The New York Heart Association Classifies The Stages Of Heart Failure As Follows: 2
No limitation of physical activity. Ordinary physical activity does not cause undue fatigue, palpitation, dyspnea .
Slight limitation of physical activity. Comfortable at rest. Ordinary physical activity results in fatigue, palpitation, dyspnea .
Unable to carry on any physical activity without discomfort. Symptoms of heart failure at rest. If any physical activity is undertaken, discomfort increases.
European Society Of Cardiology Guidelines For Genetic Counseling And Testing
Arrhythmogenic cardiomyopathy
Offer genetic counseling and testing all patients with suspected ACM and all first-degree adult relatives of patients with ACM and a disease-causing mutation, regardless of their phenotype to preclinically identify genetically affected individuals.
Genetic family screening may also be used for arrhythmic risk stratification.
First-degree relatives with the same definite disease-causing mutation as the patient should undergo clinical evaluation, electrocardiography , echocardiography, and possibly cardiac magnetic resonance imaging . In the setting of no definite identified genetic mutation in the patient or no genetic testing is undertaken, consider clinical evaluation in first-degree adult relatives with ECG and echocardiography, and repeat every 2-5 years or less if nondiagnostic abnormalities are present.
Dilated cardiomyopathy or hypokinetic nondilated cardiomyopathy
All patients with suspected DCM or HNDC and all first-degree adult relatives of such patients and a definite disease-causing mutation, regardless of their phenotype, should undergo genetic counseling and testing to preclinically identify genetically affected individuals. Repeat the evaluation every 5 years or less in first-degree adult relatives when aged younger than 50 years or in the presence of nondiagnostic abnormalities.
All first-degree relatives of patients should undergo clinical evaluation, ECG, echocardiography, and possibly CMRI.
Hypertrophic cardiomyopathy
Relationships With Industry And Other Entities
The ACC and AHA have rigorous policies and methods to ensure that documents are developed without bias or improper influence. The complete policy on relationships with industry and other entities can be found online. of the guideline lists writing committee members relevant RWI for the purposes of full transparency, their comprehensive disclosure information is available in a . Comprehensive disclosure information for the Joint Committee is also available online.
Recommended Reading: How To Fix Congestive Heart Failure
What Are The Stages Of Heart Failure
- print page
- Bookmark for later
Heart failure can be a misunderstood diagnosis. It describes a heart that is not pumping blood as well as it should, but it doesnt mean the heart has “failed” or stopped working.1 There are different types of heart failure and different classifications used by healthcare providers to assess the stage and functional status of a person with HF.
American College Of Cardiology/american Heart Association/heart Failure Society Of America Recommendations For Genetic Evaluation And Testing
Genetic screening and counseling are recommended for first-degree relatives of selected individuals with genetic or inherited cardiomyopathies to detect cardiac disease and to encourage review of therapies for lowering HF progression and sudden death.
It is reasonable to refer select patients with nonischemic cardiomyopathy for genetic counseling and testing to identify conditions that could guide treatments for patients and family member.
Don’t Miss: Which Arm Pain Is Sign Of Heart Attack
New York Heart Association Functional Classification
The New York Heart Association Functional Classification system focuses on categorizing people with heart failure based on their doctor’s objective assessment of the impact the condition has on their day-to-day activities:
- Class I: There is no objective evidence of cardiovascular disease, and there are no symptoms or limitations with ordinary physical activity.
- Class II: There is slight objective evidence of cardiovascular disease, you are comfortable at rest, and moderate physical activity induces mild symptoms of heart failure.
- Class III: There is objective evidence of moderately severe cardiovascular disease, and you are only comfortable at rest. Even less than normal physical activity results in limitations due to heart failure symptoms.
- Class IV: There is objective evidence of severe cardiovascular disease, and you have symptoms of heart failure even at rest. There are severe limitations with physical activity due to the severity of your heart failure symptoms.
Esc Clinical Practice Guidelines
The aim of this ESC guideline is to help health professionals manage people with heart failure according to the best available evidence. Fortunately, we now have a wealth of clinical trials to help us select the best management to improve the outcomes for people with HF for many, it is now both preventable and treatable. This guideline provides practical, evidence-based recommendations. The format of the previous 2016 ESC HF Guidelines was revised to make each phenotype of HF stand-alone in terms of its diagnosis and management. The therapy recommendations mention the treatment effect supported by the class and level of evidence and are presented in tables. In this guideline, we have decided to focus on the diagnosis and treatment of HF, not on its prevention.
Guidelines and related materials are for use by individuals for personal or educational purposes. No commercial use is allowed. Re-use permission must be correctly obtained .
Don’t Miss: Rapid Heart Rate While Sleeping
Evaluation With Cardiac Imaging
Recommendations for Evaluation With Cardiac Imaging
Referenced studies that support the recommendations are summarized in the .
| COR | |
|---|---|
| C-LD | |
| 1. |
In patients with suspected or new-onset HF, or those presenting with acute decompensated HF, a chest x-ray should be performed to assess heart size and pulmonary congestion and to detect alternative cardiac, pulmonary, and other diseases that may cause or contribute to the patients symptoms . |
1C-LD
| 2. |
In patients with suspected or newly diagnosed HF, transthoracic echocardiography should be performed during initial evaluation to assess cardiac structure and function . |
1C-LD
| 3. |
In patients with HF who have had a significant clinical change, or who have received GDMT and are being considered for invasive procedures or device therapy, repeat measurement of EF, degree of structural remodeling, and valvular function are useful to inform therapeutic interventions . |
1C-LD
| 4. |
In patients for whom echocardiography is inadequate, alternative imaging is recommended for assessment of LVEF . |
2aB-NR
| B-NR | |
| 1. |
In ambulatory or hospitalized patients with HF, validated multivariable risk scores can be useful to estimate subsequent risk of mortality . |
Synopsis
Table 8 Selected Multivariable Risk Scores to Predict Outcome in HF
| Risk Score |
|---|
| 2010 |
Recommendation-Specific Supportive Text
| 1. |
High Output Versus Low Output Heart Failure
- Low Output Failure: The cardiac output is reduced, and the systemic vascular resistance is high. In low output failure, there is an inadequate supply of blood flow to meet normal metabolic demands.
- High Output Failure: The cardiac output is increased, and the systemic vascular resistance is low. Rather than an inadequate supply of blood flow to meet normal metabolic demands as occurs in low output failure, in high output failure there is an excess requirement for oxygen and nutrients and the demand outstrips what the heart can provide. Causes of high output heart failure include severe anemia, Gram negative , beriberi , thyrotoxicosis, Paget’s disease, arteriovenous fistulae, or arteriovenous malformations.
Don’t Miss: How To Measure Resting Heart Rate
Ology And Evidence Review
The recommendations listed in this guideline are, whenever possible, evidence based. An initial extensive evidence review, which included literature derived from research involving human subjects, published in English, and indexed in MEDLINE , EMBASE, the Cochrane Collaboration, the Agency for Healthcare Research and Quality, and other selected databases relevant to this guideline, was conducted from May 2020 to December 2020. Key search words included but were not limited to the following: heart failure heart failure with reduced ejection fraction heart failure with preserved ejection fraction heart failure with mildly reduced ejection fraction systolic heart failure heart failure rehabilitation cardiac failure chronic heart failure acute decompensated heart failure cardiogenic shock beta blockers mineralocorticoid receptor antagonists ACE-inhibitors, angiotensin and neprilysin receptor antagonist sacubitril valsartan angiotensin receptor antagonist Sodium glucose co-transporter 2 or SGLT2 inhibitors cardiac amyloidosis atrial fibrillation congestive heart failure guideline-directed medical therapy HFrEF diabetes mellitus cardiomyopathy cardiac amyloidosis valvular heart disease mitral regurgitation cardiomyopathy in pregnancy reduced ejection fraction right heart pressure palliative care.
American College Of Cardiology/american Heart Association Classification
The American College of Cardiology/American Heart Association classification of heart failure stages focus more on the condition’s structural impact on the heart, such as the measurement of ejection fraction:
- Stage A: You do not have any structural disorder of the heart, but are at high risk for developing congestive heart failure due to a family history of heart failure or a personal history of hypertension, diabetes, coronary artery disease, alcohol abuse, viral infections, or use of drugs that are toxic to the heart.
- Stage B: You have a structural disorder of the heart, but no symptoms of heart failure .
- Stage C: You have a structural disorder of the heart and you have currently or previously displayed symptoms of heart failure.
- Stage D: People in this final stage of heart failure do not get better with treatment.
Recommended Reading: How To Tell If You Had A Heart Attack
Acc/aha Joint Committee Members
Joshua A. Beckman, MD, MS, FAHA, FACC, Chair
Patrick T. OGara, MD, MACC, FAHA,Immediate Past Chair
Sana M. Al-Khatib, MD, MHS, FACC, FAHA
Anastasia L. Armbruster, PharmD, FACC
Kim K. Birtcher, PharmD, MS, AACC
Joaquin E. Cigarroa, MD, FACC
Lisa de las Fuentes, MD, MS, FAHA
Anita Deswal, MD, MPH, FACC, FAHA
Dave L. Dixon, PharmD, FACC
Lee A. Fleisher, MD, FACC, FAHA
Federico Gentile, MD, FACC
Zachary D. Goldberger, MD, FACC, FAHA
Bulent Gorenek, MD, FACC
Adrian F. Hernandez, MD, MHS
Mark A. Hlatky, MD, FACC, FAHA
José A. Joglar, MD, FACC, FAHA
W. Schuyler Jones, MD, FACC
Joseph E. Marine, MD, FACC
Daniel B. Mark, MD, MPH, FACC, FAHA
Debabrata Mukherjee, MD, FACC, FAHA
Latha P. Palaniappan, MD, MS, FACC, FAHA
Tanveer Rab, MD, FACC
Erica S. Spatz, MD, MS, FACC
Jacqueline E. Tamis-Holland, MD, FAHA, FACC
Duminda N. Wijeysundera, MD, PhD
Y. Joseph Woo, MD, FACC, FAHA
Former Joint Committee member current member during the writing effort.
Acute And Chronic Heart Failure

People with acute heart failure have no previous signs and symptoms of heart failure. AHF can present with rapid swelling and fluid retention characterized by sudden weight gain. Coughing, wheezing, and shortness of breath, as well as an irregular heartbeat, could be symptoms of acute heart failure. In some cases, it is related to pre-existing cardiomyopathy.6-7 AHF often requires unexpected hospital admission. It can also be associated with a poor prognosis and a high risk of readmission and death post-discharge.8 Treatment options include medication, surgery, and implanted medical devices, as well as recommended lifestyle modifications.
Chronic heart failure describes the heartâs inability to pump enough blood through the body and provide a sufficient supply of oxygen. This is caused by a weaker than a normal heart. CHF is most common in men and risk factors include age, high blood pressure, being overweight and the presence of metabolic disorders like diabetes. CHF is as its name describes – it is a long-term condition that can get worse over time. It generally cannot be cured but it can be medically managed.7
Don’t Miss: When Should I Worry About My Heart Rate
Stages Of Heart Failure
The stages classified by the AHA and ACC are different than the New York Heart Association clinical classifications of heart failure that rank patients as class I-II-III-IV, according to the degree of symptoms or functional limits. Ask your doctor what stage of heart failure you are in.
Stage A
Presence of heart failure risk factors but no heart disease and no symptoms
Stage B
Heart disease is present but there are no symptoms
Stage C
Structural heart disease is present AND symptoms have occurred
Stage D
Presence of advanced heart disease with continued heart failuresymptoms requiring aggressive medical therapy
Acc/aha Heart Failure Staging
- Patients with known heart failure.
- Patients at risk for heart failure.
- Developed jointly by the American College of Cardiology and American Heart Association to complement, but not replace, the more widely-used New York Heart Association functional classification.
- Based on expert consensus.
- Matches stage to treatment options, unlike other classification systems.
- Other heart failure classification systems include Forrester Class and NYHA Class.
- Unlike other classification systems, the ACC/AHA stages include patients at risk for heart failure and corresponding management options.
You May Like: Fat Burning Heart Rate Chart
Heart Rhythm Society And The European Heart Rhythm Association Select Recommendations For Genetic Testing For Channelopathies And Cardiomyopathies
Long QT syndrome
Comprehensive or LQT1-3 targeted LQTS genetic testing is recommended for the following:
- Individuals with a strong clinical index of suspicion for LQTS based on the patient’s clinical history, family history, and expressed electrocardiographic phenotype
- Asymptomatic individuals with idiopathic QT prolongation on serial 12-lead ECGs defined as QTc over 480 ms or longer than 500 ms may also be considered in asymptomatic individuals with idiopathic QT prolongation on serial 12-lead ECGs for QTc values over 460 ms or longer than 480 ms
Mutation-specific genetic testing is recommended for family members following identification of the LQTS mutation in an index case.
Catecholaminergic polymorphic ventricular tachycardia
- Comprehensive or CPVT1 and CVPT2 targeted CPVT genetic testing is recommended for any individual with a clinical index of suspicion for CPVT based on the patient’s clinical history, family history, and expressed ECG phenotype during provocative stress testing with cycle, treadmill, or catecholamine infusion.
- Mutation-specific genetic testing is recommended for family members following identification of the CPVT mutation in an index case.
Brugada syndrome
Cardiac conduction disease
Short QT syndrome
ACM / arrhythmogenic right ventricular cardiomyopathy
Left ventricular noncompaction
Restrictive cardiomyopathy
Document Review And Approval
This document was reviewed by 2 official reviewers nominated by the AHA 1 official reviewer nominated by the ACC 2 official reviewers from the HFSA 1 official Joint Committee on Clinical Practice Guidelines reviewer and 32 individual content reviewers. Reviewers RWI information was distributed to the writing committee and is published in this document .
This document was approved for publication by the governing bodies of the ACC, AHA, and HFSA.
Don’t Miss: Can Ecg Tell Heart Attack
Heart Failure Symptoms By Class And Stage
- print page
- Bookmark for later
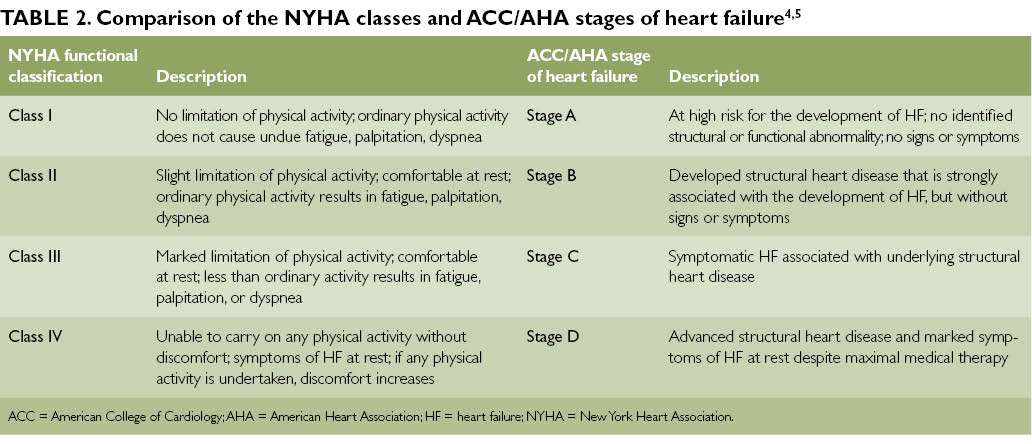
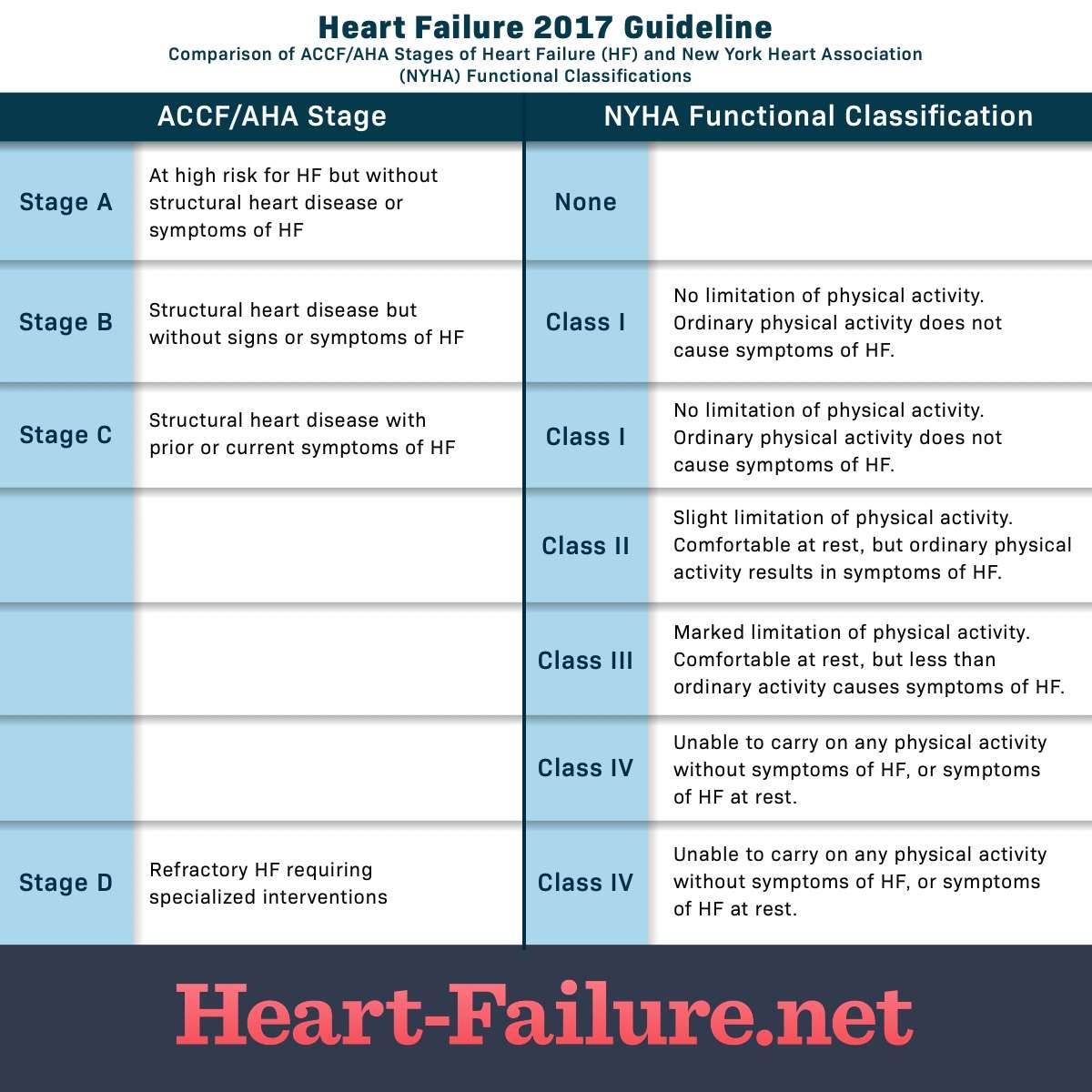
Heart failure is a complex, chronic syndrome that gets worse over time. During the diagnostic process, physicians classify each case of heart failure. The American College of Cardiology/American Heart Association and the New York Heart Association have complementary classification systems.1-4
The ACC/AHA stages reflect the range from a high risk of developing heart failure to advanced heart failure and are associated with an approach to treatment plans.1-4 The New York Heart Association clinical classifications of heart failure reflect the severity of symptoms or functional limits due to heart failure.1-2 A diagnosis can have an assignment of a stage and a class.
Figure 1 Heart Failure Stages And Classes
The stages above describe the range from a high risk of developing heart failure on through advanced heart failure. The stages are correlated to treatment plans. The stages are also progressive, as HF worsens, you advance to the next stage of heart failure. There is no reversal through the stages. The objective is that with treatment, progression through the stages may be delayed.4
Also Check: Congestive Heart Failure Pulmonary Edema
What Is Heart Failure
The heart’s pumping ability is measured by the ejection fraction. Using percentages, the ejection fraction is a measure of the amount of blood pumped out of the heart with each heartbeat. A normal ejection fraction is 50% to 70%.
Heart failure occurs when the heart cannot pump enough blood to meet the body’s needs. Essentially, the demands of the body exceed the heart’s pumping ability. The heart then attempts to meet the body’s needs by developing several compensatory mechanisms:
- Stretching or enlarging: Stretching allows the heart to fill with more blood, which it can then pump to meet the body’s demands. Eventually, the heart struggles to maintain the larger size, and its ability to pump blood declines.
- Developing more muscle mass: Initially, this allows the heart to pump more blood. But, over time, the heart cannot sustain the increase in muscle mass, and its ability to pump blood lessens.
- Pumping faster: Increasing your heart rate lets the heart pump more blood, at least initially. Over time, the heart cannot keep up with the higher pace and eventually pumps more slowly.
As the heart’s compensatory mechanisms begin to fail, the ejection fraction may begin to drop. An ejection fraction of 40% or less indicates heart failure with a reduced ejection fraction.
Universal Definition And Classification Of Heart Failure: A Step In The Right Direction From Failure To Function

- A
Quick Takes
- The proposed universal definition describes HF as a clinical syndrome with symptoms and/or signs caused by a structural and/or functional cardiac abnormality and corroborated by elevated natriuretic peptide levels and/or objective evidence of pulmonary or systemic congestion.
- HF stages have been revised to emphasize symptomatic nature of HF as a clinical syndrome: At risk for HF , PreHF , Symptomatic HF and Advanced HF .
- Classification of HF according to LVEF now includes:
- HFrEF: symptomatic HF with LVEF 40%
- HFmrEF: symptomatic HF with LVEF 41-49%
- HFpEF: symptomatic HF with LVEF 50%
- HFimpEF: symptomatic HF with a baseline LVEF 40%, a 10-point increase from baseline LVEF, and a second measurement of LVEF > 40%
A revised classification of HF by left ventricular ejection fraction was also proposed and is as follows:
Figure 1. Courtesy of Gibson GT, Blumer V, Mentz RJ, Lala A.
Figure 1
The new Universal Definition and Classification of HF represents a landmark advancement in our field. The standardization of the definition of HF is valuable for several reasons:
References
Don’t Miss: How To Raise Your Heart Rate
