Doctor’s Notes On Congestive Heart Failure
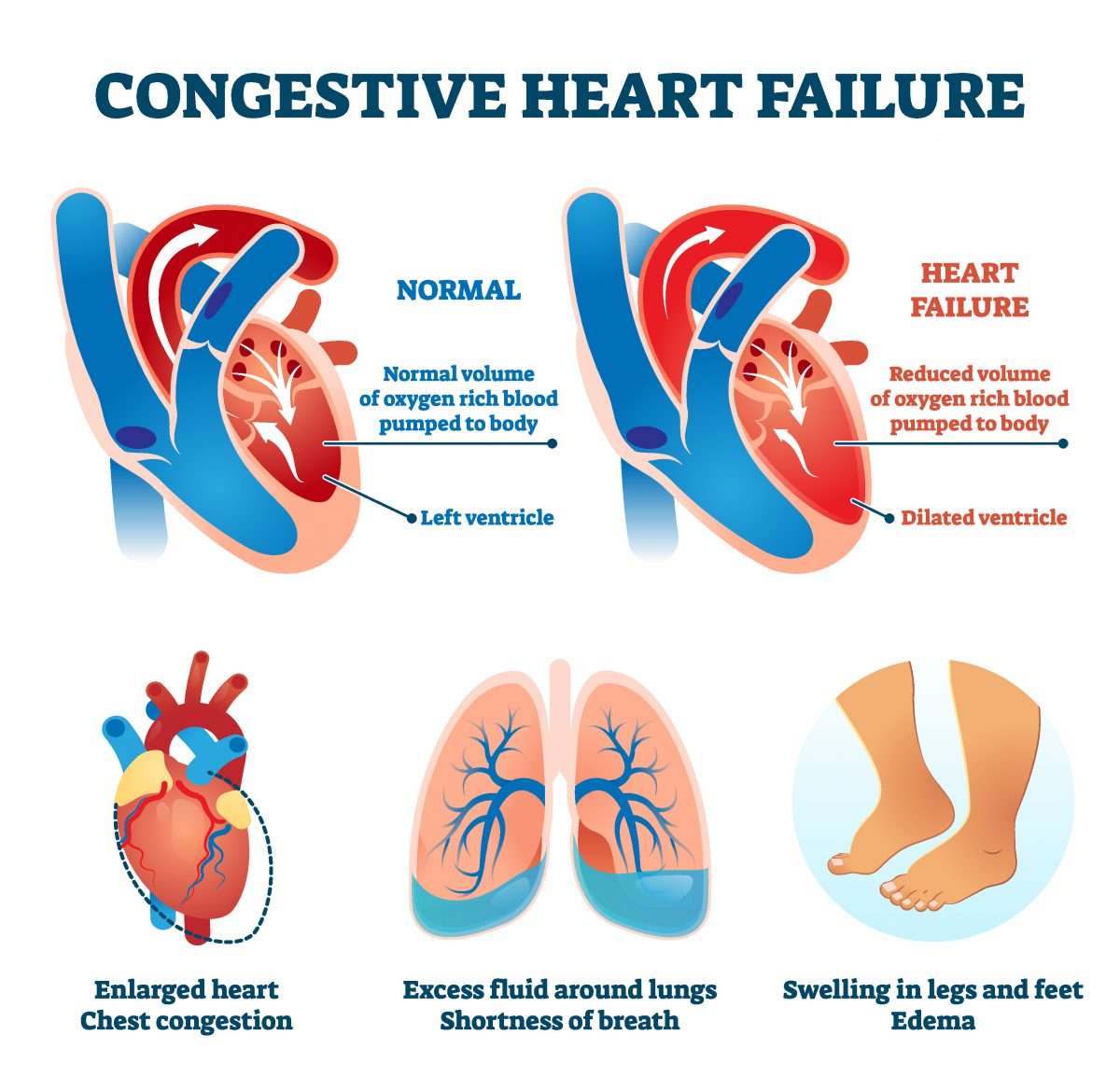
Congestive heart failure refers to a condition in which the heart is no longer able to pump blood sufficiently to meet all the bodys needs for oxygen. The inability of the heart to pump sufficiently ultimately causes fluid to leak from capillary blood vessels, causing many of the characteristic symptoms. Any disease that can weaken the heart can cause congestive heart failure. Some of the more common causes are:
Fluid buildup in the lungs is known as pulmonary edema, which leads to shortness of breath. Other associated symptoms include:
- problems sleeping when reclining.
What Is the Treatment for Congestive Heart Failure ?
The treatment for congestive heart failure is to some extent dependent upon the cause of the heart failure and usually involves a combination of different medications, which may include:
- Diuretics to control fluid buildup
- Medications to control blood pressure, including angiotensin converting inhibitors , beta-blockers, androgen receptor-2 blockers, or others
- Medication to strengthen the hearts activity such as digoxin
- Vericiguat , which a type of drug known as an oral soluble guanylate cyclase stimulator
- Nitrate medications to control chest pain
- Blood-thinning medications to prevent clots
Some people, depending on the cause of their CHF, may require:
- Surgery to repair or replace heart valves
- Coronary bypass surgery
- Insertion of a pacemaker, ventricular assist devices
- Heart transplantation
What Tests Might I Have To Diagnose Cardiomyopathy
If your healthcare provider suspects you have a heart condition, you will see a cardiologist . A cardiologist performs a full assessment that may include a range of diagnostic tests. You may have:
- Ambulatory monitoring uses devices that track your heart rhythm.
- Cardiac CT uses X-rays to make a video of your blood vessels and heart.
- Cardiac MRI uses radio waves and magnets to create images of your heart.
- Echocardiogram uses sound waves to create an image of your blood flow and heartbeat.
- Electrocardiogram records your hearts electrical activity.
- Exercise stress test raises your heart rate in a controlled way to see how your heart responds.
- Cardiac catheterization uses a catheter to measure your hearts blood flow and pressure.
- Myocardial biopsy studies a small sample of your heart muscle tissue to look for cell changes.
Advanced Heart & Vascular Institute In Boca Raton Fl
Congestive heart failure is one of many cardiac and blood vessel conditions our board-certified physicians treat. Dr. Eli Levine and Dr. Michael Schechter are board-certified interventional cardiologists who are Boca Ratons experts in preventing and treating congestive heart failure.
If you or your PCP suspect you have this serious heart condition, please contact our clinic for a diagnostic work-up and treatment plan. If you have CHF, we can help you manage it.
Please call us at 235-5621, or request your appointment online through our website. The sooner you contact us, the sooner you can begin a healthier life.
You May Like: What Does Resting Heart Rate Mean
How Is Cardiomyopathy Treated
Cardiomyopathy treatment focuses on controlling your symptoms. Treatment also slows the diseases progression. You will have regular checkups to keep an eye on your hearts health.
Your healthcare provider may recommend:
- Medications: Heart medications can improve your blood flow, control symptoms or treat underlying conditions. You may take blood thinners such as warfarin , beta blockers such as propranolol or medications to lower cholesterol.
- Devices to correct arrhythmias:Pacemakers or implantable cardioverter defibrillators treat irregular heart rhythms. These devices monitor your heartbeat. They send electrical impulses to your heart when an arrhythmia starts.
- Devices to improve blood flow: Some devices help your heart pump blood more efficiently. Cardiac resynchronization therapy devices control the contractions between the left and right sides of the heart. A left ventricular assist device helps your heart pump blood.
- Surgery: If you have severe symptoms or underlying heart conditions, your provider may recommend heart surgery. Providers usually only recommend open-heart surgery or a heart transplant when all other treatments have failed to bring relief.
Angiotensin Converting Enzyme Inhibitors
ACE inhibitors relax and widen your blood vessels. This helps to improve the flow of blood around your body, which reduces the amount of work your heart has to do.
ACE inhibitors have been shown to improve the symptoms of heart failure, reduce the need for hospital admission and improve life expectancy caused by heart failure.
Your symptoms should improve within a few weeks of starting treatment.
The main side effects of ACE inhibitors are dizziness and a cough. You will need to have regular blood tests, at least once every year, while taking an ACE inhibitor.
If you are taking an ACE inhibitor, you should check with your doctor or pharmacist before taking any other medicines. In particular, nonsteroidal anti-inflammatory medicines should not be taken with an ACE inhibitor. You should also avoid products containing high levels of potassium, such as salt substitutes.
Also Check: Open Heart Surgery Recovery Time
Monitor Your Health With Modern Heart And Vascular
Catching cardiac conditions in the earliest stages gives you the greatest chance of living a long and healthy life. At Modern Heart and Vascular, we provide advanced testing with state-of-the-art diagnostic tools. We focus on prevention to avoid unnecessary surgeries and procedures.
Our compassionate staff is dedicated to providing the highest quality patient care. Well answer all your questions and fully explain your treatment options, so you feel in control of your heart health.
We provide modern cardiovascular care for modern patients using modern technology. For more information about Modern Heart and Vascular Institute or to schedule an appointment, contact us today. If youd like to learn more about our practice, read our providers bios.
This article does not provide medical advice. It is intended for informational purposes only. It is not a substitute for professional medical advice, diagnosis or treatment. If you need cardiovascular care, please call us at 832-644-8930.
Shortness Of Breath While Lying Flat And With Exertion
Shortness of breath while lying flat. People who have left heart failure may experience shortness of breath when lying flat . The person will start using two or three pillows to prop themselves up while in bed so that they can breathe easier. If the shortness of breath is more severe, the person may begin sleeping in a chair or recliner.
Shortness of breath with exertion. Shortness of breath with exertion is referred to as dyspnea on exertion. Dyspnea on exertion occurs because the lungs cannot supply enough oxygen and the heart cannot adequately pump oxygen-rich blood to the body. Initially, the shortness of breath may occur when walking long distances or up flights of stairs, but as the heart failure progresses, less activity may produce more symptoms.
Read Also: What Does Heart Rate Mean
Don’t Miss: Average Exercise Heart Rate
A Persistent Dry Cough
Fluid accumulating in the lungs often triggers coughing that does not produce mucus. People with congestive heart failure tend to cough a lot. However, this is again a non-specific symptom since many things can trigger a dry cough, such as cold air, air pollution, allergies, asthma, a lingering respiratory infection, and lung cancer.
Does Heart Failure Show Up On Ecg
An electrocardiogram is often abnormal in patients with heart failure, although up to 10% of patients may have a normal ECG. Natriuretic peptides are a useful biomarker for heart failure and a negative result can rule out the diagnosis. This can be helpful in determining who should be referred for echocardiogram.
You May Like: How To Reverse Heart Disease
Factors That Can Worsen Symptoms Of Heart Failure
The symptoms of heart failure can be worsened by a number of factors, including:
- too much salt, fluid, or alcohol in the diet
- some viral and bacterial infections
- kidney diseases
Treatment for heart failure may include:
- medicines, such as
- diuretics to remove excess fluid and improve symptoms of heart failure
- mineralcortiocoid receptor antagonists are also recommended and used in most patients with heart failure to reduce mortality and hospitalisation
- ACE inhibitors to open up blood vessels, reduce blood pressure and reduce sodium retention and water retention
- certain beta-blockers to slow the heart rate and reduce its work
- aldosterone blockers to reduce blood pressure and reduce the effects of damage to the heart muscle
- ACE inhibitors, beta blockers and aldosterone blockers can increase survival and reduce the likelihood of hospitalisation.
How Is Congestive Heart Failure Diagnosed
Early symptoms of congestive heart failure are often mistaken by patients for other medical problems. Physicians diagnose congestive heart failure with the aid of images and other tests. These include chest x rays, electrocardiogram, blood tests, echocardiogram, stress tests, MRIs, and cardiac catheterization.
Don’t Miss: What Time Of Day Are Heart Attacks Most Common
Symptoms Of Heart Failure
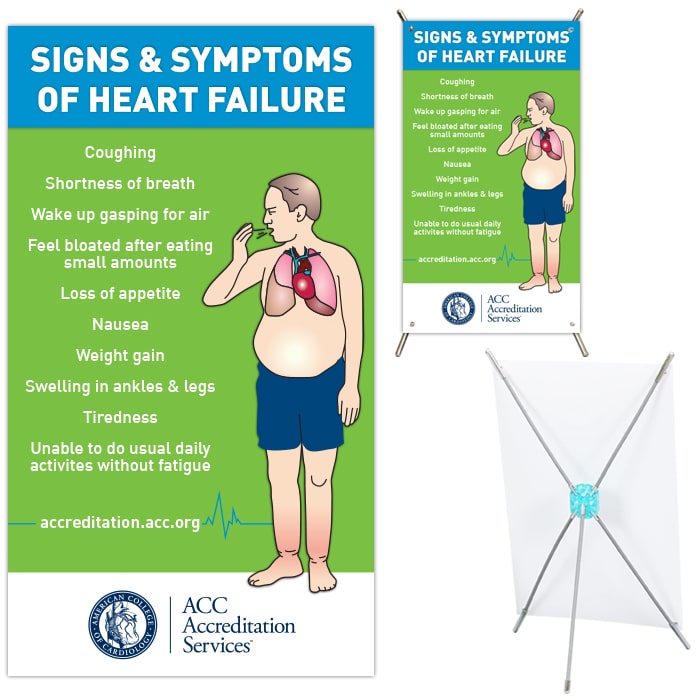
The main symptoms of heart failure are:
- breathlessness after activity or at rest
- feeling tired most of the time and finding exercise exhausting
- feeling lightheaded or fainting
- swollen ankles and legs
Some people also experience other symptoms, such as a persistent cough, a fast heart rate and dizziness.
Symptoms can develop quickly or gradually over weeks or months .
Types Of Heart Failure
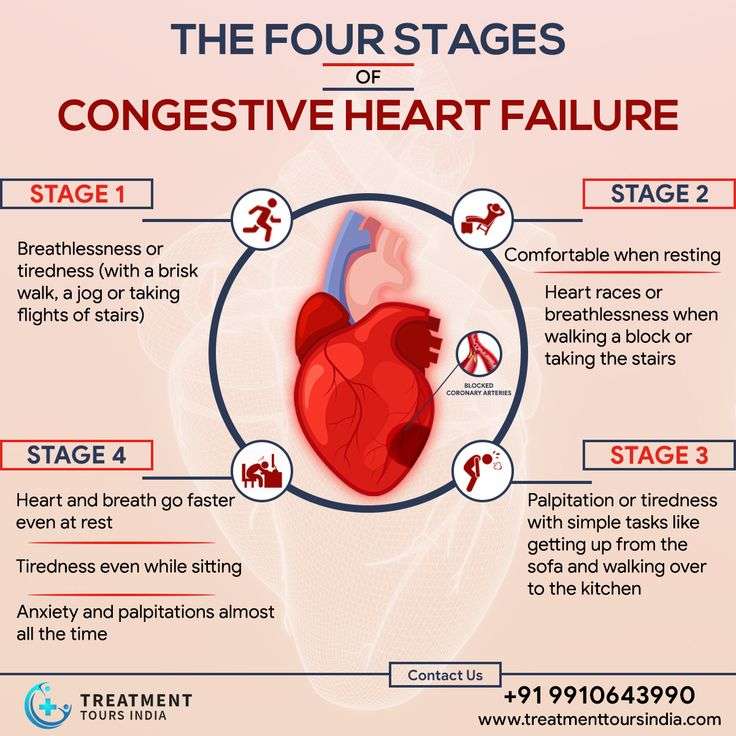
The main types of heart failure are named for where they occur in the heart:
- Left-sided heart failure
- Biventricular heart failure
Clinicians also may classify heart failure as:
- Acute: You have active symptoms of heart failure, with either a new diagnosis or with long-term heart failure.
- Chronic: You have a history of heart failure, but your condition is relatively stable with no symptoms or with manageable symptoms.
Read Also: How To Calculate Heart Rate Zones
Can Surgery Be Used To Treat Heart Failure
In heart failure, surgery may sometimes prevent further damage to the heart and improve the heart’s function. Procedures used include:
- Coronary artery bypass grafting surgery. The most common surgery for heart failure caused by coronary artery disease is . Although surgery is more risky for people with heart failure, new strategies before, during, and after surgery have reduced the risks and improved outcomes.
- Heart valve surgery. Diseased heart valves can be treated both surgically and non-surgically .
- Implantable left ventricular assist device . The LVAD is known as the “bridge to transplantation” for patients who haven’t responded to other treatments and are hospitalized with severe systolic heart failure. This device helps your heart pump blood throughout your body. It allows you to be mobile, sometimes returning home to await a heart transplant. It may also be used as destination therapy for long-term support in patients who are not eligible for transplant.
- Heart transplant. A heart transplant is considered when heart failure is so severe that it doesn’t respond to all other therapies, but the person’s health is otherwise good.
European Society Of Cardiology’s Guidelines For Diagnosis Of Heart Failure
Essential features
- ArrhythmiasAtrial fibrillation ventricular arrhythmias bradyarrhythmias
- ThromboembolismStroke peripheral embolism deep venous thrombosis pulmonary embolism
- GastrointestinalHepatic congestion and hepatic dysfunction malabsorption
- MusculoskeletalMuscle wasting
- RespiratoryPulmonary congestion respiratory muscle weakness pulmonary hypertension
Recent observational data from the studies of left ventricular dysfunction and vasodilator heart failure trials indicate that mild to moderate heart failure is associated with an annual risk of stroke of about 1.5% , rising to 4% in patients with severe heart failure. In addition, the survival and ventricular enlargement study recently reported an inverse relation between risk of stroke and left ventricular ejection fraction, with an 18% increase in risk for every 5% reduction in left ventricular ejection fraction this clearly relates thromboembolism to severe cardiac impairment and the severity of heart failure. As thromboembolic risk seems to be related to left atrial and left ventricular dilatation, echocardiography may have some role in the risk stratification of thromboembolism in patients with chronic heart failure.
Don’t Miss: Which Chamber Of The Heart Pumps Blood To The Lungs
A Bluish Tint To The Skin
As congestive heart failure worsens, the poor circulation and fluid accumulation in the lungs can make it difficult for the body to provide sufficient oxygen to the tissues. This symptom can cause the skin to appear pale or even mildly blue since well-oxygenated blood is bright red while poorly oxygenated blood is blue.
Nitrates Apresoline Beta Blockers And Inotropes Drugs For Congestive Heart Failure
Nitrates are venous vasodilators that include isosorbide mononitrate and isosorbide dinitrate . They are commonly used in combination with an arterial vasodilator, such as hydralazine .
- Nitroglycerin is a nitrate preparation that is administered to treat acute chest pain, or angina.
Hydralazine is a smooth muscle arterial vasodilator that may be used for congestive heart failure. Clinical trial data has shown hydralazine plus nitrates to be especially effective in African-Americans with heart failure, when used in addition to ACE inhibitors or ARBs.
- Isosorbide dinitrate and hydralazine is a fixed dose combination of isosorbide dinitrate and hydralazine . This drug is indicated for heart failure in African-Americans based in part on results of the African American Heart Failure Trial .
- Hydralazine is also especially valuable in patients who have poor kidney function and/or are intolerant to ACE inhibitors and ARBs.
Beta-blockers: These drugs slow down the heart rate, lower blood pressure, and have a direct effect on the heart muscle to lessen the workload of the heart. Specific beta-blockers, such as carvedilol and long-acting metoprolol , have been shown to decrease symptoms, hospitalization due to congestive heart failure, and deaths. Other beta-blockers include bispropolol , atenolol , propranolol , and , but they are generally not used with significant congestive heart failure.
Getting the most out of congestive heart failure medications involves the following:
Read Also: What Is My Target Heart Rate
How Is Congestive Heart Failure Treated
To treat CHF, doctors give medicines to:
- help the heart beat stronger
- help the heart beat at the right rate
- reduce the amount of fluid in the body
- lower the blood pressure so the heart doesnt have to work so hard to push blood out of the heart into the blood vessels
Some kids might need a pacemaker to help their heart beat at the right rate. Doctors do surgery to place this small device under the childs skin and muscle. It uses electrical impulses to control the speed and rhythm of the heartbeat.
If heart failure keeps getting worse, doctors can use one of these until the child gets better:
- a ventricular assist device to take over the work of the heart
- extracorporeal membrane oxygenator to take over the work of the heart and lungs
Sometimes, treating the cause of the CHF cures the heart failure. Very rarely, a heart transplant is needed.
What Causes Congestive Heart Failure
Congestive heart failure is not a disease itself, but a syndrome that can have many different causes. The heart itself becomes weak due to other heart problems or problems with the blood vessels.
Common causes of heart failure include cardiomyopathy, damaged heart valves, coronary artery blockage, previous or impending heart attacks, environmental exposures like alcohol and cocaine, infections, hypertension, congenital heart disease, and arrhythmias.
According to St. Judes Medical, about half of all cases of congestive heart failure are caused by underlying coronary artery disease. In addition to more common causes of heart failure, there are hundreds of less common causes. In many cases, the exact cause of congestive heart failure is unknown.
Certain lifestyle choices are associated with a worsening of congestive heart failure. Smoking tobacco products and drinking alcohol excessively can exacerbate heart failure. Morbid obesity and a sedentary lifestyle can contribute to heart failure. A diet high in salt can make fluid retention worse for patients.
Recommended Reading: What Type Of Pain In Arm Heart Attack
What Clinical Signs Should I Expect
The most common clinical sign of congestive heart failure is persistent coughing accompanied by difficulty breathing. This is due mainly to pulmonary edema or the accumulation of fluid in the lungs. The enlarged heart will also push against the trachea, causing irritation that can induce a cough.
“The most common clinical sign of congestive heart failure is persistent coughing accompanied by difficulty breathing.”
Many dogs with CHF will tire out more easily, have reduced stamina, and do not engage in playing or walking as they once did. Coughing when at rest or sleeping, excessive panting, persistent loss of appetite, a swollen belly, and pale or bluish gums are also signs associated with heart failure. The dog will develop generalized weight loss and muscle wasting due to the effects of CHF on other body systems. If any of these signs develop in a pet with a heart murmur, notify your veterinarian immediately.
How Can I Take Care Of Myself With Cardiomyopathy
Lifestyle choices can affect how quickly cardiomyopathy progresses. To manage symptoms and increase your heart health, your provider may recommend:
- Achieving and maintaining an ideal weight for your height and age.
- Eating a heart-healthy diet, including reducing your sodium intake.
- Managing underlying conditions such as sleep apnea or diabetes.
- Scheduling regular checkups with a healthcare provider.
- Taking all medications as prescribed.
Read Also: Congestive Heart Failure Fluid In Lungs
Tips For Managing Congestive Heart Failure End
You may be asking, How can I provide comfort to my loved one as they experience the end-of-life signs of congestive heart failure? Its only natural that you as a loved one and/or caregiver will want to be as helpful as possible, and ensure that your loved one is experiencing as little pain as possible. Heres some ways you can help:
- Communicate with the doctors and healthcare professionals: Your loved one may be too weak, or simply forget, to communicate their symptoms to the doctors and nurses. You can help by sharing this information with them in order to make sure your loved one gets what they need.
- Provide comfort: Sometimes it is just as simple as spending time with your loved one while watching a TV show, or talking about things they love. These conversations can help in alleviating some of their depression and anxiety.
- Help them remember to take their medicine: There will likely be various pills and medications that your loved one needs to take. You can help by assisting your loved one in staying on schedule.
