Support Them To Make Decisions About Treatments
As well as having an advance care plan, patients should be given the chance to discuss the following issues:
- Whether to deactivate an implantable cardioverter defibrillator , if they have one. This can prevent the ICD activating at the end of life, which can be distressing.
- What the patient would want to happen if they had a cardiac arrest. They may decide they do not want to have cardiopulmonary resuscitation .
- When to stop medication that no longer reduces symptoms or improves their quality of life. This can be a difficult conversation and it’s best carried out sooner rather than later. Make sure the patient and the people important to them understand what changes are being made to their medication and why.
Stages Or Classes Of Heart Failure
Your patient may have been told what stage or class their heart failure is at this explains how severe it is.
NYHA classification divides heart failure into four classes:
- Class 1: no limitation of physical activity. Ordinary physical activity does not cause undue fatigue, breathlessness, or palpitations.
- Class 2: slight limitation of physical activity. Comfortable at rest but ordinary physical activity results in undue breathlessness, fatigue, or palpitations.
- Class 3: marked limitation of physical activity. Comfortable at rest but less than ordinary physical activity results in undue breathlessness, fatigue, or palpitations.
- Class 4: unable to carry out any physical activity without discomfort. Symptoms at rest can be present. If any physical activity is undertaken discomfort is increased.
Patients with advanced heart failure will usually fit into class 3 and 4, despite the best specialist treatment. Read more about the definition of heart failure from NICE .
Mechanisms Of Scd In Hfref
HF was associated with increased action potential duration and transmural heterogeneity of repolarization, leading to increased arrhythmic events and SCD . This electrical remodeling is the consequence of dysregulation of different ion channels, especially the potassium channels , and the transient outward potassium current has been shown to result in electrical dispersion and triggered activity in the failing hearts. Sodium channels are also responsible for the maintenance of AP plateau and repolarization so that alterations of INa in HF patients may lead to pro-arrhythmic states . Intracellular calcium not only mediates myocardial contraction but also influences electrophysiological balance . Dysregulation of calcium channels is also responsible for excitationcontraction uncoupling and arrhythmogenesis .
You May Like: Does Caffeine Increase Heart Rate
Also Check: Patients Who Are Experiencing A Heart Attack Often Complain Of:
What Medications Should I Avoid If I Have Heart Failure
There are several different types of medications that are best avoided in those with heart failure including:
- Nonsteroidal anti-inflammatory medications such as Motrin or Aleve. For relief of aches, pains, or fever take Tylenol instead.
- Most calcium channel blockers
- Some nutritional supplements, such as salt substitutes, and growth hormone therapies
- Antacids that contain sodium
If youâre taking any of these drugs, discuss them with your doctor.
Itâs important to know the names of your medications, what theyâre used for, and how often and at what times you take them. Keep a list of your medications and bring them with you to each of your doctor visits. Never stop taking your medications without discussing it with your doctor. Even if you have no symptoms, your medications decrease the work of your heart so that it can pump more effectively.
Sensitivity Specificity And Predictive Value Of Symptoms Signs And Chest X Ray Findings For Presence Of Heart Failure In 1306 Patients With Coronary Artery Disease Undergoing Cardiac Catheterisation
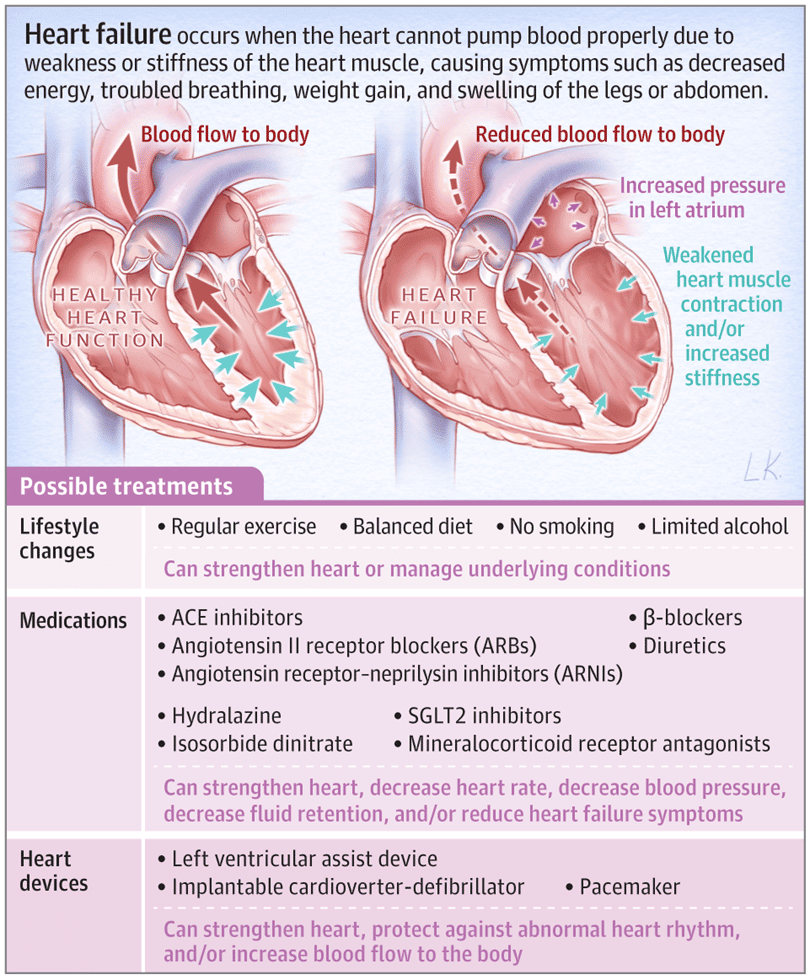
| Clinical features |
| 32 |
Oedema
Swelling of ankles and feet is another common presenting feature, although there are numerous non-cardiac causes of this symptom. Right heart failure may manifest as oedema, right hypochondrial pain , abdominal swelling , loss of appetite, and, rarely, malabsorption . An increase in weight may be associated with fluid retention, although cardiac cachexia and weight loss are important markers of disease severity in some patients.
Recommended Reading: When To Go To The Hospital For Rapid Heart Rate
Faces Of Heart Failure
Heart failure occurs when something damages the heart muscle or reduces the heart’s ability to pump effectively. Most often, the damage stems from coronary artery disease or heart attack. But faulty heart valves, longstanding high blood pressure, or genetic disease may also be to blame. No matter what the cause, the failing heart can no longer pump well enough to keep up with the body’s demand for oxygen-rich blood.
To help both doctors and patients quickly spot a possible combination of heart failure symptoms, the Heart Failure Society of America developed a handy tool that goes by the acronym FACES.
F = Fatigue. When the heart can’t pump enough oxygen-rich blood to meet the body’s energy needs, a general feeling of tiredness or fatigue sets in.
A = Activity limitation. People with heart failure are often unable to do their normal activities because they become easily tired and short of breath.
C = Congestion. Fluid buildup in the lungs can result in coughing, wheezing, and breathing difficulty.
E = Edema or ankle swelling. When the heart doesn’t have enough pumping power to force used blood back up from the lower extremities, fluid can collect in the ankles, legs, thighs, and abdomen. Excess fluid can also cause rapid weight gain.
How To Get Palliative Care
In order to get palliative care for your loved one from a home hospice care provider, it will be necessary to obtain a referral from his or her primary physician. The physician may inquire about know which treatments your loved one may or may not want and then will refer your loved one to local providers that offer the specified services.
Typical palliative care services offered from home hospice care providers may include:
- Medical care to alleviate a patients symptoms manage symptoms
- Provide spiritual and emotional support for a patient and his or her family
- Offer assistance with practical matters, such as insurance
Having to make plans regarding the end-of-life care for you loved may be difficult. However, keeping in mind what his or her wishes are regarding the end of his or her life can help you make the right decisions.
You May Like: How Does Blood Flow Through The Heart Step By Step
What Raises A Persons Risk Of Developing Pulmonary Hypertension
Risk factors for developing pulmonary hypertension include:
- Family history of blood clots.
- Family history of pulmonary hypertension.
- Living at high altitudes.
- Smoking and using tobacco products.
- Use of diet medications such as fen-phen .
- Use of some prescription medications that treat cancer and depression.
- Use of recreational drugs.
Talk with your provider about your risk factors and what you can do to lower your risk.
You May Like: How Many Season Of When Calls The Heart
Initial Stages Of Chf
In the initial, mild stage A, there are underlying high-risk factors for CHF such as smoking or high blood pressure. However, the affected person has no symptoms or limitations at rest or with physical activity and there are no signs of CHF on evaluation by a doctor.
In stage B, the person develops mild symptoms of fatigue, shortness of breath, or heart palpitations with routine physical activity. There are minor signs of heart dysfunction on a doctor’s evaluation. There might also be a mild, intermittent collection of fluid, known as edema, in the ankles and feet.
Also Check: Congestive Heart Failure Ecg Images
When To Begin Planning
It can be hard to know when to start making plans for the end of life. The progression of a long-term condition like heart failure can be unpredictable, which makes it difficult to know when the time is right. Its important to discuss things with your healthcare professional as early as you can. Many routine face-to-face appointments are being cancelled because of coronavirus, so check if your nurse or doctor is running telephone appointments instead. By discussing things as early as possible, it means you to have time to think about treatment options and preferences and where youd want to be cared for towards the end of your life. This may help you achieve some peace of mind and a sense of control.
What Dietary Changes Should I Make
Your provider will give you specific recommendations. One key step involves reducing your sodium intake. This means:
- Avoid adding salt at the table or using seasoning salt.
- Avoid smoked, cured, salted and canned meat products.
- Buy foods that are low sodium or low salt.
- Limit fast foods and prepared foods.
Other dietary changes include:
- Eat foods high in fiber .
- Eat foods high in potassium .
- Eat foods high in magnesium .
- Limit foods that contain refined sugar, saturated fat and cholesterol.
Also Check: What Does It Mean If Your Heart Rate Is High
Weeks Before End Of Life
Some of the earliest signs have to do with a sense of resignation. That may involve low mood, lack of motivation, and withdrawal. The person may spend more time reminiscing about their childhood and earlier life experiences.
Loss of appetite, general weakness, and increasing fatigue become noticeable.
A: Patient Understanding Of Disease And Prognosis

A1: Dealing with advanced heart failure and ageing
Patient statements revealed different levels of perspectives related to heart failure, ranging from descriptions of their illness adaption to changing conditions , appraisal of their own quality of life , and their handling of information regarding their illness .
A1.a: Perception of heart failure
The patients described various experiences with symptoms of heart failure, in particular, limitations such as shortness of breath, dizziness, and restrictions in activities of daily living. Frequently, they did not perceive heart failure as a life-limiting, chronic disease with a long-term course, but rather as a disease with acute life-threatening events. The patients often believed their condition was a result of their old age and not a genuine illness. Medical definitions and personal experiences may diverge: Despite their specific diagnosis and treatment, the patients reported feeling well. Consequently, they may play down their symptoms and not take their medications. However, changes in the patients perceptions were sometimes observed when their condition worsened:
Patient P1, T3 : But my heart, thats not really the problem. That is high blood pressure. Yes, I have that! Oh, yeah! You know, now now I have it under control. You know, I have never taken any pills. Yeah, and I watch out for my blood pressure. But if I say I take my tablets, that I do not do that anymore.
A.1b: Adaption to changing conditions
Don’t Miss: How Do You Determine Your Target Heart Rate
Helping Individuals With End
According to the National Hospice and Palliative Care Organization, heart disease is on the rise in the United States. Additionally, the disease comes with a high symptom burden, specifically at the end-of-life. Therefore, individuals with end-stage heart disease and congestive heart failure can benefit from hospice services.
Hospice of Southern Illinois focuses on comfort care for individuals with heart disease and CHF rather than curative treatment. Keeping in mind that your loved ones wishes are most important, our team including the medical director, pharmacist, nurse practitioner, nurses, social workers, counselors, hospice aides and volunteers will work together to create an individualized plan of care to reduce pain and keep symptoms managed, including but not limited to, chest pain, shortness of breath and fatigue. We will cover medications, equipment and services related to the patients terminal prognosis. Contact us today for more information on hospice for CHF, care for individuals with heart disease, and care for advanced heart failure. No one has to go through the dying process alone. Hospice of Southern Illinois is here to help.
Thinking About What Care And Treatment You Would Like
For different heart conditions, there are different things you might need to consider when approaching the end of life:
-
Some people with heart failure are at risk of dying suddenly because they may develop a life-threatening heart rhythm. This can lead to a cardiac arrest. You may want to think about what you would want to happen if you had a cardiac arrest and whether you would want to have CPR or not. Without CPR, your heart rhythm would not be restored, and you would die.
-
If you have an ICD fitted, you might want to discuss whether to deactivate it . This would mean that if you were to have a cardiac arrest, your ICD wouldnt be there to restore your heart rhythm which would help to minimise any discomfort or distress. Read our ICD deactivation FAQs for more information.
-
Antibiotics are given to help your body fight infection. You may decide to refuse antibiotics.
Its good idea to involve loved ones in these kinds of decisions so theyre aware of your wishes. You might also want to discuss matters like organ donation and how you intend for your wishes to be recorded.
Also Check: Does Anxiety Cause Heart Palpitations
Also Check: Which Is A Manifestation Of Right-sided Heart Failure
Early Attention To Heart Disease
Congestive heart failure is one of the leading causes of death in the elderly and is not curable. The best course is to avoid or treat early known causes of the disease to prevent or limit damage to the heart. See your doctor if you notice early signs that might indicate CHF such as shortness of breath or fluid in your legs.
How To Disable Otg On Infinix Hot 8
cpt code for psma pet scan
apex legends hacks free 2022
2022. 7. 28. ·CHF is a condition that occurs when the heart is unable to pump enough blood to meet the needs of the entire body . We will write a custom Presentation on Congestive Heart Failure : Causes, Treatment and Prevention specifically for you. for only $16.05 $11/page. 808 certified writers online. Stage C. Stage C is where heart failure has begun to cause symptoms that result from the weakening of the left ventricle. This is also the stage where symptoms such as fatigue and shortness of breath are a common occurrence. Swelling in.
paypal pay in 4 charged twice
symptoms of nazar lagna
Read Also: Diets For Congestive Heart Failure
Is Congestive Heart Failure Considered A Disability
When Is Congestive Heart Failure Considered a Disability Making You Eligible for Disability Benefits? The Social Security Administration has detailed criteria in its Blue Book listing that must be met in order for CHF to be considered a disability. A person must have one of these types of CHF: Systolic failure.
What Can Hospice Do For A Patient With Congestive Heart Failure Or Heart Disease
Your hospice team evaluates the patients status and updates the plan of care as CHF or heart disease symptoms and conditions change, even on a day-to-day basis. The goal of hospice is to manage symptoms and relieve physical/emotional distress so patients can live as fully as possible, retain their dignity and remain comfortable at home.
The hospice plan of care treats a wide range of heart disease symptoms, including:
- Shortness of breath
- Functional decline
When you turn to hospice, you are not alone in your journey your hospice care team is educated and experienced in advanced cardiac care, such as:
- Monitoring and managing your symptoms
- Communicating with your cardiologists office to intervene early and stabilize worsening conditions
- Providing medication, oxygen and other medical equipment related to your heart disease
- Providing services to reduce acute symptoms and avoid re-hospitalization
- Providing an average of 5 home visits per week and proactive phone calls
Hospice offers comprehensive services for patients with heart disease, such as:
You May Like: What To Expect After Infant Open-heart Surgery
What Are The Symptoms Of Heart Failure
You may not have any symptoms of heart failure, or the symptoms may be mild to severe. Symptoms can be constant or can come and go. The symptoms can include:
- Congested lungs. Fluid backup in the lungs can cause shortness of breath with exercise or difficulty breathing at rest or when lying flat in bed. Lung congestion can also cause a dry, hacking cough or wheezing.
- Fluid and water retention. Less blood to your kidneys causes fluid and water retention, resulting in swollen ankles, legs, abdomen , and weight gain. Symptoms may cause an increased need to urinate during the night. Bloating in your stomach may cause a loss of appetite or nausea.
- Dizziness, fatigue, and weakness. Less blood to your major organs and muscles makes you feel tired and weak. Less blood to the brain can cause dizziness or confusion.
- Rapid or irregular heartbeats. The heart beats faster to pump enough blood to the body. This can cause a rapid or irregular heartbeat.
If you have heart failure, you may have one or all of these symptoms or you may have none of them. They may or may not indicate a weakened heart.
Heart Failure: Know The Symptoms And When To Seek Help
If you have stage B or stage C heart failure, you may require hospitalization and treatment with heart failure medications and other therapies. If you have shortness of breath, weakness, or swelling, you should seek medical attention. If you are unsure if you have CHF, you should consult with your doctor. If you have CHF, you may require hospitalization. There are, however, many treatments that can help you feel better while also keeping you out of the hospital.
Read Also: Heart Ablation Surgery Procedure
Afib And Congestive Heart Failure
Considering overall heart health, there are often other heart issues that go along with atrial fibrillation. A common condition those living with AFib often face is congestive heart failure, commonly known as CHF. CHF often refers to a weak heart but can also signify a stiff heart, meaning it doesnt pump blood efficiently throughout the body.
This can lead to back-flow, causing fluid buildup in the lungs or swelling of the legs, which are the most common symptoms of congestive heart failure.
