Types Of Heart Failure
Centers for Disease Control and Prevention estimates that heart failure affects 6.2 million adults in the United States. Its most common in people 65 years old and over.
If you have heart failure, your heart cant pump enough blood to other tissues and organs in your body, or it requires higher pressure to pump the blood.
Your outlook and recommended treatment plan depend on the underlying cause of your heart failure as well as the severity of your condition.
Take a moment to learn about the different types of heart failure and how they may affect you.
Systolic And Diastolic Heart Failure Defined
Both sides of the heart are prone to dysfunction, but heart failure on the left side is more common.
- Systolic heart failure occurs when the left side of the heart becomes too weak to squeeze normal amounts of blood out of the heart when it pumps.
- Diastolic heart failure occurs when the left side of the heart is too stiff to relax and fill normally with blood.
The most common culprits of left-sided heart failure are:
Pathophysiology Of Impaired Diastolic Relaxation
To start with, hereâs a reminder of what a normal LV pressure-volume loop looks like. The shape of this loop is governed by the end-systolic and the diastolic pressure-volume relationships on the bottom, the diastolic pressure-volume relationship and on the top the end-systolic pressure volume relationship.
Now, the term âelastanceâ will be used here because elastance is the change in pressure per change in volume, whereas compliance is a change in volume per change in pressure. The flimsy rationale for using this term is as follows.
- In diastole, the preload volume is what distends the ventricle.
- The ventricle experiences an increase in pressure as the result of this distension
- The mechanical property of the ventricle which changes this pressure/volume relationship is described by the resistance to deformation or the tendency to spring back to original dimensions in response to distension.
- For this property, the closest mechanical terminology is âelastanceâ
- Conversely, compliance is the change in volume per change in unit pressure, and it would make no logical sense to discuss the ventricle in those terms because the change in volume is the initiating factor.
Anyway. Hereâs what an LV pressure-volume loop looks like when the diastolic relaxation is impaired. The shape of the curve is borrowed from a paper by Zile et al they took real measurements from patients with varying degrees of diastolic dysfunction.
Now, let us see what happens when we increase preload.
Don’t Miss: What Are The Types Of Heart Attacks
What Is The Outlook For Diastolic Heart Failure
As long as you follow your doctors instructions, diastolic heart failure have a significant impact on your everyday life.
You can greatly improve your response to treatment by caring for yourself in the following ways:
- tracking your symptoms
- taking any prescribed medications
To achieve the best outlook possible, seek medical attention as soon as symptoms appear. This ensures you have the best chance possible at maintaining a good quality of life.
Articles On Heart Failure Types & Stages
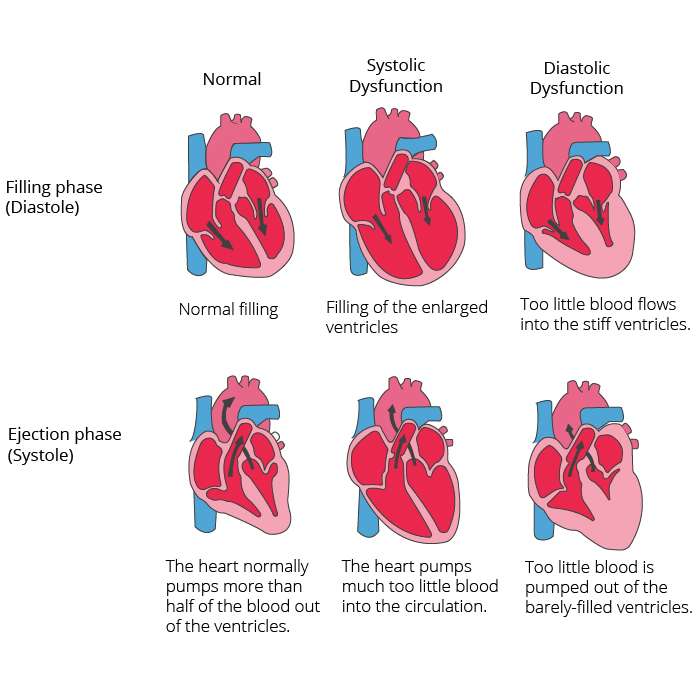
If you have diastolic heart failure, your left ventricle has become stiffer than normal. Because of that, your heart can’t relax the way it should. When it pumps, it can’t fill up with blood as it’s supposed to. Because there’s less blood in the ventricle, less blood is pumped out to your body.
Recommended Reading: How To Calm Heart Rate
Systolic Heart Failure Treatment
A persons medical care team may treat systolic heart failure with various medications, including:
- diuretics, which help reduce fluid buildup in the body
- angiotensin converting enzyme inhibitors, which help lower blood pressure and reduce strain on the heart
- beta-blockers, to reduce the heart rate and blood pressure
- mineralocorticoid receptor antagonists , to lower blood pressure
- angiotensin receptor blockers , which doctors can prescribe if a person cannot tolerate ACE inhibitors
- angiotensin receptor-neprilysin inhibitors , a combination medication that doctors use to lower blood pressure and reduce fluid buildup
- SGLT2 inhibitors, which are a treatment for diabetes but also improve outcomes in people with heart failure
- ivabradine , to reduce the heart rate
- digoxin , which lowers the heart rate and strengthens heart contractions
- vasodilators, to lower blood pressure
Systolic heart failure may require a person to take a combination of medications.
Research from 2016 found that taking a combination of ACE inhibitors and beta-blockers can reduce a persons risk of death due to heart failure by .
The same research also found that taking a combination of medications could reduce the risk of hospitalization for a person with HFrEF by 64%.
What Are The Risk Factors For Diastolic Heart Failure
There are particular factors that are known to increase the risk of experiencing diastolic heart failure, :
- A preexisting heart condition such as congenital heart disease: If you were born with valves or chambers in your heart that did not form correctly, the rest of the heart may have to work harder to pump blood. This can lead to stiffening of the muscle causing diastolic heart failure.
- High blood pressure: The extra pressure in your blood vessels means the heart muscle has to work even harder to move the blood out of the heart. As a result, the heart muscle gets thicker, eventually getting stiffer and increasing your risk of diastolic heart failure.
- Diabetes: Long-term health conditions, such as diabetes, can increase your blood pressure or cause microscopic scarring, meaning the heart can get stiffer.
- : Drinking and smoking can increase the risk of heart failure.
- Sleep apnea: Disruption to your breathing during sleep can result in decreased oxygen levels and often an irregular heartbeat. Together, these can stiffen the heart muscle.
- Obesity: Obesity can increase your risk of developing diastolic heart failure.
- Physical inactivity: This can reduce the health of the heart muscle.
Don’t Miss: Heart Transplant Surgery Time
Measurement Of Diastolic Dysfunction
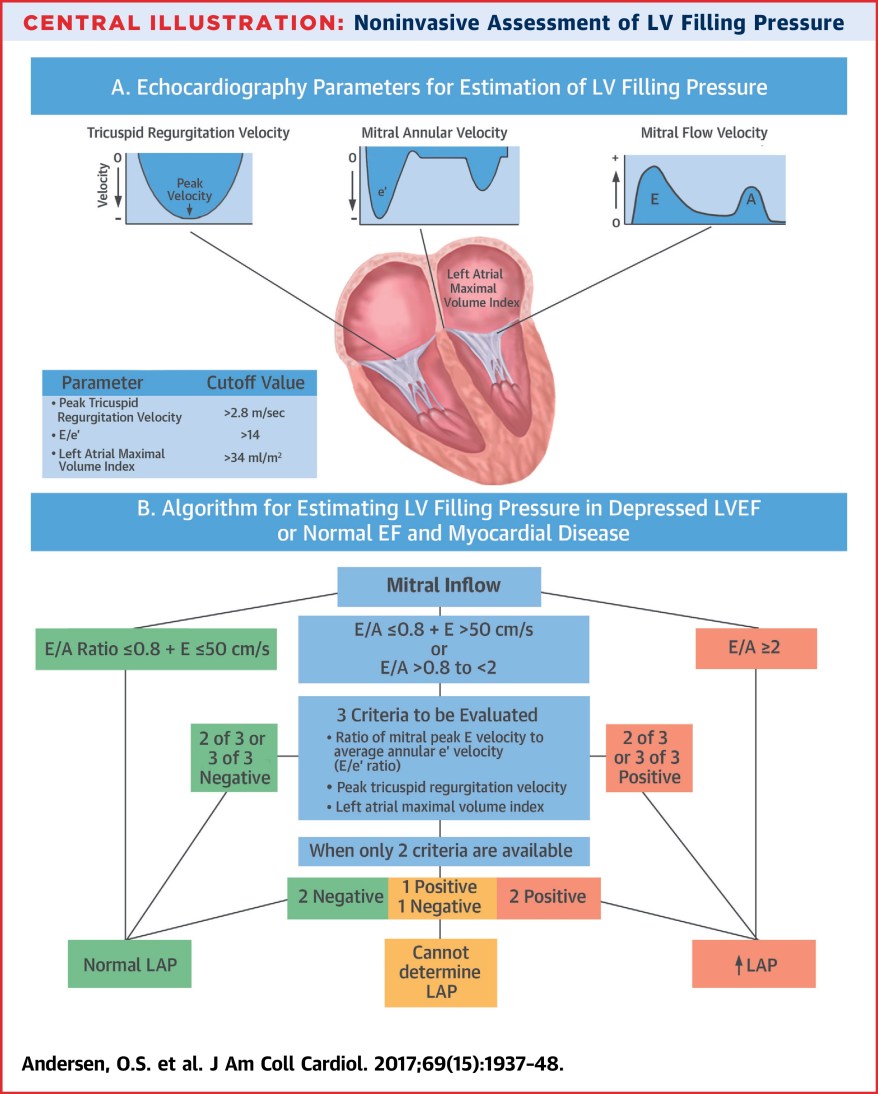
The gold standard for measuring diastolic dysfunction is echosonography. In case one ever requires an official document, the criteria for measurement are described by the ASE/EACI . At risk of trivialising the mighty art of critical care ultrasonography, an oversimplification suitable for the time-poor exam candidate would be to say that diastolic function is measured with the use of the mitral inflow E/A ratio.
The E/A ratio is measured by measuring a pulse wave Doppler across the mitral valve in an apical 4-chamber view:
That gives you a waveform with two characteristic peaks pointing towards the probe , termed E and A waves.
The E wave is the early diastolic filling wave, which describes left atrial filling pressure. This is the blood flow early in diastole, which occurs immediately after the mitral valve opens following isovolumetric relaxation.
The E wave also has a deceleration time parameter, i.e. the rate at which the flow decays after the mitral valve opens. This represents the rise in LV pressure during diastole obviously the more rapid the rise in pressure , the less diastolic filling there is going to be.
The A wave is the late diastolic wave, which represents the atrial “kick”. This is affected by LA pressure and LV compliance at the end of diastole, and also by atrial contractility and rhythm . If an A-wave is present and the patient has diastolic dysfunction, the A-wave is shorter in amplitude and in duration.
What Does Diastolic Dysfunction Feel Like
Diastolic heart dysfunction often creates the same array of symptoms that are found in other types of heart failure and cardiopulmonary diseases, including: Shortness of breath with exertion that gets progressively worse. Excessive fatigue.
Diastolic Heart Failure Pathophysiology | Circulatory System And Disease | Nclex-Rn | Khan Academy
Also Check: What Are Signs Of Heart Failure
Treatment Options For Diastolic Heart Dysfunction
We work with patients to pursue a full range of treatment options, including:
- A Healthy Lifestyle this includes maintaining a healthy weight, eating a balanced diet that’s low in salt and getting regular cardiovascular exercise, either on your own or as part of a cardiac rehabilitation program.
- Medications water pills can often help to alleviate the edema that is caused by diastolic dysfunction, and other medications can help to treat underlying medical problems like high blood pressure, diabetes or other heart conditions such as atrial fibrillation.
- Left Ventricular Assist Devices UPMC cardiologists have been on the leading edge of LVAD treatment since the technology was introduced in the 1980s, and have been leaders in improving the technology since then. These implantable devices pump blood into the body just as a healthy heart would, either as a “bridge” while waiting for a heart transplant or as a permanent valve replacement.
- Heart Transplant in rare cases, a heart transplant may be considered as a treatment for diastolic dysfunction. Our physicians are leading experts in heart transplantation as part of the UPMC Thomas E. Starzl Transplantation Institute, a nationally regarded center of excellence in transplantation.
Outlook For Heart Failure
Heart failure is a serious long-term condition that will usually continue to get slowly worse over time.
It can severely limit the activities you’re able to do and is often eventually fatal.
But it’s very difficult to tell how the condition will progress on an individual basis.
It’s very unpredictable. Lots of people remain stable for many years, while in some cases it may get worse quickly.
Don’t Miss: Symptoms Of Heart Attack.in Women
Transition From Diastolic Dysfunction To Heart Failure
Abnormalities in diastolic function may be manifested as impaired relaxation, which may or may not deteriorate LV filling during exertion but not at rest . This mildest form of diastolic dysfunction occurring typically at the initial stage of LV hypertrophy and can remain asymptomatic for several years . Diastolic abnormalities may lead to elevated filling pressure during exercise with the progression of the disease . When the disease goes on, diastolic dysfunction occurs, which may lead to elevated filling pressure at rest, left atrial enlargement, and, ultimately, atrial fibrillation, reduced exercise tolerance with signs of congestive heart failure .
Pathophysiology of diastolic heart failure. Abnormal relaxation and increased stiffness are associated with diastolic filling abnormalities and normal exercise tolerance in the early phase of diastolic dysfunction. When the disease progresses, pulmonary pressures increase abnormally during exercise with reduced exercise tolerance. When filling pressures increases further, left atrial pressure and size increase and exercise tolerance falls with clinical signs of congestive heart failure .
Preserved Systolic Function And Diastolic Dysfunction
Differences between proven diastolic heart failure and preserved systolic function are outlined in Chapter 6, together with definitions . Major causes are increasing age and/or left ventricular hypertrophy . Prognosis is serious, similar to that of systolic failure.257 Therapy trials are scant. Logically, the aim is regression of LVH, often the underlying cause. Vigorous therapy of underlying hypertension or aortic stenosis is essential. In clinical heart failure with hypertension, tight 24-hour BP control is mandatory. Other measures are a reduction in central blood volume by diuretics, countering tachycardia, aggressive treatment of AF, and management of concomitant coronary artery disease, including revascularization. Does RAAS blockade give specific benefit? Angiotensin II has powerful profibrotic and proapoptotic properties in the hypertrophic heart.258 Regarding ARBs, candesartan gave only modest benefit in one arm of the CHARM studies, in which there was heart failure with relatively preserved LV function.259 The ACE inhibitor perindopril also gave only modest benefits in clinical heart failure in the elderly, of whom 79% were hypertensive therapy decreased the BP and hospitalization.260 In Chapter 6 we concluded that clinical diastolic heart failure, however defined, merits the same overall therapy as systolic heart failure.
BERNARD J. GERSH, LIONEL. H. OPIE, in, 2013
Don’t Miss: Hypertension And Heart Failure
Systolic Heart Failure: A Closer Look
Systolic heart failure occurs due to a problem in the hearts contraction phase. Its characterized by stretching and weakening of the left ventricular muscle, due to which the heart pumps out less oxygenated blood to the body.
Its also known as heart failure with reduced ejection infraction. As the condition worsens, it can also weaken the right ventricle and take a toll on its pumping power too.
Related: What Are the Symptoms of Diastolic Dysfunction?
Obstructive Sleep Apnea And Diastolic Heart Failure
Isolated left ventricular diastolic heart failure with relative preservation of left ventricular systolic function is the most common form of heart failure in elderly subjects. The pathophysiologic consequences of this form of heart failure relate to a hypertrophied, noncompliant left ventricle, shifting the pressure-volume curve upward and to the left. Therefore, for a given left ventricular volume, left ventricular end-diastolic pressure increases, resulting in elevated left atrial and pulmonary capillary pressure, and pulmonary congestion and edema.
As noted previously, hemodynamic studies6364 of patients with OSA have documented that pulmonary capillary pressure increases during the course of an obstructive apnea, indicating development of diastolic dysfunction. During obstructive apnea, left ventricular transmural wall tension increases because of an increase in aortic blood pressure and a simultaneous decrease in juxtacardiac pressure. Furthermore, hypoxemia may impair left ventricular relaxation, further impairing diastolic function.77 Repeated exposure to nocturnal hypertension and hypoxemia, and consequent development of OSA-induced systemic hypertension and increased left ventricular mass, may also contribute to left ventricular diastolic dysfunction.
BERNARD J. GERSH, LIONEL H. OPIE, in, 2009
Don’t Miss: Early Signs Of Heart Failure
Heart Failure With Reduced Ejection Fraction
Systolic heart failure is also called heart failure with reduced ejection fraction .
Ejection fraction is the percentage of blood the left ventricle pumps out with every beat. A normal, healthy ejection fraction is 55% to 65%. If its higher or lower, that can indicate a heart problem.
With systolic heart failure, the ejection fraction is usually less than 50%.
Sex Differences In Cad And Diastolic Function
Diastolic heart failure is common and growing in prevalence, and women make up two-thirds of HFpEF cohorts and 40% of HFrEF.45 There are few published reports on sex differences in the association between CAD and diastolic function, except from Cho et al. from the Korean Womens Chest Pain Registry. Women and men were compared using propensity matching, and differences in diastolic functional parameters according to CAD severity were only found in women.46 CAD severity was associated with the presence of diastolic dysfunction only in women, with odds ratio of 1.92 . These authors suggest that myocardial ischemia may be the underlying pathophysiology for the higher prevalence of diastolic dysfunction and HFpEF in women.46 Although men are more likely to have obstructive coronary lesions, women are more likely to have microvascular disease and endothelial dysfunction, along with thicker arterial walls, nonobstructive CAD, and coronary vasospasm, which can lead to hypertrophy and fibrosis.45 These mechanisms likely play an important role in the development of HFpEF in women.
Pavan Bhat, W.H. Wilson Tang, in, 2021
You May Like: Congestive Heart Disease
Diastolic Heart Failure: Symptoms Causes Treatment
Heart failure has become a prevalent disease in both males and females worldwide. Heart failure can occur from any condition that comprises the contractility of the heart that is systolic heart failure or interferes with the relaxation ability of the heart is diastolic heart failure.
You can know or guess whether you are affected by a Diastolic heart failure condition or not you can study the symptoms that Ill describe here. Causers of diastolic heart failure and some basic treatment ideas are also included in this article. Lets move to the next.
Jump to…
Prevalence Of Diastolic Heart Failure
Diastolic heart failure is, unfortunately, more common than cardiologists previously believed. Echocardiographic studies have found the condition in 15 percent of participants under 50 years old, and in about 50 percent of people over the age of 70. It is largely a disorder for women, as up to 75 percent of those diagnosed are female. The failure is diagnosed when someone with diastolic dysfunction develops an episode of pulmonary congestion severe enough to present symptoms. If diastolic heart failure occurs once, the chances of it happening again are extremely high.
Recommended Reading: Acute Diastolic Congestive Heart Failure
Medications For Systolic Heart Failure
Depending on the severity of systolic heart failure and its underlying cause, your doctor may prescribe medications. Some of the drug options for treating systolic heart failure include:
- Angiotensin-converting enzyme inhibitors and angiotensin receptor blockers relax the blood vessels to lower blood pressure.
- Beta blockers make the heart beat more slowly and with less force.
- Aldosterone blockers help the body release sodium and water.
- Angiotensin receptorneprilysin inhibitors reduce excess fluid in the body and relax blood vessels, making it easier for your heart to pump blood.
How To Differentiate Systolic From Diastolic Dysfunction
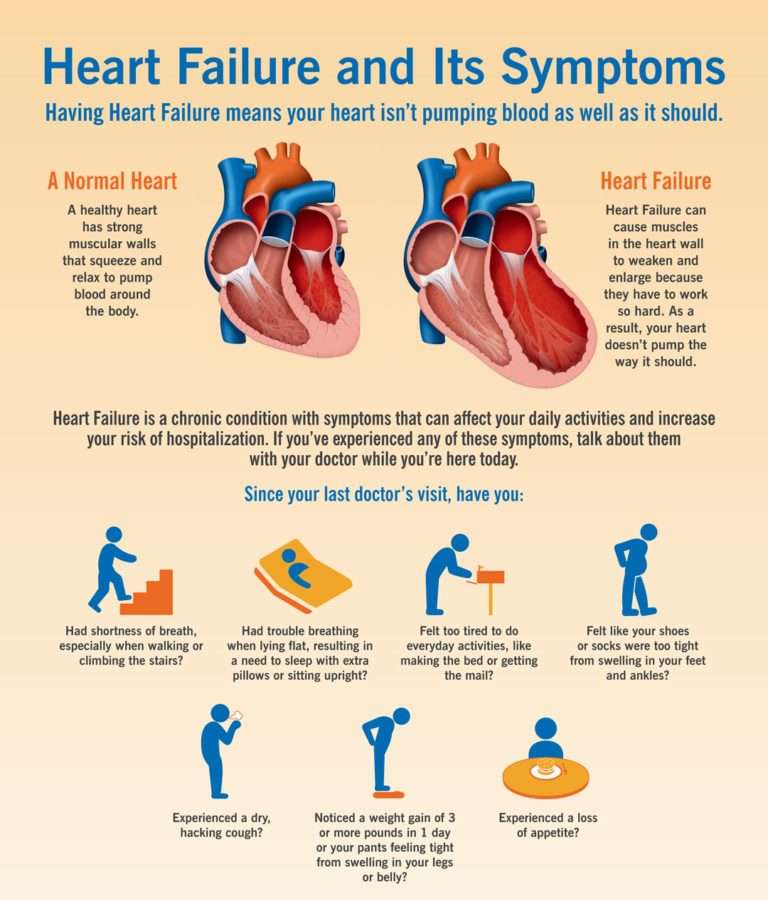
In contrast to systolic dysfunction where the heart muscle is weak, in diastolic dysfunction the heart is stiff. This means that the heart is unable to pump blood out of the heart in systolic dysfunction whereas the heart is unable to accept further blood in diastolic dysfunction. Both conditions lead to congestion or fluid accumulation in various organs of the body. Differentiation of heart failure from systolic and diastolic dysfunction is not possible as both diseases present with similar symptoms.
You May Like: Is Green Tea Good For Heart Attack Patients
Invasive Assessment Of Diastolic Function
Cardiac catheterization with simultaneous pressure and volume measurements is the gold standard for assessing LV diastolic function. Prerequisites are high-fidelity pressure recordings with simultaneous angio- or echocardiography or the use of the conductance technique. The rate of LV relaxation, rate and timing of diastolic filling as well as myocardial and chamber stiffness can be determined .
2.3.1 Isovolumic relaxation
The most commonly used index for quantitation of isovolumic relaxation is the time constant of relaxation . The pressure fall has been shown to be exponential under most circumstances but may deviate from a true mono-exponential pressure curve in aortic regurgitation or during myocardial ischemia. Calculation of the time constant of relaxation is currently the only reliable method for measuring the rate of relaxation . All other parameters such as isovolumic relaxation time, peak negative dP/dt, etc. are not true representatives of LV relaxation but are dependent on heart rate, peak systolic pressure, etc.
2.3.2 Diastolic filling
2.3.3 Passive diastolic function
PaVcSaEC
