How Is Congenital Heart Disease Diagnosed
In most cases, congenital heart disease is diagnosed during pregnancy, but it may only be diagnosed after birth.
Diagnosis during pregnancy
During pregnancy, congenital heart disease can be detected during the ultrasound scan at around 1822 weeks, also known as the anatomy scan. If your doctor suspects your baby has a congenital heart disease, they will refer you for further testing, such as a foetal echocardiography to specifically scan the heart of your baby to confirm the diagnosis. However, it is not always possible to detect heart defects using foetal echocardiography if the defect is mild.
Diagnosis after birth
Your doctor can diagnose congenital heart disease after your baby is born if they show symptoms such as being blue around their skin or lips, swelling in their tummy or around their eyes, or shortness of breath when feeding. Your doctor will check your babys heart as part of the newborn and 6-week check examinations. If your baby doesnt have any symptoms, a heart exam can sometimes pick up murmurs, which may be a sign of congenital heart disease.
Depending on what your doctor thinks is causing the symptoms, further testing may be needed, including:
- a chest x-ray
- echocardiography
- electrocardiography
- cardiac catheterisation this procedure involves passing special tubes through an artery or vein to take recordings and x-rays of the heart under anaesthetic.
In some types of congenital heart disease, symptoms dont show up until later as a child or an adult.
What Else Should I Know
As kids get older, it’s important to help them learn how to take charge of their medical care. A younger teen could fill a prescription or schedule an appointment. Older teens should understand health insurance coverage and know how to access their medical records.
Help an older teen move from a pediatric cardiologist to one who cares for adults. He or she should play an active role in choosing the new doctor. Encourage your child to make appointments, ask questions and take notes, and set aside time to speak with the doctor alone.
To prepare for adulthood and manage their health care, teens should know:
- about their heart condition
- when to get care
- the names of all medicines, their dosages and when to take them, common side effects, and interactions with other medicines
- if they have allergies to food or medicine
- the answers to most questions about their health and medical history
- how to:
How Do You Know If Your Baby Has A Congenital Heart Defect
If your health care provider doesnt find a severe congenital heart defect in your baby during pregnancy, its usually diagnosed soon after birth or during the first few months of life. Less severe heart defects may not be found until children are older.
During pregnancy
Your provider may use a test called fetal echocardiogram to check your babys heart. This test uses ultrasound to make a picture of your babys heart while still in the uterus . You can have this test at about 18 to 24 weeks of pregnancy.
You may need a fetal echocardiogram if:
- Your provider finds a possible problem, like an abnormal heart rhythm in your baby, during an ultrasound.
- Your baby has a genetic or chromosomal condition, like Down syndrome, that may be linked to CHDs.
- You have a family history of heart problems. This means that you, your partner or someone in your families has heart problems.
- You have a health condition, like diabetes, that may play a role in CHDs.
- Youre taking a medicine that can increase the risk of your baby having a CHD.
After birth
Your baby is tested for critical CHDs as part of newborn screening before she leaves the hospital after birth. Newborn screening checks for serious but rare and mostly treatable conditions. It includes blood, hearing and heart screening. All states require newborn screening, and all states except California require screening for critical CHDs. California requires that providers offer screening for critical CHDs.
You May Like: Can Flonase Cause Heart Palpitations
Problems That Cause Too Much Blood To Pass Through The Lungs
These defects allow oxygen-rich blood that should be traveling to the body to re-circulate through the lungs, causing increased pressure and stress in the lungs. They include:
- Patent ductus arteriosus : This defect short circuits the normal pulmonary vascular system and allows blood to mix between the pulmonary artery and the aorta. Prior to birth, there is an open passageway between the two blood vessels. This opening closes soon after birth. When it does not close, some blood returns to the lungs. Patent ductus arteriosus is often seen in premature infants.
- Atrial septal defect : In this condition, there is an abnormal opening between the two upper chambers of the heart the right and left atria causing an abnormal blood flow through the heart.
- Ventricular septal defect : In this condition, a hole in the ventricular septum occurs. Because of this opening, blood from the left ventricle flows back into the right ventricle, due to higher pressure in the left ventricle. This causes an extra volume of blood to be pumped into the lungs by the right ventricle, often creating congestion in the lungs.
- Atrioventricular canal : AVC is a complex heart problem that involves several abnormalities of structures inside the heart, including atrial septal defect, ventricular septal defect, and improperly formed mitral and/or tricuspid valves.
What Is Congenital Heart Disease
Posted in Blog
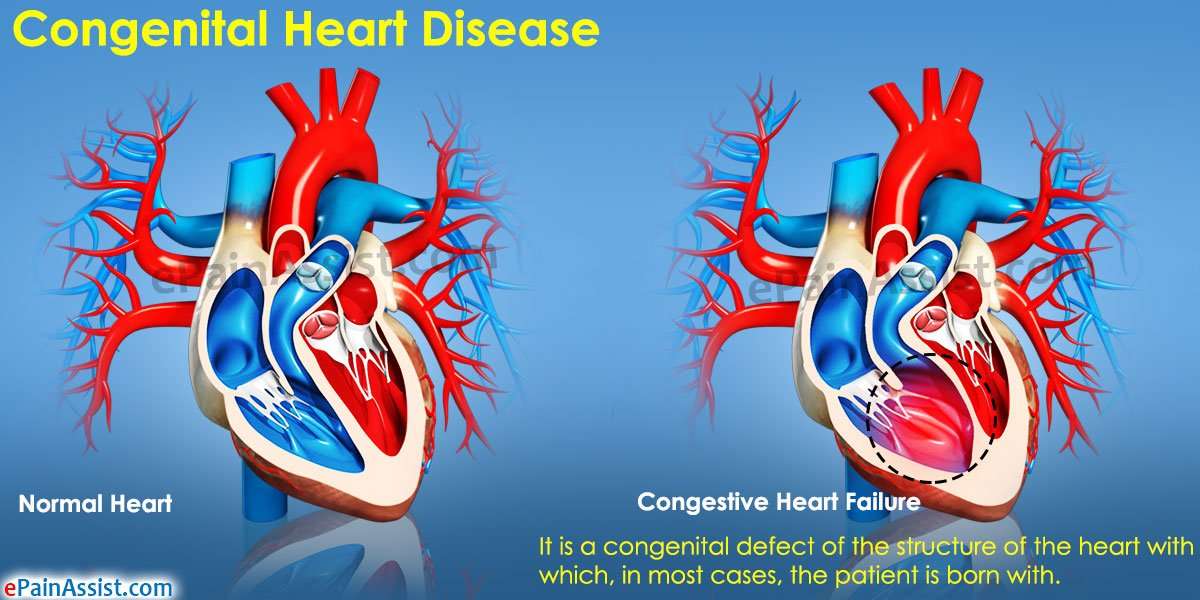
Congenital heart disease is a term for a variety of birth defects that affect the normal way the heart works. Congenital means the condition is present at birth. Known as the most common birth defect, 1 out of every 100 babies born in the United States suffer from congenital heart disease.
But What is Congenital Heart Disease? And why does it happen?
Read Also: Heart Palpitations Prednisone
Implications Of Classifying Congenital Heart Disease As A Heart Failure Syndrome
What is the usefulness of this new categorisation? First and most obviously neurohormones are an important therapeutic target in patients with heart failure. Plasma neurohormone levels are of prognostic importance in this condition and neurohormonal activation appears to beget further neurohormonal activation by perpetuating a decline in cardiac function. The antagonism of neurohormonal systems appears to retard this process and consequently improves symptoms and increases survival rates. The prognostic significance of neurohormonal activation in the context of congenital heart disease ought to be ascertained although a case could be made for commencing neurohormonal antagonism, by analogy to work already published in other heart failure syndromes, even in the absence of this data. Longitudinal studies are clearly required to gauge the impact of neurohormonal antagonism on morbidity and mortality in these previously untested groups.
How Can I Improve My Quality Of Life With Heart Failure
There are several things you can do to improve your quality of life if you have heart failure. Among them:
- Eat a healthy diet. Limit your consumption of sodium to less than 1,500 milligrams each day. Eat foods high in fiber. Limit foods high in trans fat, cholesterol, and sugar. Reduce total daily intake of calories to lose weight if necessary.
- Exercise regularly. A regular cardiovascular exercise program, prescribed by your doctor, will help improve your strength and make you feel better. It may also decrease heart failure progression.
- Don’t overdo it. Plan your activities and include rest periods during the day. Certain activities, such as pushing or pulling heavy objects and shoveling may worsen heart failure and its symptoms.
- Prevent respiratory infections. Ask your doctor about flu and pneumonia vaccines.
- Take your medications as prescribed. Do not stop taking them without first contacting your doctor.
- Get emotional or psychological support if needed. Heart failure can be difficult for your whole family. If you have questions, ask your doctor or nurse. If you need emotional support, social workers, psychologists, clergy, and heart failure support groups are a phone call away. Ask your doctor or nurse to point you in the right direction.
Don’t Miss: How To Calculate Target Heart Rate Zone
Can Surgery Be Used To Treat Heart Failure
In heart failure, surgery may sometimes prevent further damage to the heart and improve the heart’s function. Procedures used include:
- Coronary artery bypass grafting surgery. The most common surgery for heart failure caused by coronary artery disease is . Although surgery is more risky for people with heart failure, new strategies before, during, and after surgery have reduced the risks and improved outcomes.
- Heart valve surgery. Diseased heart valves can be treated both surgically and non-surgically .
- Implantable left ventricular assist device . The LVAD is known as the “bridge to transplantation” for patients who haven’t responded to other treatments and are hospitalized with severe systolic heart failure. This device helps your heart pump blood throughout your body. It allows you to be mobile, sometimes returning home to await a heart transplant. It may also be used as destination therapy for long-term support in patients who are not eligible for transplant.
- Heart transplant. A heart transplant is considered when heart failure is so severe that it doesn’t respond to all other therapies, but the person’s health is otherwise good.
The Future Of Personalized Treatment Of Hf In Achd
Another promising aspect of how genomics can help tailor therapy in HF in ACHD is targeted therapy of particular pathways known to be involved in the progression to heart failure. While it seems early to discuss therapeutics because most of the complex genetic aspects of HF in CHD remains incompletely understood, there has been at least one example with inhibition of the pathways that leads to HCM in NS, where a clinical trial using a MEK1 inhibitor is underway . Once other pathways are clearly defined, similar targeted therapy for the prevention of HF in other forms of ACHD may follow. Progress towards this goal has been enabled by high throughput sequencing technologies and with the availability of patient-specific induced pluripotent stem cells from patients with cardiomyopathies where drug specific cardiotoxicity was demonstrated at the single-cell level. These cells could be used for rapid screening of cardioactive drugs with the patients genetic background, an approach being assesed in primary cardiomyopathy.,
Also Check: Does Tylenol Increase Heart Rate
Natural Treatments For Heart Failure
Avoiding alcohol if you have had heart failure is an essential way to reduce your risk of any future heart complications. If you smoke, your doctor will also recommend that you quit, which will reverse any damage done to your blood vessels and preventing future problems.
Getting enough sleep is also important for preventing heart failure because a lack of restful sleep leaves your heart tired, which reduces its efficiency.
There are also supplements that have been shown to boost heart health and prevent heart failure as well as maintain better health if you have already had heart failure. The top natural supplements to try include:
Omega-3 fatty acid MagnesiumAstaxanthin
Types Of Congenital Heart Defects
There are many different types of congenital heart defects, but in general, they are typically divided into three main categories:
- Heart valve defects: Valves inside the heart direct blood flow and sometimes close up or leak this affects the hearts ability to pump blood correctly.
- Heart wall defects: When the natural walls that exist between the left and right sides of the heart do not develop correctly, the upper and lower chambers of the heart can cause blood to back up. This goes into the heart and may build up in places where it doesnt belong. This puts more pressure on the heart, which requires it to work harder. Often this leads to high blood pressure.
- Blood vessel defects: The arteries and veins in your body carry blood to the heart and back out to the body. If these do not work properly, they can reduce or block blood flow.
Recommended Reading: Can Flonase Cause Heart Palpitations
Single Ventricle Defects And The Fontan Circulation
Congenital heart defects in which only one of the hearts two ventricles is fully formed are called single ventricle defects. Often, a heart valve is missing.
Children diagnosed at birth with a single ventricle defect are treated with multiple, staged surgeries to create a new configuration called the Fontan circulation, in which blood passes from the veinsinstead of the ventricleto the pulmonary artery and then to the lungs. Oxygenated blood returns from the lungs to the heart, where it is pumped to the body by the ventricle. Adults with the Fontan circulation can develop heart rhythm disorders, blood clots, heart failure, or liver disease.
Factors That Can Worsen Symptoms Of Heart Failure
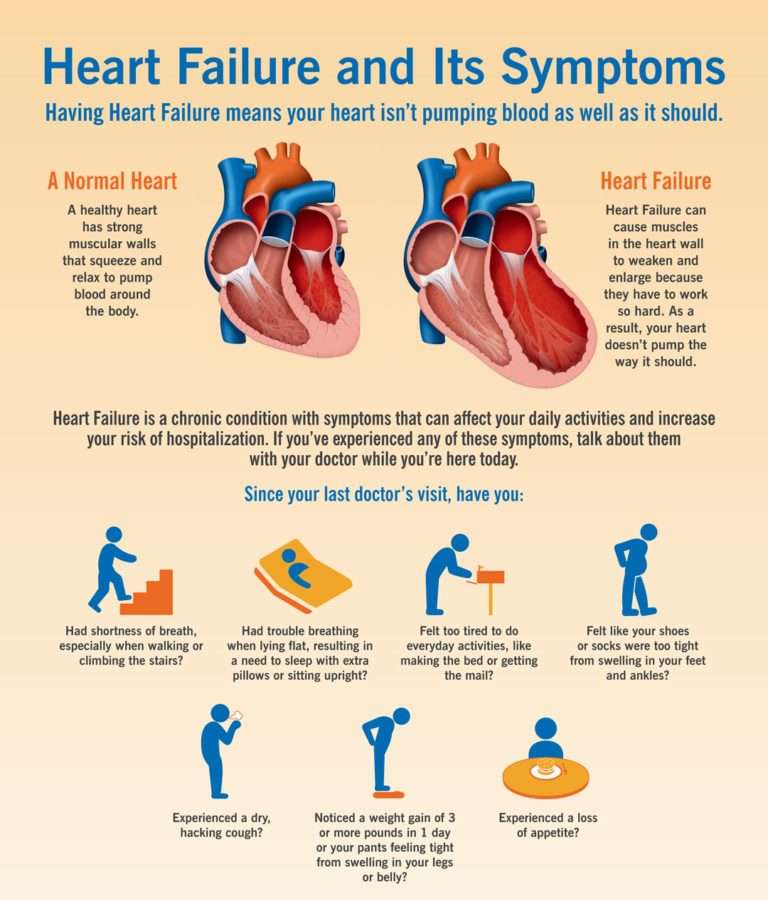
The symptoms of heart failure can be worsened by a number of factors, including:
- anaemia
- too much salt, fluid, or alcohol in the diet
- pregnancy
- some viral and bacterial infections
- kidney diseases
Treatment for heart failure may include:
- medicines, such as
- diuretics to remove excess fluid and improve symptoms of heart failure
- mineralcortiocoid receptor antagonists are also recommended and used in most patients with heart failure to reduce mortality and hospitalisation
- ACE inhibitors to open up blood vessels, reduce blood pressure and reduce sodium retention and water retention
- certain beta-blockers to slow the heart rate and reduce its work
- aldosterone blockers to reduce blood pressure and reduce the effects of damage to the heart muscle
- ACE inhibitors, beta blockers and aldosterone blockers can increase survival and reduce the likelihood of hospitalisation.
Recommended Reading: Does Benadryl Lower Heart Rate
What Is The Best Diet For Congestive Heart Failure
Once you are diagnosed with congestive heart failure, you will meet with your medical team, which includes a nutritionist. They will provide you with guidelines on what activities you can do, along with an eating plan that helps manage your condition. Your diet should be low in sodium, cholesterol, and saturated fat. You can still eat lean protein like chicken, certain types of fish, seafood, legumes, whole grains, fresh fruit, and vegetables.
Monogenic Causes Of Heart Failure In Cardiomyopathy And Chd
The genetic basis of HCM was first described in 1990., Following this discovery, the principal genetic causes of hypertrophic, dilated and arrythmogenic cardiomyopathies have been identified. Depending on phenotype, a disease causing mutation can be found in 3070% of patients. Culprit genes encode structural proteins such as those that form the sarcomere, cellular cytoskeleton, or ion channels. Genetic testing for inherited cardiomyopathies is clinically available and improves the efficiency of family screening, enabling early diagnosis and timely clinical management in at-risk individuals.
Don’t Miss: Why Do Av Nodal Cells Not Determine The Heart Rate
Congenital Heart Defects May Or May Not Impact A Child’s Life
There are no cures for congenital heart defects. When it comes to determining how dangerous they are, Dudley says that congenital heart defects occur on a spectrum.
On one end are the defects that aren’t very dangerous, where a person can live normally. These include small holes in the heart, as with atrial septal defects, that don’t cause symptoms and may close over time.
On the other side are critical defects that must be dealt with immediately, as with single ventricle defects, where the baby could die within the first month of life. Of all babies born with a heart defect, 25% will have a critical defect that requires heart surgery within their first year of life, according to the CDC.
A doctor must decide if a congenital heart defect is dangerous enough to require intervention immediately, or if the treatment can wait until the child is older and more developed. Depending on the severity, a child might need medication such as ibuprofen to expedite the closing of holes in the heart or a more serious heart procedure like surgery or catheterization.
Those with congenital heart defects can live a normal life, though Dudley says they might not be able to exercise as vigorously as those born with healthy hearts.
If you’re pregnant, having a congenital heart defect is a common cause of heart problems and complications for the pregnancy. So you are especially advised to talk to a doctor about how the condition can affect both you and the baby.
What Are Common Congenital Heart Defects And How Are They Treated
Common CHDs include:
Patent ductus arteriosus . This condition happens in the connection between two major blood vessels leading from the heart: the pulmonary artery and the aorta. The ductus arteriosus is open when a baby is in the womb. If it doesnt close properly after birth, blood that doesnt have enough oxygen can flow in the wrong direction. This can weaken the heart muscle and lead to heart failure. Sometimes a PDA may close on its own. But some babies need medicine, procedures with catheters or heart surgery.
These conditions leave a hole in the septum. This can cause blood to go in the wrong direction or to the wrong place, or it can cause extra blood to be pumped to the lungs. Types of septal defects include:
- Atrial septal defect . This is when the hole is in the wall that separates the right and left atria.
- Ventricular septal defect . This is when the hole is in the wall that separates the right and left ventricles. VSDs are the most common type of heart defect.
- Atrioventricular septal defect . This is when there are holes between the chambers of the right and left side of the heart, and the valves between these chambers may not form correctly.
Some small septal defects close on their own. Heart surgery or procedures with catheters can fix larger septal defects. Babies with AVSD usually need heart surgery.
Read Also: What Is A Typical Resting Heart Rate For A Healthy Individual
