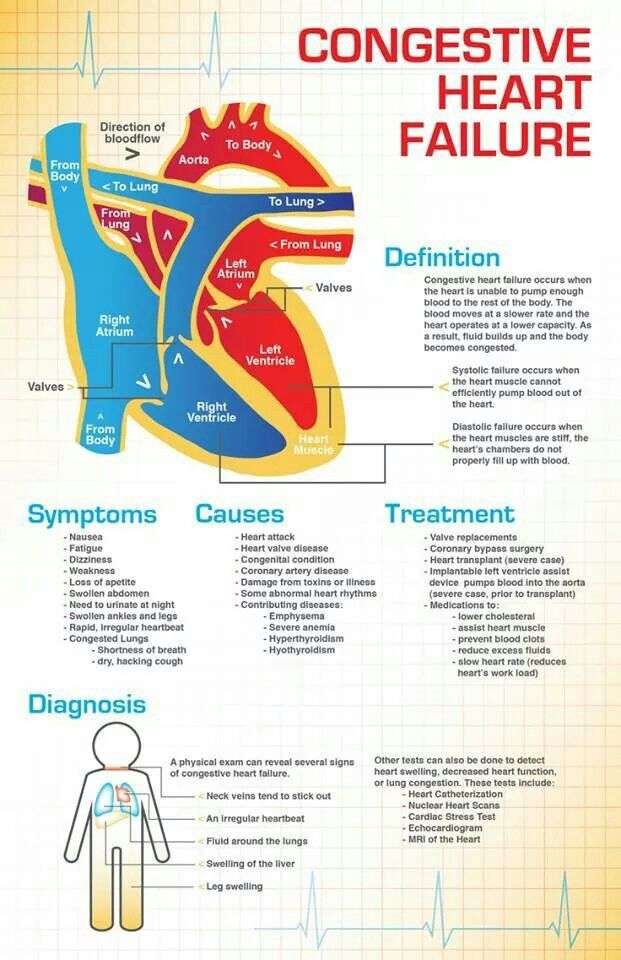
What Is Congestive Heart Failure
Congestive heart failure is a progressive condition in which the heart gradually becomes weaker and less capable of pumping blood. The word congestive refers to the fluid that builds up around the heart and in the lungs as a consequence of the weakening heart.
Early stages of heart failure can be treated through medication and lifestyle changes. However, if the condition is not diagnosed and treated early, it will progress to a stage that cannot be treated due to irreversible damage being inflicted on the heart.
Untreated high blood pressure and congenital heart valve defects can cause heart failure. It also links to high LDL cholesterol levels, diabetes, obesity, thyroid disease, certain kinds of infections, and severe allergic reactions.
What Medications Should I Avoid If I Have Heart Failure
There are several different types of medications that are best avoided in those with heart failure including:
- Nonsteroidal anti-inflammatory medications such as Motrin or Aleve. For relief of aches, pains, or fever take Tylenol instead.
- Most calcium channel blockers
- Some nutritional supplements, such as salt substitutes, and growth hormone therapies
- Antacids that contain sodium
If youâre taking any of these drugs, discuss them with your doctor.
Itâs important to know the names of your medications, what theyâre used for, and how often and at what times you take them. Keep a list of your medications and bring them with you to each of your doctor visits. Never stop taking your medications without discussing it with your doctor. Even if you have no symptoms, your medications decrease the work of your heart so that it can pump more effectively.
Congestive Heart Failure Drugs
There are several medications that can be used to treat CHF, including ACE inhibitors, beta-blockers, and more.
ACE inhibitors
Angiotensin-converting enzyme inhibitors open up narrowed blood vessels to improve blood flow. Vasodilators are another option if you cant tolerate ACE inhibitors.
You may be prescribed one of the following:
- perindopril
- trandolapril
ACE inhibitors shouldnt be taken with the following medications without consulting a doctor, because they may cause an adverse reaction:
- Potassium-sparing diuretics and potassium supplements. These diuretics can cause potassium buildup in the blood, which may lead to abnormal heart rhythms. Examples include: riamterene , eplerenone , and spironolactone .
- Nonsteroidal anti-inflammatory drugs .NSAIDs such as ibuprofen, aspirin, and naproxen, can cause sodium and water retention. This may reduce the ACE inhibitors effect on your blood pressure.
This is an abbreviated list, so always speak with your doctor before taking any new medications.
Beta-blockers
Beta-blockers decrease the work the heart has to do and can reduce blood pressure and slow a rapid heart rhythm.
This may be achieved with:
Beta-blockers should be taken with caution with the following medications, as they may cause an adverse reaction:
Some medications may not be listed here. You should always consult your doctor before taking any new medications.
Diuretics
Your doctor may recommend:
Read Also: How To Find Thrz
What Is The Outlook For Heart Failure Patients
Very good, particularly now compared to prior generations, says Dr. Jacoby. We have medicines and treatments that reverse many cases of heart failure, and in most cases, the outlook is generally very good.
In cases where reversal of damage to the heart and affected areas is not possible, Dr. Jacoby says that the Yale Medicine team follows the patient closely and works to optimize quality of life while treating him or her.
Pearls And Other Issues
To reduce heart failure hospitalizations, it is reasonable to use Ivabradine in patients with NYHA II-III with guideline-directed medical therapy and heart rate of more than 70 bpm.
Heart failure disease management is a complex condition that requires a multidisciplinary framework for the care of patients, including discharge planning, patient education, and frequent outpatient assessment.
Recommended Reading: How Do You Say Heart Attack In Spanish
How Do I Know If My Chf Is Getting Worse
Because early treatment of worsening CHF is most effective in preventing hospitalizations, it is very important for the patient to recognize when his symptoms are getting worse. The early symptoms or warning signs of a CHF exacerbation can be different for each person. The patient is the best person to know if he or she is having difficulty breathing, feeling more tired, or gaining more weight. Family members or friends may also recognize some of these signs. Therefore, it is important that you inform your family and friends of these warning signs and let them know what to do if they see them. A change or increase in the symptoms usually experienced may be the only early warning signs you get.
You may notice one or more of the following signs of worsening CHF:
Weight gain: A gain of more than 3 pounds in 24 hours or 5 pounds in a week, no matter what your symptoms are.
Persistent coughing or wheezing: Though some-times misinterpreted by patients and doctors as a chest cold or bronchitis, coughing and wheezing can be a sign of worsening CHF. It results from a build-up of fluid in the lungs. When it is severe, the patient may notice white or pink blood-tinged mucus. This is a serious sign and should prompt a call to your physician and requires a trip to the emergency room.
Malaise:Any feeling of ill health, increased fatigue, and lack of energy that continues for more than 24 hours.
Cyanosis:Any blue color in the lips or fingernails.
Weird Aches And Pains
Heart failure rarely causes chest pain. Instead, weirdly enough, strange aches and pains may appear in odd places during mild exertion, such as climbing stairs. The jaw is a common location to experience heart failure pain. Other sites the pain can occur are the arms, the shoulders, the back, and even the abdomen. If you feel weird pains during exertion that subside once youve rested, you should consult a doctor.
Recommended Reading: Can Reflux Cause Heart Palpitations
A Bluish Tint To The Skin
As congestive heart failure worsens, the poor circulation and fluid accumulation in the lungs can make it difficult for the body to provide sufficient oxygen to the tissues. This symptom can cause the skin to appear pale or even mildly blue since well-oxygenated blood is bright red while poorly oxygenated blood is blue.
Outlook For Heart Failure
Heart failure is a serious long-term condition that’ll usually continue to get slowly worse over time.
It can severely limit the activities you’re able to do and is often eventually fatal.
But it’s very difficult to tell how the condition will progress on an individual basis.
It’s very unpredictable. Lots of people remain stable for many years, while in some cases it may get worse quickly.
You May Like: Can Anemia Cause Heart Failure
What Are The Symptoms Of Congestive Heart Failure
Daniel Louis Jacoby, MD, director of Yale Medicines General Heart Failure Program and the Cardiomyopathy Inherited Cardiovascular Disease Program, says that symptoms may be mild or severe and may not always be noticeable.
Most commonly, though, a patient may experience shortness of breath, fatigue, problems with the hearts rhythm called arrhythmias, and edemaor fluid buildupin the legs, he says.
Living With Heart Failure
Today, people with heart failure are living longer and more comfortably. Therapeutic advances have played a large role, but they aren’t the only answer. If you have heart failure, here are some ways you can improve your quality of life:
Reduce risk factors. It’s never too late to eliminate the factors that may have contributed to heart failure. Stop smoking. Lose weight. Be physically active. Eat a heart healthy diet loaded with vegetables, fruits and whole grains. Avoid salt. Use monounsaturated and polyunsaturated fats rather than saturated fat. Drink alcohol only if allowed by your doctor.
Take your medication. Dont change your dose or quit taking a medication without consulting your clinician, even if you’re feeling better.
Weigh yourself daily. If you suddenly gain a few pounds, you may have increased fluid build-up that demands immediate attention.
Monitor yourself carefully. Some patients keep a daily log to record their weight and evaluate key symptoms breathlessness, fatigue, and swelling on a one-to-five scale. See your physician at the first sign of a new or worsening symptom. Many people with heart failure die because they wait too long to seek help.
Recommended Reading: Reflux And Palpitations
How Does Heart Failure Affect The Body
Heart failure can affect the right side of the heart, the left side of the heart, or both sides.
When the right side of the heart begins to function less efficiently, it is unable to pump much blood forward into the vessels of the lungs. Because of the congestion in the right side of the heart, blood flow begins to back up into the veins. Eventually, swelling is noticed in the feet, ankles, lower legs, eyelids, and abdomen due to fluid retention.
When the left side of the heart fails, it is unable to pump blood forward out to the body efficiently. Blood begins to back up into the vessels in the lungs, and the lungs become stressed. Breathing becomes faster and more difficult. Also, the body does not receive enough blood to meet its needs, resulting in fatigue and poor growth in children.
Surgical Treatments For Congestive Heart Failure
A variety of surgical procedures may be used in the treatment of some cases of congestive heart failure including:
- and stent placement or coronary artery bypass may be an option for people with congestive heart failure who have severely blocked coronary arteries.
- Heart transplant may be the only treatment option in severe cases of congestive heart failure in which medications and lifestyle and dietary changes do not improve heart function.
- Left is a device surgeons connect to the heart to improve heart function. It may be used as a “bridge treatment” while waiting for a or as a treatment in itself.
- may be used in some cases to control abnormal heart rhythms.
- Valve surgery repair or replacement of damaged heart valves
Recommended Reading: How Much Can Marijuana Increase A Person’s Heart Rate
Signs Of Congestive Heart Failure People Often Miss
Most people are unaware that congestive heart failure affects 5% of people older than 60 and 2% of people between the ages of 40 and 60 this condition can also affect children, teenagers, and young adults. It affects men and women at equal rates, and black Americans are at higher risk of developing the condition than white Americans, Asian-Americans, or Hispanic-Americans. Doctors in the United States diagnose an estimated half a million new cases of heart failure each year.
Individuals with heart failure often end up being hospitalized multiple times, and the five-year survival rate after diagnosis is less than 50%. People with heart failure are also prone to just suddenly dying close to 300,000 people die from heart failure in the US every year.
Everyone knows the signs of an acute heart attack. Men usually experience severe pain in their chest along with cold sweating and dizziness, while women may or may not experience pain in their jaw, neck, arms, or upper back, along with severe sweating and dizziness. However, practically no one is aware of the signs and symptoms of heart failure. Here, we will discuss how to recognize the possible presence of heart failure.
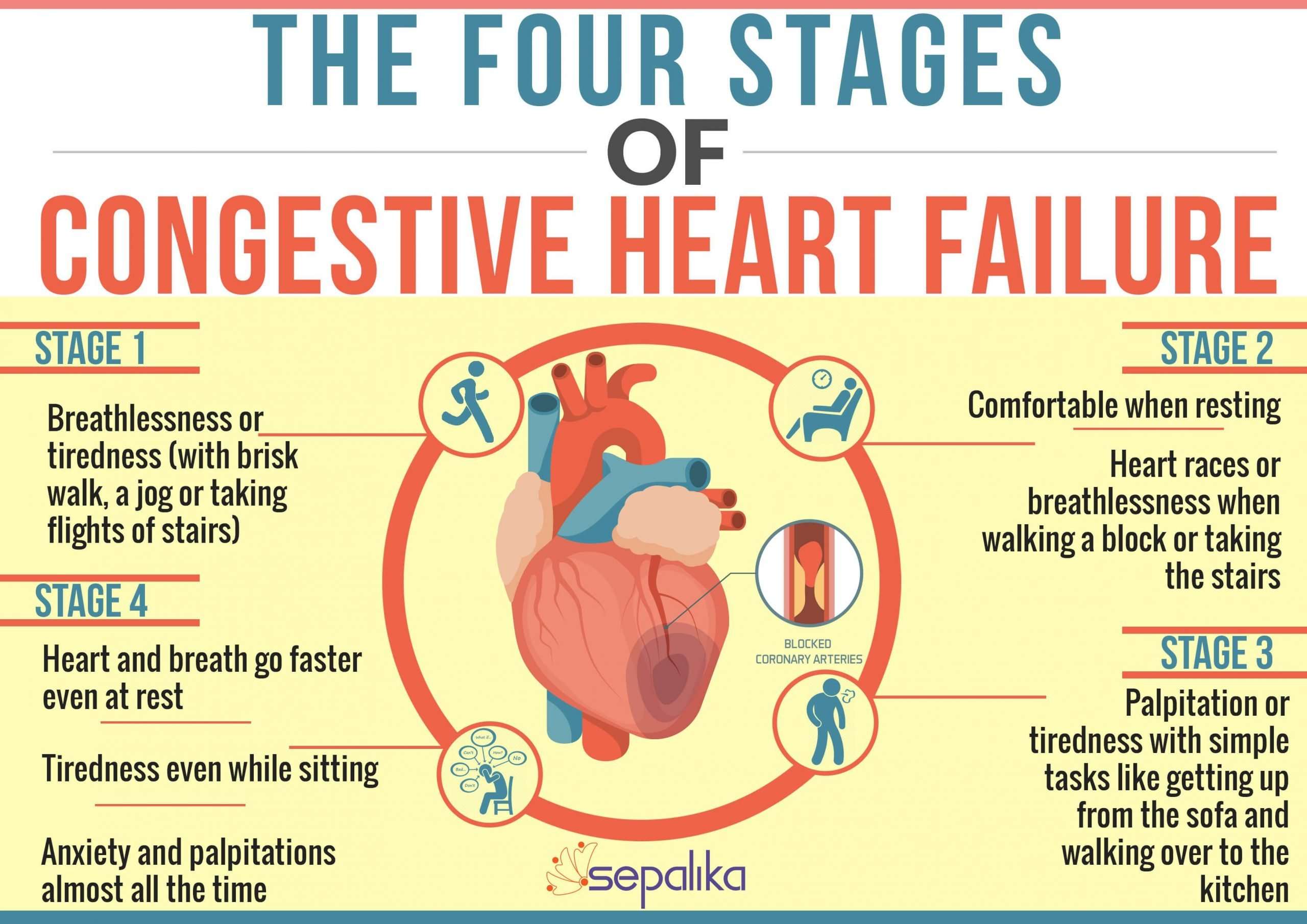
What Are The Stages Of Heart Failure
Heart failure is a chronic long-term condition that gets worse with time. There are four stages of heart failure . The stages range from “high risk of developing heart failure” to “advanced heart failure,” and provide treatment plans. Ask your healthcare provider what stage of heart failure you are in. These stages are different from the New York Heart Association clinical classifications of heart failure that reflect the severity of symptoms or functional limits due to heart failure.
As the condition gets worse, your heart muscle pumps less blood to your organs, and you move toward the next stage of heart failure. You cannot go backwards through the stages. For example, if you are in Stage B, you cannot be in Stage A again. The goal of treatment is to keep you from progressing through the stages or to slow down the progression.
Treatment at each stage of heart failure may involve changes to medications, lifestyle behaviors and cardiac devices. You can compare your treatment plan with those listed for each stage of heart failure. The treatments listed are based on current treatment guidelines. The table outlines a basic plan of care that may apply to you. If you have any questions about any part of your treatment plan, ask a member of your healthcare team.
Read Also: How Much Blood Does An Adult Heart Pump Every Day
Diuretics And Vasodilator Drugs For Congestive Heart Failure
Medications help control both the underlying causes of heart failure and the symptoms. Medications are the most critical part of therapy for heart failure. Usually, several types of medications are required to address as many of the physiologic imbalances as possible.
People with heart failure usually take several different medications that work in different ways to lessen heart failure symptoms, to prevent worsening of the underlying disease, and to prolong life.
Diuretics : The buildup of fluid is usually treated with a diuretic.
Vasodilators: These medications enlarge the small arteries or arterioles, which relieve the systolic workload of the left ventricle. Therefore, the heart has to work less to pump blood through the arteries. This also generally lowers blood pressure. Just as importantly, they reduce the levels of certain deleterious hormones and signals that can worsen heart failure.
What Makes Yale Medicines Approach To Treating Congestive Heart Failure Unique
We have a very patient-focused team at Yale Medicine, says Dr. Jacoby. Every person seen here, we treat as an individual, rather than offering a simple cookie-cutter treatment plan.
Yale Medicines multidisciplinary team comprises of heart failure cardiologists and cardiac surgeons, dedicated advanced-practice, registered nurses and nurse coordinators, dietitians, exercise physiologists, financial counselors, immunologists specializing in transplants, psychologists, and specialists in palliative care.
In our multidisciplinary approach, we include the patients desires as well as input from the family, Dr. Jacoby says. We develop a plan for social work support and take into account all of their financial and emotional stresses in addition to their physical treatment needs.
Recommended Reading: How Accurate Is Fitbit Charge 2 Heart Rate
Stages Of Heart Failure
In 2001, the American Heart Association and American College of Cardiology described the “Stages of Heart Failure.” These stages, which were updated in 2005, will help you understand that heart failure is often a progressive condition and can worsen over time. They will also help you understand why a new medication was added to your treatment plan and may help you understand why lifestyle changes and other treatments are needed.
The stages classified by the AHA and ACC are different than the New York Heart Association clinical classifications of heart failure that rank patients as class I-II-III-IV, according to the degree of symptoms or functional limits. Ask your doctor what stage of heart failure you are in.
Check the table below to see if your therapy matches what the AHA and ACC recommend. Note that you cannot go backward in stage, only forward.
The table below outlines a basic plan of care that may or may not apply to you, based on the cause of your heart failure and your special needs. Ask your doctor to explain therapies that are listed if you do not understand why you are or are not receiving them.
The New York Heart Association clinical classifications of heart failure rank people as class I-II-III-IV, according to the degree of symptoms or functional limits. You can ask your doctor if you want to know what stage of heart failure youâre in.
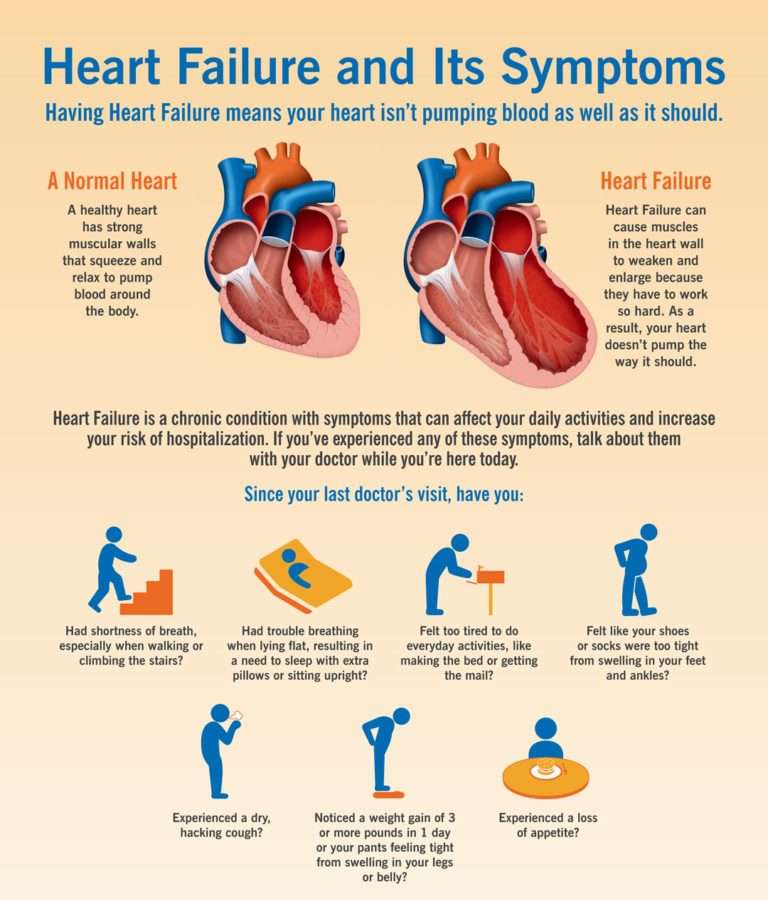
Symptoms Of Heart Failure
Symptoms of heart failure include:
- new or worsening shortness of breath
- difficulty lying flat at night
- fainting or passing out
- weight gain
- muscular fatigue, tiredness
- swelling of ankles or legs
- swelling of abdomen
- heart palpitations
- chest pain or discomfort in parts of the upper body
- unexplained coughing and wheezing
- constipation.
You May Like: How To Calculate Target Heart Rate Zone
How Is Congestive Heart Failure Treated
We assess the current health status of the patient to establish a baseline and develop a long-term health plan with the goal of improving the patients health, says Dr. Jacoby. This may involve the optimization of medicines and therapies, adding new medication or maybe enrollment in one of the clinical trials going on here.
Theres no quick fix, he says. Stabilizing and/or reversing a patients condition often involves long-term collaborative follow-up with a referring cardiologist or physician, Dr. Jacoby says.
In worst-case scenarios, we may offer advanced therapies, which include mechanical solutions, a heart transplant or hospice, Dr. Jacoby says. But first, we work very closely with our partners in cardiology and Interventional Cardiology Program at Yale to see if the patient would benefit from any interventional strategies.
“Yale has the best program in the area for heart transplants and artificial parts, but we want to exhaust all other options to avoid either if we can.
What You Can Do
Although some risk factors of heart failure, like age, cant be modified, people with CHF can take actions to improve their long-term prognosis. The first step is to become familiar with any family history of heart disease and learn about all the possible symptoms. Don’t ignore suspicious symptoms: let your doctor know about them. Regular exercise and managing concurrent conditions can also help keep CHF under control.
Read Also: How Much Can Marijuana Increase A Person’s Heart Rate
