Facts About Heart Failure In The United States
- About 6.2 million adults in the United States have heart failure.1
- In 2018, heart failure was mentioned on 379,800 death certificates .1
- Heart failure costs the nation an estimated $30.7 billion in 2012.2 This total includes the cost of health care services, medicines to treat heart failure, and missed days of work.
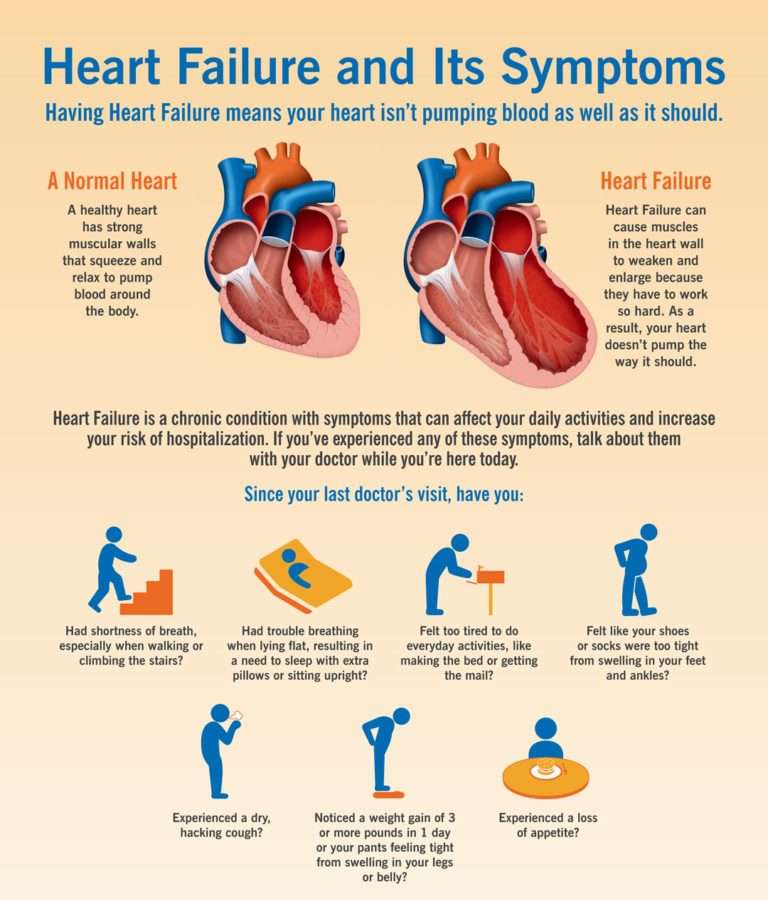
The 4 Stages Of Congestive Heart Failure
There are four stages of CHF, including Stage A, B, C, and D. In the early stages a patient may have a high risk of developing heart failure, whereas a patient with Stage D, will have advanced heart failure.
To find out what stage youre in, ask your doctor. Next, well take a closer look at what each stage of heart failure entails.
Among The Nation’s Best
U.S. News & World Report has once again ranked the Herma Heart Institute at Children’s Wisconsin among the top programs in the nation for pediatric cardiology and heart surgery. This ranking reflects the excellent outcomes and care we provide for even the most complex heart conditions. Families travel from across the country, and even around the world, to receive care from our specialists who are experienced in treating congenital heart disease from before birth and into adulthood.
Don’t Miss: How Does Heart Disease Affect The Skeletal System
How Do I Know If My Chf Is Getting Worse
Because early treatment of worsening CHF is most effective in preventing hospitalizations, it is very important for the patient to recognize when his symptoms are getting worse. The early symptoms or warning signs of a CHF exacerbation can be different for each person. The patient is the best person to know if he or she is having difficulty breathing, feeling more tired, or gaining more weight. Family members or friends may also recognize some of these signs. Therefore, it is important that you inform your family and friends of these warning signs and let them know what to do if they see them. A change or increase in the symptoms usually experienced may be the only early warning signs you get.
You may notice one or more of the following signs of worsening CHF:
Weight gain: A gain of more than 3 pounds in 24 hours or 5 pounds in a week, no matter what your symptoms are.
Persistent coughing or wheezing: Though some-times misinterpreted by patients and doctors as a chest cold or bronchitis, coughing and wheezing can be a sign of worsening CHF. It results from a build-up of fluid in the lungs. When it is severe, the patient may notice white or pink blood-tinged mucus. This is a serious sign and should prompt a call to your physician and requires a trip to the emergency room.
Malaise:Any feeling of ill health, increased fatigue, and lack of energy that continues for more than 24 hours.
Cyanosis:Any blue color in the lips or fingernails.
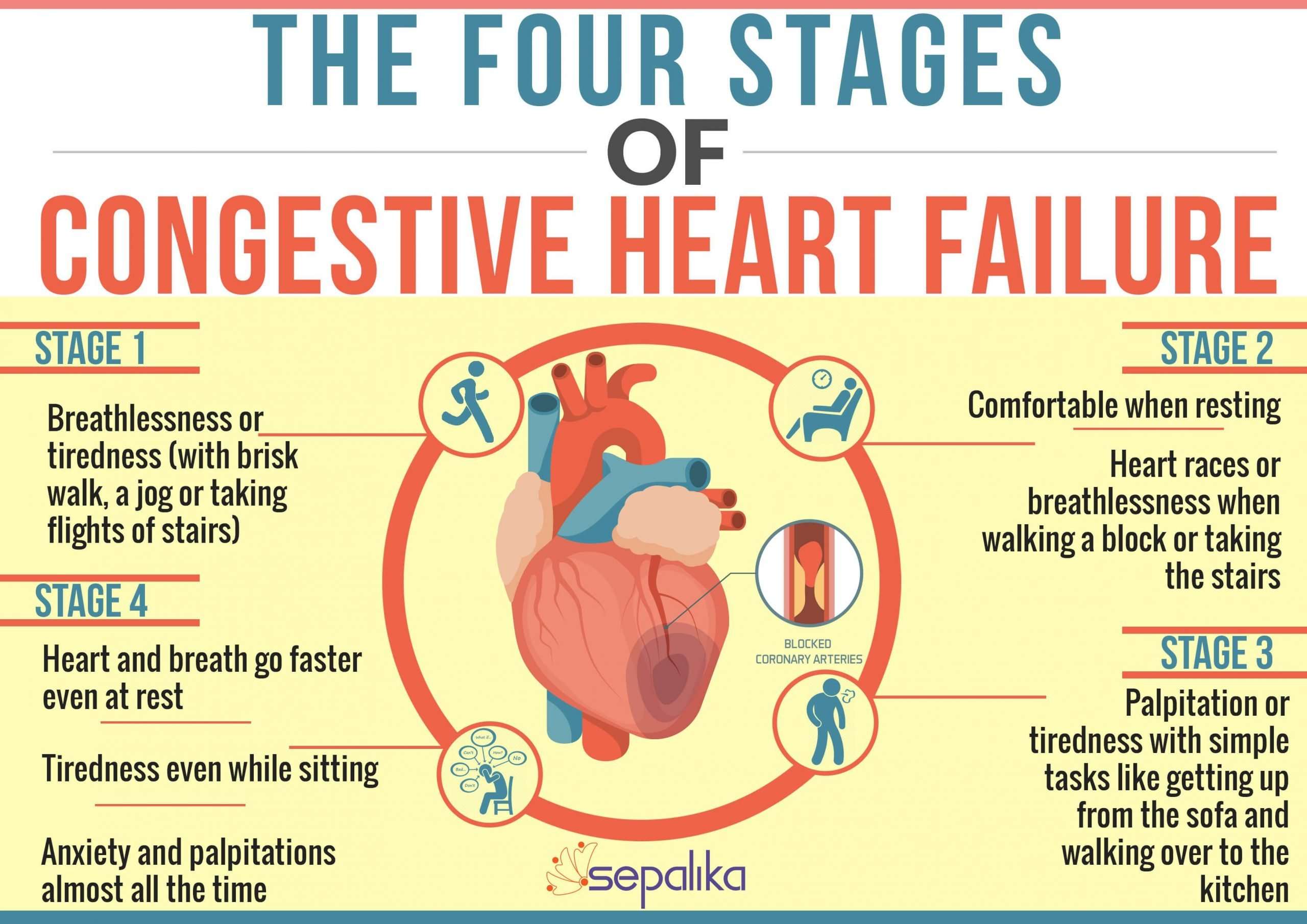
Stages Of Heart Failure
In 2001, the American Heart Association and American College of Cardiology described the “Stages of Heart Failure.” These stages, which were updated in 2005, will help you understand that heart failure is often a progressive condition and can worsen over time. They will also help you understand why a new medication was added to your treatment plan and may help you understand why lifestyle changes and other treatments are needed.
The stages classified by the AHA and ACC are different than the New York Heart Association clinical classifications of heart failure that rank patients as class I-II-III-IV, according to the degree of symptoms or functional limits. Ask your doctor what stage of heart failure you are in.
Check the table below to see if your therapy matches what the AHA and ACC recommend. Note that you cannot go backward in stage, only forward.
The table below outlines a basic plan of care that may or may not apply to you, based on the cause of your heart failure and your special needs. Ask your doctor to explain therapies that are listed if you do not understand why you are or are not receiving them.
The New York Heart Association clinical classifications of heart failure rank people as class I-II-III-IV, according to the degree of symptoms or functional limits. You can ask your doctor if you want to know what stage of heart failure youâre in.
Recommended Reading: Does Benadryl Lower Heart Rate
Understanding What Can Happen To Your Liver When Taking Ace Inhibitors
The first thing you need to know about using ACE Inhibitors is that you need to take the recommended dose on a daily basis. To be clear, the suggested dose is two times that of your maximum blood pressure. If you take your dose twice a day, you will have a significant rise in your blood pressure.
You should not exceed the maximum blood pressure that you would have if you were taking only one ACE Inhibitor tablet a day, and you should take it for the maximum suggested dosing period on a daily basis only. If you miss any of your doses, you should contact your doctor immediately to see if you need to increase the dose or stop taking it. If you do experience any side effects, these will need to be discussed with your doctor.
ACE Inhibitors can help you live longer and make your heart disease less of a risk. Your risk of developing congestive heart failure is much greater if you have high blood pressure. Many people with congestive heart failure do not receive the treatments they need because they are at risk of developing kidney failure.
The second thing that you need to know about taking ACE Inhibitors is that there are some serious side effects that you could experience. One of the side effects of taking ACE Inhibitors is called myocardial infarction. This is also known as heart attack, heart blockage, or sudden cardiac arrest.
Signs Of Congestive Heart Failure
No matter which type of congestive heart failure you may have developed, the symptoms are generally the same and include:
- Shortness of breath
- Trouble breathing when youre lying down
- Swelling in your ankles, legs, and abdomen
- Heart palpitations
- Dry cough
- Frequent urination at night
Many different conditions can lead to some of these symptoms. For example, a respiratory infection can often leave you short of breath, tired, and unable to breathe well when youre lying flat. If youre feeling these symptoms without an identifiable cause, such as the flu-like scenario we just described, its time to come see us for a full evaluation.
Don’t Miss: Can Flonase Cause Heart Palpitations
One Of The Other Dangerous Side Effects Of Taking Ace Inhibitors Is Called Dry Cough
This can be life-threatening, especially if you are elderly or have other health conditions that make it difficult for your body to properly breathe. In addition to experiencing dry cough, you may also experience nausea, vomiting, and severe diarrhoea. If you are pregnant, you should avoid taking the ace inhibitors at all costs, as well as any medications that contain bradykinin.
You should also be aware of the many side effects that can occur from taking ACE Inhibitors. If you notice any strange side effects that youve never experienced before, you should immediately contact your doctor and discuss the situation.
Your doctor will help you determine the correct dosage to take, as well as the proper way to use the medication. Although Aceon is one of the safest prescription drugs available, you should be aware of all of its possible side effects and should always keep tabs on your current doses.
When Left Alone Congestive Heart Failure Can Cause A Number Of Additional Problems Including
- Shortness of breath due to insufficient oxygen getting to the lungs
- Chest pains and palpitations
- Urinary retention
- Lightheadedness or dizziness
Patients with weak hearts are also at higher risk for low blood pressure, fainting and comatose. It is also very helpful to have close family and close friends who understand your situation to offer you encouragement and motivation.
Recommended Reading: Flonase Heart Racing
Factors That Can Worsen Symptoms Of Heart Failure
The symptoms of heart failure can be worsened by a number of factors, including:
- anaemia
- too much salt, fluid, or alcohol in the diet
- pregnancy
- some viral and bacterial infections
- kidney diseases
Treatment for heart failure may include:
- medicines, such as
- diuretics to remove excess fluid and improve symptoms of heart failure
- mineralcortiocoid receptor antagonists are also recommended and used in most patients with heart failure to reduce mortality and hospitalisation
- ACE inhibitors to open up blood vessels, reduce blood pressure and reduce sodium retention and water retention
- certain beta-blockers to slow the heart rate and reduce its work
- aldosterone blockers to reduce blood pressure and reduce the effects of damage to the heart muscle
- ACE inhibitors, beta blockers and aldosterone blockers can increase survival and reduce the likelihood of hospitalisation.
Cardiac Mortality In Placebo Controlled Heart Failure Trials
Trial
| 33 | 1.2 |
EF ejection fraction. SOLVD-P, SOLVD-T=studies of left ventricular dysfunction prevention arm and treatment arm .
H-ISDN=hydralazine and isosorbide dinitrate.
*Treatment with H-ISDN.
Treatment with angiotensin converting enzyme inhibitors prevents or delays the onset of symptomatic heart failure in patients with asymptomatic, or minimally symptomatic, left ventricular systolic dysfunction. The increase in mortality with the development of symptoms suggests that the optimal time for intervention with these agents is well before the onset of substantial left ventricular dysfunction, even in the absence of overt clinical symptoms of heart failure. This benefit has been confirmed in several large, well conducted, postmyocardial infarction studies.
You May Like: Does Benadryl Lower Heart Rate
Who Gets Congestive Heart Failure And What Are The Risk Factors
An estimated 6.2 million people in the United States have heart failure. Diseases and conditions that increase the risk of developing heart disease or cardiovascular disease also increase the risk of eventually developing congestive heart failure as a complication.
Risk factors include:
- Atherosclerosis and coronary artery disease
- Excessive alcohol consumption
- Sedentary lifestyle
- Smoking
Having high levels of certain substances in the body, which can be determined by blood tests, can also increase the risk for and congestive heart failure. These include:
- High cholesterol, which can lead to atherosclerosis
- High C-reactive protein level, which reflects inflammation
- High homocysteine level, which may damage artery walls and increase the risk of developing . Blood clots can cause a and lead to congestive heart failure.
Reducing your risk of congestive heart failure
You can reduce your risk of developing heart disease and congestive heart failure by:
- Eating a heart-healthy diet that is low in saturated fat and trans fats and high in fiber, whole grains, fruits, and vegetables
- Limiting alcohol intake to one drink per day for women and two drinks per day for men
- Maintaining a healthy weight
- Participating in a regular exercise program
- Reducing excessive stress
- Seeking regular medical care and prenatal care and following your treatment plan for such conditions as , obesity, hypertension, and diabetes
Causes Of Heart Failure
The heart is a double pump made up of four chambers. Deoxygenated blood from the veins enters the right upper chamber , is passed to the right lower chamber , and then pumped to the lungs.
Oxygenated blood from the lungs enters the left upper chamber and then enters the left lower chamber . The blood is then pumped around the body, under pressure, via arteries.
In a person with heart failure, one or both ventricles dont empty properly. This leads to increased pressure in the atria and the nearby veins. This backlog of blood can affect the kidneys and lungs interfering with their function and leading to a build-up of fluid in the lungs, abdominal organs and legs.
In some people with heart failure, rather than failed pumping of the blood from the ventricle, there is failed relaxation of the ventricle.
If the heart is not pumping and becomes stiff and unable to relax, it can cause the blood to pool in the hearts ventricles. This can cause pressure build up and can put strain on the heart.
Heart failure can be caused by several conditions, including:
Don’t Miss: Does Tylenol Increase Heart Rate
Sensitivity Specificity And Predictive Value Of Symptoms Signs And Chest X Ray Findings For Presence Of Heart Failure In 1306 Patients With Coronary Artery Disease Undergoing Cardiac Catheterisation
Clinical features
| 32 |
Oedema
Swelling of ankles and feet is another common presenting feature, although there are numerous non-cardiac causes of this symptom. Right heart failure may manifest as oedema, right hypochondrial pain , abdominal swelling , loss of appetite, and, rarely, malabsorption . An increase in weight may be associated with fluid retention, although cardiac cachexia and weight loss are important markers of disease severity in some patients.
What Do The Numbers Mean
Ejection Fraction 55% to 70%
- Pumping Ability of the Heart: Normal.
- Level of Heart Failure/Effect on Pumping: Heart function may be normal or you may have heart failure with preserved EF .
Ejection Fraction 40% to 54%
- Pumping Ability of the Heart: Slightly below normal.
- Level of Heart Failure/Effect on Pumping: Less blood is available so less blood is ejected from the ventricles. There is a lower-than-normal amount of oxygen-rich blood available to the rest of the body. You may not have symptoms.
Ejection Fraction 35% to 39%
- Pumping Ability of the Heart: Moderately below normal.
- Level of Heart Failure/Effect on Pumping: Mild heart failure with reduced EF .
Ejection Fraction Less than 35%
- Pumping Ability of the Heart: Severely below normal.
- Level of Heart Failure/Effect on Pumping: Moderate-to-severe HF-rEF. Severe HF-rEF increases risk of life-threatening heartbeats and cardiac dyssynchrony/desynchronization .
Normal Heart. A normal left ventricular ejection fraction ranges from 55% to 70%. An LVEF of 65%, for example means that 65% of total amount of blood in the left ventricle is pumped out with each heartbeat. Your EF can go up and down, based on your heart condition and how well your treatment works.
HF-pEF. If you have HF-pEF, your EF is in the normal range because your left ventricle is still pumping properly. Your doctor will measure your EF and may check your heart valves and muscle stiffness to see how severe your heart failure is.
Recommended Reading: Ibs And Heart Palpitations
Hypertension Or High Blood Pressure
Another cause of congestive heart failure is high blood pressure or hypertension. If you have high blood pressure, your heart muscle works extra hard to pump blood through your body.
As time passes, because of the overexertion, the muscles in your heart can become too weak or too stiff to properly circulate blood to your body. If you have high blood pressure, your heart muscle workextra hard to pump blood through your body.
A Bluish Tint To The Skin
As congestive heart failure worsens, the poor circulation and fluid accumulation in the lungs can make it difficult for the body to provide sufficient oxygen to the tissues. This symptom can cause the skin to appear pale or even mildly blue since well-oxygenated blood is bright red while poorly oxygenated blood is blue.
Also Check: Does Benadryl Lower Heart Rate
From Our Health Library At Upmccom
- Destination therapy
Bridge to transplantation
Each year, more people with end-stage heart failure are evaluated and listed for transplantation. Unfortunately, there are not enough suitable donor organs for all of the patients waiting for a heart transplant.
People who are listed for heart transplantation and are too ill to wait any longer, or are expected to have prolonged wait times, are referred for a VAD as a bridge to transplantation. The VAD allows them to recover and wait at home for an organ to become available.
Bridge to recovery
In some cases of heart failure particularly newly diagnosed CHF or heart failure after other cardiac surgery the heart may recover after a period of support on a VAD. These patients are supported temporarily as a bridge to recovery.
After implantation, the VAD is turned down and the heart is reassessed to see if its function has improved enough to allow the VAD to be removed.
Typically, people recommended for VAD as a bridge to recovery have CHF as a result of:
- Viral infection
Outlook For Heart Failure
Heart failure is a serious long-term condition thatll usually continue to get slowly worse over time.
It can severely limit the activities youre able to do and is often eventually fatal.
But its very difficult to tell how the condition will progress on an individual basis.
Its very unpredictable. Lots of people remain stable for many years, while in some cases it may get worse quickly.
You May Like: Can Anemia Cause Heart Failure
Recommended Reading: What Is A Dangerously High Heart Rate When Exercising
Congestive Heart Failure Drugs
There are several medications that can be used to treat CHF, including ACE inhibitors, beta-blockers, and more.
ACE inhibitors
Angiotensin-converting enzyme inhibitors open up narrowed blood vessels to improve blood flow. Vasodilators are another option if you cant tolerate ACE inhibitors.
You may be prescribed one of the following:
- perindopril
- trandolapril
ACE inhibitors shouldnt be taken with the following medications without consulting a doctor, because they may cause an adverse reaction:
- Potassium-sparing diuretics and potassium supplements. These diuretics can cause potassium buildup in the blood, which may lead to abnormal heart rhythms. Examples include: riamterene , eplerenone , and spironolactone .
- Nonsteroidal anti-inflammatory drugs .NSAIDs such as ibuprofen, aspirin, and naproxen, can cause sodium and water retention. This may reduce the ACE inhibitors effect on your blood pressure.
This is an abbreviated list, so always speak with your doctor before taking any new medications.
Beta-blockers
Beta-blockers decrease the work the heart has to do and can reduce blood pressure and slow a rapid heart rhythm.
This may be achieved with:
Beta-blockers should be taken with caution with the following medications, as they may cause an adverse reaction:
Some medications may not be listed here. You should always consult your doctor before taking any new medications.
Diuretics
Your doctor may recommend:
