What Are The Symptoms
Your feet, legs, and ankles will likely to swell because blood is backing up in your veins. This symptom is called edema.
- If it backs up into your stomach or liver, you may notice that your abdomen is distended, too.
- You might find that you have to go to the bathroom more, especially at night. This is caused by fluid buildup, too.
As your heart failure gets worse, you may also see some of these symptoms:
- Itâs hard to breathe.
- Your neck veins are swollen.
- Your pulse is fast or feels âoff.â
- Your chest hurts.
- Youâre gaining weight from excess fluid.
- You donât feel like eating.
- Your skin is cold and sweaty.
- Youâre very tired.
Whats The Outlook For People With Right
For many people, the right combination of therapies and lifestyle changes can slow or stop the disease and improve symptoms. They can lead full, active lives.
About 1 in 10 American adults who live with heart failure have advanced heart failure. That means treatments arent working, and symptoms are getting worse. You may feel symptoms, such as shortness of breath, even when youre sitting. If you have advanced heart failure, talk with your care team about important care decisions and next steps.
Deterrence And Patient Education
Compliance with lifestyle modification and pharmacologic treatment and control of precipitating factors are crucial to prevent hospitalizations for heart failure exacerbation and improve the quality of life. Many of those precipitating factors are potentially under patient control. That is why patient education is an integral part of a multidisciplinary approach to decrease mortality and morbidity due to heart failure.
Recommended Reading: What Causes Left Sided Heart Failure
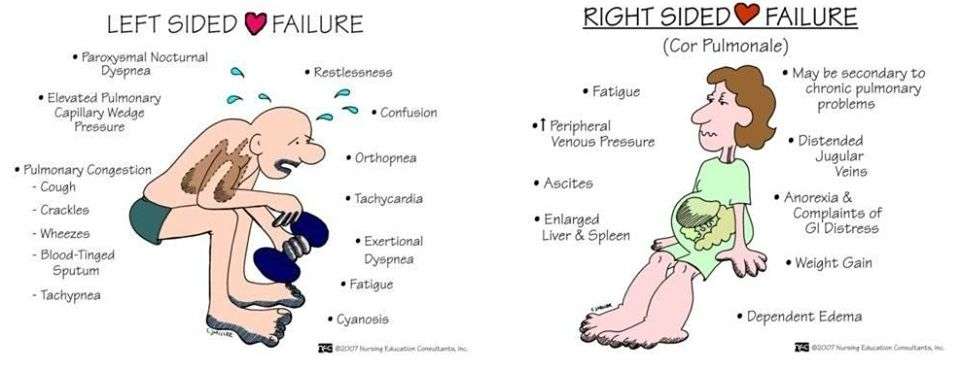
Clinical Manifestations Of Heart Failure
The clinical manifestation of heart failure is largely influenced by the primary side of dysfunction as left sided, right sided or biventricular. Left ventricular dysfunction increases pulmonary pressure and consequently pulmonary congestion occurs leading to dyspnoea and tachypnoea . As the peripheral circulation is reduced , renal dysfunction, peripheral malperfusion and malabsorption of nutrition with the signs of cardiac cachexia develop. In a chronic state, the permanent activation of neurohumoral systems lead to further volume overload , peripheral vasoconstriction , increased heart rate at rest and during exercise, and to a further deterioration of the cardio-renal system. Anemia , increased pulmonary pressure and muscle fatigue deteriorate the symptoms of dyspnoea as well. Overload of the heart leads to enlargement of the heart itself and as a measure the cardiothoracic index increases with leftward shift of the palpable cardiac pulsation. Mostly in volume overload situations filling volume of the ventricle increases periodically and a typical 3rd or 4th heart sound as protodiastolic gallop occurs . In consequence, heart failure influences almost all organ systems and thus heart failure is a systemic disease or a syndrome with a broad clinical spectrum.
Systolic And Diastolic Failure
Systolic and diastolic heart failure each result in a decrease in stroke volume. This leads to activation of peripheral and central baroreflexes and chemoreflexes that are capable of eliciting marked increases in sympathetic nerve traffic.
Although there are commonalities in the neurohormonal responses to decreased stroke volume, the neurohormone-mediated events that follow have been most clearly elucidated for individuals with systolic heart failure. The ensuing elevation in plasma norepinephrine directly correlates with the degree of cardiac dysfunction and has significant prognostic implications. Norepinephrine, while directly toxic to cardiac myocytes, is also responsible for a variety of signal-transduction abnormalities, such as downregulation of beta1-adrenergic receptors, uncoupling of beta2-adrenergic receptors, and increased activity of inhibitory G-protein. Changes in beta1-adrenergic receptors result in overexpression and promote myocardial hypertrophy.
Don’t Miss: What Is Target Heart Rate Definition
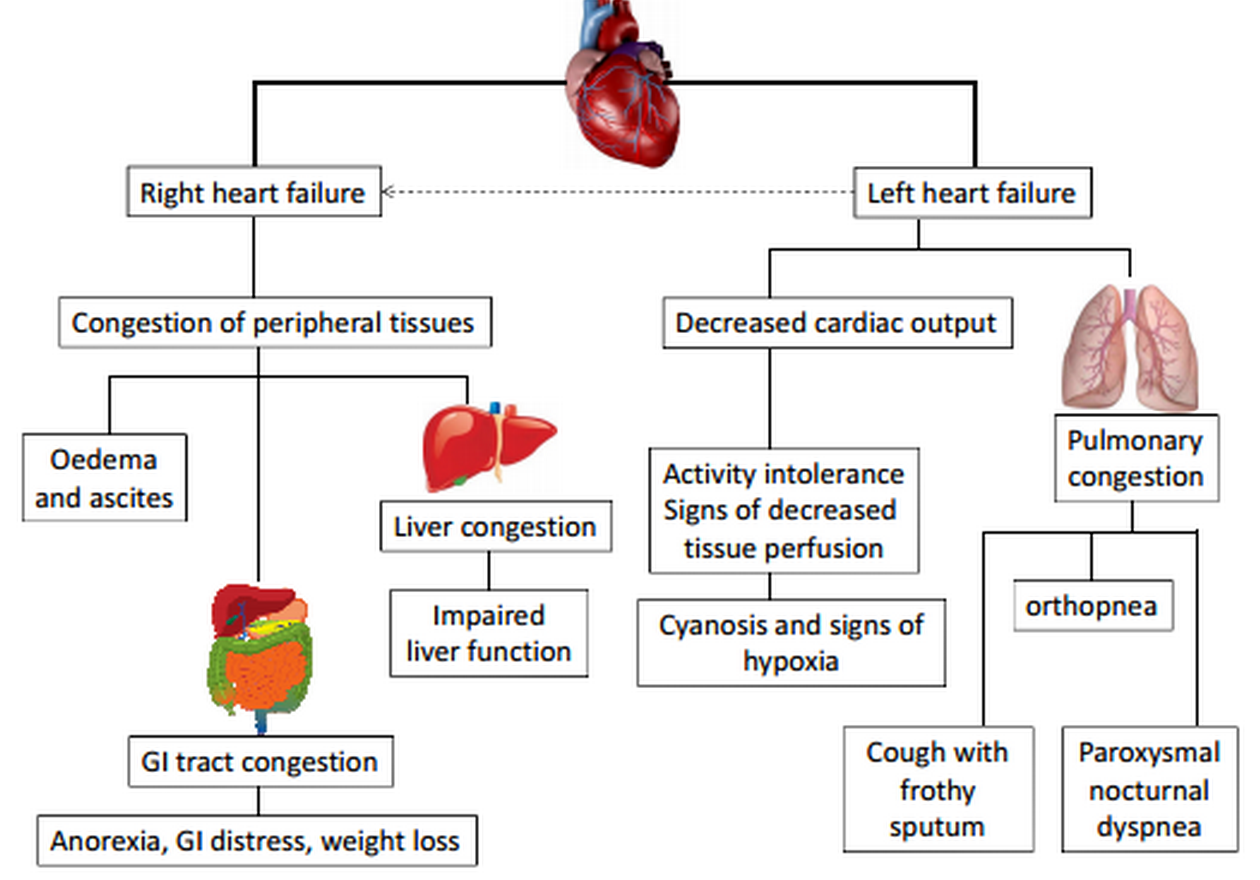
What Is A Right Sided Heart Failure
When the heart fails to pump blood adequately to the body tissues owing to the decrease in the pumping capacity of the right heart chambers, that condition is identified as the right heart failure.
The right sided heart failure occurs secondary to the left sided heart failure on most occasions. When the left side of the heart, specifically the left ventricle, fails to pump blood sufficiently into the aorta, blood starts to pool inside the left heart chambers. Consequently the pressure inside these chambers increases. This impairs the drainage of blood into the left atrium from the lungs via the pulmonary veins. As a result, the pressure inside the pulmonary vasculature also rises. Therefore, the right ventricle has to contract more vigorously against a higher resistive pressure to pump blood into the lungs. With the long-term prevalence of this condition, heart muscles of the right chambers start to wear down ultimately resulting in the right sided heart failure.
Figure 01: Heart
Although not frequently seen, right sided heart failure can also be caused by different intrinsic pulmonary pathologies such as COPD, bronchiectasis, and pulmonary thromboembolism.
Left Side Of The Heart
The job of the heart muscle is to transport oxygenated blood coming from the lungs to the left atrium and on through to the left ventricle. The left ventricle is the main pumping portion of the heart. It is larger than the other chambers and plays a fundamental role in normal heart function. When there is HF on the left side of the heart, the heart muscle has to work harder to squeeze out the same volume of blood. This is referred to as left ventricular heart failure. It is the most common type of HF.1
Also Check: What Should My Heart Rate Be While Working Out
About Heart And Vascular Institute
The UPMC Heart and Vascular Institute has long been a leader in cardiovascular care, with a rich history in clinical research and innovation. As one of the first heart transplant centers in the country and as the developer of one of the first heart-assist devices, UPMC has contributed to advancing the field of cardiovascular medicine. We strive to provide the most advanced, cutting-edge care for our patients, treating both common and complex conditions. We also offer services that seek to improve the health of our communities, including heart screenings, free clinics, and heart health education. Find an expert near you.
Tags
Precipitating Causes Of Heart Failure
A previously stable, compensated patient may develop heart failure that is clinically apparent for the first time when the intrinsic process has advanced to a critical point, such as with further narrowing of a stenotic aortic valve or mitral valve. Alternatively, decompensation may occur as a result of the failure or exhaustion of the compensatory mechanisms but without any change in the load on the heart in patients with persistent, severe pressure or volume overload. In particular, consider whether the patient has underlying coronary artery disease or valvular heart disease.
The most common cause of decompensation in a previously compensated patient with heart failure is inappropriate reduction in the intensity of treatment, such as dietary sodium restriction, physical activity reduction, or drug regimen reduction. Uncontrolled hypertension is the second most common cause of decompensation, followed closely by cardiac arrhythmias . Arrhythmias, particularly ventricular arrhythmias, can be life threatening. Also, patients with one form of underlying heart disease that may be well compensated can develop heart failure when a second form of heart disease ensues. For example, a patient with chronic hypertension and asymptomatic LV hypertrophy may be asymptomatic until an MI develops and precipitates heart failure.
- Profound anemia
- Pregnancy
- Nutritional deficiencies
You May Like: Who Performed The First Open Heart Surgery Successful
Comorbidities: Anemia Iron Deficiency Kidney Failure Diabetes Frailty
Moderate anemia is often prevalent in patients with heart failure regardless of HFrEF or HFpEF . The incidence is higher in women, elderly and diabetic patients as well as in patients with renal failure. Increased blood loss in patients treated with oral anticoagulants , aspirin or both as well as decreased absorption of vitamin and/or iron may favor anemia. Similar as in other chronic illnesses iron deficiency is common in heart failure and may influence prognosis worse. Whether anemia and/or iron deficiency are markers of heart failure severity or whether they affect outcome of heart failure disease and thus should be treated is not entirely clear. In patients with heart failure with as well as without anemia intravenous ferric carboxymaltose has improved quality of life and NYHA class but not prognosis .
Heart failure and chronic kidney disease frequently coexist and share many risk factors also. CKD worsen prognosis in heart failure patients however, patients with severe CKD often have been excluded from randomized clinical trials and thus there is limited evidence-based therapy available.
Comorbidities and aging via influencing cognitive and self-care ability affect management of heart failure patients. Also, polypharmacy is present often. In addition, frailty is common in these patients. In consequence, a multidisciplinary team is needed to take care especially for older heart failure patients to reduce hospitalizations and improve outcome.
How Common Is Heart Failure
In the United States alone, more than six million adults have been diagnosed with heart failure.
Heart failure is usually divided into two categories based on which side of the heart it mainly affects. The right side of the heart collects oxygen-depleted blood from the body and brings it to the lungs to be filled with fresh oxygen. The left side of the heart receives oxygen-rich blood from the lungs and sends it out to the rest of the body.
While the end result is the same, symptoms can vary based on whether the right or left side of the heart is affected.
Verywell / Jessica Olah
Recommended Reading: Does Drinking Raise Your Heart Rate
How Heart Failure Is Diagnosed
A diagnosis of heart failure or CHF is made by a doctor who specializes in the diagnosis and treatment of heart-related conditions, called a cardiologist. Your cardiologist will take a complete medical history, conduct a physical exam, and may order a variety of tests, including blood work and imaging tests.
The following tests and scans may be performed to help diagnose heart failure:
- Natriuretic peptide tests: Measures levels of B-type natriuretic peptide or N-terminal prohormone of B-type natriuretic peptide , which are released into the blood by the heart
- Echocardiogram: Determines the percent of blood that is pumped out of the heart with each heartbeat and evaluates the structure and function of the heart
- Electrocardiogram : Provides a tracing of the hearts electrical activity
- Stress test: Measures how the heart responds to exercise or chemically induced stress in a controlled environment
- Cardiac catheterization:Shows the interior of the arteries in your heart to see if they are blocked and allows for measurement of right and left heart pressures
- Other imaging tests such as cardiac computed tomography scan, cardiac magnetic resonance imaging , or nuclear heart scan can be used to show how well the heart is working.
Types Of Heart Attacks
A heart attack, also known clinically as myocardial infarction, is a form of acute coronary syndrome . It occurs when a significant blockage in the coronary arteries restricts blood flow to the heart.
The main types of heart attacks include:
- Non-ST segment elevation myocardial infarction
- ST-segment elevation myocardial infarction
You May Like: How To Calculate Target Heart Rate Zone
When Should I See A Healthcare Provider About Right Heart Failure
If you have chest pains or suspect you may be having a heart attack, call 911 or go to the nearest emergency room.
Get in touch with your healthcare provider if you experience:
- Shortness of breath.
What else should I ask my provider?
If you have right-sided heart failure, ask your provider:
- What treatment is best for me?
- Is there a special diet I should follow?
- Should I go to cardiac rehab?
- Will I need surgery?
- Will I need a heart transplant?
- What can I do to stop heart failure from progressing?
- What medications will I need?
A note from Cleveland Clinic
Right-sided heart failure means the right side of the heart can no longer pump blood efficiently. Fluid builds up in tissues, causing swelling. Treatment focuses on managing symptoms so the disease doesnt worsen. Healthy lifestyle habits, along with cardiac rehab, improve symptoms for many people. Other treatment options include cardiac devices and surgery. If you have shortness of breath, swelling or chest discomfort, talk to your healthcare provider.
What Is Congestive Heart Failure Right
Right-sided Congestive Heart Failure occurs when the right ventricle of the heart has difficulty pumping blood into your lungs. As a result, blood backs up in your blood vessels, that triggers fluid retention in the lower abdomen, extremities, and other vital organs. Right sided congestive heart failure can occur on its own, for example when triggered due to lung disease or heart valve disease. In severe cases, hepatomegaly can happen resulting in altering liver function, coagulopathy and jaundice.
Recommended Reading: What If My Heart Rate Is Over 100
Atrial Natriuretic Peptide And B
ANP and BNP are endogenously generated peptides activated in response to atrial and ventricular volume/pressure expansion. ANP and BNP are released from the atria and ventricles, respectively, and both promote vasodilation and natriuresis. Their hemodynamic effects are mediated by decreases in ventricular filling pressures, owing to reductions in cardiac preload and afterload. BNP, in particular, produces selective afferent arteriolar vasodilation and inhibits sodium reabsorption in the proximal convoluted tubule. It also inhibits renin and aldosterone release and, therefore, adrenergic activation. ANP and BNP are elevated in chronic heart failure. BNP especially has potentially important diagnostic, therapeutic, and prognostic implications.
For more information, see the Medscape Drugs & Diseases article Natriuretic Peptides in Congestive Heart Failure.
What Is Heart Failure
Although the term heart failure suggests your heart isnt able to function at all, it actually means your heart muscles just arent functioning well enough to support your bodys needs. It develops when your heart muscles are either too weak or not elastic enough to pump blood properly. About 6.2 million people in the United States are living with heart failure.
Heart failure is usually a chronic and progressive condition, but it can develop quickly after a heart attack or other conditions that damage your heart. The most common cause of heart failure is coronary artery disease, which is a narrowing of the arteries that supply blood to your heart.
Also Check: How Long Can Pre Heart Attack Symptoms Last
How Do I Take Care Of Myself If I Have Right
The most important thing is to make healthy lifestyle habits part of your daily routine. The more you make healthy living part of your new lifestyle, the better youll feel. Try to:
- Work with a nutritionist or dietitian to create a nutritious, filling meal plan you can stick with long-term.
- Find an exercise routine you enjoy so youll be motivated to get moving every day.
- Track and manage your symptoms. Report any changes to your healthcare provider.
- Take medications as instructed.
Summary Right Sided Vs Left Sided Heart Failure
When the heart fails to pump blood adequately to the body tissues, owing to the decrease in the pumping capacity of right heart chambers, that condition is identified as the right heart failure. On the other hand, when the heart failure is due to the faltering of the pumping capacity of the left heart chambers, it is known as left sided heart failure. Thus, the difference between right sided and left sided heart failure is that in right heart failure, the function of right heart chambers is impaired whereas the function of left heart chambers is impaired in the left heart failure.
Read Also: Why Does Heart Rate Increase During Running
Complications Of Left Heart Failure
Because left heart failure leads to a backup of blood in the lungs, other organs do not receive enough oxygen-rich blood. Symptoms of decreased blood flow to the brain, such as trouble with memory and concentration, affect people with advanced left heart failure. The kidneys are also vulnerable to poor blood flow in left heart failure. When the kidneys fail to receive enough blood and oxygen, kidney damage eventually occurs. Without treatment, most causes of left heart failure also lead to an enlarged heart. If the heart becomes dilated and enlarged, it is more prone to dangerous, abnormal heart rhythms — another complication of left heart failure.
What Can I Do To Manage Swelling From Extra Fluid
- Elevate your legs above the level of your heart. This will help with fluid that builds up in your legs or ankles. Elevate your legs as often as possible during the day. Prop your legs on pillows or blankets to keep them elevated comfortably. Try not to stand for long periods of time during the day. Move around to keep your blood circulating.
- Limit sodium . Ask how much sodium you can have each day. Your healthcare provider may give you a limit, such as 2,300 milligrams a day. Your provider or a dietitian can teach you how to read food labels for the number of mg in a food. He or she can also help you find ways to have less salt. For example, if you add salt to food as you cook, do not add more at the table.
- Drink liquids as directed. You may need to limit the amount of liquid you drink within 24 hours. Your healthcare provider will tell you how much liquid to have and which liquids are best for you. He or she may tell you to limit liquid to 1.5 to 2 liters in a day. He or she will also tell you how often to drink liquid throughout the day.
- Weigh yourself every morning. Use the same scale, in the same spot. Do this after you use the bathroom, but before you eat or drink. Wear the same type of clothing each time. Write down your weight and call your healthcare provider if you have a sudden weight gain. Swelling and weight gain are signs of fluid buildup.
Don’t Miss: Can Smoking Cause Heart Attack
