How The Heart Works
The heart is comprised of four chambers: the right atrium, the right ventricle, the left atrium, and the left ventricle. There are valves between these chambers that regulate blood flow through the heart. In a normally functioning heart, the veins of the body deliver deoxygenated blood through the right atrium into the right ventricle. The blood flows through the pulmonary artery and becomes oxygen-rich. The blood is then pumped into the left ventricle and then goes through the left atrium out to the body via the arteries. When a disease is present in one or more areas of the heart, the blood cannot flow properly and fluid can build up in the heart and surrounding areas.
What Is An Ejection Fraction
An ejection fraction is a measurement of the blood pumped out of your heart with each beat, expressed in a percentage. It can be measured using an echocardiogram , multigated acquisition scan, nuclear stress test,;magnetic resonance imaging ,;or during a cardiac catheterization. A normal ejection fraction is between 55% and 70%.
People at this stage may have some slight symptoms like:
- Slight physical limitations
- Shortness of breath with physical activity
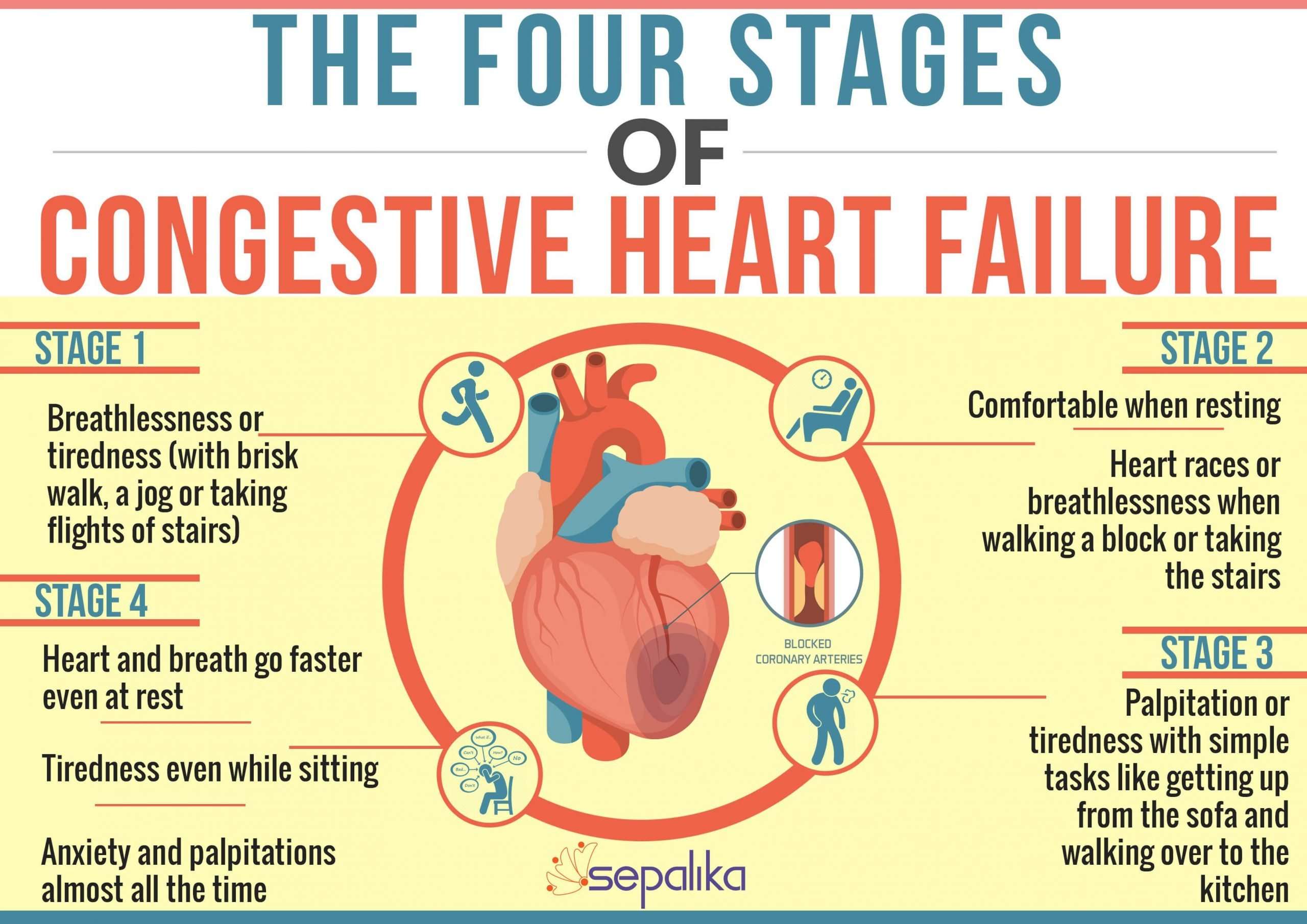
Stages Of Heart Failure
In 2001, the American Heart Association and American College of Cardiology described the “Stages of Heart Failure.” These stages, which were updated in 2005, will help you understand that heart failure is often a progressive condition and can worsen over time. They will also help you understand why a new medication was added to your treatment plan and may help you understand why lifestyle changes and other treatments are needed.
The stages classified by the AHA and ACC are different than the New York Heart Association clinical classifications of heart failure that rank patients as class I-II-III-IV, according to the degree of symptoms or functional limits. Ask your doctor what stage of heart failure you are in.
Check the table below to see if your therapy matches what the AHA and ACC recommend. Note that you cannot go backward in stage, only forward.
The table below outlines a basic plan of care that may or may not apply to you, based on the cause of your heart failure and your special needs. Ask your doctor to explain therapies that are listed if you do not understand why you are or are not receiving them.
The New York Heart Association clinical classifications of heart failure rank people as class I-II-III-IV, according to the degree of symptoms or functional limits. You can ask your doctor if you want to know what stage of heart failure youâre in.
Don’t Miss: Why Do I Keep Having Heart Palpitations
What Is Heart Failure
Heart failure doesnât mean the heart has stopped working. Rather, it means that the heart works less efficiently than normal. Due to various possible causes, blood moves through the heart and body at a slower rate, and pressure in the heart increases. As a result, the heart canât pump enough oxygen and nutrients to meet the body’s needs.
The chambers of the heart may respond by stretching to hold more blood to pump through the body or by becoming stiff and thickened. This helps to keep the blood moving, but the heart muscle walls may eventually weaken and become unable to pump as efficiently. The kidneys may respond by causing the body to retain fluid and salt. If fluid builds up in the arms, legs, ankles, feet, lungs, or other organs, the body becomes congested. Congestive heart failure is the term used to describe the condition.
B What’s The Evidence For Specific Management And Treatment Recommendations
There are three main guidelines that address the treatment of patients with acute heart failure:
Lindenfeld, J, Albert, NM, Boehmer, JP. âHFSA 2010 comprehensive heart failure practice guidelineâ. J Card Fail. vol. 16. 2010. pp. e1-194. , and is updated.)
Hunt, SA, Abraham, WT, Chin, MH. â2009 focused update incorporated into the ACC/AHA 2005 guidelines for the diagnosis and management of heart failure in adults: A report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines developed in collaboration with the International Society for Heart and Lung Transplantationâ. J Am Coll Cardiol. vol. 53. 2009. pp. e1-e90. was a new addition to this set of guidelines.)
McMurray, JJ, Adamopoulos, S, Anker, SD. âESC guidelines for the diagnosis and treatment of acute and chronic heart failure 2012: The task force for the diagnosis and treatment of acute and chronic heart failure 2012 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association of the ESCâ. Eur Heart J. 2012. (The ESC had an independent set of guidelines for AHF in 2005, which were incorporated into, and updated in, the 2008 and 2012 documents.
It should be noted that there is very limited clinical trial evidence upon which these guidelines are based. However, there are some central articles that inform current practice and perspectives, a brief selection of which follows with annotations:
Recommended Reading: What’s Resting Heart Rate
Hypertension Or High Blood Pressure
Another cause of congestive heart failure is high blood pressure or hypertension. If you have high blood pressure, your heart muscle works extra hard to pump blood through your body.;
As time passes, because of the overexertion, the muscles in your heart can become too weak or too stiff to properly circulate blood to your body.; If you have high blood pressure, your heart muscle workextra hard to pump blood through your body.;
Women And Heart Failure
Women are just as likely as men to develop heart failure, but there are some differences:
- Women tend to develop heart failure later in life compared with men.
- Women tend to have heart failure caused by high blood pressure and have a normal EF .
- Women may have more shortness of breath than men do. There are no differences in treatment for men and women with heart failure.
Recommended Reading: How Does High Blood Pressure Affect The Heart
What Causes Heart Failure
Heart failure is caused by many conditions that damage the heart muscle, including:
- Coronary artery disease.Coronary artery disease , a disease of the arteries that supply blood and oxygen to the heart, causes decreased blood flow to the heart muscle. If the arteries become blocked or severely narrowed, the heart becomes starved for oxygen and nutrients.
- Heart attack. A heart attack happens when a coronary artery becomes suddenly blocked, stopping the flow of blood to the heart muscle. A heart attack damages the heart muscle, resulting in a scarred area that doesnât work the way it should.
- Cardiomyopathy. Damage to the heart muscle from causes other than artery or blood flow problems, such as from infections or alcohol or drug abuse.
- Conditions that overwork the heart. Conditions including high blood pressure, valve disease, thyroid disease, kidney disease, diabetes, or heart defects present at birth can all cause heart failure. In addition, heart failure can happen when several diseases or conditions are present at once.
Surgery And Medical Device Options
The goal of surgery is to make your heart work better.
. Routes blood around a blocked artery. Learn more about heart bypass surgery.
Cardiac resynchronization therapy . When your heartbeat is off-kilter, it can make heart failure worse. This treatment uses a pacemaker that sends timed electrical impulses to both of your heart’s lower chambers so they pump better and more in sync. Your doctor may call it a biventricular pacemaker. They could also pair it with an ICD . Read more on CRT, also called biventricular pacing, for heart failure.
Heart transplant. This is done when heart failure is so severe that it doesn’t respond to any other treatments. Get more information on heart transplant for heart failure.
Heart valve surgery. If a faulty heart valve causes your heart failure, your doctor may recommend repairing or replacing it. A surgeon can repair or replace the valves. Find out more on heart valve disease.
Implantable cardioverter-defibrillator . This device is similar to a pacemaker. It’s put under your skin in your chest. Wires lead through your veins and into your heart to keep track of your heart rhythm. If your heart starts to beat at a dangerous rhythm, or if it stops, the ICD tries to pace your heart or shock it back into normal rhythm. An ICD can also act as a pacemaker and speed your heart up if it’s going too slow. Learn more about ICDs for heart failure.
Don’t Miss: How Low Should Your Heart Rate Be
Living With Congestive Heart Failure: What To Expect
Yes, there are several lifestyle changes you should take into account if youve been diagnosed with congestive heart failure. But remember your diagnosis;doesnt;mean you should necessarily stop doing things you love.
You are supposed to be exercising walking, biking, swimming, or doing light weight exercises, says Mountis. The American Heart Association recommends at least 30 minutes of moderate intensity aerobic activity at least five days a week for optimal heart health. Avoid exercises that make you feel breathless, and make sure to talk to your doctor before starting a new exercise routine.
Your healthcare provider will also likely suggest dietary changes that can help reduce the swelling associated with congestive heart failure and slow the progression of the condition. Those changes may include following a;low- or reduced-salt diet, or reducing how much fluid you drink to lessen the bodys water content.
Other lifestyle changes that can slow the progression of heart failure include:
How Is Heart Failure Diagnosed
Your doctor will ask you many questions about your symptoms and medical history. Youâll be asked about any conditions you have that may cause heart failure . Youâll be asked if you smoke, take drugs, drink alcohol , and about what drugs you take.
Youâll also get a complete physical exam. Your doctor will listen to your heart and look for signs of heart failure as well as other illnesses that may have caused your heart muscle to weaken or stiffen.
Your doctor may also order other tests to determine the cause and severity of your heart failure. These include:
Other tests may be ordered, depending on your condition.
Also Check: What Branch Of Medicine Deals With Heart Disease
C Laboratory Tests To Monitor Response To And Adjustments In Management
Serial evaluation of electrolytes and renal function is important. Iatrogenic diuretic-induced hypokalemia can result in life-threatening arrhythmias and is best prevented by adequate supplementation, rather than treated once present. Decreases in renal function are common during treatment of AHF. Although initially thought to be associated with poor outcomes, transient decreases do not seem to portend a poor prognosis.
Serial BNP testing is not recommended for the routine inpatient management of patients with AHF. Serial testing with chest radiography is usually not necessary in the absence of new signs or symptoms.
How Is Congestive Heart Failure Diagnosed

With CHF, doctors look for signs such as rapid or strained breathing, an irregular or rapid heartbeat, abnormal heart sounds, swollen legs, distended neck veins, abnormal sounds from fluid buildup in the lungs heard via a stethoscope, and swelling of the liver.
Tests commonly obtained to determine the presence of congestive heart failure include an electrocardiogram, a chest x-ray and an echocardiogram, which uses sound waves to create a detailed moving picture of the heart. Other diagnostic tests for CHF may include a cardiac stress test, heart catheterization, which involves passing a thin, flexible tube into the right or left side of the heart, usually from the groin or the arm; an MRI of the heart ; and nuclear heart scans, non-invasive tests in which radioactive tracers are used to illuminate changes in the heart. Blood tests can help determine whether damage to heart muscle has occurred, detect how well the kidneys are functioning, determine whether a person is anemic, and assess sodium and potassium levels as well as brain natriuretic peptide , a substance secreted by the lower chambers of the heart in response to the development or worsening of heart failure.
Also Check: How To Lower My Resting Heart Rate
Hawthorne Berry For Congestive Heart Failure
If your response to CoQ10 is insufficient, the next step is to add hawthorn berry , a congestive heart failure treatment I’ve used extensively, particularly in patients sensitive to digoxin.
According to clinical research, hawthorn berry can increase the action of digoxin, making it possible to decrease the dose of digoxin, thereby avoiding or lessening digoxin-related side effects.In fact, some patients with mild congestive heart failure get significant relief with hawthorn berry alone, an effect supported by double-blind studies in Europe. The German government recognizes hawthorn berries as an approved heart medicine.How does hawthorn work? It is believed to improve the heart’s ability to metabolize energy and utilize oxygen, and the berry’s extracts contain flavonoids that increase the heart muscle’s force of contraction.
Hawthorn berries also normalize irregular heartbeats, help lower blood pressure and enhance circulation by dilating the arteries.Aim for 5001500 mg daily or take as a tincture in water three times daily. For prevention, I recommend drinking hawthorn berry tea, which you can make by pouring boiling water over a cup of berries and letting them steep for 15 minutes.
Who Gets Congestive Heart Failure And What Are The Risk Factors
An estimated 6.2 million people in the United States have heart failure. Diseases and conditions that increase the risk of developing heart disease or cardiovascular disease also increase the risk of eventually developing congestive heart failure as a complication.
Risk factors include:
- Atherosclerosis and coronary artery disease
- Excessive alcohol consumption
- Sedentary lifestyle
- Smoking
Having high levels of certain substances in the body, which can be determined by blood tests, can also increase the risk for and congestive heart failure. These include:
- High cholesterol, which can lead to atherosclerosis
- High C-reactive protein level, which reflects inflammation
- High homocysteine level, which may damage artery walls and increase the risk of developing . Blood clots can cause a and lead to congestive heart failure.
Reducing your risk of congestive heart failure
You can reduce your risk of developing heart disease and congestive heart failure by:
- Eating a heart-healthy diet that is low in saturated fat and trans fats and high in fiber, whole grains, fruits, and vegetables
- Limiting alcohol intake to one drink per day for women and two drinks per day for men
- Maintaining a healthy weight
- Participating in a regular exercise program
- Reducing excessive stress
- Seeking regular medical care and prenatal care and following your treatment plan for such conditions as , obesity, hypertension, and diabetes
You May Like: How Does Exercise Affect Heart Rate
Know When To Seek Help
Watch for signs that heart failure is getting worse,;such as;new or worsening;symptoms. Weight gain, ankle swelling,;or increasing shortness of breath;may mean that fluids are building up in your body. Ask your doctor how often you should check your weight and when to report weight changes.;
Your;symptoms may suddenly get worse.;Ask your doctor when to make an office visit or get emergency care.;Keep the following handy:;
- Phone numbers for your doctor, the hospital, and someone who can take you for medical care;;
- Directions to the doctor’s office and hospital;;
- A;list of all the medicines youre taking;;
How Common Is Heart Failure
About 920,000 people in the UK currently have heart failure.There are around 67,000 admissions to hospital for heart failure in England and Wales each year. Heart failure becomes more common as people become older. It is commonly diagnosed in people in their 70s. In the UK around one in seven people aged 85 or more have heart failure. In people aged 65-74, around one in 35 have heart failure.
Recommended Reading: How Do You Calculate Heart Rate
Surgical Treatments For Congestive Heart Failure
A variety of surgical procedures may be used in the treatment of some cases of congestive heart failure including:
- and stent placement or coronary artery bypass may be an option for people with congestive heart failure who have severely blocked coronary arteries.
- Heart transplant may be the only treatment option in severe cases of congestive heart failure in which medications and lifestyle and dietary changes do not improve heart function.
- Left is a device surgeons connect to the heart to improve heart function. It may be used as a “bridge treatment” while waiting for a or as a treatment in itself.
- may be used in some cases to control abnormal heart rhythms.
- Valve surgery repair or replacement of damaged heart valves
I Acute Heart Failure: What Every Physician Needs To Know
Acute heart failure , also known as acute decompensated heart failure or cardiac failure, is not a single disease entity, but rather a syndrome of the worsening of signs and symptoms reflecting an inability of the heart to pump blood at a rate commensurate to the needs of the body at normal filling pressure. AHF is often not acute in onset, typically developing gradually over the course of days to weeks, where the acuity is a function of the need for urgent or emergent therapy due to the severity of these signs or symptoms.
AHF may be the result of a primary disturbance in the systolic or diastolic function of the heart or of abnormal venous or arterial vasoconstriction, but generally represents an interaction of multiple factors, including volume overload. The majority of patients have decompensation of chronic heart failure and consequently much of the discussion of the pathophysiology, presentation, and diagnosis of CHF is directly relevant to an understanding of AHF.
Read Also: How Does Blood Move Through The Heart
What Therapies Does Dr Weil Recommend For Congestive Heart Failure
Dr. Weil emphasizes the preventive importance of dietary changes to control obesity and diabetes, both of which are linked to the development of congestive heart failure. He advises consulting a nutritionist to develop a diet designed for individual situations and also recommends the following measures:
- If you smoke, quit. Tobacco has direct and damaging effects on the cardiovascular system.
- Avoid salt. Sodium promotes fluid retention. Avoid high-sodium foods, heavily processed foods and unnecessary salt.
- Take your prescribed medication. Diuretics , beta blockers, digoxin and others can reduce stress on the heart and make it work more efficiently.
- Check other meds. Over-the-counter NSAIDS, such as aspirin, Motrin and Aleve may increase fluid retention. Tell your doctor about any remedies you are taking.
- Control risk factors. Work with your doctor to address high blood pressure, diabetes and atherosclerosis or other heart problems.
- Reduce stress. The hormones released by the body in response to stress, anxiety and depression make the heart work harder. Practice relaxation techniques, volunteer, and seek positive social interactions. The relaxing breath exercise can improve the oxygenation of blood and take workload off the heart.
Nutrition and Supplements If you are coping with, or are at risk of congestive heart failure, Dr. Weil suggests trying the following supplements:
