How Is Heart Failure Treated
Your treatment will depend on the type of heart failure you have and, in part, what caused it. Medications and lifestyle behaviors are part of every treatment plan. Your healthcare provider will talk to you about the best treatment plan for you. Treatment is the same, regardless of gender.
As heart failure gets worse, your heart muscle pumps less blood to your organs, and you move toward the next stage of heart failure. Since you cant move backward through the heart failure stages, the goal of treatment is to keep you from moving forward through the stages or to slow down the progression of your heart failure.
Stage A treatment
The usual treatment plan for people with Stage A heart failure includes:
- Regular exercise, being active, walking every day.
- Stopping the use of tobacco products.
- Treatment for high blood pressure .
- Treatment for high cholesterol.
- Not drinking alcohol or using recreational drugs.
- Angiotensin-converting enzyme inhibitor or an angiotensin II receptor blocker if you have coronary artery disease, diabetes, high blood pressure, or other vascular or cardiac conditions.
- Beta-blocker if you have high blood pressure.
Stage B treatment
The usual treatment plan for people with Stage B heart failure includes:
Stage C treatment
The usual treatment plan for people with Stage C HF-rEF includes:
If the treatment causes your symptoms to get better or stop, you still need to continue treatment to slow the progression to Stage D.
Stage D treatment
What Kind Of Diet That Is Healthy For Your Heart
Eat foods that are low in saturated fat, trans fat, sodium, and cholesterol. These nutrients tend to raise blood pressure and increase the risk of blood clots, both which can be detrimental to heart health.
The DASH diet published by the American Heart Association for managing blood pressure recommends plenty of fruits, vegetables, whole-grains, nut and legumes, low-fat dairy products, skinless chicken and fish, and vegetable oils. Red meats and sweetened foods and beverages should be limited.
Epidemiology Of Congestive Heart Failure And Evolution Of Treatment
Congestive heart failure continues to be a major health problem. Despite significant advances in the prevention and treatment of cardiovascular diseases, the incidence and prevalence of congestive heart failure have been increasing in recent years. Contributing factors include increased survival in patients with coronary artery disease , an aging population and significant advances in the control of other potentially lethal diseases.
In the past two decades, the treatment of congestive heart failure has evolved and is now directed at the attenuation of neurohormonal activation using angiotensin-converting enzyme inhibitors, beta blockers7 and, more recently, spironolactone .8 Because neurohormonal antagonists have been shown to prolong survival in patients with congestive heart failure,8â11 the role of digoxin has become less certain.
Recommended Reading: How Is A Heart Attack Treated
What Is The Importance Of Ejection Fraction
Your ejection fraction is one way to measure the severity of your condition. If its below normal, it can mean that you have heart failure. Your ejection fraction tells your healthcare provider how good of a job your left or right ventricle is doing at pumping blood. Usually, your EF number is talking about how much blood your left ventricle is pumping out because its your heart’s main pumping chamber.
Several non-invasive tests can measure your EF. With this information, your healthcare provider can decide how to treat you or find out if a treatment is working as it should.
A normal left ventricular ejection fraction is 53% to 70%. An LVEF of 65%, for example, means that 65% of the total amount of blood in your left ventricle is pumped out with each heartbeat. Your EF can go up and down, based on your heart condition and how well your treatment works.
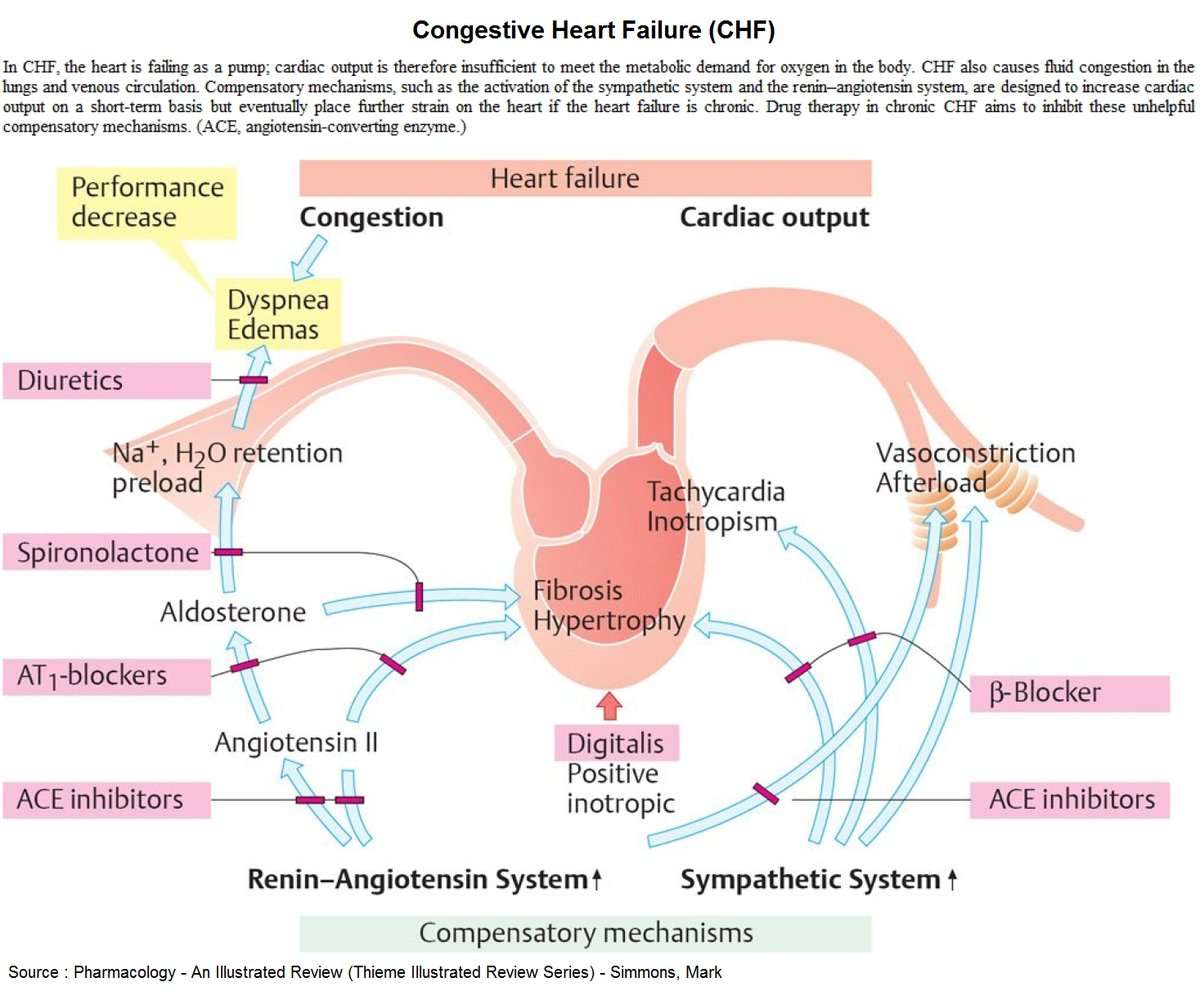
Pharmacological Management Of Heart Failure
Drugs used in heart failure include those used to initially manage mild to moderate failure and those used more commonly in severe to very severe conditions.
First Agents Used:
Selection of agents and their combinations depend on initial clinical state and on patient responsiveness to initial therapy
Additional Agents:
Selection of agents and their combinations depend on initial clinical state and on patient responsiveness to initial therapy.
An implantable cardioverter-defibrillator is indicated for primary prevention of sudden cardiac death in patients with HF who have an LVEF of less than or equal to 35%.
You May Like: Causes Of Systolic Heart Failure
Is There A Treatment For Heart Failure
There are more treatment options available for heart failure than ever before. Tight control over your medications and lifestyle, coupled with careful monitoring, are the first steps. As the condition progresses, doctors specializing in the treatment of heart failure can offer more advanced treatment options.
The goals of treating heart failure are to try to keep it from getting worse , to ease symptoms, and to improve quality of life.
Some common types of medicines used to treat it are:
- ACE inhibitors
- Aldosterone antagonists
- ARBs
- ARNIs
- Selective sinus node inhibitors
- Soluble guanylate cyclase stimulator
Your doctor may also recommend a program called cardiac rehabilitation to help you exercise safely and keep up a heart-healthy lifestyle. It usually includes workouts that are designed just for you, education, and tips to lower your chance of heart trouble, like quitting smoking or changing your diet.
Cardiac rehab also offers emotional support. You can meet people like you who can help you stay on track.
Can Surgery Be Used To Treat Heart Failure
In heart failure, surgery may sometimes prevent further damage to the heart and improve the heart’s function. Procedures used include:
- Coronary artery bypass grafting surgery. The most common surgery for heart failure caused by coronary artery disease is . Although surgery is more risky for people with heart failure, new strategies before, during, and after surgery have reduced the risks and improved outcomes.
- Heart valve surgery. Diseased heart valves can be treated both surgically and non-surgically .
- Implantable left ventricular assist device . The LVAD is known as the “bridge to transplantation” for patients who haven’t responded to other treatments and are hospitalized with severe systolic heart failure. This device helps your heart pump blood throughout your body. It allows you to be mobile, sometimes returning home to await a heart transplant. It may also be used as destination therapy for long-term support in patients who are not eligible for transplant.
- Heart transplant. A heart transplant is considered when heart failure is so severe that it doesn’t respond to all other therapies, but the person’s health is otherwise good.
Don’t Miss: What Is An Impending Heart Attack
What Is The Role Of Implanted Devices In Congestive Heart Failure
An ICD is an implantable cardiac defibrillator that can be life-saving. The ICD is implanted under the skin in the chest or abdomen. The device is able to monitor your heart rate 24 hours a day.
ICDs can act as pacemakers, which means that they can send electric signals to your heart when an abnormal heart rhythm is detected. This can result in a return to a normal heart rhythm. Another option is CRT implantation.
CRT is selected for patients with a normal heart rhythm but reduced left heart ejection fraction. A cardiologist will be able to determine the most suitable device.
When Should I Call An Ambulance
If you have any of the symptoms below, call triple zero immediately and ask for an ambulance. If calling triple zero does not work on your mobile phone, try calling 112.
- chest pain thats severe or worsening, or has lasted longer than 10 minutes
- chest pain that feels heavy, crushing or tight
- other symptoms, such as breathlessness, nausea, dizziness or a cold sweat
- pain in your jaw or down your left arm
Also Check: How Much Do Beta Blockers Lower Heart Rate
Anticoagulant Medications Can Reduce The Risk Of Blood Clots And Heart Attacks
A heart attack occurs when blood flow in the blood vessels of the heart is blocked. People with congestive heart failure may benefit from taking an anticoagulant medication to lower the risk of developing blood clots.
According to an article by Dr. Allison Tsao published for The American College of Cardiology, aspirin and warfarin have been proven to lower the risk of stroke and cardiac ischemia in patients with heart failure and risk factors such as diabetes, obesity, and atrial fibrillation.
Treatment Of Congestive Heart Failure
Congestive heart failure is a condition that occurs when a pets heart can no longer pump enough blood, causing fluid to back up into the lungs or the belly. The specific treatment for congestive heart failure depends on the underlying type of heart disease and its severity.
The primary goals of treating congestive heart failure are to reduce the buildup of fluid and to increase the blood being pumped by the heart to the lungs and the rest of the body. These outcomes can help to improve the quality and length of your pet’s life. A variety of medications, diets, and nutritional supplements are available to help reach these goals. To learn more about supplements and diets that may be appropriate for a pet with heart disease or congestive heart failure, please visit our Nutrition tab.
Usually once a pet has congestive heart failure, they require life-long medications. Sometimes treatment is started during a short stay in the hospital, and other times your veterinarian will feel comfortable starting treatment at home.
Medications that are commonly used to treat congestive heart failure include diuretics like furosemide and spironolactone, ACE inhibitors like enalapril, benazepril or lisinopril, and a drug called pimobendan. Pimobendan increases the strength of contraction of the heart and has been shown to prolong survival of dogs with congestive heart failure.
Read Also: What Happens To Heart Rate During Heart Attack
How Much Alcohol Can You Drink If You Have Congestive Heart Failure
Alcohol increases the risk of high blood pressure, which can exacerbate congestive heart failure. Therefore, people with congestive heart failure should drink alcohol in moderation.
The American Heart Association recommends limiting alcohol to 1 drink per day for women and 1-2 drinks per day for men.
Life Expectancy With Congestive Heart Failure
The life expectancy of someone with congestive heart failure depends on the type of heart failure, the cause, the stage of the disease, and how effective treatment is.
When heart failure results from cardiomyopathy or coronary artery disease, a person typically has a less positive outlook than someone with heart failure in its earliest stage.
You May Like: What Is A Normal Resting Heart Rate For Adults Over The Age 18
What Are The Symptoms Of Heart Failure
You may not have any symptoms of heart failure, or the symptoms may be mild to severe. Symptoms can be constant or can come and go. The symptoms can include:
- Congested lungs. Fluid backup in the lungs can cause shortness of breath with exercise or difficulty breathing at rest or when lying flat in bed. Lung congestion can also cause a dry, hacking cough or wheezing.
- Fluid and water retention. Less blood to your kidneys causes fluid and water retention, resulting in swollen ankles, legs, abdomen , and weight gain. Symptoms may cause an increased need to urinate during the night. Bloating in your stomach may cause a loss of appetite or nausea.
- Dizziness, fatigue, and weakness. Less blood to your major organs and muscles makes you feel tired and weak. Less blood to the brain can cause dizziness or confusion.
- Rapid or irregular heartbeats. The heart beats faster to pump enough blood to the body. This can cause a rapid or irregular heartbeat.
If you have heart failure, you may have one or all of these symptoms or you may have none of them. They may or may not indicate a weakened heart.
Chronic Treatment Of Congestive Heart Failure In Dogs
Chronic treatment of patients with CHF shifts from trying to control pulmonary edema to trying to negate deleterious effects of neurohormonal stimulation. The aim of chronic CHF treatment is to increase longevity of the patient, as well as improve quality of life. As a result, treatment for chronic CHF generally involves the use of 4 medications: furosemide, pimobendan, an angiotensin-converting enzyme inhibitor, and spironolactone. These drugs are usually continued indefinitely. Other drugs may also be required.
Recommended Reading: How To Tell If You Had A Heart Attack
Congestive Heart Failure Medications
Medications are in most cases the primary treatment for heart failure. Medications are used in combination to manage the effects of heart failure such as fluid retention, swelling, vasoconstriction, and increased heart rate. In more advanced cases, medications are used to maintain a normal heart rhythm or to keep heart failure patients alive before surgery or heart transplant.
What Medications Should I Avoid If I Have Heart Failure
There are several different types of medications that are best avoided in those with heart failure including:
- Nonsteroidal anti-inflammatory medications such as Motrin or Aleve. For relief of aches, pains, or fever take Tylenol instead.
- Most calcium channel blockers
- Some nutritional supplements, such as salt substitutes, and growth hormone therapies
- Antacids that contain sodium
If youâre taking any of these drugs, discuss them with your doctor.
Itâs important to know the names of your medications, what theyâre used for, and how often and at what times you take them. Keep a list of your medications and bring them with you to each of your doctor visits. Never stop taking your medications without discussing it with your doctor. Even if you have no symptoms, your medications decrease the work of your heart so that it can pump more effectively.
Don’t Miss: What Is An Elevated Heart Rate
What Foods Should Be Avoided With Congestive Heart Failure
Dietary changes are a major part of heart failure treatment, and they will require certain foods to be reduced or eliminated in the diet:
- Salt: Above all else, avoid salty foods. Sodium contributes to the swelling and fluid retention that damages the heart, lungs, and other organs in patients with heart failure.
- Alcohol: Alcohol damages the heart muscle and will worsen heart failure.
- Fats: Saturated fats and trans-unsaturated fatty acids are associated with coronary heart disease, so your cardiologist or nutritionist will reduce your intake of saturated and trans fats.
- Carbohydrate snacks: Crackers, chips, cookies, popcorn all put on the pounds without adding much nutrition to the diet. Life expectancy is significantly reduced in heart failure patients who carry excess weight.
- Water: Fluid retention is common to heart failure and damages the heart and other organs, so only drink as much water and other liquids as advised by your cardiologist or nutritionist.
Is Exercise Good For Congestive Heart Failure
Exercise will be prescribed for all but the most advanced cases of congestive heart failure, but the exertion level will vary. Exercise helps to slow adverse physical changes in the heart and, for patients in the earliest stages of heart failure, may help to remodel the heart and potentially reverse the condition.
You May Like: Congestive Heart Failure And Afib In Elderly
What Is The Outlook For People With Heart Failure
With the right care, heart failure may not stop you from doing the things you enjoy. Your prognosis or outlook for the future will depend on how well your heart muscle is functioning, your symptoms, and how well you respond to and follow your treatment plan.
Everyone with a long-term illness, such as heart failure, should discuss their desires for extended medical care with their doctor and family. An “advance directive” or “living will” is one way to let everyone know your wishes. A living will expresses your desires about the use of medical treatments to prolong your life. This document is prepared while you are fully competent in case you are unable to make these decisions at a later time.
Show Sources
Ace Inhibitors Arbs And Mras

The first-line medications for heart failure are ACE inhibitors and ARBs . The body responds to heart failure by producing angiotensin, a protein that causes blood vessels to tighten and increase blood pressure. The increased blood pressure increases the efficiency of each heartbeat but also puts more strain on the heart, causing further changes to the heart that reduce blood output. ACE inhibitors, such as lisinopril, ramipril, or enalapril, and angiotensin receptor blockers , such as valsartan, losartan, or candesartan, block angiotensin, keep blood pressure low, and therefore slow or prevent some of the cardiac remodeling that would otherwise occur with this compensatory pathway.
Mineralcorticoid receptor antagonists , such as spironolactone and eplerenone, work by blocking a hormone called aldosterone. Aldosterone causes high blood pressure which in turn can increase the strain on the left ventricle, contributing to the development of or worsening already present heart failure. Blocking aldosterone with this class of medications has demonstrated a reduction in poor outcomes in patients with heart failure.
You May Like: Does Alcohol Raise Heart Rate
