How Do I Take Care Of Myself If I Have Right
The most important thing is to make healthy lifestyle habits part of your daily routine. The more you make healthy living part of your new lifestyle, the better youll feel. Try to:
- Work with a nutritionist or dietitian to create a nutritious, filling meal plan you can stick with long-term.
- Find an exercise routine you enjoy so youll be motivated to get moving every day.
- Track and manage your symptoms. Report any changes to your healthcare provider.
- Take medications as instructed.
What Can I Do To Manage Swelling From Extra Fluid
- Elevate your legs above the level of your heart. This will help with fluid that builds up in your legs or ankles. Elevate your legs as often as possible during the day. Prop your legs on pillows or blankets to keep them elevated comfortably. Try not to stand for long periods of time during the day. Move around to keep your blood circulating.
- Limit sodium . Ask how much sodium you can have each day. Your healthcare provider may give you a limit, such as 2,300 milligrams a day. Your provider or a dietitian can teach you how to read food labels for the number of mg in a food. He or she can also help you find ways to have less salt. For example, if you add salt to food as you cook, do not add more at the table.
- Drink liquids as directed. You may need to limit the amount of liquid you drink within 24 hours. Your healthcare provider will tell you how much liquid to have and which liquids are best for you. He or she may tell you to limit liquid to 1.5 to 2 liters in a day. He or she will also tell you how often to drink liquid throughout the day.
- Weigh yourself every morning. Use the same scale, in the same spot. Do this after you use the bathroom, but before you eat or drink. Wear the same type of clothing each time. Write down your weight and call your healthcare provider if you have a sudden weight gain. Swelling and weight gain are signs of fluid buildup.
Heart Failuresigns And Symptoms
Heart failure is a condition in which the heart fails to function properly. The terms “heart failure” and “congestive heart failure ” don’t mean that the heart has actually “failed” or stopped but mean one or more chambers of the heart “fail” to keep up with the volume of blood flowing through them.
Heart failure is brought on by a variety of underlying diseases and health problems.
Your condition may involve the left side, the right side or both sides of the heart. Each side has two chambers:
- An atrium or upper chamber
- A ventricle or lower chamber
Any one of these four chambers may not be able to keep up with the volume of blood flowing through it.
Two types of heart dysfunction can lead to heart failure, including:
- Systolic Heart Failure This is the most common cause of heart failure and occurs when the heart is weak and enlarged. The muscle of the left ventricle loses some of its ability to contract or shorten. In turn, it may not have the muscle power to pump the amount of oxygenated and nutrient-filled blood the body needs.
- Diastolic Failure The muscle becomes stiff and loses some of its ability to relax. As a result, the affected chamber has trouble filling with blood during the rest period that occurs between each heartbeat. Often the walls of the heart thicken, and the size of the left chamber may be normal or reduced.
Don’t Miss: What Should Be Your Resting Heart Rate
Heart Failure With Reduced Ejection Fraction
Symptoms of HFrEF include:
- Shortness of breath
Your healthcare provider will also look for evidence that your left ventricle has reduced pumping power and isn’t able to deliver as much blood as it should. This is usually seen on an echocardiogram.
With HFrEF, the left ventricular ejection fraction is equal to or less than 40%. This means your heart is only pumping 40% or less of the blood it contains out into the body with each beat. This is considered the diagnostic hallmark of HFrEF.
If your echocardiography is inconclusive, your healthcare provider might order more tests. These may include:
- Radionuclide scan
- Cardiopulmonary exercise testing
Classification Based On Course Of The Disease
Heart failure can develop suddenly, for instance after a heart attack or due to certain heart rhythm problems. This is known as acute heart failure.
But it usually develops gradually over time as a result of a different medical problem, such as permanently high blood pressure. This is known as chronic heart failure.
Don’t Miss: With Respect To Heart Rate, Which Of The Following Worked In Opposition To Each Other
Treatments For Heart Failure
Treatment for heart failure usually aims to control the symptoms for as long as possible and slow down the progression of the condition.
How youâre treated will depend on what is causing your heart failure.
Common treatments include:
- lifestyle changes including eating a healthy diet, exercising regularly and stopping smoking
- medicine a range of medicines can help many people need to take 2 or 3 different types
- devices implanted in your chest these can help control your heart rhythm
- surgery such as a or a heart transplant
Treatment will usually be needed for life.
A cure may be possible when heart failure has a treatable cause. For example, if your heart valves are damaged, replacing or repairing them may cure the condition.
How Can You Prevent Heart Failure From Getting Worse
How Can I Prevent Heart Failure From Getting Worse?
Recommended Reading: What Is The Average Resting Heart Rate For Adults
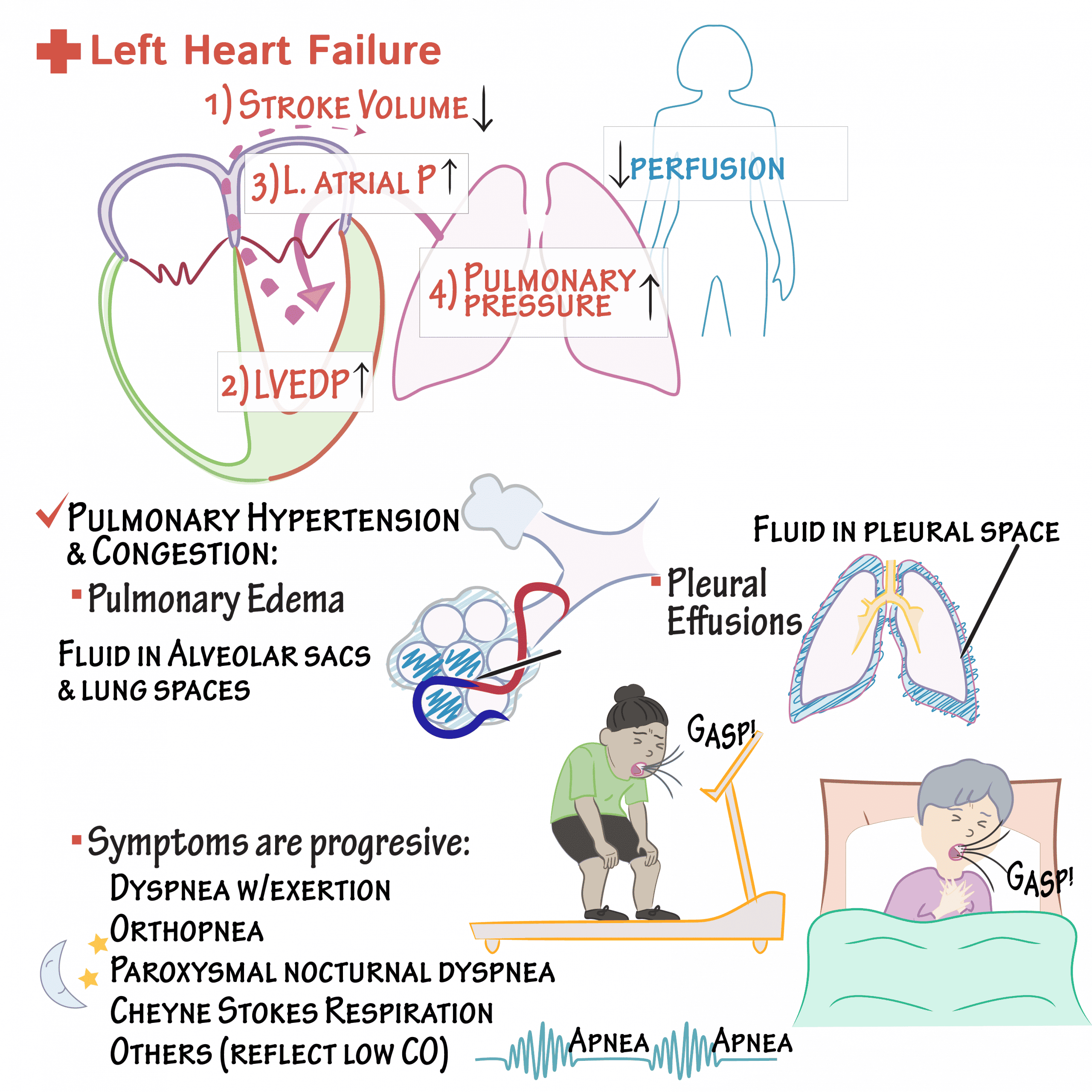
Systolic And Diastolic Failure
Systolic and diastolic heart failure each result in a decrease in stroke volume. This leads to activation of peripheral and central baroreflexes and chemoreflexes that are capable of eliciting marked increases in sympathetic nerve traffic.
Although there are commonalities in the neurohormonal responses to decreased stroke volume, the neurohormone-mediated events that follow have been most clearly elucidated for individuals with systolic heart failure. The ensuing elevation in plasma norepinephrine directly correlates with the degree of cardiac dysfunction and has significant prognostic implications. Norepinephrine, while directly toxic to cardiac myocytes, is also responsible for a variety of signal-transduction abnormalities, such as downregulation of beta1-adrenergic receptors, uncoupling of beta2-adrenergic receptors, and increased activity of inhibitory G-protein. Changes in beta1-adrenergic receptors result in overexpression and promote myocardial hypertrophy.
Dont Miss: Increased Heart Rate When Standing Up
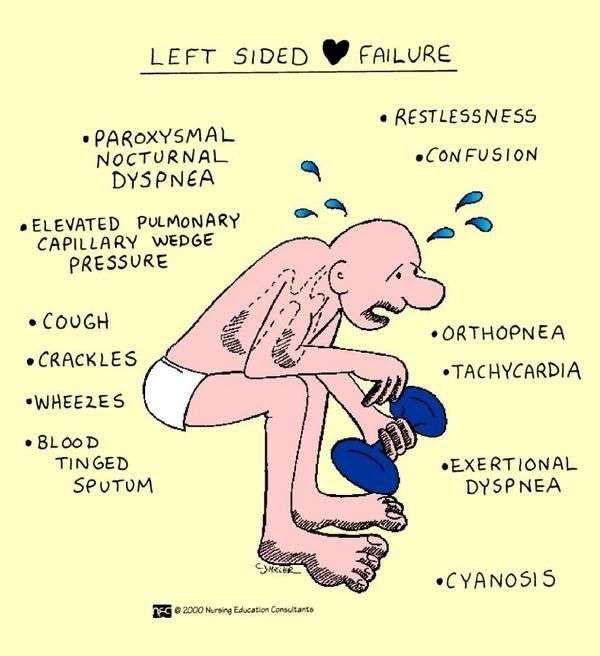
What Are The Symptoms Of Left Ventricular Failure
There are a number of different left-sided heart failure symptoms. As we mentioned earlier, shortness of breath occurs because of fluid backing up into the lungs. This shortness of breath often gets worse at night, so some sufferers have to sleep upright. As time goes on, left-sided heart failure can cause shortness of breath at any time of day even when resting.
Here are the other common symptoms of left ventricular failure:
Some of the symptoms described here are due to forward failure, which means the heart isnt pumping enough of the blood out to other parts of the body. Fatigue, chest discomfort, and a decrease in urine are caused by forward failure.
Other symptoms, such as difficulty breathing, coughing with blood, and weight gain are a result of backward failure, which occurs when the heart isnt receiving enough blood.
Don’t Miss: When Did Bob Harper Have His Heart Attack
Heart Failure During Covid
Your heart failure nurse might have been redeployed, making it hard to have in-person appointments or check-ups. âThe key thing is to look after yourself well, and always phone your GP or heart failure team if your symptoms change or worsen,â says BHF nurse Lucy Martin. âIn fact, call your GP or heart failure team if you have any concerns about your medication or care â they are there to help you.â
Your GP is qualified to answer any questions you might have. Dont worry about wasting their time this is exactly what theyre there for.
- Find out more about coronavirus and how it affects people with heart conditions at our coronavirus support hub.
You May Like: Why Is It Important To Know Your Target Heart Rate
Why Is It Important To Recognize Right Sided Heart Failure
It is important to recognize right-sided heart failure, because its causes, the symptoms it produces, and the treatment it requires, are often different from the more typical, predominantly left-sided types of heart failure. Compared to the left side of the heart, the right heart is rather unimpressive.
Don’t Miss: What Branch Of Medicine Deals With Heart Disease
What Is The Life Expectancy Of Someone With Diastolic Dysfunction
Although there have been recent improvements in congestive heart failure treatment, researchers say the prognosis for people with the disease is still bleak, with about 50% having an average life expectancy of less than five years. For those with advanced forms of heart failure, nearly 90% die within one year.
Comorbidities: Anemia Iron Deficiency Kidney Failure Diabetes Frailty
Moderate anemia is often prevalent in patients with heart failure regardless of HFrEF or HFpEF . The incidence is higher in women, elderly and diabetic patients as well as in patients with renal failure. Increased blood loss in patients treated with oral anticoagulants , aspirin or both as well as decreased absorption of vitamin and/or iron may favor anemia. Similar as in other chronic illnesses iron deficiency is common in heart failure and may influence prognosis worse. Whether anemia and/or iron deficiency are markers of heart failure severity or whether they affect outcome of heart failure disease and thus should be treated is not entirely clear. In patients with heart failure with as well as without anemia intravenous ferric carboxymaltose has improved quality of life and NYHA class but not prognosis .
Heart failure and chronic kidney disease frequently coexist and share many risk factors also. CKD worsen prognosis in heart failure patients however, patients with severe CKD often have been excluded from randomized clinical trials and thus there is limited evidence-based therapy available.
Comorbidities and aging via influencing cognitive and self-care ability affect management of heart failure patients. Also, polypharmacy is present often. In addition, frailty is common in these patients. In consequence, a multidisciplinary team is needed to take care especially for older heart failure patients to reduce hospitalizations and improve outcome.
Don’t Miss: Can Pneumonia Cause Congestive Heart Failure
Types Of Heart Failure
divides heart failure into one of three categories based on the part of your heart thats affected:
- Diastolic failure. This means your left ventricle doesnt relax properly due to stiffness and your heart doesnt fill with enough blood between beats, or the pressure for the heart to function is very high.
- shortness of breath when lying down
- sleeping on extra pillows at night
Diagnosis Of Heart Failure Of Acute Onset
|
Data from Ponikowski P, Voors AA, Anker SD, et al: 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology Developed with the special contribution of the Heart Failure Association of the ESC. European Heart Journal 37:2129-2200, 2016. doi: 10.1093/eurheartj/ehw128 |
You May Like: Laparoscopic Bypass Surgery Heart
How Can I Prevent Left
Living a heart-healthy lifestyle can lower your risk of left-sided heart failure. If youve already experienced this condition, healthy habits can help you avoid future issues.
Steps you can take to prevent left-sided heart failure include:
- Get high blood pressure or coronary artery disease under control.
- Make time for regular physical activity and a good nights sleep.
- Maintain a healthy weight and eat fruits and vegetables.
- Manage stress with deep breathing or relaxation techniques.
- Quitting tobacco if you use it and avoiding secondhand smoke.
Heart Failure With Preserved Ejection Fraction
To make a diagnosis of HFpEF, your healthcare provider looks for:
- The clinical signs and symptoms of heart failure, and
- Evidence that the left ventricle contracts normally, or near normally, and that it pumps out greater than 50% of the blood it contains with each beat, and
- Evidence of reduced diastolic function seen on an echocardiogram
A diagnosis of diastolic heart dysfunction can also be measured invasively, using a catheter, or non-invasively, using doppler imaging techniques. Exercise tests can also help your healthcare provider diagnose your condition.
There are multiple conditions that can contribute to HFpEF, but the most common are:
- High blood pressure
Recommended Reading: Congestive Heart Failure End Stages
Energetic Aspects In Heart Failure
The contractile machinery is dependent on a substrate utilization , oxidative phosphorylation , and high-energy phosphate metabolism . Each of these components or a combination of these may be affected in heart failure and lead to energy starvation and in consequence affect contractile function . Mitochondrial high-energy phosphate production is the predominant energy source for cardiomyocytes. Alterations in the mitochondrial energy support lead to myocyte dysfunction , promote apoptosis and thus may favor heart failure further . Thus, reduced energy levels inhibit Ca2+ influx via the sarcolemmal L-Type calcium channel and reduce sarcoplasmatic Ca2+-re-uptake via reduced phosphorylation of phospholamban. These mechanisms reduce contractility and slower relaxation and may also be the target for treatment options . In patients with heart failure treatments targeting substrate utilization and/or oxidative stress in mitochondria will be tested in addition to the well defined neuroendocrine inhibition .
The Ticker Tapes Podcast
Claire Beroucheâs life changed in ways she could never have imagined following a family afternoon at the cinema. Claire was given the shock news that she had suffered a heart attack and subsequently heart failure which is irreversible. Hear her story and other real experiences from people living with heart and circulatory diseases.
Read Also: Can Covid Cause Heart Palpitations
Read Also: What Causes Fast Heart Rate And Shaking
The Flow Of Blood Through Your Heart
To understand the different types of heart failure, it helps to know how your heart pumps blood:
What Do I Need To Know About Heart Failure
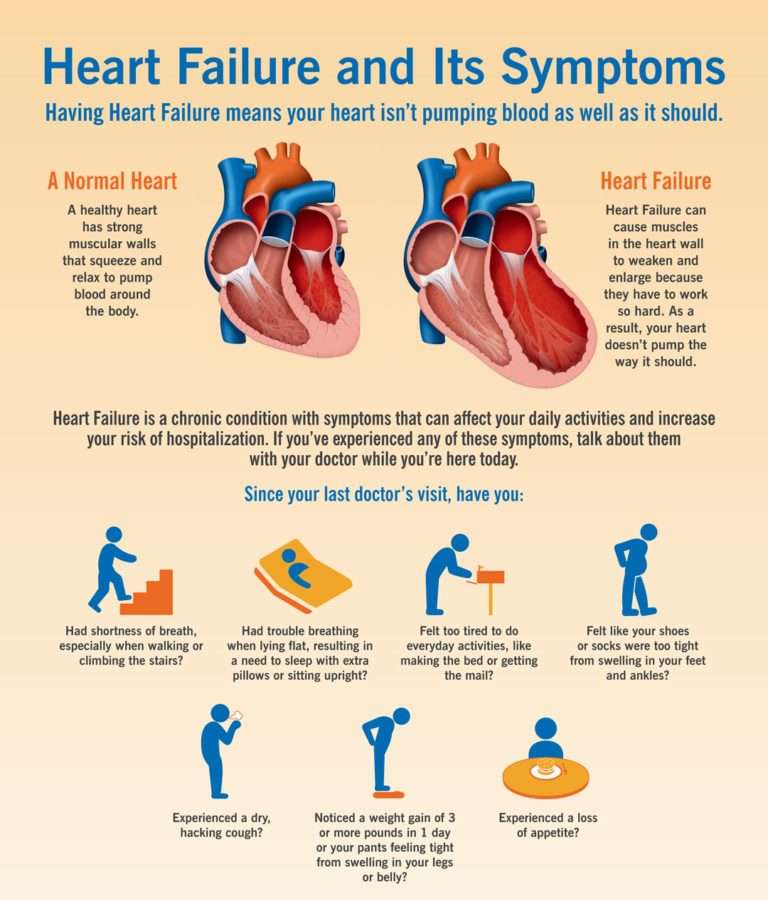
Heart failure is a condition that does not allow your heart to fill or pump properly. Heart failure may begin on the left or right side of the heart. If one side does not work properly, the other side has to work harder to function. Over time, heart failure affects both sides of the heart. Heart failure is a long-term condition that tends to get worse over time. It is important to manage your health to improve your quality of life.
You May Like: Can You Fly After Heart Surgery
Left Ventricular Assist Device
A left ventricular assist device is a mechanical pump operated by a battery that’s implanted via open-heart surgery. There are different types, but they all have four parts, including:
Nyha Functional Classification System
The New York Heart Association functional classification considers heart failure symptoms that happen during exercise to determine stage. Patients can go back and forth between stages depending on how well-controlled symptoms are on a given day.
- Stage 1: The person has heart disease, but it isnt yet causing symptoms or limiting activities.
- Stage 2: The person has mild symptoms that only slightly limit activity.
- Stage 3: The person has significant limitations to activities. He or she is only comfortable when resting.
- Stage 4: The person has major limitations and experiences symptoms when at rest.
Read Also: How Accurate Is Heart Rate On Apple Watch
Also Check: Why Is My Resting Heart Rate Going Up
Frequent Urination At Night
One of the other symptoms of this condition is frequent urination at night, which is also known as nocturia. This is usually seen as an effect of the edema, wherein the fluid that gets accumulated on the ankle and legs returns into systemic circulation when the person is sleeping or is in supine position. This leads to excessive urine being produced, and hence excess urination.
Also Check: What Is My Resting Heart Rate
How To Spot Left Ventricular Heart Failure Signs
This article was medically reviewed by Jonas DeMuro, MD. Dr. DeMuro is a board certified Pediatric Critical Care Surgeon in New York. He received his MD from Stony Brook University School of Medicine in 1996. He completed his fellowship in Surgical Critical Care at North Shore-Long Island Jewish Health System and was a previous American College of Surgeons Fellow.There are 9 references cited in this article, which can be found at the bottom of the page. This article has been viewed 13,697 times.
There are many signs and symptoms that can be indicative of left ventricular heart failure. If you suspect that you may have heart failure, it is important to see a doctor immediately to receive appropriate evaluation and treatment. The diagnosis can be confirmed by a physical exam, as well as blood tests and other imaging and heart function tests.
Read Also: Under Resting Conditions, Heart Rate Is Primarily Under The Control Of What Control System
