What Is Atrial Fibrillation
Atrial fibrillation is a specific type of irregular heartbeat where the upper chambers of the heart beat out of sync with the lower chambers. A patient might notice symptoms such as irregular heartbeat, heart palpitations, shortness of breath, fatigue, and weakness. Some types of arrhythmias are chronic, but post-operative AFib often resolves on its own by the time the chest heals.
Areas For Further Investigation
As described above, there is a paucity of definitive data in the form of appropriately powered randomized controlled trials to determine whether a successful reduction in AFACS burden by means of the above prevention and treatment strategies translates into a meaningful decrease in adverse outcomes, such as cerebrovascular events or other thromboembolic events, morbidity from anticoagulation, mortality, critical care or hospital lengths-of-stays, or quality of life. Unfortunately, as eloquently noted by Sessler in his recent call to action , this lack of adequately sized trials providing clinically actionable results is not limited to AFACS investigations but is widespread across many disciplines.
It remains uncertain whether prophylactic interventions to prevent AFACS should be limited only to high-risk patients or whether all patients should receive at least some of these interventions.
Risk Factors For Afacs
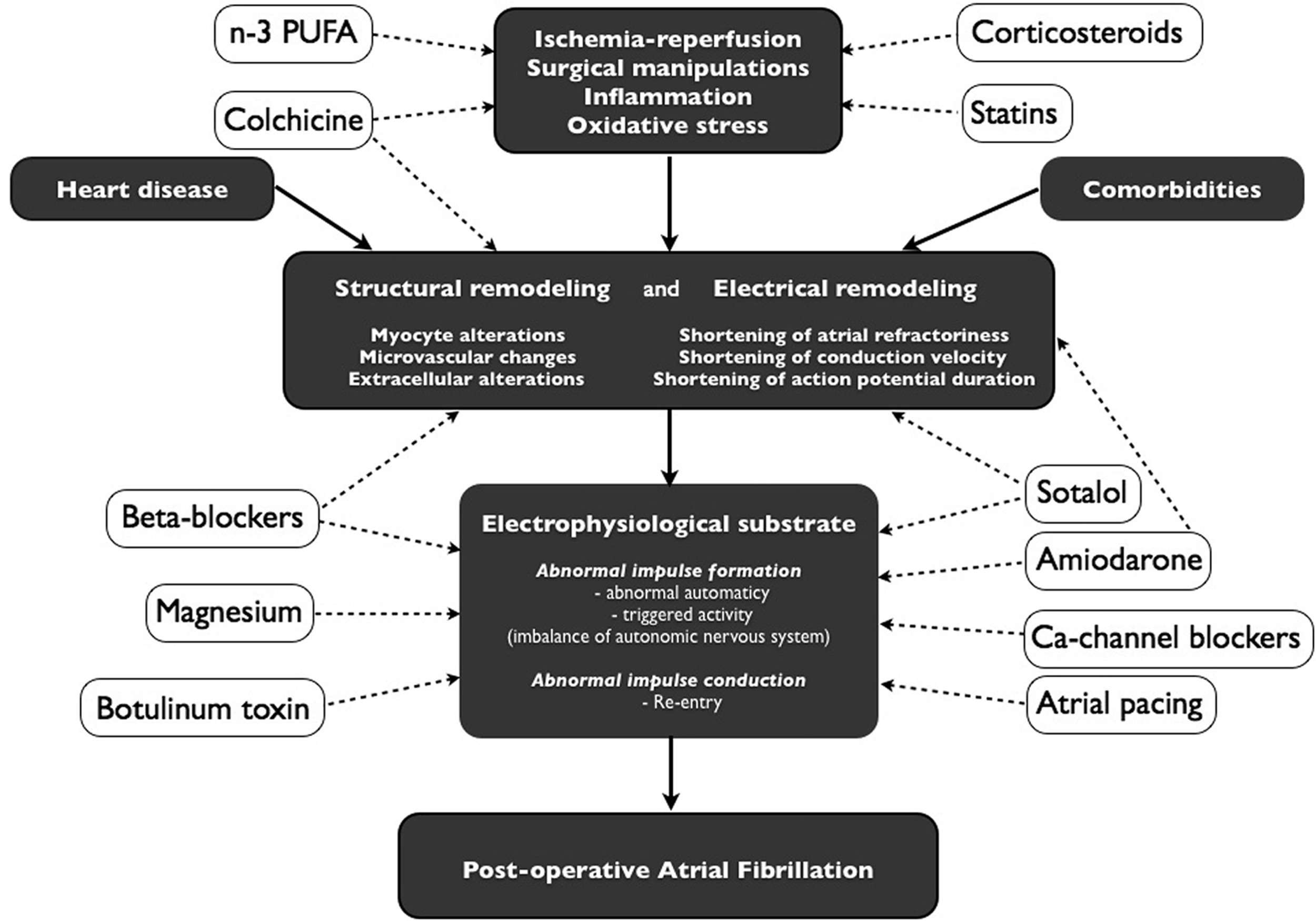
Different series have reported a number of risk factors for the development of AFACS including a prior history of paroxysmal AF, obesity, chronic obstructive pulmonary disease, chronic renal failure, rheumatic heart disease, and male gender, as well as echocardiographic predictors such as abnormal left ventricular systolic and diastolic function, left ventricular hypertrophy, and increased left atrial volume. The most consistent independent risk factor across multiple studies has been increasing patient age . A number of scoring systems have been generated to predict the risk of developing AFACS with the goal of being able to preoperatively identify high-risk patients to allow for use of appropriately targeted prophylactic regimens as recommended by a number of societal guidelines . Furthermore, to date, consistent reproducibility of factors between studies has been lacking and a post hoc validation analysis utilizing three risk scores derived from some of the largest trials obtained a low predictive value for these scores when applied prospectively to a patient cohort . It remains speculative whether the identification of a higher risk AF population could ultimately translate to improve patient outcomes, although AFACS rates, and associated increases in length of stay and cost, might as well be reducible with targeted aggressive prevention.
Fig. 1.
Don’t Miss: Can Anemia Cause Heart Failure
Anticoagulation Strategies For The Management Poaf
In contrast, the use of such therapy increases the risk of bleeding and cardiac tamponade, due to complex coagulation changes, including reduction of coagulation factors, changes in platelet function, and increase in fibrinolytic products related to the procedure. However, the merit of anticoagulation in postoperative patients after cardiac surgery should be carefully weighed against the increased risk of bleeding. This risk may even exceed the benefits in reducing stroke in some patients, especially those with the following risk factors: advanced age, uncontrolled hypertension, and previous bleeding history.
Understanding The Heart’s Electrical System
To understand AF, it helps to understand the heart’s internal electrical system. The heart’s electrical system controls the rate and rhythm of the heartbeat.
With each heartbeat, an electrical signal spreads from the top of the heart to the bottom. As the signal travels, it causes the heart to contract and pump blood. The process repeats with each new heartbeat.
Each electrical signal begins in a group of cells called the sinus node or sinoatrial node. The SA node is located in the right atrium. In a healthy adult heart at rest, the SA node fires off an electrical signal to begin a new heartbeat 60 to 100 times a minute.
From the SA node, the electrical signal travels through the right and left atria. This causes the atria to contract and pump blood into the ventricles.
The electrical signal then moves down to a group of cells called the atrioventricular node, located between the atria and the ventricles. Here, the signal slows down just a little, allowing the ventricles time to finish filling with blood.
The electrical signal then leaves the AV node and travels to the ventricles. This causes the ventricles to contract and pump blood out to the lungs and the rest of the body. The ventricles then relax, and the heartbeat process starts all over again in the SA node.
For more information on the heart’s electrical system and detailed animations, go to the Diseases and Conditions Index How the Heart Works article.
Also Check: Can Lexapro Cause Heart Palpitations
How Else Can I Improve The Success Rate Of An Afib Ablation
Another reason why some people exeprience AFib after an ablation is what I would call: missing pieces of the puzzle. There are many factors that are outside of the ablation itself which have been found to improve the success rate of the ablation procedure as well. Most of these are involved in the category of lifestyle modifications or managing other health conditions. Probably one of the most studied lifestyle modification that can also improve AFib ablation is weight loss. Weight loss had been found to significantly improve AFib, but it has also been found to improve AFib in the setting of a catheter ablation, to improve the success rate of the ablation itself.
When patients are overweight they are also at increased risk for high blood pressure and diabetes, which can also contribute AFib, as well as increasing the scar tissue in the left atrium. However, the fat molecules themselves, whether that’s fat molecules around the waist or even fat molecules that develop around the heart tissue, can all secrete hormones which increase inflammation, which can then in turn continue to lead to progressions of AFib. That is a reason why weight loss has been shown to have significant improvement in AFib. And one of the biggest diet studies to date called the LEGACY trial.
Is Atrial Fibrillation Common After Open Heart Surgery
Answered by: Dr U Kaul | Director, Director of Cardiology, Fortis Group of Hospitals, Noida and New Delhi
Q: My father recently had an aortic valve replaced. The surgery went well, but the cardiologist told us that he has atrial fibrillation post surgery, which is normal. To correct this, he has to be admitted to the hospital for a month and have his heart shocked into normal sinus rhythm. Why is this needed? Was the heart purposely left in the a-fib state, only to be returned to normal after sometime?
A:Transient atrial fibrillation after open heart surgery is seen often.It usually responds to drugs like amiodarone, which some surgeons like to continue for a few weeks to months. Most cardiovascular teams usually prefer to send the patient home in normal sinus rhythm even if cardioversion is required. However, it is the choice of the treating team.It is always preferable to bring the patient to normal rhythm even though atrial fibrillation with control of the heart rate can be resorted to in cases with frequent recurrences.
Read Also: Flonase Heart Rate
Af Pathophysiology And Mechanisms
AF is a supraventricular arrhythmia characterized by erratic atrial depolarizations leading to disorganized, ineffective atrial contractions, and variable atrioventricular nodal conduction, which results in an irregular ventricular rate . An expert consensus document defined the diagnosis of AF as requiring a 12-lead electrocardiogram or a rhythm strip of at least 30-s duration that demonstrates irregular RR intervals in the absence of complete AV block, an absence of distinct P waves on surface ECG, and an atrial cycle length that is variable and generally less than 200 ms .
Two separate phases regarding the risk of development of AFACS, with distinct associated factors, have been described. The first phase encompasses the first 18 h postoperatively with the greatest risk at hour zero, and the second phase occurs with the risk peaking at 2448 hrs . This observation raises the possibility that separate mechanisms may be responsible for AFACS development within each phase.
How Should I Prepare For My Surgical Ablation
Donât smoke for at least 2 weeks before your heart surgery. It may cause problems with your breathing or blood clotting during or after your procedure.
The night before your surgery, bathe or shower. Donât eat after midnight the day before your surgery. Food or drinks in your stomach may cause you to have problems with your anesthesia. It can cause you to vomit and breathe it in.
Don’t Miss: Does Acid Reflux Cause Heart Palpitations
How Does Anesthesia Affect Your Heart
Even in healthy patients having minor operations, anesthetic agents can cause significant cardiac depression and hemodynamic instability. Virtually all anesthetic agents have intrinsic myocardial depressant properties, although some may mask this with sympathetic stimulation.
Who Is At Risk For Atrial Fibrillation
More than 2 million people in the United States have atrial fibrillation . It affects both men and women.
The risk of AF increases as you age. This is mostly because as you get older, your risk for heart disease and other conditions that can cause AF also increases. However, about half of the people who have AF are younger than 75.
AF is uncommon in children.
You May Like: Does Benadryl Increase Your Heart Rate
What To Expect Before And During The Maze Procedure
At the hospital, your nurse may test your blood or urine, or give you a chest X-ray to make sure you donât have any infections or problems that may hurt your surgeryâs success. You may be given medication to help you relax before the surgery.
Youâll have electrocardiogram electrodes attached to your chest and back to keep track of your heartbeat. You will get anesthesia to put you to sleep during the surgery.
After you are asleep, your doctor will connect you to a respirator that has a tube that goes down your throat. This will help you breathe during the operation. You may have a tube inserted into your throat to help collect fluid or air in your stomach during the operation. You may also have a catheter inserted in your bladder to collect urine during the operation.
Your surgeon will cut into your chest during your operation, and they will insert instruments to make the small interior cuts or make lesions on your heart tissue. Depending on the type of maze procedure you have, your surgeon may use tiny video cameras or robotic arms to help perform the operation.
Approaches To Treating Underlying Causes And Reducing Risk Factors
Your doctor also may recommend other treatments for an underlying condition that may be causing AF or to reduce AF risk factors. For example, he or she may prescribe medicines to treat an overactive thyroid or reduce blood pressure.
Your doctor also may recommend lifestyle changes, such as following a healthy diet, cutting back salt intake , quitting smoking, and reducing stress.
Limiting or avoiding stress and alcohol, caffeine, or other stimulants that may increase your heart rate also may help reduce the risk of AF.
Read Also: How Does Heart Disease Affect The Skeletal System
Rate Vs Rhythm Control
Available data suggest that most cases of AFACS return to a sinus rhythm at the end of 24 hrs regardless of treatment strategy . An RCT published in 2000 randomized 50 cardiac surgery patients with new-onset AF to rate vs rhythm control and found no difference in the time of conversion to sinus rhythm and no difference in relapse rates for the 2-month follow-up duration, although hospital length of stay was reduced in the antiarrhythmic arm .
The most frequently used agents for rate control are beta-blockers and non-dihydropyridine calcium channel blockers, and these can potentially be used in combination . A variety of target ventricular rates, from 80110 bpm, have been proposed . The cumulative effects of drugs given for controlling the ventricular response rate in AF can cause problematic bradycardia in the event of spontaneous cardioversion to sinus rhythm.
SCA/EACTA, ESC, and ACC/AHA/HRS guidelines all include Class IIa recommendations for managing asymptomatic patients with rate control and anticoagulation, with ACC/AHA/HRS guidelines also recommending cardioversion if the AF does not spontaneously revert to sinus rhythm during subsequent follow-up .
Digoxin
Treatment Strategies And Associated Evidence Base
The treatment strategies for AFACS depend on hemodynamic stability and clinical symptoms. The approach to a hemodynamically stable patient is broadly classified into rate control, rhythm control, and concomitant thromboprophylaxis . These treatment strategies and the associated strength of society recommendation, if available, are summarized in Table 2.
Recommended Reading: 10 Second Trick To Prevent Heart Attack
Pathophysiology Of Postoperative Atrial Fibrillation
At present, it is hypothesized that AF is initiated by ectopic beats predominantly originating from the thoracic veins. Reentry, increased automaticity, and triggered activity have all been postulated as mechanisms that can cause arrhythmogenesis from the pulmonary veins. Some studies have indicated that an electrophysiological substrate within the pulmonary veins allows reentry due to heterogeneous refractory periods and decremental conduction. The pathophysiology of AF involved reentry of multiple wavelets which circulate around the atrium. Other studies have indicated that automaticity is the potential mechanism because of dependence on adrenergic stimuli and the presence of dissociated autonomic rhythms within the pulmonary veins that are electrically isolated from the left atrium. It has been noted that soon after disconnection of the pulmonary veins from the left atrium, the cycle length of electrical activity within the pulmonary veins becomes longer, and eventually the tachycardia resolves suggesting that the muscle sleeves surrounding the pulmonary veins depend upon electrical input from the left atrium to maintain pulmonary vein tachycardia. Dependence on an external input and the response to calcium channel blockers are in accordance to triggered activity. It is likely that the mechanism responsible for the initiation and perpetuation of AF is multifactorial .
Atrial Fibrillation After Surgery Increases Risk Of Heart Attacks Strokes
- Date:
- Loyola University Health System
- Summary:
- An irregular heartbeat following surgery known as post-operative atrial fibrillation often is dismissed as a transient phenomenon. But a study has found that POAF can significantly increase the risk of heart attack or stroke during the first 12 months after surgery.
As many as 12 percent of patients undergoing major, non-cardiac surgery experience an irregular heartbeat called atrial fibrillation.
Post-operative atrial fibrillation often is dismissed as a transient phenomenon. But a Loyola University Medical Center study has found that POAF can significantly increase the risk of heart attack or stroke during the first 12 months after surgery.
Among bladder cancer patients who underwent a cystectomy and developed POAF, 24.8 percent experienced a heart attack or stroke during the first 12 months after surgery. By comparison, 10.9 percent of patients who did not experience postoperative atrial fibrillation experienced a heart attack or stroke during the first year.
“Physicians should be vigilant in assessing postoperative atrial fibrillation, even when transient, and establish appropriate follow-up, given the increased risk of cardiovascular morbidity,” first author Robert Blackwell, MD, senior author Gopal Gupta, MD, and colleagues report in the Journal of Urology.
Story Source:
Read Also: Does Tylenol Increase Heart Rate
Medical And Family Histories
Your doctor will ask questions about your:
- Signs and symptoms. What symptoms are you having? Have you had palpitations? Are you dizzy or short of breath? Are your feet or ankles swollen ? Do you have any chest pain?
- Medical history. This includes other health problems, such as a history of heart disease, high blood pressure, lung disease, diabetes, or thyroid problems.
- Family’s medical history. Does anyone in your family have a history of AF? Has anyone in your family ever had heart disease or high blood pressure? Has anyone had thyroid problems? Are there other illnesses or health problems in your family?
- Health habits. Your doctor may ask whether you smoke or use alcohol or caffeine.
Effectiveness Of Pulmonary Vein Isolation In Prevention Of Atrial Fibrillation Following Heart Bypass Surgery
| The safety and scientific validity of this study is the responsibility of the study sponsor and investigators. Listing a study does not mean it has been evaluated by the U.S. Federal Government. Read our disclaimer for details. |
| First Posted : June 20, 2006Last Update Posted : February 8, 2011 |
Atrial fibrillation is an irregular heart rhythm that occurs in 30% to 40% of patients following heart surgery. This irregular heart rhythm, although often self-limiting, can be cause for concern. AF is associated with a two-fold increase in patient complications and mortality after heart surgery. During AF, the heart muscle does not contract properly causing the blood flow through the heart to slow down potentially forming clots. A clot may then enter the blood stream and be carried to the brain, possibly causing a stroke. Patients in persistent AF require blood thinners to prevent strokes, and this carries its own bleeding risks especially in elderly patients.
Recently, Medtronic has developed the Cardioblate® BP and BP 2 Surgical Ablation System devices to perform pulmonary vein isolation to treat AF. Vichol et al have demonstrated a mean ablation time of 15.2 seconds per lesion with the use of this device.
Study Question/Purpose:
Hypothesis:
Trial Implementation
Recommended Reading: Fitbit Charge 2 Heart Rate Accuracy
Taking Care Of Atrial Fibrillation After Surgery
While in recovery following heart or other surgery, you’re likely to be on a heart monitor so that the nursing staff can check you for atrial fibrillation by looking for a heart rate that’s over 160 beats per minute . Most people can feel if their heart flutters and their pulse races. But some, exhausted from surgery, may not, Doshi says. That’s why patients are closely monitored.
Most of the time, post-operative afib goes away by itself. If not, you may need to take medication to control both heart rate and heart rhythm.
Your doctor also may give you a blood thinner to prevent a stroke, which is the biggest concern with afib. Blood thinners prevent clots that can form and break off, causing a stroke. But depending on the type of surgery you had, your doctor may need to wait for your safety before prescribing a blood thinner. The wait can vary from a day to a week or so, Doshi says.
Depending on the extent of the afib, your heart might need to be shocked back into normal rhythm with a procedure known as cardioversion, notes the Heart and Vascular Institute at Johns Hopkins Medicine in Baltimore.
