lowering hemoglobin A1C can be reached.
Medication to manage weight may improve glycemic and metabolic control in both people with diabetes and obese patients, and, when deemed appropriate, bariatric surgery may be an option for obese and diabetic patients.
Before you begin any sort of weight-loss program, consult with your cardiologist and diabetes management team first.
What Happens To Tongue When Dying
In the dying process, the symphony of swallowing becomes a cacophony of weak and mistimed movements. Sometimes the tongue propels saliva backward before the epiglottis has time to cover the airway. Other times, the tongue fails to push at all and saliva trickles down the airway to the lungs in a steady stream.
Recommended Reading: Does Higher Heart Rate Burn More Calories
How Long Can You Live With Congestive Heart Failure
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
Leaking Heart Valves Life Expectancy
- Although a leaky heart valve can have fatal effects, it is usually diagnosed accidentally as it does not have specific signs and symptoms.
- Nearly every person has a small amount of valvular regurgitation which can be effectively managed with the help of suitable diet and exercise
- In some patients, a leaky heart valve remains in the same condition lifelong, not causing any trouble while in some it may develop rapidly leading to heart failure.
Therefore, it can be said that life expectancy with leaking heart valves is quite relative and can vary from person to person.If you are diagnosed with a leaky valve, irrespective of how minor the leak is, it is advisable to keep a regular follow-up with your doctor to be updated about your leaky valve.
You May Like: Can Ibs Cause Heart Palpitations
What Do Symptoms Of End Stage Congestive Heart Failure Look Like
Dyspnea
Dyspnea or shortness of breath can occur both during activity and rest. This is the symptom that often sends patients racing to the hospital late at night. Work with your hospice or palliative care team to manage symptoms at home and avoid these stressful hospital trips.
Chronic Cough
When the heart cannot keep up with the supply of blood moving between it and the lungs, fluid can build up in the lungs. This results in a chronic cough or wheezing that can produce white or pink mucus.
Edema
As the hearts ability to pump slows down, fluid can build up in the body. This creates swelling in the extremities particularly the feet, ankles, legs, or abdomen.
Lack of Appetite
As the digestive system receives less blood, patients may feel full or nauseous. Not wanting to eat is a natural part of the body shutting down, but families often find this distressing. Learn more about why it is okay for your loved one to stop eating and drinking at end of life.
High Heart Rate
In response to a loss in pumping capacity, the heart begins to beat faster. The patient experiences this as a racing or throbbing heartbeat.
Confusion
When the heart stops working effectively, it can change sodium levels in the blood. This leads to memory loss, confusion, and a general feeling of disorientation.
Stages Of Heart Failure
According to statistics, every year about 550,000 people in the United States are diagnosed with heart failure. Some cardiologists describe heart failure by stages. They indicate the risk and/or severity of the condition:
-
A: No signs of structural damage to the heart or symptoms or heart failure, but you are at high risk of developing heart failure.
-
B: No signs or symptoms of heart failure, but tissue damage can be seen with imaging tests, such as .
-
C: Symptoms of heart failure and damage to the heart.
-
D: Serious signs and symptoms of heart failure.
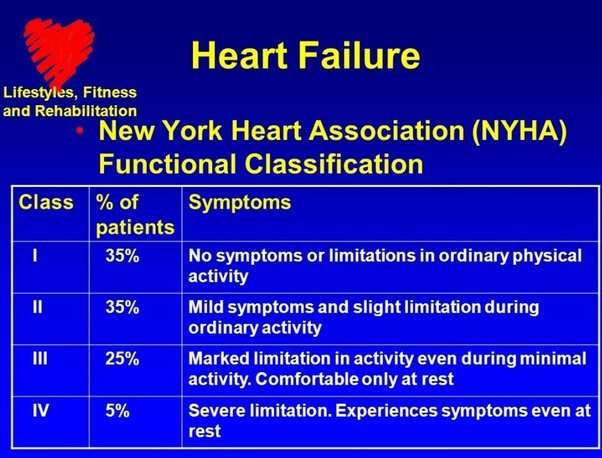
Other doctors use a classification system called the New York Heart Association classification, or functional classification:
-
1: You have but dont have any symptoms and you dont have to limit everyday physical activity.
-
2: You have mild symptoms of heart disease that may slightly limit your regular physical activities.
-
3: You experience enough symptoms to significantly limit your ability to be active. You only feel comfortable when you are resting.
-
4: You have severe symptoms and limitations. You even have symptoms while resting.
Don’t Miss: Can Lexapro Cause Heart Palpitations
When Should I Ask For Help
If you feel you need more support to support the patient, speak to their GP, cardiology team or specialist team.
Some parts of the country have specialist heart failure nurses who can be involved in a persons end of life care, so you may want to see if there is one covering your locality. They can visit people at home, in hospital or a hospice and give the person and their family support and guidance.
If the persons heart failure is due to an inherited heart condition such as hypertrophic cardiomyopathy, their family may have concerns about what the future holds for themselves. Give the family an opportunity to voice their worries and, if its appropriate, mention the possibility of referring immediate family members to a clinic which specialises in inherited heart conditions. This may be done when the person was initially diagnosed.
Inherited heart conditions services offer specialist assessment and investigations, genetic counselling and testing. GPs can refer to this service. Additionally signpost your patient to the British Heart Foundation Genetic Information Service , which offers information and support and helps with referrals.
Treating Congestive Heart Failure Symptomshow Palliative Care Can Help
Palliative care is specialized medical care for people facing a serious illness like CHF. The goal is to improve quality of life for both you and your family. You can have palliative care at any age and at any stage of your illness. You can also have it together with curative treatment.
Palliative care is provided by a team of palliative care doctors, nurses and social workers. They work together with your cardiologist to give you an extra layer of support.
The team has a wide variety of approaches to treating congestive heart failure symptoms. These may include medicines, but not always.
Palliative care teams are expertly trained to manage symptoms, side effects and stresses. For example, they may perform highly effective lymphatic drainage. This is a technique for reducing leg swelling and its associated pain.
Theyll educate you about how to stand, sit and lie down to improve your breathing. Theyll also train you in the use of fans, relaxation methods, meditation and breathing exercises to decrease any anxiety or panic that may accompany feelings of breathlessness.
Read Also: Why Do Av Nodal Cells Not Determine The Heart Rate
How Long Can A Person Live With Congestive Heart Failure
The life expectancy of congestive heart failure patient has not undergone much of the advancements in recent years. The treatment procedures are known to undergo a lot of improvements. However, the life expectancy of the disease remains almost the same. Patients with initial stages of the disease are known to live on an average of five years while patients suffering from the later stages of the disease are reported to live not more than a year or so. Thus early diagnosis along with early treatment is equally important.
How Does Heart Failure Affect Quality Of Life And Lifestyle
With the right care and treatment plan, heart failure may limit your activities, but many adults still enjoy life. How well you feel depends on how well your heart muscle is working, your symptoms and how well you respond to and follow your treatment plan. This includes caring for yourself and living a healthy lifestyle .
Because heart failure is a chronic long-term illness, talk to your doctor and your family about your preferences for medical care. You can complete an advance directive or living will to let everyone involved in your care know your desires. A living will details the treatments you do or dont want to prolong your life. It is a good idea to prepare a living will while you are well in case you arent able to make these decisions at a later time.
Reviewed by a Cleveland Clinic medical professional.
References
Recommended Reading: Flonase Heart Racing
What Are The Overall Benefits Of Hospice Care
If you or a loved one is facing a life-limiting illness, you may have heard the term hospice. Friends or family might have told you about the specialized medical care for patients or the support services for loved ones. But most people are unaware of the many other benefits of hospice.
Comfort. Hospice works with patients and families, providing them the support and resources to assist them through this challenging chapter of life and to helping the patient remain in comfortable and familiar surroundings.
Personal attention. Working with a patient and/or family, the hospice team members become participants in the end-of-life process, a very personal experience for any individual. The hospice mission is to care for each person individually. We listen to patients and loved ones. We advocate for them. We work to improve their quality of life.
Reduced rehospitalization. In the last months of life, some people who are seriously ill make frequent trips to the emergency room others endure repeated hospitalizations. Hospice care reduces rehospitalization: a study of terminally ill residents in nursing homes shows that residents enrolled in hospice are much less likely to be hospitalized in the final 30 days of life than those not enrolled in hospice .2
2Miller SC, Gozalo P, Mor V. Hospice enrollment and hospitalization of dying nursing home patients. American Journal of Medicine 2001 111:38-44
Heart Failure Risk Factors
A recent report published by the American Heart Association estimates that 6.2 million American adults have heart failure, and that number is growing as the U.S. population continues to age. Heart failure is most common in African Americans, individuals with a family history of HF, and those who are 65 and older. It is the number one reason older people are hospitalized.
Unhealthy lifestyle factors and certain medical conditions like diabetes, high blood pressure, chronic kidney disease and obesity are also associated with an elevated risk for HF.
You May Like: What Is A Dangerously High Heart Rate When Exercising
What Exactly Pacemakers Do
Pacemakers help in controlling the heartbeat of a patient. Doctors implant them temporarily for treating a slow heartbeat post heart attack, medicine overdose or surgery. Even in some cases, doctors implant pacemakers permanently for correcting slow heartbeat problems and for the treatment of heart failure in some cases.
Pacemakers monitor the heartbeat of patients and in case if it is excessively slow, pacemaker increases the heart rate by simply sending the necessary electric signals to the heart. Furthermore, most of the pacemakers come with sensors to detect the breathing rate and body motion of patients. Based on the detected signals, pacemakers increase the heart rate when individuals do any physical exercise to fulfill the increased requirement for oxygen and blood in their bodies.
How To Live With Congestive Heart Failure
In order to live with congestive heart failure, one has to make certain lifestyle changes to live a quality life along with medical treatment.
Low Sodium Diet: Low sodium diet should be followed by patients with congestive heart failure. Patients with such a disorder are prone to water retention and edema, thus sodium content should be reduced as it facilitates water retention.
Alcohol:Alcohol consumption should also be restricted and limited, as alcohol can cause harm to the muscles of the heart.
Exercise: Exercise helps in keeping the blood circulation uniform and also helps in maintaining the functioning of the heart. Thus, any form of aerobic exercise can be of help. However, one must be consistent and regular with the exercise. Also, it is important to talk about the exercise plan with the doctor prior starting.
Maintaining Proper Weight: The patient must keep track of his body weight. Increased weight may be a sign of water retention in the body. Thus, it is important to keep checking the body weight to ensure there is not excessive fluid accumulation. If there is an abnormal increase of body weight within few days, it should be reported to the doctor as early as possible.
Monitoring Fluid Intake: It is important for a patient to monitor the fluid intake per day, as excessive fluid intake may lead to its accumulation in the body. Discussions should be made by the doctor about the average and maximum level of fluid intake throughout the day.
You May Like: Why Do Av Nodal Cells Not Determine The Heart Rate
Heart Failure Patients Too Optimistic
Study Shows Patients Overestimate Their Life Expectancy
A new study shows nearly two-thirds of people with congestive heart failure overestimate their remaining life expectancy by an average of 40% compared with what’s realistic based on their prognosis.
Heart failure, which occurs when the heart is too weak to pump enough blood to meet the body’s needs, causes 55,000 deaths each year and indirectly contributes to 230,000 more deaths annually in the U.S.
Although there have been recent improvements in congestive heart failure treatment, researchers say the prognosis for people with the disease is still bleak, with about 50% having an average life expectancy of less than five years. For those with advanced forms of heart failure, nearly 90% die within one year.
“Patient perception of prognosis is important because it fundamentally influences medical decision making regarding medications, devices, transplantation, and end-of-life care,” write researcher Larry A. Allen, MD, MHS, of the Duke Clinical Research Institute and colleagues in The Journal of the American Medical Association.
