Have A Heart Failure Action Plan
A heart failure action plan provides you with instructions and information on how to manage your heart failure on a daily basis and also how to recognise and cope with worsening symptoms, such as flare-ups . You can develop your heart failure action plan with your healthcare provider and fit the plan to suit how severe your heart failure is and your wishes. At each visit with your healthcare provider, you can review the plan and make adjustments as needed.
Here’s an example of a heart failure action plan by the Heart Foundation NZ.
Atrial Natriuretic Peptide And B
ANP and BNP are endogenously generated peptides activated in response to atrial and ventricular volume/pressure expansion. ANP and BNP are released from the atria and ventricles, respectively, and both promote vasodilation and natriuresis. Their hemodynamic effects are mediated by decreases in ventricular filling pressures, owing to reductions in cardiac preload and afterload. BNP, in particular, produces selective afferent arteriolar vasodilation and inhibits sodium reabsorption in the proximal convoluted tubule. It also inhibits renin and aldosterone release and, therefore, adrenergic activation. ANP and BNP are elevated in chronic heart failure. BNP especially has potentially important diagnostic, therapeutic, and prognostic implications.
For more information, see the Medscape Drugs & Diseases article Natriuretic Peptides in Congestive Heart Failure.
How Does Pulmonary Hypertension Affect My Body
Pulmonary hypertension can cause serious problems in your body, including:
PH is dangerous for people who are pregnant. It can cause complications for both the birthing parent and fetus.
Without treatment, pulmonary hypertension can overtax your heart and eventually be fatal. High blood pressure in your pulmonary arteries forces your heart to work harder to send oxygen-poor blood to your lungs. Your right ventricle is responsible for pumping this blood to your lungs. So, over time, PH causes your right ventricle to get bigger due to the extra work. This condition can lead to right-sided heart failure.
Right-sided heart failure has a ripple effect throughout your body. It can disrupt the normal workings of many organs and systems.
Because pulmonary hypertension can affect your entire body, its essential that youre diagnosed and treated as early as possible. Your provider will prescribe treatment based on whats causing your PH. No matter the cause, untreated PH is life-threatening.
You May Like: How Accurate Is Ecg For Heart Attack
How A Heart Attack Can Cause Heart Failure
Heart attacks are the most common cause of heart failure. If you have a heart attack, one of the arteries supplying your heart muscle itself has become completely blocked, cutting off the blood supply, and blocking the supply of oxygen and nourishment to that part of your heart muscle, causing it to die.
What Are The Treatments For Heart Failure
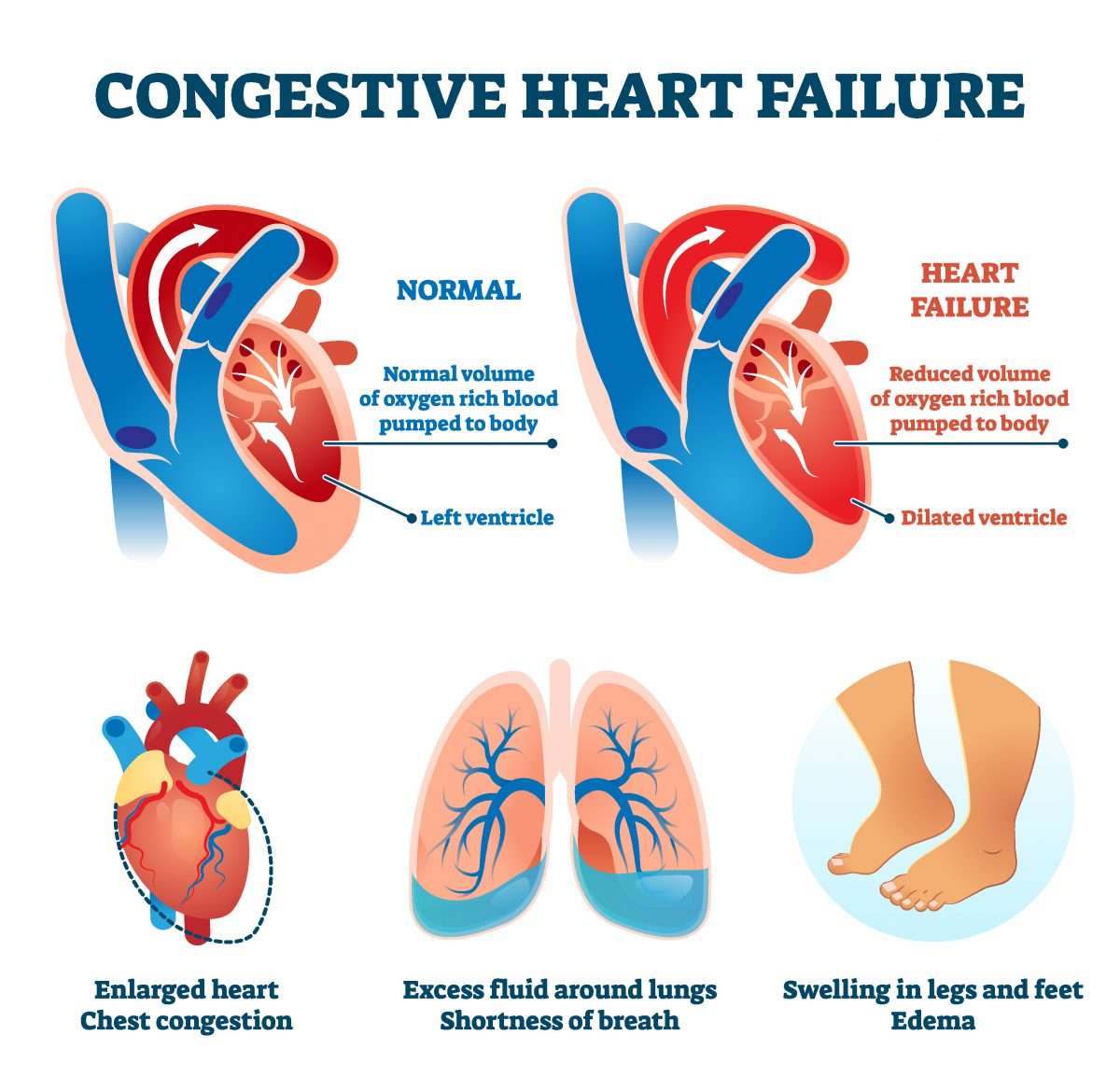
Your treatment will depend on the type of heart failure you have and how serious it is. There’s no cure for heart failure. But treatment can help you live longer with fewer symptoms.
Even with treatment, heart failure usually gets worse over time, so you’ll likely need treatment for the rest of your life.
Most treatment plans include:
You may need heart surgery if:
- You have a congenital heart defect or damage to your heart that can be fixed.
- The left side of your heart is getting weaker and putting a device in your chest could help. Devices include:
- A biventricular pacemaker .
- A mechanical heart pump or a total artificial heart).
As part of your treatment, you’ll need to pay close attention to your symptoms, because heart failure can worsen suddenly. Your provider may suggest a cardiac rehabilitation program to help you learn how to manage your condition.
Also Check: How Fast Should Your Heart Rate Be
When Should I Call My Healthcare Provider
- A fast heart rate .
- A respiratory infection or cough thats getting worse.
- Constantly feeling dizzy or lightheaded.
- Episodes of chest pain or discomfort with physical activity.
- Extreme fatigue or decreased ability to do your normal activities.
- Nausea or lack of appetite.
- Restlessness or confusion.
- Shortness of breath thats gotten worse, especially if you wake up feeling short of breath.
- Swelling in your ankles, legs or tummy thats gotten worse.
- Trouble breathing with regular activities or at rest.
How To Treat And Prevent Congestive Heart Failure
Treatment for heart failure varies depending on the severity of your condition. Adopting a healthy lifestyle tends to significantly impact treating and preventing congestive heart failure. If you form these habits early, you can lower your risk of developing heart failure in the first place. Consider the following strategies to prevent heart failure:
- Avoid smoking: People who smoke are 2-4 times more likely to develop coronary heart disease that can lead to heart failure.
- Eat healthy foods: Eating primarily fruits, vegetables, low-fat dairy, healthy fats and lean protein promotes your heart health and overall well-being.
- Stay active: Exercising regularly is great for your heart, and it helps control your weight. Maintaining a healthy weight lowers your risk of heart failure.
- Take care of yourself: Many types of heart disease can lead to heart failure. If you have an existing cardiovascular condition, monitor and manage it carefully. Take your medications as prescribed to maintain your heart health.
For most people, heart failure is a lifelong condition. Fortunately, treatment can reduce your symptoms and increase your chances of enjoying a long and healthy life. Here are some treatment options to slow the progression of congestive heart failure:
You May Like: What Happens To Heart Rate During Heart Attack
Outlook For Heart Failure
Heart failure is a serious long-term condition that will usually continue to get slowly worse over time.
It can severely limit the activities you’re able to do and is often eventually fatal.
But it’s very difficult to tell how the condition will progress on an individual basis.
It’s very unpredictable. Lots of people remain stable for many years, while in some cases it may get worse quickly.
Quality Of Patient Care
Brigham and Womens Hospital is committed to providing all of our patients with the safest, highest-quality, most-satisfying care possible and follow established protocols that have been shown to improve patient outcomes. Our quality of patient care we provide and how we are measured compared with other hospitals.
Read Also: Why Am I Getting Heart Palpitations
What Raises A Persons Risk Of Developing Pulmonary Hypertension
Risk factors for developing pulmonary hypertension include:
- Family history of blood clots.
- Family history of pulmonary hypertension.
- Living at high altitudes.
- Smoking and using tobacco products.
- Use of diet medications such as fen-phen .
- Use of some prescription medications that treat cancer and depression.
- Use of recreational drugs.
Talk with your provider about your risk factors and what you can do to lower your risk.
Heart Failure Treatment Is A Team Effort
Heart failure management is a team effort, and you are the key player on the team. Your heart doctor will prescribe your medications and manage other medical problems. Other team members — including nurses, dietitians, pharmacists, exercise specialists, and social workers — will help you achieve success. But it is up to YOU to take your medications, make dietary changes, live a healthy lifestyle, keep your follow-up appointments, and be an active member of the team.
If you notice anything unusual, don’t wait until your next appointment to discuss it with your doctor. Call them right away if you have:
- Unexplained weight gain
- Swelling in your ankles, feet, legs, or belly that gets worse
- Shortness of breath that gets worse or happens more often, especially if you wake up feeling that way
- Bloating with a loss of appetite or nausea
- Extreme fatigue or more trouble finishing your daily activities
- A lung infection or a cough that gets worse
- Fast heart rate
- New irregular heartbeat
Read Also: Women’s Heart Failure Symptoms
What Do The Results Mean
The results help your doctor or nurse determine if you have heart failure, if worsening fatigue or shortness of breath are due to heart failure or another problem or if heart failure has progressed toward end-of-life. It is important to note that this test is only one method your doctor or nurse uses to monitor your condition. Based on your results, your doctor can choose the best treatment plan for you.
A normal level of NT-proBNP, based on Cleveland Clinics Reference Range is:
- Less than 125 pg/mL for patients aged 0-74 years
- Less than 450 pg/mL for patients aged 75-99 years
If you have heart failure, the following NT-proBNP levels could mean your heart function is unstable:
- Higher than 450 pg/mL for patients under age 50
- Higher than 900 pg/mL for patients age 50 and older
Your doctor or nurse can give you more specific information about your test results. Depending on your personal health history, your normal range may differ from other patients with different backgrounds.
More information about BNP/NT-proBNP is available in the references below.
Last reviewed by a Cleveland Clinic medical professional on 04/25/2019.
References
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services.Policy
How Does Heart Failure Affect The Quality Of Life And Lifestyle
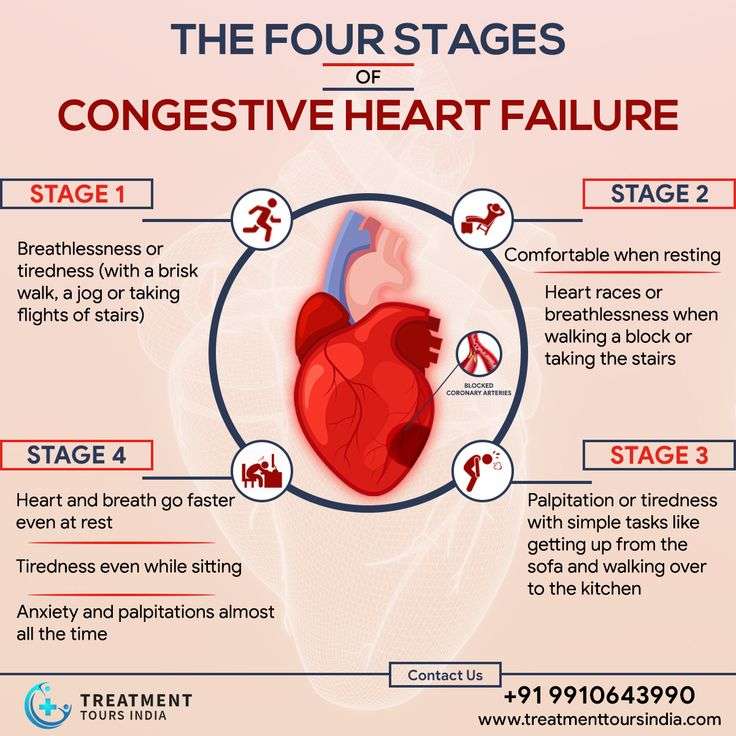
With the right care and treatment plan, many adults still enjoy life even though heart failure limits their activities. How well you feel depends on:
- How well your heart muscle is working.
- How well you respond to your treatment plan.
- How well you follow your treatment plan.
This includes caring for yourself by:
- Taking your medications.
You May Like: What Is Considered Elevated Heart Rate
Living Well With Heart Failure
The Heart Foundation has developed a range of resources for people living with heart failure, and their families and carers.
- Living well with heart failure booklet, which includes information about what to do when you feel sick, managing symptoms, and monitoring your fluid and salt intake.
- Living well with heart failure video series, which includes seven videos covering topics to help you manage your condition. The series is available in a range of languages.
- Heart failure fact sheet, which includes questions to ask your health professional and what changes you might need to make to your daily life.
- Heart failure action plan, which helps you to identify the most important parts of your heart failure management to focus on right now.
Access these resources on the Heart Foundation website.
What Are The Later Symptoms Of Pulmonary Hypertension
As PH progresses, youll feel shortness of breath even when youre not moving around. Other symptoms include:
- Bluish color on your skin or lips.
- Feeling less hungry than usual.
- Pain in the upper right side of your tummy.
- Racing heartbeat.
- Swelling in your ankles, legs or tummy.
PH symptoms make it hard for you to exercise or carry out your normal daily routine.
Also Check: Does Fever Increase Heart Rate
Stage A Treatment Options
Treatment options in stage A mainly focus on promoting your overall health and disease prevention. If you meet the stage A criteria, your doctor will recommend lifestyle changes to slow or stop disease progression.
Heart Failure Doctor Discussion Guide
How Do I Take Care Of Myself
Surviving sudden cardiac arrest is the start of a long recovery for many. Depending on how long your brain was without oxygen, youll likely have brain damage. This means you may not be able to do all the things you used to do every day. Also, you may have some mental health challenges like stress and depression.
If a rehabilitation program is available, you can use it to regain your abilities. This will take time and patience. Researchers have found that sudden cardiac arrest survivors quality of life got better after six months.
You May Like: Dementia And Heart Failure Life Expectancy
Nyha Functional Classification System
The New York Heart Association functional classification considers heart failure symptoms that happen during exercise to determine stage. Patients can go back and forth between stages depending on how well-controlled symptoms are on a given day.
- Stage 1: The person has heart disease, but it isnt yet causing symptoms or limiting activities.
- Stage 2: The person has mild symptoms that only slightly limit activity.
- Stage 3: The person has significant limitations to activities. He or she is only comfortable when resting.
- Stage 4: The person has major limitations and experiences symptoms when at rest.
Types Of Heart Failure
The main types of heart failure are named for where they occur in the heart:
- Left-sided heart failure
- Biventricular heart failure
Clinicians also may classify heart failure as:
- Acute: You have active symptoms of heart failure, with either a new diagnosis or with long-term heart failure.
- Chronic: You have a history of heart failure, but your condition is relatively stable with no symptoms or with manageable symptoms.
Also Check: What Is The Ideal Heart Rate
What Is Heart Failure
Heart failure doesnât mean the heart has stopped working. Rather, it means that the heart works less efficiently than normal. Due to various possible causes, blood moves through the heart and body at a slower rate, and pressure in the heart increases. As a result, the heart canât pump enough oxygen and nutrients to meet the body’s needs.
The chambers of the heart may respond by stretching to hold more blood to pump through the body or by becoming stiff and thickened. This helps to keep the blood moving, but the heart muscle walls may eventually weaken and become unable to pump as efficiently. The kidneys may respond by causing the body to retain fluid and salt. If fluid builds up in the arms, legs, ankles, feet, lungs, or other organs, the body becomes congested. Congestive heart failure is the term used to describe the condition.
What Can I Expect If I Have Sudden Cardiac Arrest
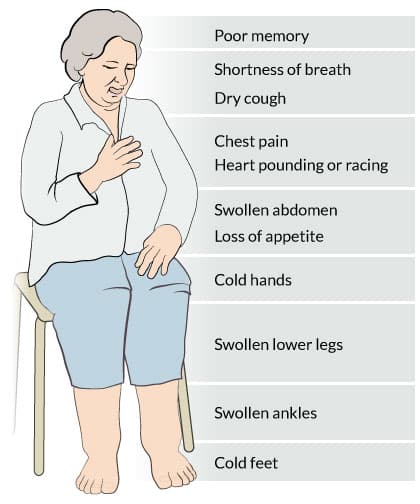
Most people who have a sudden cardiac arrest outside of a hospital dont survive. This is usually because they dont get help in time. Most cases of sudden cardiac arrest that dont happen in a hospital take place at home. Every minute that you dont receive help is another minute your brain is without the oxygen it needs.
People who survive sudden cardiac arrest have a varied outlook, depending on how fast they received medical treatment. They usually need help regaining skills they had before their sudden cardiac arrest. This happens because you can have brain damage if too many minutes pass without oxygen reaching your brain. Other organs may also be affected, including resulting in kidney failure, liver failure and long-term heart disease.
Don’t Miss: Congestive Heart Failure Early Signs
Management Of Heart Failure
“Once heart failure has been diagnosed, the goal of treatment is to improve symptoms and signs and avoid or reduce hospital admissions. In the majority of patients with symptomatic heart failure,
- a diuretic is used first-line to reduce fluid overload.
- An ACE inhibitor and beta-blocker are then added,
- followed by spironolactone if the patient is still symptomatic.
- An angiotensin-II receptor blocker, digoxin and anticoagulants can be added as appropriate.
- Surgical interventions may be considered for some patients.”
How Is Pulmonary Hypertension Diagnosed
Your provider will perform a physical exam and run tests to reach a pulmonary hypertension diagnosis.
First, youll have a physical exam to check for signs of pulmonary hypertension as well as other heart or lung issues. During this exam, your provider will:
- Ask you questions about your health and your medical history.
- Ask about your symptoms.
- Check the size of the veins in your neck. Bulging neck veins could be a sign of right-sided heart failure.
- Check the size of your liver by feeling the upper right area of your tummy.
- Listen to your heart and lungs with a stethoscope.
- Look at your belly, ankles and legs for edema.
- Measure your blood pressure.
- Measure the oxygen level in your blood using a pulse oximeter.
Pulmonary hypertension can be difficult to diagnose since many signs of PH are similar to those of other conditions. So, after your physical exam, your provider may run some tests to get more information.
Your provider may also refer you to a pulmonologist or cardiologist.
Also Check: What Is Normal Resting Heart Rate By Age
How Is Congestive Heart Failure Diagnosed
Patients will typically have an intake visit with a heart specialist and nurse or physicians assistant. During this visit, the doctor will review the patients prior records and his or her current health status. This allows the doctor to establish a picture of where the patient is along the spectrum, and make a plan for prognosis and treatment.
The process often takes more than one meeting and involves both the patients local cardiologist or referring physician.
What Is The Life Expectancy For People With Pulmonary Hypertension
The life expectancy varies from person to person. It depends how quickly youre diagnosed and what other medical conditions you have. Talk with your provider about what you can expect in your individual situation.
Pulmonary hypertension is a progressive disease. That means it gets worse over time. It progresses more quickly in some people than in others. Treatment can improve your chances of surviving pulmonary hypertension for many years.
You May Like: End Stage Heart Failure Symptoms Death
Signs Of Heart Failure Progression
As heart failure progresses, your symptoms will most likely worsen. You may also begin to experience:
- Shortness of breath: Fluid may leak into the lungs, causing breathlessness, especially during physical activity. As your condition progresses, this symptom may also occur while youre at rest.
- Irregular heartbeat: A weakened heart may develop arrhythmia or an irregular heartbeat. You may feel like your heart is racing, fluttering or skipping a beat.
- Coughing: Because heart failure may cause fluid to build up in your lungs, you may experience persistent coughing. Some people cough up white mucus tinged with blood.
- Confusion or memory loss: A lack of nutrients in your blood can cause confusion and disorientation.
- Abdominal pain: Restricted blood flow to your digestive system makes it challenging for your body to process food. You may lose your appetite or feel sick to your stomach. Fluid retention may also cause swelling and pain in this area.
