Is Ed Common After Getting A Heart Stent
Yes, ED is common in men being treated with stents in their heart arteries for advanced heart blockages, Kahn said.
Sometimes ED is an earlier sign of heart disease
In fact, if you ask men about ED at the time of their stent placement, Kahn says youll often learn that theyve had sexual performance concerns for years and that these werent recognized as risk factors for heart disease. This means that the opportunity for earlier diagnosis was lost.
Kahn says men who are getting stents often have:
- high cholesterol
- low physical activity
This leads to heart disease and ED. The risk factors are identical, he said.
Other reasons for experiencing ED after having a heart stent put in place include medications and depression.
Medications after stent placement can cause ED
Some people take beta-blockers for continued treatment after getting a heart stent. A common side effect from these medications is sexual dysfunction due to changes in blood pressure and heart rate.
ED from beta-blockers can be reversible when the medication is stopped.
Depression and antidepressants can affect sex drive
Many people who have had a heart bypass or heart stent placed depression. Depression is associated with a low libido, or sex drive. Antidepressant medications can also lead to ED.
Your Heart Failure To
Eat a healthy diet. Limit the salt you eat to less than 1,500 milligrams each day. Eat foods high in fiber and potassium. Cut back on things high in saturated fat, cholesterol, and sugar. If you need to drop some weight, reduce the number of calories you eat.
Exercise regularly. A regular program that’s OK’d by your doctor will improve your symptoms and strength and make you feel better. It may also slow your heart failure.
Don’t overdo it. Plan out your activities and include rest periods during the day.
Prevent lung infections. Ask your doctor about flu and pneumonia vaccines.
Take your medications as prescribed. Don’t stop taking them without first asking your doctor. Even if you have no symptoms, the drugs help your heart pump better.
Get emotional or psychological support, if you need it. Don’t face things alone. Get the backing you need from social workers, psychologists, clergy, and support groups. Ask your doctor to point you in the right direction.
How Do I Take Care Of Myself And Manage Side Effects
Theres a lot you can do at home to take care of yourself. Below are some general tips for managing common side effects of heart failure medications. Your healthcare provider will give you specific advice tailored to your medications and overall health.
- Check your blood pressure on a regular basis. Ask your provider to recommend a reliable home blood pressure monitor.
- Check your blood sugar levels if you have diabetes.
- Check your pulse on a regular basis.
- Dont stand up too quickly after youve been sitting or lying down. Some medications can make you feel dizzy, especially when you suddenly change your body position.
- Weigh yourselfat the same time every day, and keep a log of your daily weight. If you gain more than four pounds, call your provider.
Your medications play a big role in helping you take care of yourself. But healthy lifestyle changes are also important. Things you can do include:
- Avoid smoking and tobacco use.
- Go to cardiac rehab.
Taking care of your mental health is also important. People with heart disease, including heart failure, often feel sad or depressed. Youre managing a lot of emotions and dealing with changes to your usual routine. Ask your provider about resources that can help you cope. Your provider may recommend:
- Conversations with a social worker.
- Online resources.
- Support groups where you can meet people whore also living with heart failure.
Also Check: Does Fitbit Inspire Track Heart Rate
What Makes Yale Medicines Approach To Treating Congestive Heart Failure Unique
Yale Medicines team comprises heart failure cardiologists and cardiac surgeons, dedicated advanced-practice, registered nurses and nurse coordinators, dietitians, exercise physiologists, financial counselors, immunologists specializing in transplants, psychologists, and specialists in palliative care.
With a multidisciplinary approach, Yale Medicine physicians include the patients desires as well as input from the family to develop a comprehensive treatment plan that’s right for them.
Surgery And Medical Device Options
The goal of surgery is to make your heart work better.
. Routes blood around a blocked artery. Learn more about heart bypass surgery.
Cardiac resynchronization therapy . When your heartbeat is off-kilter, it can make heart failure worse. This treatment uses a pacemaker that sends timed electrical impulses to both of your heart’s lower chambers so they pump better and more in sync. Your doctor may call it a biventricular pacemaker. They could also pair it with an ICD . Read more on CRT, also called biventricular pacing, for heart failure.
Heart transplant. This is done when heart failure is so severe that it doesn’t respond to any other treatments. Get more information on heart transplant for heart failure.
Heart valve surgery. If a faulty heart valve causes your heart failure, your doctor may recommend repairing or replacing it. A surgeon can repair or replace the valves. Find out more on heart valve disease.
Implantable cardioverter-defibrillator . This device is similar to a pacemaker. It’s put under your skin in your chest. Wires lead through your veins and into your heart to keep track of your heart rhythm. If your heart starts to beat at a dangerous rhythm, or if it stops, the ICD tries to pace your heart or shock it back into normal rhythm. An ICD can also act as a pacemaker and speed your heart up if it’s going too slow. Learn more about ICDs for heart failure.
Don’t Miss: Can Iron Supplements Cause Heart Palpitations
Other Drugs For Heart Failure
Many people with heart disease take either aspirin or clopidogrel . These drugs help prevent blood clots from forming in your arteries. This can lower your risk of a stroke or heart attack.
Coumadin is recommended for people with heart failure who have a higher risk for blood clots. You will need to have extra blood tests to make sure your dose is correct. You may also need to make changes to your diet.
Drugs used less commonly for heart failure include:
- Digoxin to help increase the heart’s pumping strength and slow the heart rate.
- Hydralazine and nitrates to open up arteries and help the heart muscle pump better. These drugs are mainly used by people who are unable to tolerate ACE inhibitors and angiotensin receptor blockers.
- Calcium channel blockers to control blood pressure or angina from coronary artery disease .
Statins and other cholesterol-lowering drugs are used when needed.
Antiarrhythmic medicines are sometimes used by heart failure people who have abnormal heart rhythms. One such drug is amiodarone.
Another medicine, Ivabradine , acts to lower the heart rate and may help people with heart failure by reducing the heart’s workload.
Epidemiology Of Congestive Heart Failure And Evolution Of Treatment
Congestive heart failure continues to be a major health problem. Despite significant advances in the prevention and treatment of cardiovascular diseases, the incidence and prevalence of congestive heart failure have been increasing in recent years. Contributing factors include increased survival in patients with coronary artery disease , an aging population and significant advances in the control of other potentially lethal diseases.
In the past two decades, the treatment of congestive heart failure has evolved and is now directed at the attenuation of neurohormonal activation using angiotensin-converting enzyme inhibitors, beta blockers7 and, more recently, spironolactone .8 Because neurohormonal antagonists have been shown to prolong survival in patients with congestive heart failure,8â11 the role of digoxin has become less certain.
Recommended Reading: Can You Die From Congestive Heart Failure
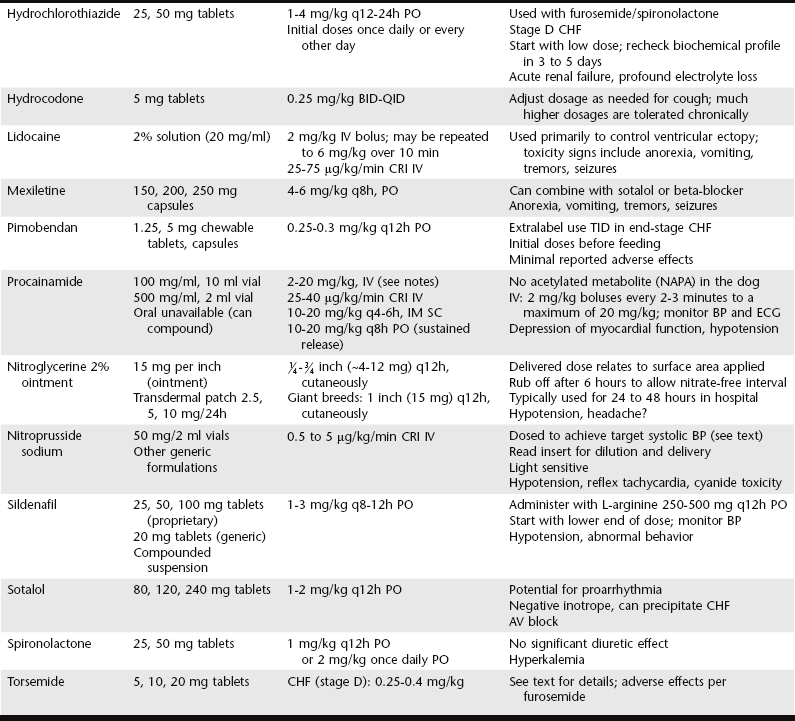
Common Heart Failure Medications
Your doctor has more choices to make within each class of heart failure medicine. Finding the right one for you may involve some trial and error.
Here are 10 drugs commonly prescribed for heart failure:
Carvedilol is a beta blocker. The usual dose for the regular tablet is twice daily. You take the controlled-release capsule once daily in the morning. You should take both with food.
Enalapril is an ACE inhibitor. At low doses, you might take it once daily. Your doctor may recommend splitting higher doses to twice a day.
Furosemide is a diuretic. You usually take it once daily. However, your doctor may have you take it only on certain days of the week to treat edema. Taking diuretics in the morning allows you to pass the extra fluids throughout the day. This minimizes sleep interruptions to urinate.
Lisinopril is an ACE inhibitor. It is also a drug you usually take once a day.
Losartan is an ARB. In most cases, the dose is once a day.
Metoprolol is a beta blocker. It comes in both an immediate-release and an extended-release form. Taking metoprolol helps lower the risk of repeat heart attacks in those who have already experienced one.
Ramipril is another ACE inhibitor. For heart failure, the usual dose is twice daily.
Spironolactone is an aldosterone antagonist. The usual dose for heart failure is once daily, preferably in the morning. Do not use salt substitutes containing potassium. They could cause your potassium level to be dangerously high on this drug.
Older Heart Failure Patients Are Often Prescribed 10 Or More Medications
Research published in Circulation: Heart Failure, an AHA journal, in 2020 revealed an alarming statistic: more than half of older patients hospitalized for CHF are discharged with 10 or more prescriptions. Most of these are not medications to treat heart failure or other cardiovascular conditions.
Such “excessive polypharmacy,” which is defined by a BMJ Open article as “concurrent use of 10 or more different drugs,” brings with it serious risks. In the AHA press release about the 2020 research, Dr. Parag Goyal, the senior study author and a geriatric cardiologist, states, “High medication burden, also known as polypharmacy, is commonly associated with adverse events and reactions. As the treatment options for various conditions including heart failure expand and the population ages, it is becoming increasingly important to weigh the risks and possible benefits of multiple medications.”
In a 2021 blog post, we explored pharmacy in the elderly, highlighting the reasons why polypharmacy is so much more prevalent in older adults and dangers associated with these contributing factors. You can access the post here.
Also Check: What Can You Do To Lower Your Heart Rate
Water Pills Or Diuretics
Diuretics help your body get rid of extra fluid. Some types of diuretics may also help in other ways. These drugs are often called “water pills.” There are many brands of diuretics. Some are taken once a day. Others are taken 2 times a day. The most common types are:
- Thiazides. Chlorothiazide , chlorthalidone , indapamide , hydrochlorothiazide , and metolazone
- Loop diuretics. Bumetanide , furosemide , and torasemide
- Potassium-sparing agents. Amiloride , spironolactone , and triamterene
When you take these medicines, you will need regular blood tests to check how well your kidneys are working and measure your potassium levels.
Ace Inhibitors And Arbs
ACE inhibitors and ARBs work by opening blood vessels and lowering blood pressure. These medicines can:
- Reduce the work your heart has to do
- Help your heart muscle pump better
- Keep your heart failure from getting worse
Common side effects of these drugs include:
When you take these medicines, you will need to have blood tests to check how well your kidneys are working and to measure your potassium levels.
Most of the time, your provider will prescribe either an ACE inhibitor or an ARB.
Also Check: What Is A Dangerous Heart Rate For A Woman
Causes Of Heart Failure
The heart is a double pump made up of four chambers. Deoxygenated blood from the veins enters the right upper chamber , is passed to the right lower chamber , and then pumped to the lungs.
Oxygenated blood from the lungs enters the left upper chamber and then enters the left lower chamber . The blood is then pumped around the body, under pressure, via arteries.
In a person with heart failure, one or both ventricles dont empty properly. This leads to increased pressure in the atria and the nearby veins. This backlog of blood can affect the kidneys and lungs interfering with their function and leading to a build-up of fluid in the lungs, abdominal organs and legs.
In some people with heart failure, rather than failed pumping of the blood from the ventricle, there is failed relaxation of the ventricle.
If the heart is not pumping and becomes stiff and unable to relax, it can cause the blood to pool in the hearts ventricles. This can cause pressure build up and can put strain on the heart.
Heart failure can be caused by several conditions, including:
Medicines For Heart Failure
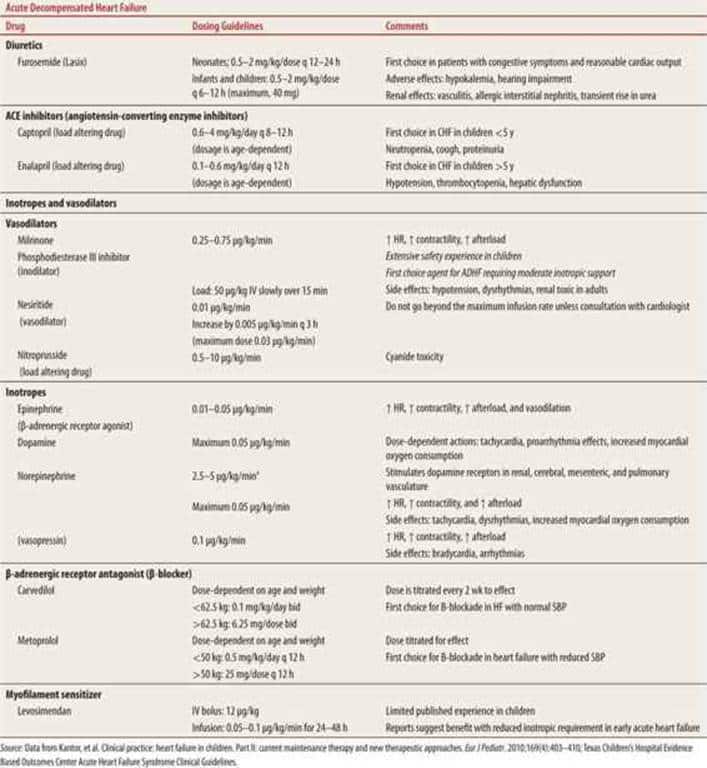
Most people with heart failure are treated with medication. Often you’ll need to take 2 or 3 different medicines.
Some of the main medicines for heart failure include:
- SGLT2 inhibitors
You may need to try a few different medicines before you find a combination that controls your symptoms but doesn’t cause unpleasant side effects.
You May Like: What Are Signs Of A Heart Attack In A Man
Activities That Are Good For Ed And Your Heart
- Eat a heart-healthy diet with an emphasis on fruits, vegetables, whole grains, healthy fats, and lean protein.
- Get regular exercise that includes cardiovascular activities, resistance training, and mindfulness-based exercise like yoga.
- Reduce or eliminate alcohol use.
- If you smoke or use other substances, consider quitting. Support is available. A doctor can help you outline a plan.
- If needed, lose weight or manage your current weight.
The American Urological Association recommends a referral to a mental health professional to help you:
- bridge the gap between treatment and your sexual relationships
- promote continuing your treatments
- reduce performance anxiety
The focus of counseling sessions will be helping you reduce anxiety about sexual situations and improving communication between you and your sexual partner about any sexual concerns.
You can also discuss ways to include ED treatments in your sex life.
for ED. The most common are sildenafil and tadalafil . Others include vardenafil HCL and avanafil .
These four PDE5 inhibitors are the only oral medications by the Food and Drug Administration to treat ED.
Kahn says that after lifestyle modifications, PDE5 inhibitors are the second approach to ED treatment.
They are generally safe to use in stable heart patients not taking nitroglycerin medication, if the extent of their heart disease is known and if they have at least average fitness and stability, he said.
Prognosis Of Dogs With Congestive Heart Failure
The development of heart failure represents a specific measurable point in the development of heart disease. For DMVD, the average survival of dogs with CHF is 9 months.5 However, within survival times in this group vary widely, with some patients living over 3 years.5 Survival in dogs with DCM is similar.16
Parameters that can help stratify risk by suggesting poorer prognosis include large left atrial and left ventricular size and high mitral E wave velocity.
When owners are questioned, it is evident that most would trade some longevity for improved quality of life. With a logical approach, heart failure can be controlled for many months with a good quality of life in most dogs.
Read Also: What Time Of Day Are Heart Attacks Most Common
What Are The Types Of Heart Failure
Systolic dysfunction happens when the heart muscle doesn’t contract with enough force, so there is less oxygen-rich blood pumped throughout the body.
Diastolic dysfunction happens when the heart contracts normally, but the ventricles donât relax properly or are stiff, and less blood enters the heart during normal filling.
A calculation done during an echocardiogram, called the ejection fraction , is used to measure how well your heart pumps with each beat to help determine if systolic or diastolic dysfunction is present. Your doctor can discuss which condition you have.
Medication Reconciliation Is Vital For Congestive Heart Failure Patients
Considering the sheer number of medications likely to be prescribed to patients with CHF a figure that will typically increase as the patient ages medication reconciliation takes on an elevated importance in the care of CHF patients. Med rec, one of the core components of medication management, should play an ongoing role in helping ensure patients are consistently taking the right medications at the right times for their specific and evolving health issues.
Furthermore, every hospitalized patient, including those with CHF, should receive medication reconciliation post-discharge . Why? As Cureatr Chief Executive Officer Richard Resnick states, “The discharge from the hospital to the home is one of the most dangerous care transitions for all patients, but particularly for those with complex medication regimens” such as most CHF patients. The Centers for Medicare & Medicaid Services, he notes, has set the target for completed MRPs at 80%, but it really should occur 100% of the time as research has revealed that more than half of all discharges have at least one medication error.
You May Like: How To Figure Out Your Heart Rate
Congestive Heart Failure: Prevention Treatment And Research
Congestive heart failure is a serious condition in which the heart doesnt pump blood as efficiently as it should. Despite its name, heart failure doesnt mean that the heart has literally failed or is about to stop working. Rather, it means that the heart muscle has become less able to contract over time or has a mechanical problem that limits its ability to fill with blood. As a result, it cant keep up with the bodys demand, and blood returns to the heart faster than it can be pumped outit becomes congested, or backed up. This pumping problem means that not enough oxygen-rich blood can get to the bodys other organs.
The body tries to compensate in different ways. The heart beats faster to take less time for refilling after it contractsbut over the long run, less blood circulates, and the extra effort can cause heart palpitations. The heart also enlarges a bit to make room for the blood. The lungs fill with fluid, causing shortness of breath. The kidneys, when they dont receive enough blood, begin to retain water and sodium, which can lead to kidney failure. With or without treatment, heart failure is often and typically progressive, meaning it gradually gets worse.
More than 5 million people in the United States have congestive heart failure. Its the most common diagnosis in hospitalized patients over age 65. One in nine deaths has heart failure as a contributing cause.
