Clinical Consequence Of Findings At Echocardiographic Screening
Echocardiographic screening could potentially have an impact on management for 31 of the participating patients. Only one of the 19 patients who were found to have an LVEF40% without previously having been diagnosed with a heart failure, received both beta-blockers and angiotensin-converting enzyme inhibitors/angiotensin receptor blockers . Thus, 7% of the screened population would potentially benefit from early detection of systolic dysfunction and initiation of evidence- based heart failure therapy. With regards to valve disease, none of the patients who were found with previously unrecognized aortic or mitral stenosis or regurgitation in our study would qualify for valve replacement based on severity and symptoms combined. However, the findings in 13 patients who were previously unrecognized suggest that they should undergo careful clinical and echocardiographic reevaluation at regular or intensified intervals. It was not evident if and why the two patients with symptomatic, severe aortic stenosis had not been evaluated for valve replacement.
Fig. 2
Prevalence of evidence based heart failure treatment in haemodialysis patients with LVEF40%. ACE-I denotes angiotensin converting enzyme inhibitor ARB, angiotensin receptor blocker MRA mineralocorticoid/aldosterone receptor antagonist LVEF, left ventricular ejection fraction
Logistic Regression Analysis Of The Heart Failure Risk Using The Nyha Classification
The multivariate logistic regression analysis of the heart failure risk using the NYHA classification found that CTR, Hb, Ht, and weekly CCr were not associated with heart failure classification. The Youden indexes on the ROC curves for the NYHA classification for CTR, Hb, Ht, and weekly CCr were > 51.9%, < 9.4g/dL, < 29.2%, and < 80.9L/week/1.73m2, indicating a high risk of heart failure. Moreover, a CTR of 0.430.49 has been previously reported to be associated with higher in-hospital mortality and poor long-term clinical outcomes . However, a CTR> 0.5 is traditionally considered abnormal, and the target Hb for PD patients has been set at 1113g/dL in Japan . Furthermore, as described earlier, a weekly CCr> 50L/week/1.73m2 is recommended . The present findings are consistent with the use of these values.
A previous study has shown that intravenous iron therapy may be effective for iron deficiency anemia , but its benefit is partially independent of Hb concentration . Other studies have demonstrated direct links between IDA and both quality of life and mortality, and iron repletion reduces the severity of the restless legs symptom and improves cognition, physical performance, exercise tolerance, and immune function, implying that both anemia and iron deficiency contribute to the cardiovascular risk and mortality .
The Use Of Peritoneal Dialysis In Heart Failure: A Systematic Review
- The Japan PDOPPS Study Committee
- Adult Palliative care for Nursing, Health and Social Care2019
- Adult Palliative care for Nursing, Health and Social Care2019
- Solution-Focused Therapy: Theory, Research & Practice2011
- Solution-Focused Therapy: Theory, Research & Practice2011
- Stress Management: From Basic Science to Better Practice2005
- Research in Psychotherapy and Counselling2008
- Handbook of Group Counseling and Psychotherapy2004
Read Also: How To Calculate Training Heart Rate
Ckd: Protect Your Heart
Over time, CKD often gets worse and can lead to kidney failure. A person with kidney failure will need regular dialysis or a kidney transplant to survive.
Although dialysis is needed because of CKD, heart disease is the most common cause of death for someone on dialysis. This is because when kidneys dont function properly, the heart has to work harder to circulate blood, leading to high blood pressure and possibly heart disease.
If you or a loved one needs dialysis, look at these tips to help protect your heart:
- Choose foods that are healthiest for your heart and your kidneys. Ask your doctor for a referral to a dietitian whos trained in CKD nutrition to understand which foods and beverages are best for you. You can learn more about dialysis and a healthy diet here.
- Regular physical activity helps to lower your blood pressure and improve your heart health. Moving more doesnt have to be strenuous! Some great ways to get active are gardening, yoga, or a brisk walk around the block. Ask your doctor about which activities are best for you and if there are any you should avoid.
- Manage your weight and blood sugarthis can be done with diet and exercise! Meet with a dietitian to create an eating plan that works for you and your kidneys or check out these resources to help you manage your blood sugar.
Heart Failure With Preserved Ejection Fraction In Patients With Ckd
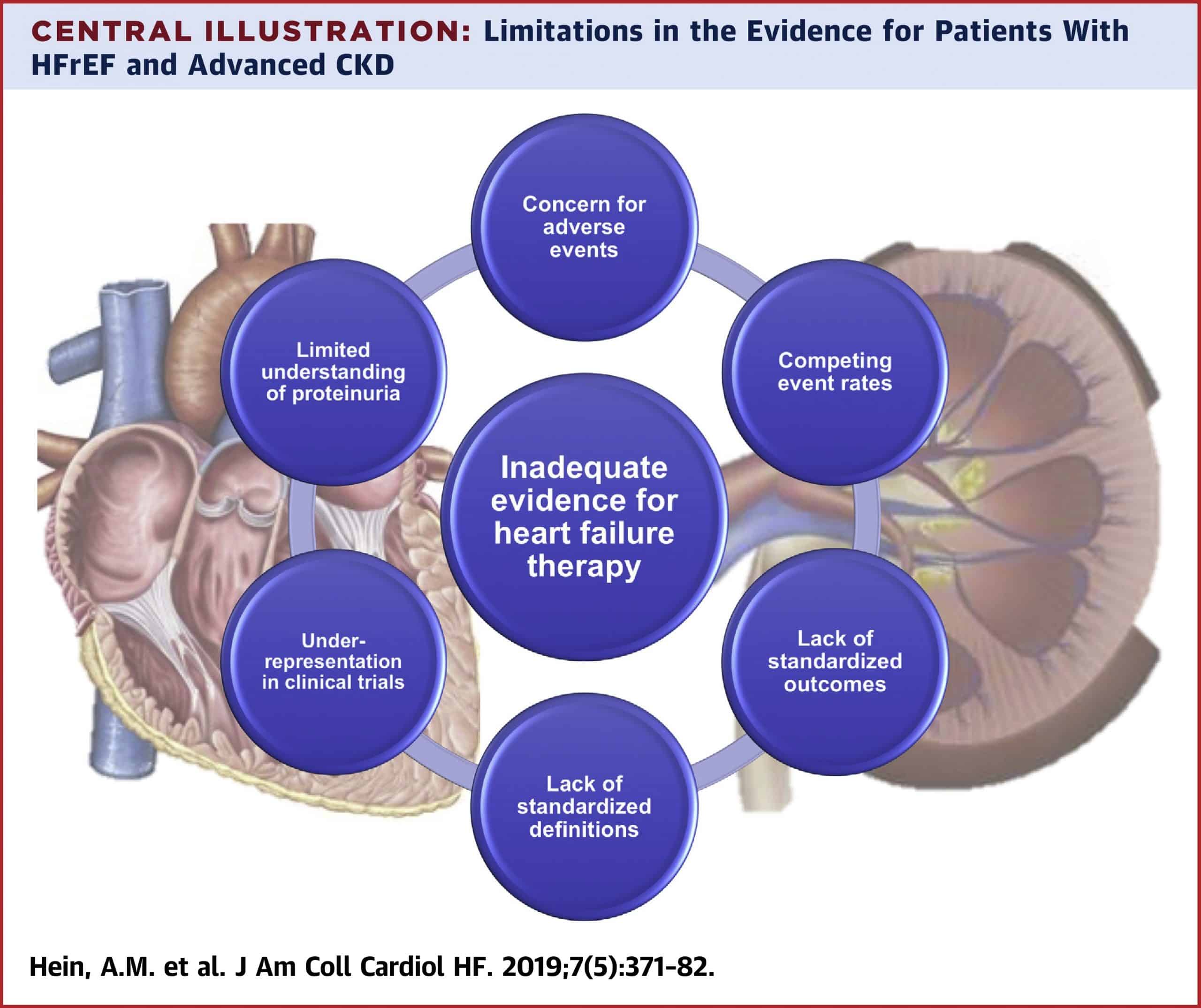
The diagnosis of HFpEF in patients with CKD may be challenging. The BNP levels may be elevated because of the CKD and may not be diagnostic. The fluid overload may be a result of CKD itself. These patients have similar risk of poor outcomes and suffer frequent hospital admissions because of fluid overload, similar to patients with heart failure with reduced ejection function . Careful use of diuretics is necessary to control the symptoms of volume overload. Nonsteroidal anti-inflammatory drugs should be avoided because they can cause AKI and fluid retention in patients with CKD, and mimic HFpEF. There is no compelling evidence for effective therapy in HFpEF to improve outcomes such as cardiovascular mortality or heart failure hospitalizations. However, large trials are underway, such as FINEARTS-HF , a randomized controlled trial of finerenone in patients with CKD and HFpEF.
Read Also: How To Calculate Resting Heart Rate
Correlation Between Bnp And Nt
Cardiac biomarkers, such as BNP and NT-proBNP, are commonly used to diagnose CHF . Pre-proBNP is synthesized in cardiac myocytes in response to ventricular wall stress and stretch, associated with greater cardiac filling pressure . After the removal of a signal peptide in the cytosol, proBNP is released as either NT-proBNP or BNP from myocytes into the circulation . NT-proBNP is the inactive form, while BNP is the active one. NT-proBNP is also more stable than BNP, having a longer half-life . Previous studies have demonstrated the correlations between increases in the plasma concentrations of BNP or NT-proBNP and reductions in the estimated glomerular filtration rate or advances in chronic kidney disease stage, which at least in part is likely to be because the principal route of clearance of NT-proBNP is renal . Furthermore, the observed correlation with eGFR was more marked for NT-proBNP than for BNP, and the ratio of NT-proBNP/BNP increased with advancing CKD stage . A high NT-proBNP concentration has been shown to predict morbidity and mortality, and its concentration in patients undergoing CAPD is lower than those undergoing HD . Additionally, NT-proBNP is a significant predictor of cardiovascular congestion, mortality, and adverse cardiovascular outcomes in PD patients .
What Is Heart Disease
Heart disease includes any heart or blood vessel problem that keeps your heart from pumping blood as well as it should. It is also called cardiovascular disease .
Heart disease can include:
- Pain, numbness, weakness or coldness in your legs or arms
- Pain in your neck, jaw, throat, upper belly area or back
- Swelling of your legs, ankles and feet
- Irregular heartbeats that feel fast, pounding or fluttering
- Feeling dizzy or lightheaded or fainting
Tell your doctor if you feel symptoms because heart disease is easier to treat when it is caught early.
Don’t Miss: How To Lower Heart Rate During Exercise
What Are The Tests For Kidney Disease
Tests for kidney disease include a blood test and a urine test. Both tests can be done in your doctors office or at a commercial facility.
- The blood test checks your GFR, which tells how well your kidneys are filtering. GFR stands for glomerular filtration rate.
- The urine test checks for albumin in your urine. Albumin is a protein that can pass into the urine when the kidneys are damaged.
If these tests show you have kidney disease, you may need to repeat these tests on a regular basis. More information is provided in the NIDDK health topic, Testing for Kidney Disease.
Study Population And Design
The study is a cross-sectional, observational study of patients in the two largest dialysis centres in the capital region of Denmark . The Danish healthcare system is publicly funded and provides universal healthcare free of charge, including dialysis service to all citizens. Nearly all Danish hospitals are public. All patients 18years of age who underwent maintenance haemodialysis from January through April 2014 were eligible and asked to participate. Demographics and medical history were obtained through interviews and supplemented by reviews of medical records including echocardiographic reports ).
You May Like: Does Resting Heart Rate Increase With Age
What Is Stage 4 Heart Failure
Stage 4 of Congestive Heart Failure Stage four of congestive heart failure produces severe symptoms such as rapid breathing, chest pain, skin that appears blue, or fainting. These symptoms may occur whether you are exercising or at rest. In this stage, your doctor will discuss if surgery is beneficial.
Can The Heart Repair Itself After Congestive Heart Failure
But the heart does have some ability to make new muscle and possibly repair itself. The rate of regeneration is so slow, though, that it can’t fix the kind of damage caused by a heart attack. That’s why the rapid healing that follows a heart attack creates scar tissue in place of working muscle tissue.
Also Check: How Does Atropine Increase Heart Rate
What Should I Ask My Doctor About Kidney Disease And Heart Disease
Some questions to ask your doctor include
- What is my blood pressure? What should it be?
- How often should I have my blood pressure checked?
- Should I be taking medicines to control my blood pressure?
- Should I be on a special diet?
- What are my cholesterol numbers? What should they be?
- How much exercise should I be getting?
- Where can I get help to quit smoking?
Population Characteristics And History Of Structural Heart Disease
Informed consent was obtained from 252 of 372 adult patients who received maintenance haemodialysis treatment at the two participating centres. Five patients had to be excluded due to inadequate image quality. In total, 247 echocardiograms were analysed. Patients were 66 years of age and predominantly male . Characteristics of included patients are presented in Table . Demographic characteristics were available for all patients. Diabetic nephropathy was more frequent among the included patients , otherwise there were no statistically significant differences in demographic or haemodynamic parameters between included and non-included patients. According to medical records, 38 patients had a previous history of heart failure and 26 of valve disease.
Table 1 Patient characteristics
You May Like: How To Help Heart Palpitations
What Does The Heart Do
The heart is a muscle that pumps blood filled with oxygen to all parts of your body. This job keeps every cell, organ, and system alive within your body. To move blood to each part of your body, your heart relies on your blood vessels. Together, the heart, blood and blood vessels make up a system called the cardiovascular system. Think of it as a delivery system. The delivery system moves blood from the heart carrying oxygen and nutrients throughout your body and also picks up waste products so that your body can get rid of them.
Heart Failure Pd Prescriptions
Sodium removal is key to success for most HF regimes and these are best facilitated by chronic CAPD rather than APD with glucose-based solutions, because sodium removal is hindered by early sodium sieving and short dwell times in APD . In APD, this effect is almost completely abrogated by the use of icodextrin which does not cause sodium sieving because it achieves UF mainly via small pores and not aquaporin channels with UF maintained long into the dwell cycle. Thus, a number of studies have made use of icodextrin in HF prescriptions , sometimes exceeding the licensed maximum doses with no apparent adverse events . Whilst some studies have suggested a high number of technical complications of this therapy , this is not our experience, and the incidence of peritonitis and catheter dysfunction in treating patients with HF appears no different to that of the general PD population.
Recommended Reading: How To Cause A Heart Attack Naturally
Eating Diet And Nutrition
A healthy diet can help protect you from heart disease and kidney disease. Keep your heart and kidneys healthy by eating plenty of the following foods:
- fruits and vegetables
- unsaturated fats such as olive oil or corn oil
- low-sodium foods
People with advanced chronic kidney disease may need to adjust their diet to avoid high potassium. If you have advanced kidney disease, you may need to limit foods such as bananas, oranges, potatoes, and tomatoes and eat apples, berries, grapes, and peaches instead. Check with your provider to find out if you should cut back on your potassium. Do not alter your diet without checking because you might eat less of these healthy fruits and vegetables unnecessarily.
More information is provided in the NIDDK health topic, Potassium: Tips for People with Chronic Kidney Disease.
You need protein. However, protein breaks down into wastes that your kidneys need to remove. Most people eat more protein than they need. Large amounts of protein make your kidneys work harder. High-quality proteins such as meat, fish, and eggs make fewer wastes than other sources of protein. Beans, whole grains, soy products, nuts and nut butters, and dairy products can also be good sources of protein.
More information is provided in the NIDDK health topic, Protein: Tips for People with Chronic Kidney Disease.
More information is provided in the NIDDK health topic, Phosphorous: Tips for People with Chronic Kidney Disease.
What Causes Heart Disease
Diabetes and high blood pressure, the most common causes of CKD, also cause heart disease.
Diabetes is a lifelong disease where too much sugar stays in your blood because your body cannot make or use insulin, the hormone that turns blood sugar into energy. High blood sugar can damage blood vessels in the kidneys and the heart.
High blood pressure is a condition where the force of blood in your blood vessels is too strong, which can damage your heart and the blood vessel walls. If your kidneys do not work well, your hormone system makes the heart pump harder to increase the blood supply to your kidneys. This raises your blood pressure.
Other health problems that can happen with CKD and cause heart disease include:
- High homocysteine levels, which is a protein that builds up in your blood if damaged kidneys cannot remove it this can damage blood vessels or lead to a heart attack
- Unbalanced calcium and phosphorous levels
Talk to your doctor about being tested for diabetes, high blood pressure and problems that can happen with CKD.
Also Check: Congestive Heart Failure Occurs When
The Surprising Link Between Chronic Kidney Disease Diabetes And Heart Disease
Getting active is one of the best ways to help you prevent or manage CKD, diabetes, and heart disease.
Find out how these chronic conditions are connected and how to prevent or manage all three.
The body is complicated! While organs in your body each have a specific job to do to keep you healthy, they still rely on each other to function well. When one organ isnt working the way it should, it can put stress on other organs, causing them to stop working properly as well.
The relationship between chronic kidney disease , diabetes, and heart disease is one example of the ways our organs are connected.
The body uses a hormone called insulin to get blood sugar into the bodys cells to be used as energy. If someone has diabetes, their pancreas either doesnt make enough insulin or cant use the insulin it makes as well as it should.
If someone has CKD, their kidneys are not able to filter out toxins and waste from their blood as well as they should.
Heart disease refers to several types of heart conditions. The most common condition, coronary artery disease, leads to changes in blood flow to the heart, which can cause a heart attack.
Benefits Of Pd Over Diuretics
The benefits of PD compared to diuretics may be related to the relative lack of neurohumoral activation. Specifically, PD does not seem to activate the sympathetic nervous system, renin-angiotensin-aldosterone, endothelin, and vasopressin systems often seen after intravascular volume depletion seen with diuretics , and may even result in better preservation of residual renal function . There is also speculation that other harmful mediators may also be removed .
You May Like: Open Heart Surgery Complications
How Long Can 90 Year Old Live With Congestive Heart Failure
Although there have been recent improvements in congestive heart failure treatment, researchers say the prognosis for people with the disease is still bleak, with about 50% having an average life expectancy of less than five years. For those with advanced forms of heart failure, nearly 90% die within one year.
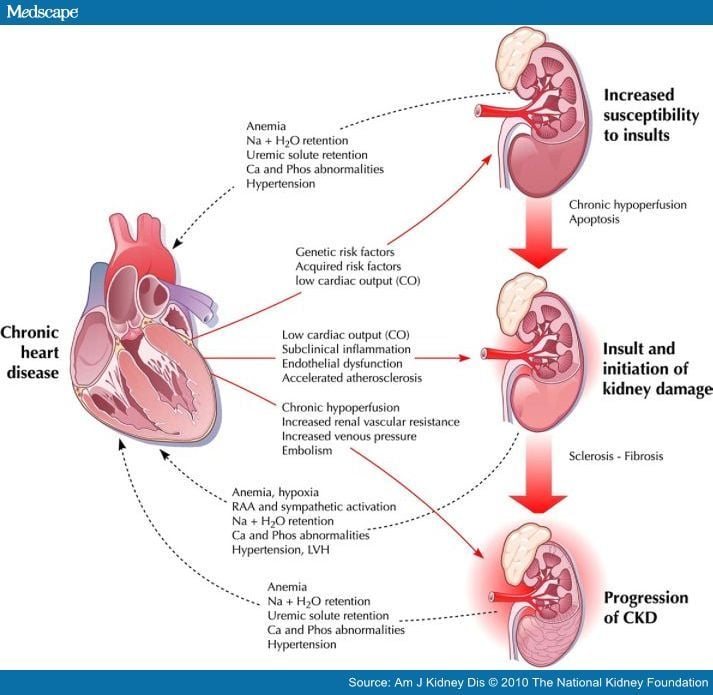
Heart Disease And Chronic Kidney Disease
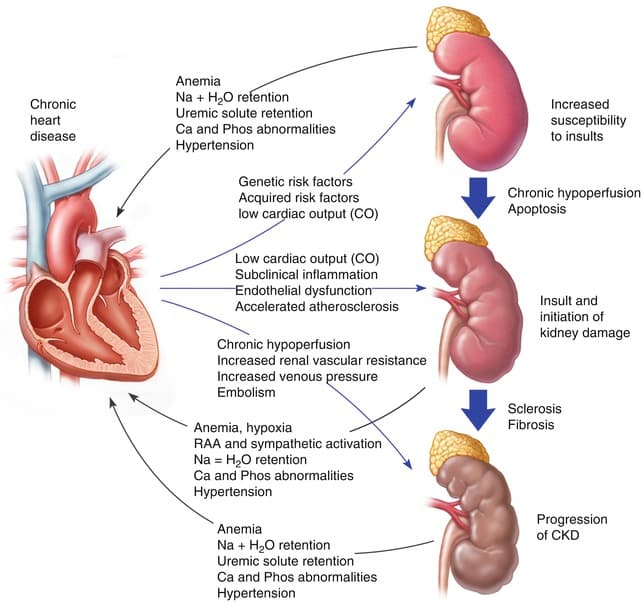
Having chronic kidney disease means you are more likely to get heart disease. CKD can cause heart disease, and heart disease can cause CKD. In fact, heart disease is the most common cause of death among people on dialysis.
The best way to prevent heart disease is to prevent or treat the problems that can cause it, such as diabetes, high blood pressure and anemia.
Recommended Reading: Can Lung Cancer Cause Heart Attack
Echocardiographic Findings In Relation To Cause Of Chronic Kidney Disease
To explore any differences between different causes of ESKD, we compared patients with an aetiology of hypertension, diabetes, glomerulonephritis and polycystic kidney disease . Left atrial volume was significantly larger in patients with hypertensive nephropathy compared to the other groups. We found no difference in the number of patients with LVEF< 50%, LVEF40%, or valve disease between groups.
Table 3 Echocardiographic findings by cause of kidney disease
