Cabg Is Performed If You Have:
1. A stable angina: Chest pain that is certain in terms of occurrence, frequency, duration, severity, and triggering factors is called as a stable angina.
2. Heart attack
3. Extensive blockage: Extensive blockage is when several coronary blood vessels are narrowed, including the main vessels, accompanied by poor pumping function.
4. If your doctor suspects that you are at risk: Based on your limitations while exercising, your doctor will decide if you are at a risk. Also, if your blood pressure is not rising to the required limit while exercising, your doctor may want to perform CABG.
What Is An Ejection Fraction
An ejection fraction is a measurement of the blood pumped out of your heart with each beat, expressed in a percentage. It can be measured using an echocardiogram , multigated acquisition scan, nuclear stress test, magnetic resonance imaging , or during a cardiac catheterization. A normal ejection fraction is between 50% and 70%.
Risk After Hip Replacement Compared To Other Joint Replacements
In a 2021 study , researchers investigated the rates of heart attack among 322,585 people who received spinal fusion or joint replacements. The researchers found that the risk of heart attack was generally higher in people receiving spinal fusion and lower in people receiving knee or hip replacements.
Dont Miss: What Heart Chamber Pushes Blood Through The Aortic Semilunar Valve
You May Like: Grain Free Dog Food Heart Failure
Endoventricular Circular Patch Plasty
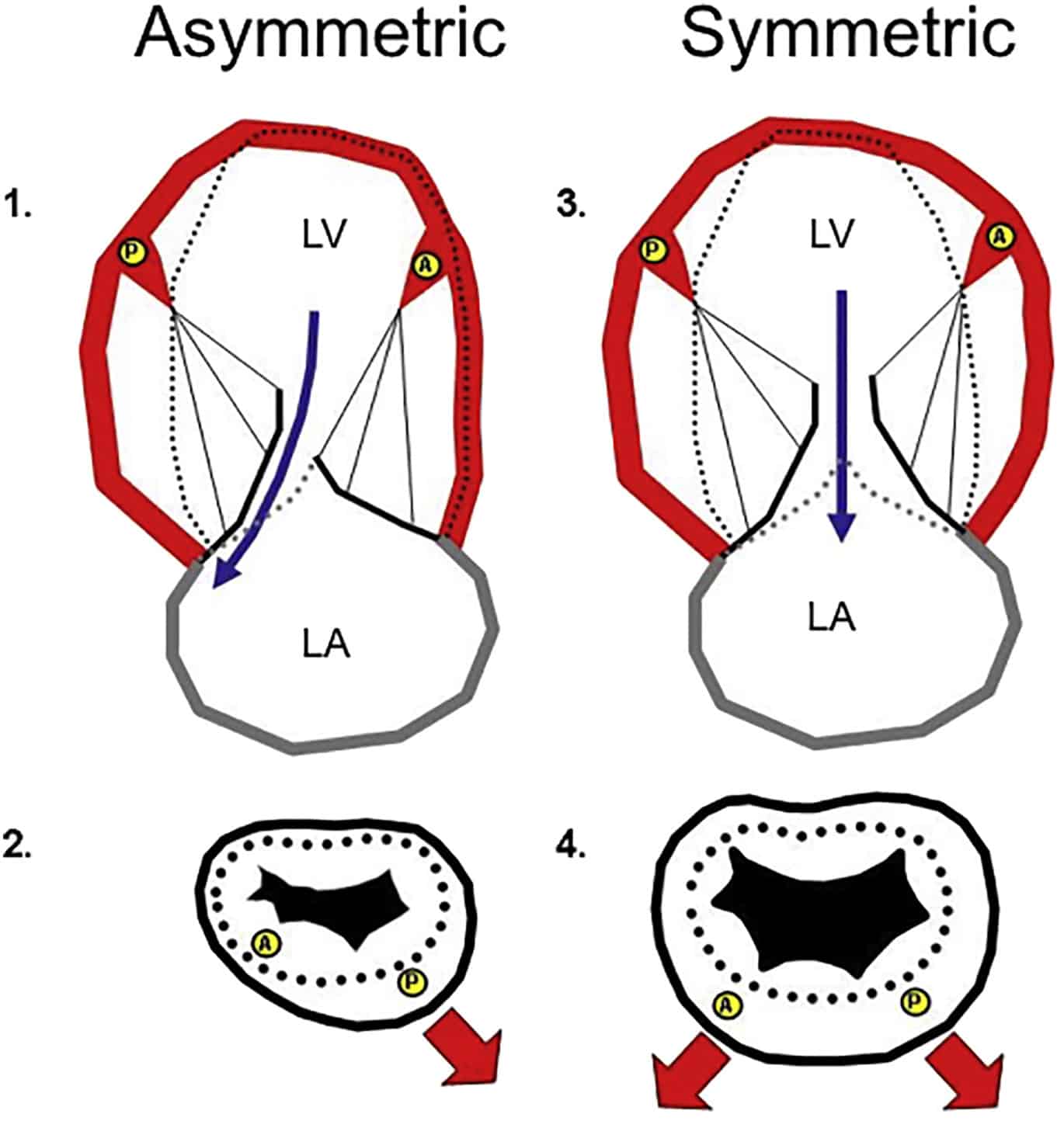
Dor and associates first described the technique of endoventricular circular patch plasty , which is used to treat patients with postinfarction left ventricular scarring. The procedure involves placement of a circular synthetic or autologous-tissue patch, which is anchored in the contractile left ventricular myocardium after the aneurysm has been resected or excluded. Both akinetic and aneurysmal segments may be repaired with this technique, which restores the circular ventricular architecture by excluding the septal scar and adjusting the Laplace relationship. In this manner, the ventricular cavity is reduced in size, improving its wall tension and hemodynamic status, and is rendered more physiologic. When indicated, myocardial revascularization is also performed., The advantages of EVCPP with geometric reconstruction are that this approach allows exclusion of nonresectable scarred areas in the septum uses an intraventricular patch to redirect the normal muscle bundles toward their original orientation and position reduces the size of the ventricular cavity and involves grafts between the infarct territory and remote muscle, which improve contractility and reduce the risk of arrhythmias.
Air Travel Is Generally Safe For Heart Patients With Appropriate Precautions
If you have heart disease, you can fly safely as a passenger on an airplane, but you need to be aware of your risks and take necessary precautions.
Heart conditions that can lead to health emergencies when flying include coronary artery disease , cardiac arrhythmia , recent heart surgery, an implanted heart device, heart failure, and pulmonary arterial disease.
When planning air travel, anxiety about the prevention and treatment of a heart attack on a plane or worrying about questions such as can flying cause heart attacks may give you the jitters. You can shrink your concern about things like fear of having a heart attack after flying by planning ahead.
Recommended Reading: Acute Exacerbation Of Heart Failure
What Are The Options For Heart Failure Surgery
If the patients heart failure has an underlying cause, doctors first consider treating that. That may mean coronary bypass surgery to unblock clogged arteries or, if the condition has been caused by a faulty valve, heart valve repair or replacement.
Other surgical options include:
Left ventricular assist device . LVADs are mechanical devices that supplement the work of the heart. They take over the work of the left ventricle, assuming the responsibility of pumping blood around the body.
An LVAD can be an effective long-term solution for cases of heart failure, or it can be a way to stabilize and improve a patients cardiac health while she waits for a heart transplant to become available.
Some patients come in with late stages of heart disease, and theyre the ones who can benefit from LVAD and transplant, says Pramod Bonde, MD, surgical director of Mechanical Circulatory Support.
Heart transplant. Heart transplantation is a solution that can radically improve a patients heart function and quality of life, but receiving a transplant depends on availability. Donations are tightly regulated, and to be on the list, a patient must be relatively young, have excellent organ function in the rest of the body, and document strong family and social support.
A few years ago, people were dying while waiting for the heart to come, Dr. Bonde says. Now, thanks to LVADs, they have an option that will help them survive.
How Do I Manage Post
A cardiac anesthesiologist is also a pain management specialist for conditions related to surgery. Your anesthesiologist will talk to you about your options for managing post-operative pain. Before your surgery, the anesthesiologist may ask about your pain tolerance to help gauge how best to manage your post-operative pain, guiding decisions such as the proper narcotics dosage, the feasibility of nonnarcotic pain medication options, and the need for nerve blocks.
Although most heart surgeries are major surgeries, they are typically not a source of long-term pain. Even in the short term, the pain may be less severe than with operations on other areas of the body. Opioids are used when necessary, but there are many other pain management options, including:
- Lidocaine infusion
Recommended Reading: Does Hydralazine Lower Heart Rate
How Do I Safely Get Dressed After A Hip Replacement
For dressing, to prevent lifting your knee higher than your hip on the surgery side, you may need a long shoehorn and a dressing stick which will help you with your shoes, socks and pants. Remember to always put your operative leg in your pants first. If you wear shoes with shoe ties, try switching to elastic shoelaces.
What Happens Before Heart Failure Surgery
Your provider will let you know what you need to do to prepare for surgery, including:
- What you can eat and drink.
- Which medications you should take.
- What to bring to the hospital.
Before surgery, youll change into a hospital gown. A nurse will start an intravenous line in your arm or hand so you can receive fluids and any medications you need. The nurse may also:
- Shave the area where the surgeon will make the incision.
- Cleanse the surgical site.
- Cover you with a sterile drape.
For most procedures, youll receive medication to put you to sleep.
Don’t Miss: What Should Your Heart Rate Variability Be
Mental And Behavioral Home Health Services
A congestive heart failure diagnosis comes with a high emotional cost. Its life-changing, and its never easy. Living with congestive heart failure takes a toll on your physical health and your mental health. Centric Healthcare offers compassionate professional services to help as you learn to cope with your new normal. Its important to remember as you live with your disease that you dont need to do it alone. We can help.
To schedule a free consultation and learn more about these and other services offered by Centric Healthcare, call us at 224-5535 in the Twin Cities, or call us at 205-7322 in Rochester.
Also Check: How To Calculate Resting Heart Rate
What Is Heart Failure
Heart failure doesnât mean the heart has stopped working. Rather, it means that the heart works less efficiently than normal. Due to various possible causes, blood moves through the heart and body at a slower rate, and pressure in the heart increases. As a result, the heart canât pump enough oxygen and nutrients to meet the body’s needs.
The chambers of the heart may respond by stretching to hold more blood to pump through the body or by becoming stiff and thickened. This helps to keep the blood moving, but the heart muscle walls may eventually weaken and become unable to pump as efficiently. The kidneys may respond by causing the body to retain fluid and salt. If fluid builds up in the arms, legs, ankles, feet, lungs, or other organs, the body becomes congested. Congestive heart failure is the term used to describe the condition.
Read Also: How To Stop Symptoms Of Heart Attack
How Is Heart Failure Treated
Early diagnosis and treatment can help people with heart failure live longer, more active lives. How heart failure is treated will depend on your type and stage of heart failure .
The goals of treatment for all stages of heart failure are to:
- Treat the underlying cause of your heart failure, such as coronary artery disease , high blood pressure or diabetes
- Reduce your symptoms
- Stop your heart failure from getting worse
- Increase your lifespan and improve your quality of life
For people with any stage of heart failure, treatment will include lifestyle measures, medicines and ongoing care. People who have more severe heart failure also may need medical procedures and surgery.
Dont Miss: Acid Reflux Cause Palpitations
What Happens After Heart Failure Surgery
After surgery, you may go to the hospitals intensive care unit to recover or directly to a hospital room. Your hospital stay will vary based on the type of surgery and your medical condition. You may stay in the hospital overnight or for several weeks. Before going home, some people may need care at a rehabilitation facility to regain their strength.
Before you go home, your healthcare team will give you a detailed plan. This plan will include your follow-up appointments and instructions on how to care for yourself.
Also Check: How Is Heart Failure Diagnosed
Fluid Retention: What It Can Mean For Your Heart
Fluid buildup indicates worsening heart failure. Learn how to spot it and treat it early.
The buildup of excess fluid in your body can take a variety of forms from belly bloating and swollen ankles to nausea, persistent coughing and fatigue. You may be tempted initially to dismiss this hodgepodge of problems as having little to do with your heart. However, they all signal water retention, which can mean trouble for people with a history of heart failure.
Fluid buildup can quickly escalate into a life-threatening situation, says Dr. Eldrin Lewis, a heart failure specialist at Harvard-affiliated Brigham and Womens Hospital.
Heart failure may start with injury from a heart attack or develop as a result of damaged valves, infection or disease of the heart muscle cells. Many times, it is the product of years of toil against high blood pressure and clogged arteries. Regardless of what triggers the decline, heart failure culminates in a progressive weakening of your hearts power to pump.
Consequently, blood circulates through your heart and body more slowly your cells thirst for fresh oxygen and nutrients. To compensate for its weakened state, the heart undergoes a series of structural transformations. Other physical processes also come into play. When the kidneys detect the diminished blood flow, they activate hormones that prompt the body to retain fluid and sodium in an effort to boost the volume of blood in circulation.
Study Design And Cohort Definition
This was an observational cohort study intended to examine the association between pre-existing CVD and the risk of post-operative cardiovascular events among patients who received hip fracture surgery. Each patient with pre-existing CVD was matched for age , gender, fracture type, and year of admission to a hip fracture patient without pre-existing CVD.
Pre-existing CVD was defined as having one of the following diagnosis at admission: coronary heart disease , cerebrovascular events , peripheral artery disease and heart failure, and other cardiovascular diseases . The diagnosis of the above conditions was undertaken by medical specialists based on patient history and medical records or admission results based on electrocardiogram, coronary computed tomography , echocardiogram, and cranial CT/magnetic resonance imaging .
Also Check: Do All Heart Attacks Damage The Heart
How Is Congestive Heart Failure Treated
Doctors will assess the current health status of the patient to establish a baseline, and develop a long-term health plan. This may involve the optimization of medicines and therapies, adding new medication, or possibly enrollment in a clinical trial.
Stabilizing and/or reversing a patients condition often involves long-term, collaborative follow-up with a referring cardiologist or physician.
In serious situations, advanced therapies, which include mechanical solutions, a heart transplant, or hospice, may be offered.
How Common Are Heart Attacks After Surgery
About 3 percent of people undergoing major surgery experience a heart attack during the procedure. Complications become more common with age and in people with a previous history of cardiovascular disease or other risk factors for heart disease.
One in 5 people over 65 or over 45 with a history of cardiovascular disease develop one or more MACE within a year of non-cardiac surgery.
Also Check: How Much Does Open Heart Surgery Cost
Read Also: Newborn Heart Rate Normal
What Is The Prosthesis Made Of
The prosthesis is constructed of metal and plastic. Titanium, stainless steel, cobalt-chromium, ceramic and polyethylene are the most common materials. A prosthesis for a total hip replacement consists of four components:
- Acetabular liner.
- Acetabular shell.
They are linked, but flexible, so that the surgeon can adjust for anything unexpected. The prosthetic is then fixed to the remaining bone using either:
- Fixation to the host bone by relying on a bony ingrowth onto or into the porous surface of the bone that has either been interference-fit or press-fit into the surrounding bone.
- Medical cement , if the original bones quality is low.
Read Also: What Is The Highest Heart Rate Ever Recorded
Treating The Underlying Causes
A number of conditions can contribute to heart failure. Treatment of these other factors may range from surgery or angioplasty to open clogged blood vessels in patients with coronary artery disease to medications prescribed to control high blood pressure, diabetes, anemia or thyroid disease. In addition, it’s particularly important to treat abnormal heart rhythms called arrhythmias in patients with heart failure.
Don’t Miss: Memory Loss After Heart Valve Surgery
Impact Of Heart Failure On Patients Undergoing Major Noncardiac Surgery
Bradley G. Hammill, Lesley H. Curtis, Elliott Bennett-Guerrero, Christopher M. OConnor, James G. Jollis, Kevin A. Schulman, Adrian F. Hernandez Impact of Heart Failure on Patients Undergoing Major Noncardiac Surgery. Anesthesiology 2008 108:559567 doi:
Changes in the demographics and epidemiology of patients with cardiovascular comorbidities who undergo major noncardiac surgery require an updated assessment of which patients are at greater risk of mortality or readmission. The authors evaluated short-term outcomes among patients with heart failure, coronary artery disease , or neither who underwent major noncardiac surgery.
Patients were aged 65 and older, had Medicare fee-for-service coverage, and underwent 1 of 13 major noncardiac procedures from 2000 through 2004, excluding patients with end-stage renal disease and patients who did not have at least 1 yr of Medicare fee-for-service eligibility before surgery. Main outcome measures were operative mortality and 30-day all-cause readmission.
Elderly patients with heart failure who undergo major surgical procedures have substantially higher risks of operative mortality and hospital readmission than other patients, including those with coronary disease, admitted for the same procedures. Improvements in perioperative care are needed for the growing population of patients with heart failure undergoing major noncardiac surgery.
How Can I Improve My Quality Of Life With Heart Failure
There are several things you can do to improve your quality of life if you have heart failure. Among them:
- Eat a healthy diet. Limit your consumption of sodium to less than 1,500 milligrams each day. Eat foods high in fiber. Limit foods high in trans fat, cholesterol, and sugar. Reduce total daily intake of calories to lose weight if necessary.
- Exercise regularly. A regular cardiovascular exercise program, prescribed by your doctor, will help improve your strength and make you feel better. It may also decrease heart failure progression.
- Dont overdo it. Plan your activities and include rest periods during the day. Certain activities, such as pushing or pulling heavy objects and shoveling may worsen heart failure and its symptoms.
- Prevent respiratory infections. Ask your doctor about flu and pneumonia vaccines.
- Take your medications as prescribed. Do not stop taking them without first contacting your doctor.
- Get emotional or psychological support if needed. Heart failure can be difficult for your whole family. If you have questions, ask your doctor or nurse. If you need emotional support, social workers, psychologists, clergy, and heart failure support groups are a phone call away. Ask your doctor or nurse to point you in the right direction.
Also Check: Sternum Pain Years After Open Heart Surgery
Nausea Or Lack Of Appetite
Nausea or lack of appetite can result from the accumulation of fluids in your abdomen.
Several of the signs and symptoms of congestive heart failure can also be associated with other diseases and medical conditions. Therefore, it is important that you see your doctor when any of them present themselves and persist.
If you are being treated for congestive heart failure and any of these signs and symptoms get worse, or if you begin to experience additional signs and symptoms, you should inform your doctor immediately. This can indicate that your heart failure is progressing and that your treatment is not working.
What Are The Risks Of Heart Failure Surgery
Risks include but arent exclusive to death, stroke, bleeding and infection. You may have additional risks, depending on your age and medical condition.
Your surgeon will explain your risks to you before surgery. Let your surgeon know if you have any questions or concerns about the procedure and any potential risks.
Don’t Miss: What Can Be Done For Congestive Heart Failure
What Causes Congestive Heart Failure In Cats
A variety of factors can cause congestive heart failure in cats. It is most commonly caused by a condition in which the walls of the heart thicken , but it can also be caused by thyroid disease, high blood pressure, or birth defects, among other things. Congestive heart failure can occur in cats of any age, breed , or gender, but it is most common in middle-aged to older cats.
CHF can also develop in a heart thats been weakened by other heart conditions, so its essential to do what you can to prevent heart disease from occurring in your pet, including preventing obesity and providing heartworm prevention.
Read Also: What Are The Types Of Heart Attacks
