Top Tips For Caring For Someone Who Needs Help Eating:
- Face the person so they can see you and their food.
- If the person normally wears glasses or hearing aids, help them to put them on. This will help them to see what youre doing and to hear what youre saying.
- Offer smaller meals or portions that dont overwhelm the person.
- Let the person eat slowly. Allow plenty of time for them to chew their food and swallow it. They might need to catch their breath before each mouthful.
- Watch for clues to help you tell when they have finished swallowing. If its hard to tell, ask the person if theyve finished or to open their mouth to see if there is any food left inside.
- For drinks, use a wide cup or glass, so the drinker doesnt have to tilt their head back. You could also use a straw, for cold drinks.
- Dont rush the meal. This could increase the risk of food entering the persons airways.
- Look out for signs of tiredness. If the person is getting sleepy, it is best for them to stop eating even if they havent finished their meal. This is because people are more likely to cough or choke on food.
- If possible, try and make sure the person waits at least 15 minutes before going back to bed or lying down. This reduces the chances of food and drink coming back up the throat and causing them to choke.
Read Also: Heart Rate When Having A Heart Attack
What Does Moving To Hospice Care Involve
If you and your family have made the decision to pursue hospice care while receiving inpatient care, a case manager or social worker can help facilitate the process. If you are at home and would like to transition to hospice care, hospice agencies can help make the arrangements. Hospice agencies will review your needs and have a doctor order the appropriate medications for you. These medications will focus not on treating your condition, but on managing your symptoms and comfort as much as possible.
Hospice And Congestive Heart Failure
When a heart failure patient has been diagnosed with six months or less to live, the added support of hospice care helps them remain in their home until end of life.
Crossroads Hospice & Palliative Care provides a team of nurses, aides, social workers, volunteers, and chaplains to support the patient and their family through the final stages of congestive heart failure symptoms. To learn more about referring your patient to hospice, please call Crossroads at 1-888-564-3405.
Don’t Miss: What Does Heart Rate Variability Tell You
How Long Can You Live With End
Heart failure is a chronic, progressive condition that worsens with each flare-up. Your outlook and prognosis are better if you are healthy overall, you have been following your treatment plan, and you are responding well to your treatments. Being willing to pursue invasive treatments like a heart transplant will also increase your life expectancy.
Recommended Reading: Why Does Your Heart Rate Go Up When You Exercise
Cardiac Cachexia Or Anorexia
Cardiac cachexia or anorexia is characterised by loss of appetite, profound weight loss and loss of muscle and fat tissue. You could suggest the person tries eating small, frequent meals. You should consider high calorie, high protein food, and supplement drinks. There are more tips on our page about hydration and nutrition. A dietitian may be able to provide you and your patient with further guidance.
Read Also: How Does Exercise Affect Heart Rate
You May Like: How To Bring Heart Rate Down Naturally
What Do Symptoms Of End Stage Congestive Heart Failure Look Like
Dyspnea
Dyspnea or shortness of breath can occur both during activity and rest. This is the symptom that often sends patients racing to the hospital late at night. Work with your hospice or palliative care team to manage symptoms at home and avoid these stressful hospital trips.
Chronic Cough
When the heart cannot keep up with the supply of blood moving between it and the lungs, fluid can build up in the lungs. This results in a chronic cough or wheezing that can produce white or pink mucus.
Edema
As the hearts ability to pump slows down, fluid can build up in the body. This creates swelling in the extremities particularly the feet, ankles, legs, or abdomen.
Lack of Appetite
As the digestive system receives less blood, patients may feel full or nauseous. Not wanting to eat is a natural part of the body shutting down, but families often find this distressing. Learn more about why it is okay for your loved one to stop eating and drinking at end of life.
High Heart Rate
In response to a loss in pumping capacity, the heart begins to beat faster. The patient experiences this as a racing or throbbing heartbeat.
Confusion
When the heart stops working effectively, it can change sodium levels in the blood. This leads to memory loss, confusion, and a general feeling of disorientation.
Heart Failure Survival Rates
The survival rates from heart failure have been improving over the years. The improvement is slow, but gradual. Clinicians measure overall patient survival from a disease by comparing large groups of people with the disease to large groups of the same age range without it. For example, a 1-year survival rate of 90% is good. It means people with the disease are 90% as likely as people without the disease to be alive for at least one year after diagnosis. For heart failure, the 1-year survival rate rose from 74% in 2000 to about 81% in 2016. The 5-year survival rate increased from 41% to 48%, and the 10-year survival rate rose from about 20% to 26%.
Keep in mind prognosis and life expectancy information is based on data registries from several years ago . Someone diagnosed with heart failure today may have a better prognosis because heart failure treatment, including heart transplant, improves with time.
If you or a loved one has heart failure and you would like to know more about your case, ask your doctor how your age, overall health, and treatment affect your prognosis and life expectancy. Knowing what to expect can help you make plans for the time you have.
Don’t Miss: How To Calculate Target Heart Rate Zone
Heart Failure Expectations Unrealistic
In the study, researchers surveyed 122 people with moderate to advanced congestive heart failure about their perception of their life expectancy.
They found the heart failure patients tended to overestimate their life expectancy by about three years. The average patient survival estimate was 13 years compared with a validated medical model estimate of 10 years.
Overall, 63% of people with heart failure overestimated their remaining life expectancy by an average of 40% compared with medical model predictions. Those who were younger and with more advanced disease were most likely to overestimate how long they had left to live.
During the three-year follow-up period, 29% of the people involved in the survey died. Researchers found no relationship between longer life expectancy perceptions and survival.
How Long Can A Chihuahua Live With Heart Failure?
Is dying of congestive heart failure painful? Pain. Some people with heart failure can experience pain or discomfort towards the end of their life. They should be assessed using a pain scale. Pain-relieving medicines can be used to relieve pain and discomfort this can include opioid and non-opioid medicines .
Stages C And D With Preserved Ef
Treatment for patients with Stage C and Stage D heart failure and reserved EF includes:
- Treatments listed in Stages A and B.
- Medications for the treatment of medical conditions that can cause heart failure or make the condition worse, such as atrial fibrillation, high blood pressure, diabetes, obesity, coronary artery disease, chronic lung disease, high cholesterol and kidney disease.
- Diuretic to reduce or relieve symptoms.
YOU ARE THE MOST IMPORTANT PART OF YOUR TREATMENT PLAN!
It is up to you to take steps to improve your heart health. Take your medications as instructed, follow a low-sodium diet, stay active or become physically active, take notice of sudden changes in your weight, live a healthy lifestyle, keep your follow-up appointments, and track your symptoms. Talk to your healthcare team about questions or concerns you have about your medications, lifestyle changes or any other part of your treatment plan.
You May Like: What Is A Normal Heart Rate For A Woman In Her 50’s
What Causes Congestive Heart Failure
There are several conditions that can impair the pumping efficiency of the heart. Below are a few common and rare conditions that can cause congestive heart failure:
- Coronary artery disease : This is the most common cause of congestive heart failure, as the arteries become blocked or severely narrowed, which decreases blood flow to the heart.
Also Check: Why Do Soccer Players Died Of Heart Attacks
Heart Failure Patients Too Optimistic
Study Shows Patients Overestimate Their Life Expectancy
A new study shows nearly two-thirds of people with congestive heart failure overestimate their remaining life expectancy by an average of 40% compared with whats realistic based on their prognosis.
Heart failure, which occurs when the heart is too weak to pump enough blood to meet the bodys needs, causes 55,000 deaths each year and indirectly contributes to 230,000 more deaths annually in the U.S.
Although there have been recent improvements in congestive heart failure treatment, researchers say the prognosis for people with the disease is still bleak, with about 50% having an average life expectancy of less than five years. For those with advanced forms of heart failure, nearly 90% die within one year.
Patient perception of prognosis is important because it fundamentally influences medical decision making regarding medications, devices, transplantation, and end-of-life care, write researcher Larry A. Allen, MD, MHS, of the Duke Clinical Research Institute and colleagues in The Journal of the American Medical Association.
Read Also: How Does Heart Rate Affect Stroke Volume
How To Get Palliative Care
In order to get palliative care for your loved one from a home hospice care provider, it will be necessary to obtain a referral from his or her primary physician. The physician may inquire about know which treatments your loved one may or may not want and then will refer your loved one to local providers that offer the specified services.
Typical palliative care services offered from home hospice care providers may include:
- Medical care to alleviate a patients symptoms manage symptoms
- Provide spiritual and emotional support for a patient and his or her family
- Offer assistance with practical matters, such as insurance
Having to make plans regarding the end-of-life care for you loved may be difficult. However, keeping in mind what his or her wishes are regarding the end of his or her life can help you make the right decisions.
Causes Of Heart Failure
Heart failure is often the result of a number of problems affecting the heart at the same time.
Conditions that can lead to heart failure include:
- coronary heart disease where the arteries that supply blood to the heart become clogged up with fatty substances , which may cause angina or a heart attack
- high blood pressure this can put extra strain on the heart, which over time can lead to heart failure
- conditions affecting the heart muscle
- heart rhythm problems , such as atrial fibrillation
- damage or other problems with the heart valves
- congenital heart disease birth defects that affect the normal workings of the heart
Sometimes obesity, anaemia, drinking too much alcohol, an overactive thyroid or high pressure in the lungs can also lead to heart failure.
Also Check: How Long Can A Heart Attack Last
What Should I Expect In The Last Few Days
As the end of life approaches, you might experience a number of physical and emotional changes. These are different for everyone. You might notice changes over weeks, days or even hours. Some of the changes might be the same as signs of a flare-up, so discuss them with your doctor or nurse.
Signs to look out for include:
Surgery And Other Approaches
Depending on the underlying cause of the condition and the specific symptoms or complications, a doctor may recommend:
- surgery, to open blocked passages in the heart or repair heart valves, for example
- monitoring the persons fluid balance, kidney health, and other factors, to manage diabetes
- assessing blood pressure, heart rate, and other cardiac measures, to control high blood pressure
- counseling, for alcohol or drug use
- preparing a follow-up plan that includes sodium and fluid restriction
Recommended Reading: What Should Heart Rate Be When Sleeping
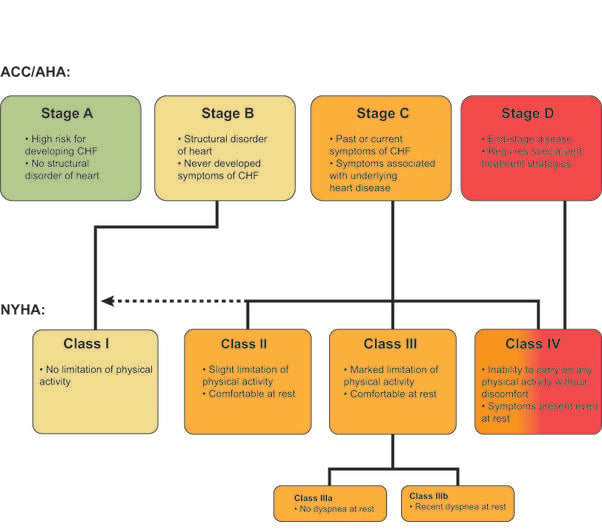
What Are The Stages Of Heart Failure
Heart failure is a chronic long-term condition that gets worse with time. There are four stages of heart failure . The stages range from high risk of developing heart failure to advanced heart failure, and provide treatment plans. Ask your healthcare provider what stage of heart failure you are in. These stages are different from the New York Heart Association clinical classifications of heart failure that reflect the severity of symptoms or functional limits due to heart failure.
As the condition gets worse, your heart muscle pumps less blood to your organs, and you move toward the next stage of heart failure. You cannot go backwards through the stages. For example, if you are in Stage B, you cannot be in Stage A again. The goal of treatment is to keep you from progressing through the stages or to slow down the progression.
Treatment at each stage of heart failure may involve changes to medications, lifestyle behaviors and cardiac devices. You can compare your treatment plan with those listed for each stage of heart failure. The treatments listed are based on current treatment guidelines. The table outlines a basic plan of care that may apply to you. If you have any questions about any part of your treatment plan, ask a member of your healthcare team.
How To Live Longer With Heart Failure
Everything you need to know about the various stages of heart failure to live longer with the condition.
A congestive heart failure diagnosis doesnt mean your heart has stopped working, it means that your heart is unable to pump enough blood throughout your body.
Heart failure is a scary term, says , a cardiologist at the Cleveland Clinic in Ohio. The condition can worsen if the proper steps arent taken to slow or halt the problem, but it does not mean your life is over.
Congestive heart failure, more simply known as heart failure, occurs when there’s a reduction in blood flow throughout the body because blood flow from the heart slows down. That means blood returning to the heart through the veins backs up, causing congestion in the body’s tissues. That congestion may cause swelling in the ankles, legs, or stomach, as well as fluid in the lungs that causes trouble breathing.
Life expectancy with congestive heart failure varies depending on the severity of the condition, genetics, age, and other factors. According to the Centers for Disease Control and Prevention , around one-half of all people diagnosed with congestive heart failure will survive beyond five years. Only around 10 percent of people diagnosed with the condition survive at least 10 years, according to a study published in August 2013 in the journal Circulation Research.
Also Check: How Long Can Someone Live With Heart Failure
Dilemmas From The Patient And Caregiver Perspective
In an interview study of 64 caregivers at 6 months after the patient’s death, there were common themes regarding end of life planning issues: lack of availability of treatment options for certain patients, changes in preferences at the very end of illness, variability in patient and caregiver desire for and readiness to hear information about the patient’s illness, and difficulties with patientâcaregiver communication. Patients and their caregivers may fail to raise end-of-life issues for various reasons including: lack of understanding their condition unpredictability of the clinical trajectory of HF discomfort and anxiety in raising end-of-life discussions and a feeling of powerlessness while viewing clinicians as unapproachable or reluctant to give out information.
In a study of patient preferences regarding end-of-life treatment in advanced HF, two distinct groups of patients were identified: one group preferred life-prolonging treatments, while the other group favoring strategies that improved quality of life despite reduced survival time. As treatment preferences were independent of functional or symptom status, this may present an important opportunity for clinicians to discuss such treatment preferences early in the course of illness and help facilitate end-of-life planning.
For Patients With Heart Failure Little Guidance As Death Nears
Americans are living longer with heart disease, managing it as a chronic condition. But there are few rules for these patients as they near the end of life.
Ricky Hurst, whose heart is failing, was told by doctors to get his affairs in order as his condition worsened. More patients like him are living longer with heart failure, but there are no widely accepted guidelines for care as they near death.CreditSean Proctor for The New York Times
Supported by
By Gina Kolata
Ricky Hursts doctors told him last year that there was nothing more they could do. His heart was failing and he should get his affairs in order. The end was coming.
His family gathered. He spoke to his pastor and resigned himself to death. If it was meant to be, it was meant to be, he said.
But. Mr. Hurst, 56, a former ranger and school football coach in Jackson, Mich., is still alive, although his heart continues to weaken. And patients like him are raising a new dilemma for doctors.
Heart disease once killed ruthlessly and quickly patients like Mr. Hurst succumbed to heart attacks and sudden death from cardiac arrest. But with improved medical care and implanted devices that bolster the heart, a growing number of heart patients survive for years, even decades, coping with a chronic, progressive condition punctuated by crises and hospitalizations.
We shouldnt have a single one of these cases happening, said Dr. Haider Warraich, a cardiology fellow at Duke University and first author of the study.
Also Check: Who Was The First Man To Perform Open Heart Surgery
