What Is The General Prognosis Of Congestive Heart Failure
The congestive heart failure is a progressive disease and is demarcated into four classes. With the progression to the next class, the condition of the patient is seen to deteriorate.
Class I The heart failure is mostly not symptomatic apart from the complaint of weakness by the patient.
Class II Patients of congestive heart failure avoid strenuous activities as such lead to heart palpitation and fatigue.
Class III Patients with Class III congestive heart failure are pretty symptomatic where most activities get limited due to the weakness.
Class IV The CHF is characterized by severe symptoms where the patient cannot even carry out basic life activities and experience severe heart palpitations and shortness of breath.
The general prognosis of the disease primarily varies from patient to patient because an amalgamation of factors leads to the disease. Nevertheless what can be definitely said is if the symptoms are brought to notice at an earlier stage, which is followed by early diagnosis. The prognosis will be much better as compared to late diagnosis.
Early diagnosis and early treatment is effective in reducing the symptoms so that the patient can live a quality life.
Living With Congestive Heart Failure: What To Expect
Yes, there are several lifestyle changes you should take into account if youve been diagnosed with congestive heart failure. But remember your diagnosis;doesnt;mean you should necessarily stop doing things you love.
You are supposed to be exercising walking, biking, swimming, or doing light weight exercises, says Mountis. The American Heart Association recommends at least 30 minutes of moderate intensity aerobic activity at least five days a week for optimal heart health. Avoid exercises that make you feel breathless, and make sure to talk to your doctor before starting a new exercise routine.
Your healthcare provider will also likely suggest dietary changes that can help reduce the swelling associated with congestive heart failure and slow the progression of the condition. Those changes may include following a;low- or reduced-salt diet, or reducing how much fluid you drink to lessen the bodys water content.
Other lifestyle changes that can slow the progression of heart failure include:
What Are The Symptoms Of Mild Congestive Heart Failure
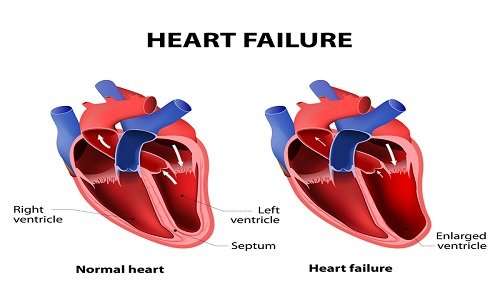
The patient may experience bouts of fluid retention and weight gain, shortness of breath on exertion, and decreased exercise tolerance. Some patients may have significant problems with swelling of their legs. This may lead the patient to depression and frustration because they can no longer do their regular activities and are having to rely more on their families. Sometimes the patient can feel the heart racing as a consequence of the heart function being reduced.
You May Like: How Can I Lower My Heart Rate From Anxiety
How Is Congestive Heart Failure Diagnosed
Patients are generally referred to Dr. Jacoby and his team by another cardiologist, or;from a patients primary care physician.
Initially, the patient will have an intake visit with a heart specialist and nurse or physicians assistant, he says. During this visit, a review of the patients prior records and his or her current health status is incorporated to establish a picture of where the patient is along the spectrum, and then a plan is established for prognosis and treatment. There will later be a discussion with the family, tailored to their needs and desires.”
The process often takes more than one meeting and involves both the;patients local cardiologist or referring physician.
We see thousands of heart patients a year, Dr. Jacoby says. Yale;provides the facilities to best evaluate what is treatable, and we offer cutting-edge treatments once a patient has been diagnosed. We employ advanced cardiac imaging, exercise testing and hemodynamic assessment.
Heart Muscle Disease Or Swelling

Any damage to the heart muscle, whether thanks to drug or alcohol use, viral infections or unknown reasons increases the risk of cardiac arrest.
Congestive Heart Failure Stages of Dying
Though there have been advancements made, 50% of patients with congestive heart failure will have an average life expectancy of five years. For individuals with advanced congestive heart failure, up to 90% will pass away within;one year. Individuals with congestive heart failure at a moderate stage will average;ten years. Death from congestive heart failure is nearly certain. The congestive heart failure stages of dying are as follows:
- Dyspnea
Recommended Reading: What Causes Low Blood Pressure And High Heart Rate
How Common Is Heart Failure
About 920,000 people in the UK currently have heart failure.There are around 67,000 admissions to hospital for heart failure in England and Wales each year. Heart failure becomes more common as people become older. It is commonly diagnosed in people in their 70s. In the UK around one in seven people aged 85 or more have heart failure. In people aged 65-74, around one in 35 have heart failure.
Factors That Can Worsen Symptoms Of Heart Failure
The symptoms of heart failure can be worsened by a number of factors, including:
- anaemia
- too much salt, fluid, or alcohol in the diet
- pregnancy
- some viral and bacterial infections
- kidney diseases
Treatment for heart failure may include:
- medicines, such as;
- diuretics to remove excess fluid and improve symptoms of heart failure
- mineralcortiocoid receptor antagonists are also recommended and used in most patients with heart failure to reduce mortality and hospitalisation
- ACE inhibitors to open up blood vessels, reduce blood pressure and reduce sodium retention and water retention
- certain beta-blockers to slow the heart rate and reduce its work
- aldosterone blockers to reduce blood pressure and reduce the effects of damage to the heart muscle
- ACE inhibitors, beta blockers and aldosterone blockers can increase survival and reduce the likelihood of hospitalisation.
You May Like: Is 116 Heart Rate High
Ways To Fight Fatigue From Congestive Heart Failure
If you’re one of the millions feeling worn out from heart failure, take back the day with these fatigue-fighting heart failure solutions.
The term “heart failure” tends to mislead. After all, people who have it don’t necessarily have a heart that has stopped working rather, their hearts can’t pump blood as well as they should.
Still, it’s serious. As your heart works overtime, it can cause tiredness, shortness of breath and a feeling of being simply worn out.
Such are the signs of fatigue, one of the most common symptoms of congestive heart failure. Nearly six million adults in the U.S. live with heart failure, the Centers of Disease Control and Prevention reports, and many of them feel tired when they do even simple things around the house, such as taking a shower.
But luckily, people can thrive with a heart failure diagnosis and fight fatigue along the way. With a few lifestyle shifts , you can bring back more energy into your day. Ask your doctor what’s right for you, and if they give the go-ahead, try these heart failure solutions to combat fatigue and live an active, exciting life.
1. Eat for Your Heart
If you have congestive heart failure, your doctor has likely already given you guidance for a heart-healthy diet. Generally, that means eating more of the good stuff and less of the bad stuff .
2. Renew Your Energy With Exercise
3. Take a Nap
4. Make Time for Mental Health
5. Get Better Sleep
Taking Back Your Day
Articles On Heart Failure Types & Stages
Congestive heart failure doesn’t mean your heart has stopped. It means it’s not pumping blood the way it should. When that happens, blood and fluid can back up in your body and make it harder for your kidneys to flush out sodium and water. That can make you hold on to too much fluid, which causes swelling.
There’s no cure. But your doctor may give you medication to do things like lower your blood pressure, relax your blood vessels, make your heart beat stronger, or ease swelling. And diet and lifestyle changes — like not smoking — can help, too.
Read Also: What Are Signs Of Heart Failure
Life Expectancy With Congestive Heart Failure
The life expectancy of someone with congestive heart failure depends on the type of heart failure, the cause, the stage of the disease, and how effective treatment is.
When heart failure results from cardiomyopathy or coronary artery disease, a person typically has a less positive outlook than someone with heart failure in its earliest stage.
Devices For Heart Failure
Various devices are implanted in a small number of people with heart failure. Examples include implantable cardioverter defibrillators and pacemakers.
ICDs work by detecting any abnormal heart rhythms that may occur. If your heart rhythm is too slow, the device can give your heart extra support by working as a normal pacemaker. If your heart beats too fast, the ICD can give you a burst of extra beats at a slightly faster rate which should return your heart back to a normal rhythm, or it can give you a shock to restore a regular heartbeat.
Pacemakers work differently. In some cases, there is some damage to the specialised heart cells that carry the signals needed for your heart to squeeze properly. This can then cause the signals to travel out of synch which leads to your heart pumping less forcefully and less efficiently. The pacemakers work to control these signals so the heart can then beat more effectively. This is also known as cardiac resynchronisation therapy.
These different devices have dramatically altered the treatment of heart failure in selected cases and have improved both the outlook and quality of life. However, these devices are only suitable for certain people with heart failure. Your doctor will be able to discuss with you in more detail if you are suitable for one of these devices.
Don’t Miss: How Many People Die From Heart Disease Each Year
Is There A Treatment For Heart Failure
There are more treatment options available for heart failure than ever before. Tight control over your medications and lifestyle, coupled with careful monitoring, are the first steps. As the condition progresses, doctors specializing in the treatment of heart failure can offer more advanced treatment options.
The goals of treating heart failure are to try to keep it from getting worse , to ease symptoms, and to improve quality of life.
Some common types of medicines used to treat it are:
- ACE inhibitors
- Aldosterone antagonists
- ARBs
- ARNIs
- Selective sinus node inhibitors
- Soluble guanylate cyclase stimulator
Your doctor may also recommend a program called cardiac rehabilitation to help you exercise safely and keep up a heart-healthy lifestyle. It usually includes workouts that are designed just for you, education, and tips to lower your chance of heart trouble, like quitting smoking or changing your diet.
Cardiac rehab also offers emotional support. You can meet people like you who can help you stay on track.
Heart Failure Treatment Is A Team Effort
Heart failure management is a team effort, and you are the key player on the team. Your heart doctor will prescribe your medications and manage other medical problems. Other team members — including nurses, dietitians, pharmacists, exercise specialists, and social workers — will help you achieve success. But it is up to YOU to take your medications, make dietary changes, live a healthy lifestyle, keep your follow-up appointments, and be an active member of the team.
If you notice anything unusual, don’t wait until your next appointment to discuss it with your doctor. Call them right away if you have:
- Unexplained weight gain
- Swelling in your ankles, feet, legs, or belly that gets worse
- Shortness of breath that gets worse or happens more often, especially if you wake up feeling that way
- Bloating with a loss of appetite or nausea
- Extreme fatigue or more trouble finishing your daily activities
- A lung infection or a cough that gets worse
- Fast heart rate
- New irregular heartbeat
Don’t Miss: Can This 10 Second Trick Prevent Your Heart Attack
How Does Heart Failure Affect Quality Of Life And Lifestyle
With the right care and treatment plan, heart failure may limit your activities, but many adults still enjoy life. How well you feel depends on how well your heart muscle is working, your symptoms and how well you respond to and follow your treatment plan. This includes caring for yourself and living a healthy lifestyle .
Because heart failure is a chronic long-term illness, talk to your doctor and your family about your preferences for medical care. You can complete an advance directive or living will to let everyone involved in your care know your desires. A living will details the treatments you do or dont want to prolong your life. It is a good idea to prepare a living will while you are well in case you arent able to make these decisions at a later time.
Reviewed by a Cleveland Clinic medical professional.
References
What Makes Yale Medicines Approach To Treating Congestive Heart Failure Unique
We have a very patient-focused team at Yale Medicine, says Dr. Jacoby.;Every person seen here, we treat as an individual, rather than offering a simple cookie-cutter treatment plan.
Yale Medicines multidisciplinary team comprises;of heart failure cardiologists and cardiac surgeons, dedicated advanced-practice, registered nurses and nurse coordinators, dietitians, exercise physiologists, financial counselors, immunologists specializing in transplants, psychologists, and specialists in palliative care.
In our multidisciplinary approach, we include the patients desires;as well as input from the family, Dr. Jacoby says. We develop a plan for social work support and take into account all of their financial and emotional stresses;in addition to their physical treatment needs.
Recommended Reading: How To Cure Congestive Heart Failure
Lifestyle And Dietary Changes
Lifestyle and dietary changes that are often recommended for people with chronic heart failure include:
- Stopping smoking: People who smoke should stop. Doctors are able to advise on the best methods of doing this.
- Limiting alcohol intake: If a personâs condition was caused by alcohol consumption, they should stop. Doctors are able to advise on the best methods of doing this.
- Losing weight: If a person is overweight, they should lose weight. This can lessen the strain placed on the heart.
- Taking regular exercise: Exercise can help to reduce symptoms such as shortness of breath and fatigue. Before beginning a new exercise regimen, however, a person should consult their doctor about how to do this in a safe way.
- Limiting salt intake: Salt can cause the retention of excess fluid in the body. By managing the amount of salt in oneâs diet, therefore, chronic heart failure can be managed. A doctor will advise on how much salt should be consumed.
- Weighing yourself daily: It is important for people who have been diagnosed with chronic heart failure to weigh themselves daily. If a personâs weight increases by around 2 kg over a period of 1 to 3 days, they should contact a doctor. This is a sign of fluid retention and may require intervention.
People with severe chronic heart failure may be asked to limit the amount of fluid, including water, they consume. Doctors will advise on exactly how much fluid to drink and how to do this in a safe way.
Initial Stages Of Chf
In the initial, mild stage A, there are underlying high-risk factors for CHF such as smoking or high blood pressure. However, the affected person has no symptoms or limitations at rest or with physical activity and there are no signs of CHF on evaluation by a doctor.
In stage B, the person develops mild symptoms of fatigue, shortness of breath, or heart palpitations with routine physical activity. There are minor signs of heart dysfunction on a doctor’s evaluation. There might also be a mild, intermittent collection of fluid, known as edema, in the ankles and feet.
Read Also: Does Ativan Lower Heart Rate
How Is Chf Diagnosed
After reporting your symptoms to your doctor, they may refer you to a heart specialist, or cardiologist.
The cardiologist will perform a physical exam, which will involve listening to your heart with a stethoscope to detect abnormal heart rhythms.
To confirm an initial diagnosis, a cardiologist might order certain diagnostic tests to examine your hearts valves, blood vessels, and chambers.
There are a variety of tests used to diagnose heart conditions. Because these tests measure different things, your doctor may recommend a few to get a full picture of your current condition.
Outlook For Heart Failure
Heart failure is a serious long-term condition that’ll usually continue to get slowly worse over time.
It can severely limit the activities you’re able to do and is often eventually fatal.
But;it’s;very difficult;to;tell how the condition will progress on an individual basis.
It’s very unpredictable. Lots of;people;remain;stable for many years, while;in some cases it;may get;worse quickly.
Also Check: How To Get Heart Attack
Congestive Heart Failure Causes
Congestive heart failure stages of dying frequently develop right after other conditions have damaged or weakened your heart. However, the heart doesnt need to become weakened to cause CHF. It can also happen if the heart becomes way too stiff.
When it comes to a result of CHF, the main pumping chambers of your heart may become stiff and not fill properly between beats. In many cases of heart failure, your heart muscle tissue may become damaged and weakened, and the ventricles stretch to the point that the heart cant push blood effectively throughout your body.
Severe lung disease When the lungs dont work properly, the heart needs to work harder to get available oxygen to the entire body.
How Is Congestive Heart Failure Treated
We assess the current health status of the patient to establish a baseline and develop a long-term health plan with the goal of improving the patients health, says Dr. Jacoby. This may involve the optimization of medicines and therapies, adding new medication or;maybe enrollment in one of the clinical trials going on here.
Theres no quick fix, he says. Stabilizing and/or reversing a patients condition often involves long-term collaborative follow-up with a referring cardiologist or physician, Dr. Jacoby says.
In worst-case scenarios, we may offer advanced therapies, which include mechanical solutions, a heart transplant or hospice, Dr. Jacoby says. But first, we work very closely with our partners in cardiology and Interventional Cardiology Program at Yale to see if the patient would benefit from any interventional strategies.
“Yale has the best program in the area for heart transplants and artificial parts, but we want to exhaust all other options to avoid either;if we can.
Don’t Miss: How Can I Stop Heart Palpitations At Night
