Mediterranean Vs Keto Diet
The Mediterranean diet is a plant-forward diet and is considered safe for most people. If you have any medical conditions, you should talk with your healthcare professional before making major dietary changes, including the Mediterranean diet.
With numerous studies investigating the health effects of the Mediterranean diet, it has been generally regarded as a heart-healthy eating pattern.
The keto diet is a high-fat, very-low-carbohydrate diet. Diets high in fat may pose risks for heart health. If you have certain medical conditions, such as liver or kidney disease, the keto diet may not be safe. Whether or not people with diabetes, especially those taking insulin, should follow a keto diet remains controversial.
How the keto diet affects HDL and LDL cholesterol, triglycerides, and overall heart health is still being researched. Most studies on the connection have been short-term and have reached a variety of conclusions. The long-term effects of the keto diet on heart health remain unclear.
One major factor that affects cholesterol and, therefore, heart health outcomes is the type of fats consumed, with unsaturated fats being preferred over saturated and trans fats. If you are choosing to follow a keto diet, your healthcare professional may recommend regularly checking your cholesterol levels to ensure LDL levels do not become too high.
How Much Salt Should You Eat
If youâre living with congestive heart failure, itâs best if you limit the sodium in your diet to less than 1,500 milligrams a day. Thatâs far less than the amount that most Americans eat — 3,400 milligrams.
You may not realize it, but itâs likely that more than 70% of the sodium in your diet comes from packaged foods and meals cooked in restaurants. Buying fresh foods and cooking at home are some of the best ways to cut back.
Foods To Avoidin The Diet
As the heart muscles in seniors with congestive heart failure become weakened, many kinds of foods can damage the heart further. That is why assisted living facilities prepare low-sodium meal plans for such seniors.
Foods that have high sodium or salt can cause the body to retain more fluids and lead to increased blood pressure. This can be very dangerous for seniors with congestive heart failure. To steer clear of excessive sodium intake, seniors are advised to avoid consuming foods like frozen dinners, canned soups, smoked, cured, or canned meat, salted snacks and nuts, instant pudding, cottage cheese, salad dressing, and vegetable juice.
Aside from that, foods rich in cholesterol and saturated fat should also be avoided to manage the symptoms of the heart condition. These include fatty pieces of meat, butter, margarine, fried foods, processed grains, white rice, pasta, white bread, and boxed cereals. Saturated fat and cholesterol can lead to the clogging of the arteries, which can disrupt the circulatory system in seniors and cause other complications.
Caregivers at assisted living communities also make sure that seniors with congestive heart failure do not consume alcohol, as that can raise blood pressure and heart rate or lead to an irregular heartbeat. Even red wine, which is usually considered good for the heart, is not recommended to seniors with congestive heart failure. Drinking too much water is also bad for seniors diagnosed with the heart disease.
Recommended Reading: What To Do When Having A Heart Attack Alone
Study Data Contradict Recommendations For A Low Sodium Diet:
Despite the organizations emphasis on keeping sodium under 1,500 mg/day to avoid heart failure, a study suggests that people who already have heart failure are at greater risk of hospitalization or death if they restrict sodium intake to less than 2,500 mg/day . The study included 833 people with heart failure out of these individuals, 145 were on a restricted sodium diet.
Do You Need Natural Health Products
You can usually get all of your vitamins and minerals by eating a heart-healthy diet that is rich in fruits and vegetables.
Your doctor might recommend a multivitamin/mineral supplement if you are undernourished or cannot completely meet your nutritional needs through food.
If you take a diuretic for heart failure, this medicine might change your dietary needs for potassium, magnesium, calcium, and zinc. Ask your doctor if you should take natural health products or eat certain foods to get enough of these minerals.
Fish oil supplements have been shown to help some heart failure patients. In some studies, fish oil supplements, taken along with other heart failure medicines, helped people stay out of the hospital and live longer.footnote 1
Talk to your doctor before you take any over-the-counter medicine or supplement. They are used along with medical treatments for heart failure, not instead of treatment.
Potassium
If you take a diuretic, ask your doctor if you need to take a potassium supplement or if you need to watch the amount of potassium in your diet. If you take a loop diuretic or thiazide diuretic, your doctor may suggest that you get extra potassium because these medicines lower your potassium levels. But if you take a potassium-sparing diuretic, you might not need to get extra potassium in your diet.
Magnesium
Good food sources of magnesium include seeds, nuts, legumes, unmilled cereal grains, and dark green vegetables.
Calcium and zinc
You May Like: How To Get Your Heart Rate Up Without Exercise
Fluid Restriction In Heart Failure
In addition to a low-sodium diet, a fluid restriction is commonly recommended for heart failure.
Limiting the amounts of fluids you consume is thought to reduce excess fluid from accumulating in your body, which can overload your heart and cause shortness of breath and swelling in your legs .
A fluid restriction usually limits fluids to 1,5002,000 mL per day but can be as low as 800 mL .
Here are examples of fluids:
Foods like ice cream, yogurt, pudding, and sauces may also need to be taken into consideration as fluids.
Like a low-sodium diet, however, the evidence for fluid restriction in heart failure remains mixed.
A review of six studies found there were no significant differences in hospital readmission rates or death from any cause in patients who restricted their fluid intakes compared with those who didnt .
The same review, however, found that brain natriuretic peptide levels were significantly higher in patients who didnt follow a fluid restriction.
BNP is a hormone that is secreted when the heart becomes stressed, and increased levels have been associated with poor health outcomes and longer hospital stays for heart failure .
While these results suggest that people who follow a fluid restriction have similar health outcomes as those who dont, additional research is necessary to determine whether fluid restriction can strongly be recommended or discouraged as a treatment option for heart failure .
Efficacy Of Dietary Sodium Restriction In Heart Failure: Urban Legend Or Scientific Fact
- A
- A
Dietary sodium restriction has traditionally been advocated to prevent fluid overload and adverse outcomes for patients with heart failure . The Study of Dietary Intervention under 100 mmol in Heart Failure was an international, open-label, randomized controlled trial designed to assess whether reduction in dietary sodium reduced the incidence of future clinical events. The primary outcome was a composite of cardiovascular-related admission to hospital, emergency department visit, or all-cause death.1
In SODIUM-HF trial, 806 patients with chronic HF class II-III receiving optimal guideline-directed medical therapy were randomized 1:1 to a low sodium diet of < 1500 mg/day or usual care.1 Over a 12 month period, all-cause death occurred in 6% of the low sodium and 4% of the usual care group while, cardiovascular-related hospitalization occurred in 10% of the low sodium and 12% of the usual care group . Cardiovascular related ED visits also occurred in 4% of patients in the low sodium and usual care group .1
References
Don’t Miss: Does Magnesium Help With Heart Palpitations
Nutrition Guide For Heart Failure
Following a low-sodium diet and drinking less fluid can help you feel better and allow your heart failure medicines to work better. A low-sodium diet may even keep you out of the hospital. It is not an easy diet to follow. You may find eating with heart failure is a bit of a balancing act. While you dont want to eat too much of high sodium foods, you have to be sure to eat enough to maintain good nutrition.
Nutrition and Heart Failure
The recommended salt intake is 2,000 mg of sodium per day.
Salt is a mineral that is made of sodium and chloride. It is found in food, table salt and sea salt. Sodium acts like a sponge and makes the body hold water.
Eating too much sodium when you have heart failure can cause fluid buildup in your legs, stomach and lungs and force you heart to work harder.
Most of the sodium we eat is hidden in foods. Even food that does not taste salty can contain a lot of sodium.
You should restrict the amount of sodium you eat to 2,000 mg or less each day. Try to keep the sodium content of each meal to less than 600 mg. This helps spread out your sodium intake over the day to prevent excessive fluid retention.
You can take a few basic steps to reduce the amount of sodium in your diet:
- Dont add salt when you cook or at the table
- Learn to read food labels
- Choose more foods that are lower in sodium
- Limit high sodium foods
Reading a Food Label for Sodium
Follow these easy steps to read the label:
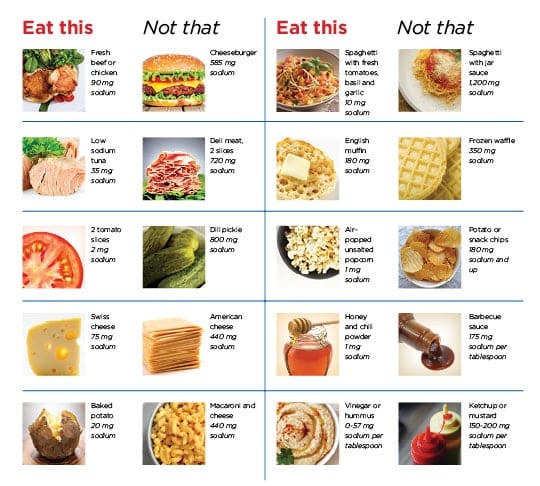
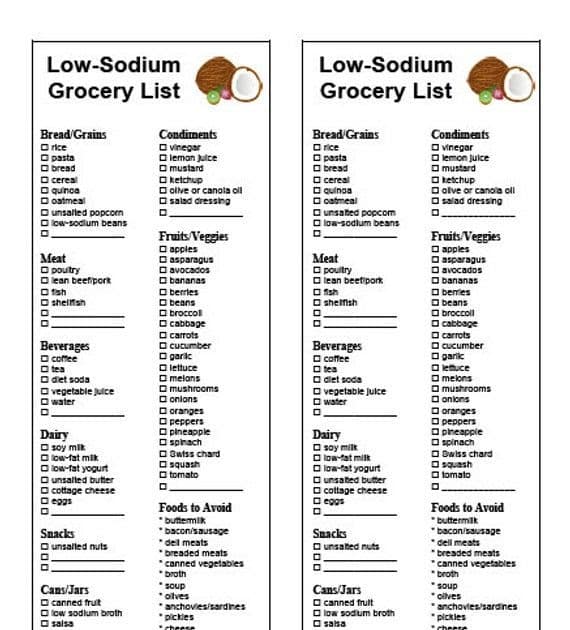
Low-Sodium Foods
Nutrition Tips For Congestive Heart Failure
If you have congestive heart failure, follow these nutrition guidelines:
- Check food labels, and bound salt and sodium to 1,500 to 2,000 milligrams per day.
- Substitute salt and other high-sodium seasonings with replacements that have no salt or are low in sodium.
- While dining out, think about unrevealed sources of salt and sodium, such as salad dressings and soups. Ask for options low in salt and sodium.
- Select meats and other foods that are low in saturated fat to help in lowering your cholesterol levels.
- Avoiding alcohol is must. If your heart failure is caused by alcohol, its especially important that you dont drink any alcoholic beverages.
Read Also: Do All Heart Attacks Damage The Heart
Recommended Reading: Heart Surgery Charity Organizations
What Causes Congestive Heart Failure In Dogs
Dog congestive heart failure, as mentioned, refers to an inability of the heart to pump blood adequately. This is most often caused by forward resistance or the back-leaking of blood into the heart.
In dogs, the two most common causes are:
- Mitral valve insufficiency: Blood leaks through the mitral valve from the left ventricle into the left atrium.
- Dilated cardiomyopathy: The ventricle stretches, thins and canât pump blood as well, and it has been linked to certain grain-free diets containing peas and/or legumes.
High blood pressure, or hypertension, is also a common cause. Blood pressure can be affected by your dogs diet.
Get Rid Of The Salt Shaker
When it comes to reducing salt in your diet, out of sight, out of mind is an effective approach. Simply getting rid of the salt shaker in your kitchen or on the dinner table can make a big impact.
Need some motivation? One shake of salt contains about 250 mg of sodium, which is one-eighth of your daily intake.
Also Check: What Should Resting Heart Rate Be For A Woman
Bread And Grains: Choose 6 Or More Servings Per Day
- Low-sodium whole-grain breads, rolls, bagels and cereals .
- 1/2 cup whole-wheat pasta .
- 1/2 cup brown rice.
- Low-sodium whole-grain crackers .
- 3 cups low-sodium popcorn.
- 1 cup fresh fruit.
- 1/4 cup unsalted nuts.
Note: For a diet in which you consume 2,000 mg of sodium per day, a sample plan might involve eating 500 mg at breakfast, 250 mg for snacks twice daily, 500 mg for lunch and 500 mg for dinner.
It takes about three to six weeks for your tastebuds to start to adjust and stop missing the salt so much, notes Taylor. Stick with it and allow your body to get used to your new food choices. Instead of focusing on all the foods to avoid, focus on all the healthy foods you should be eating. Your grocery cart should look like you just came from the farmers market full of actual foods, not just products.
What Should We Do
People with congestive heart failure should not change their dietary sodium intake on their own. Instead, we recommend discussing the latest research with a cardiologist. Heart failure is a serious condition that requires constant and careful medical supervision. Changing dietary habits suddenly could lead to disaster!
Physicians should keep up with the latest evidence with regard to sodium and health. Accepting guidelines without reviewing the underlying data does not lead to the best patient care.
Recommended Reading: Does Caffeine Affect Heart Rate
Point: Moderate Sodium Intake Is Harmful For People With Heart Failure
Sodium intake is associated with fluid retention, hence the puffiness and bloating that may follow a very salty meal. And excessive sodium intake may worsen high blood pressure, or hypertension. High blood pressure increases the risk of developing heart failure and can worsen existing heart failure. Hypertension may also lead to other types of heart disease, stroke, or kidney failure. A low-sodium diet may help lower or prevent high blood pressure, and may reduce the risk of such diseases.
High-sodium diets are also usually high in total fat and calories, which may lead to obesity and its many associated complications. Some studies also suggest that there may be a link between sodium intake and osteoporosis and stomach cancer. Additionally, consuming salty foods over a long period of time can accustom your taste buds to the taste, and in turn make you more likely to reach for saltier foods.
Recipes For Congestive Heart Failure Patients
Green Bean Casserole. Mamas Green Bean Casserole. Low-Sodium Green Bean Casserole Thanksgiving, Christmas recipe idea for low-salt diets or those who have heart failure. Slaw Recipes.
Buckwheat pancakes. Chicken and asparagus tossed with penne. Chicken brats. Chicken salad with pineapple and balsamic vinaigrette. Chicken tamales. Chili. Cinnamon French toast. Corn tamales with avocado-tomatillo salsa.
Also Check: Little Smokies Recipe With Grape Jelly
You May Like: What Does Congested Heart Failure Mean
Find Alternative Thirst Quenchers
Its tempting to guzzle a bunch of water when youre thirsty. But sometimes, just moistening your mouth can do the trick.
The next time youre tempted to gulp down some water, try these alternatives.
- Swish water around your mouth and spit it out.
- Suck on sugar-free candy or chew sugar-free gum.
- Roll a small ice cube around the inside of your mouth.
Portion Out Your Fluids
Try to distribute your fluid consumption throughout your day. If you wake up and drink a bunch of coffee and water, you might not have much room for other fluids throughout the day.
Budget the 2,000 mL throughout your day. For example, have 500 mL for breakfast, lunch, and dinner. This leaves with room for two 250 mL drinks between meals.
Work with your doctor to determine how much you need to restrict your fluid intake.
Read Also: Can Heat Cause Heart Palpitations
Heart Failure And A Very Low Sodium Diet:
In heart failure, the cardiac muscle struggles to pump blood efficiently. As a result, fluid may build up in the lower legs or even the lungs. For decades, doctors have warned heart failure patients to restrict their salt intake as much as possible, to help control blood pressure and to reduce edema.
A recent re-analysis of the data from a gold-standard heart failure trial, the TOPCAT trial, suggests this advice may not be helpful. Specifically, the people in the trial had a type of heart failure characterized as preserved ejection fraction. In this condition, the heart still pumps with vigor, but the chamber is stiff and doesnt fill up with blood as it should. Most people with this type of heart failure also have high blood pressure. As a result, physicians try to do everything they can to bring blood pressure under control. High sodium intake is associated with hypertension, so it makes sense to lower sodium intake. However, new research suggests that an extremely low sodium diet is not helpful.
Caring For Someone With Heart Failure
Looking after someone with heart failure can mean anything from helping with hospital or GP visits and collecting prescriptions, to full-time caring.
There are many ways you can support someone with heart failure.
Heart failure can be disabling and distressing, and many people with the condition find it a huge relief to share their concerns and fears with someone.
As a carer, if you can attend GP and hospital appointments with the person with heart failure, you can encourage them to ask the right questions while you note down the answers.
You could also provide the doctor with additional information or insights into the personâs condition, which can be helpful for planning the right treatment.
Another way you can help is by watching for warning signs that the personâs heart failure is getting worse or theyâre not responding to treatment.
Contact the personâs doctor if you notice a new symptom or their current symptoms are getting worse.
Signs to look out for include:
- shortness of breath that isnât related to usual exercise or activity
- increased swelling of the legs or ankles
- significant weight gain over a few days
- swelling or pain in their tummy
- trouble sleeping or waking up short of breath
- a dry, hacking cough
- increasing tiredness or feeling tired all the time
See the care and support guide for information about all aspects of caring for someone with a long-term condition.
Read Also: Heart Rate Of 100
What Is Congestive Heart Failure
Heart failure is a condition in which the chambers of your heart dont fill with enough blood or your heart isnt strong enough to pump sufficient blood from these chambers to your bodys tissues.
Its commonly caused by heart disease, high blood pressure, and diabetes, and most often occurs in older adults and people who are obese .
As a risk factor for heart disease, high cholesterol can also increase your risk of developing heart failure.
Heart failure symptoms may include :
- shortness of breath
- swelling in your ankles and feet
- swelling of your abdomen
- rapid weight gain from fluid retention
- fast heart rate
Your doctor may review your medical history, conduct a physical examination, and perform tests like a chest X-ray or heart ultrasound to diagnose heart failure .
