Physical Exam For Heart Failure
First, your doctor will want to know if you:
- Have other conditions such as diabetes, kidney disease, angina, high blood pressure, or other heart problems
- Drink alcohol, and how much
- Take medications, and which ones
Your doctor will also do a physical exam. They’ll look for signs of heart failure as well as other illnesses that may have weakened your heart.
During your visit, your doctor will:
- Listen to your heart
- Check your blood pressure
Theyâll also look at your appearance while you sit, do mild activity, and lie flat. People with mild or moderate heart failure may appear comfortable at rest, but when active, they often become short of breath. Those with heart failure may be uncomfortable if they lie flat for a few minutes.
Your doctor may check for fluid in your lungs with a stethoscope. People with heart failure may also have neck veins that are larger than normal, swelling of the legs or abdomen, or an enlarged liver.
What Did This Study Do
The REFER study included 304 adults aged over 55 years who were recruited to the study when they presented with suspected heart failure at 28 UK GP practices. The final number of participants was lower than planned, but is still larger than previous, similar studies.
Clinical assessment, blood tests, electrocardiograph and echocardiograms were carried out within seven days. Three heart specialists independently assessed each case. They were given patient data in three instalments: clinical assessment, ECG and echocardiogram results addition of clinical decision rule data and finally blood levels of NTproBNP .
The accuracy of heart failure diagnosis using the decision rule, NTproBNP level , or combination of the two was compared against a reference standard. In this case, the standard was a diagnosis confirmed by consensus of three experts using agreed standard definitions.
Diagnosing Cardiomyopathy & Heart Failure
NYU Langone specialists are experts at identifying cardiomyopathy and heart failure, a type of heart disease in which the heart fails to pump enough blood to the body. It can be inherited, or it can be caused by another condition, as well as by certain medications or lifestyle habits.
When cardiomyopathy weakens the hearts ability to pump blood, heart failure may occur. Right-sided heart failure happens when the heart cant pump enough blood to the lungs. Left-sided heart failure occurs when the heart cant pump enough blood to the rest of the body. Most of the time, the condition affects both sides of the heart.
Don’t Miss: Does Bayer Prevent Heart Attacks
What Is Heart Failure
Heart failure, or congestive heart failure, is a long-term condition that gets worse over time. Although the name sounds like your heart has stopped working, heart failure means your heart isnt able to pump blood as well as it should. When your heart has less pumping power, that can damage your organs and fluid can collect in your lungs.
Carrus Health Advanced Radiology Department

At Carrus Health, we provide the imaging tests you need for a clinical diagnosis of congestive heart failure. We currently offer CT Scans, X-rays, and ultrasounds to diagnose your condition. Our radiology facility in Sherman, Texas is spacious, clean, and comfortable.
To schedule an appointment, please call Carrus Health at 870-2600. Our friendly staff looks forward to assisting you.
Recommended Reading: Congestive Heart Failure In Cats
Coronary Catheterization And Angiogram
In coronary catheterization and angiogram, your doctor uses X-ray images taken in real time to create cross-sectional images of the heart. This enables the doctor to determine how well the heart is pumping blood to the rest of the body and to view any blockages in the blood vessels.
After you are given local anesthesia and a sedative, your doctor guides a small, hollow tube called a catheter into a puncture in a vein in the arm or groin. He or she advances it through the aorta, the bodys largest artery, to the heart.
An X-ray instrument called a fluoroscope is inserted into the catheter and led to the heart to provide live X-rays of the hearts chambers. Your doctor also injects a contrast agent into the catheter to highlight any blockages.
Diagnostic Tests And Procedures
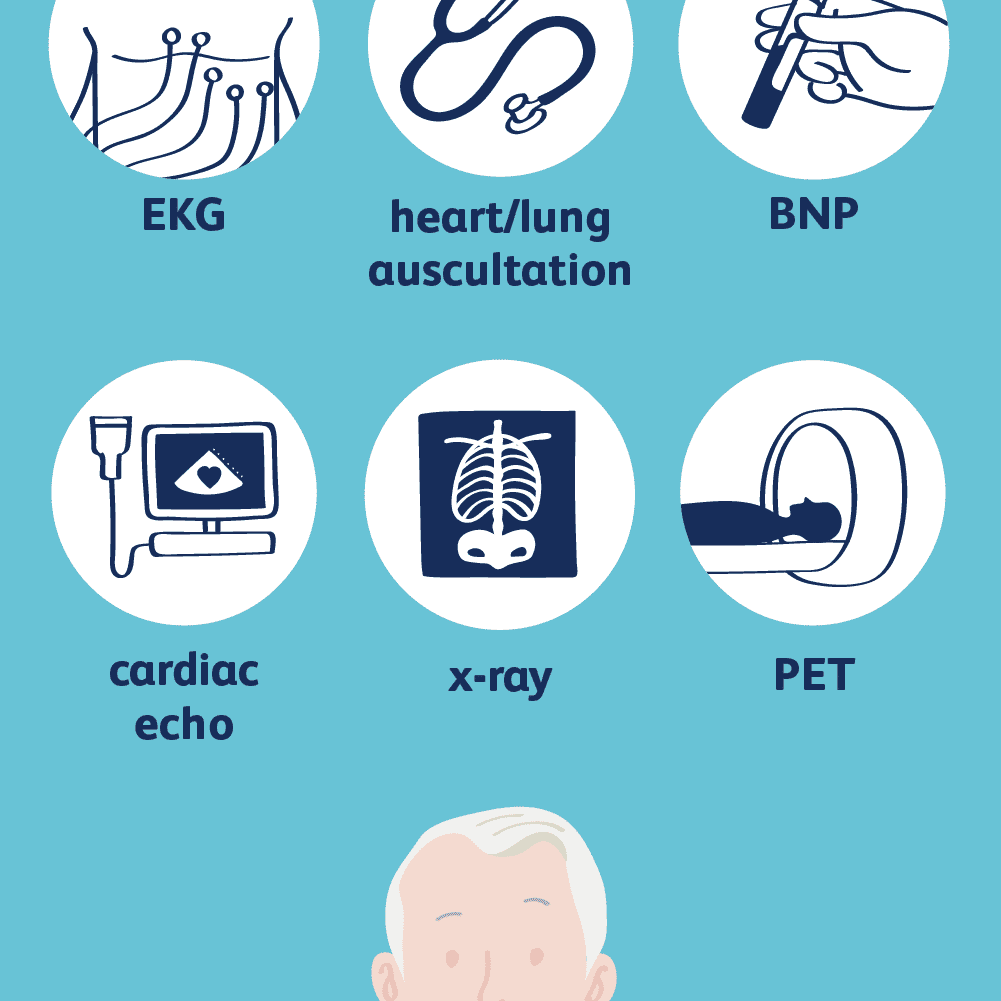
This animation discusses some of the tests used to diagnose heart failure. These tests may include an electrocardiogram to look at your hearts electrical activity, an echocardiogram to measure how well your heart is working and look at the structure, and a chest X-ray to see if your heart is enlarged or there is fluid in your lungs. Other tests may include blood tests and an exercise, or stress test. .
Also Check: Hair Loss After Heart Surgery
Center For Advanced Heart Failure/cardiomyopathy At Brigham And Womens Hospital
The Center for Advanced Heart Failure/Cardiomyopathy, an integral part of the Heart & Vascular Center at Brigham and Womens Hospital , brings together heart failure experts, including cardiologists, interventional cardiologists, cardiac surgeons, cardiovascular imaging specialists, congenital heart disease specialists, and many others, to care for patients as one team. Together, the team tailors therapies to each patients needs, offering the latest medical, interventional, and surgical approaches to congestive heart failure treatment.
Tests For Heart Failure
Tests you may have to diagnose heart failure include:
- blood tests to check whether there’s anything in your blood that might indicate heart failure or another illness
- an electrocardiogram this records the electrical activity of your heart to check for problems
- an echocardiogram a type of ultrasound scan where sound waves are used to examine your heart
- breathing tests you may be asked to blow into a tube to check whether a lung problem is contributing to your breathlessness common tests include spirometry and a peak flow test
- a chest X-ray to check whether your heart’s bigger than it should be, whether there’s fluid in your lungs , or whether a lung condition could be causing your symptoms
You can read more about tests for heart conditions on the British Heart Foundation website.
Don’t Miss: What Can Be Done For Congestive Heart Failure
What Are The Complications Of Heart Failure
Some of the complications from heart failure include:
- Irregular heartbeat.
- History of taking drugs that can damage your heart muscle, such as some cancer drugs.
Stage B
Stage B is considered pre-heart failure. It means your healthcare provider has given you a diagnosis of systolic left ventricular dysfunction but youve never had symptoms of heart failure. Most people with Stage B heart failure have an echocardiogram that shows an ejection fraction of 40% or less. This category includes people who have heart failure and reduced EF due to any cause.
Stage C
People with Stage C heart failure have a heart failure diagnosis and currently have or previously had signs and symptoms of the condition.
There are many possible symptoms of heart failure. The most common are:
- Shortness of breath.
- Need to urinate while resting at night.
- Rapid or irregular heartbeats .
- A dry, hacking cough.
- A full or hard stomach, loss of appetite or upset stomach .
There may be times that your symptoms are mild or you may not have any symptoms at all. This doesn’t mean you no longer have heart failure. Symptoms of heart failure can range from mild to severe and may come and go.
Unfortunately, heart failure usually gets worse over time. As it worsens, you may have more or different signs or symptoms.Its important to let your doctor know if you have new symptoms or if your symptoms get worse.
How Would Mrs S Know If The Medications Are Effective
Mrs. S may observe reduced swelling on her feet, ankles, hands, weight loss, and reduced pulmonary edema. Her breathing will become easier she may not require 2 or more pillows to sleep at night and she may be able to lie flat. She may observe increased urinary output and frequency and reduced wet cough after taking Lasix. Mrs. S may notice decreased symptoms of congestive heart failure, lowered blood pressure, less fatigued, and reduced heart rate within months of taking captopril.
As you continue, pro-essays.com has the top and most qualified writers to help with any of your assignments. All you need to do is place an order with us.
Also Check: Open Heart Surgery Recovery Stories
Congestive Heart Failure Drugs
There are several medications that can be used to treat CHF, including ACE inhibitors, beta-blockers, and more.
ACE inhibitors
Angiotensin-converting enzyme inhibitors open up narrowed blood vessels to improve blood flow. Vasodilators are another option if you cant tolerate ACE inhibitors.
You may be prescribed one of the following:
voluntary recall of 5 lots of the drug Accupril due to the presence of nitrosamine. Nitrosamine, a known carcinogen with the potential to cause cancer, was found to exist in the drug at levels greater than the Acceptable Daily Intake as determined by the FDA. This recall is specific only to a handful of lot numbers and does not affect all Accupril tablets made by Pfizer. If you take Accupril tablets, talk with your pharmacist or doctor and they will help you determine if your medication has been impacted by the recall.
ACE inhibitors shouldnt be taken with the following medications without consulting a doctor, because they may cause an adverse reaction:
- Potassium-sparing diuretics and potassium supplements. These diuretics can cause potassium buildup in the blood, which may lead to abnormal heart rhythms. Examples include: riamterene , eplerenone , and spironolactone .
- Nonsteroidal anti-inflammatory drugs .NSAIDs such as ibuprofen, aspirin, and naproxen, can cause sodium and water retention. This may reduce the ACE inhibitors effect on your blood pressure.
Beta-blockers
This may be achieved with:
Diuretics
Your doctor may recommend:
Bnp: An Important Cardiac Test

B-type natriuretic peptide belongs to a family of protein hormones called natriuretic peptides. These natriuretic peptides have an important role in regulating the circulation. They act on blood vessels, causing them to dilate, or widen. They also work on the kidneys, causing them to excrete more salt and water. In addition, the natriuretic peptides reduce the production of various hormones that narrow blood vessels, boost the heart rate, or affect fluid retention examples include adrenaline, angiotensin, and aldosterone.
The net effect of natriuretic peptides is to promote urine excretion, relax blood vessels, lower blood pressure, and reduce the heart’s workload. They are part of the body’s natural defense mechanisms designed to protect the heart from stress. And they surge into action when they are needed most, when the heart itself is under siege.
Read Also: Treatment For Congestive Heart Failure In Dogs
Iobenguane Scanning For Cardiac Risk Evaluation
The scintigraphic imaging agent iobenguane I 123 injection is used for the evaluation of myocardial sympathetic innervation in patients with New York Heart Association class 2-3 heart failure with an LVEF of 35% or less. This radionuclide tracer, which functions molecularly as a norepinephrine analogue, can show relative levels of norepinephrine uptake in the cardiac sympathetic nervous system and contribute to risk stratification in heart failure patients. Improved reuptake of norepinephrine is associated with a better prognosis.
Treatment For Heart Failure
Your heart failure treatment plan will depend on how far your condition has advanced. However, lifestyle changes, such as losing weight, exercising regularly and maintaining a healthy diet will always be central components of effectively managing heart failure. If needed, your cardiologist may also add dietary counseling and medication to your treatment plan. No matter the severity, we will always primarily address the underlying causes of your condition and provide appropriate treatments and procedures.
Cardiac surgery
If you’re experiencing advanced heart failure, you may need surgical treatment. Our highly trained surgeons favor minimally invasive procedures and use a variety of techniques, including regulating heart rhythms via implanting devices such as implantable cardiac defibrillators . Some of the surgical procedures we offer include:
- Cardiac resynchronization therapy
- Coronary artery bypass graft
- Heart valve repair or replacement
- ICD implantation
- Pacemaker implantation
For some, clinical trials may also be useful. Talk to your doctor about the clinical trials in our network of hospitals to find out if they may be right for you.
Recommended Reading: How Much Does Heart Surgery Cost
Natriuretic Peptides: Bnp Or Nt
- Plasma concentrations of NPs are recommended as initial diagnostic tests in patients with symptoms suggestive of HF to rule out the diagnosis.
- Elevated concentrations support a diagnosis of HF.
- Other causes of an elevated NP include atrial fibrillation, increasing age, and acute or chronic kidney disease.
- NP concentrations may be low in obesepatients.
- The upper limits of normal in the non-acute setting are 35 pg/mL for BNP, and 125 pg/mL for NT-proBNP.
The CoDE-HF decision support tool may help diagnose heart failure. The CoDE-HF interprets the N-terminal pro-B-type natriuretic peptide in various settings including obesity.
| Causes of elevated concentrations of natriuretic peptides |
- BNP or its amino-terminal cleavage equivalent is generated by cardiomyocytes in the context of numerous triggers, most notably myocardial stretch.
- BNP levels may be useful in the initial establishment of the diagnosis of heart failure in the patient with dyspnea of unclear etiology. In a meta-analysis, BNP was superior N-terminal pro-BNP and was associated with a sensitivity of 85% and specificity of 84% in the diagnosis of heart failure in the primary care setting.
- These biomarkers have been studied for the detection of elevated cardiac pressures., low ejection fraction, or both.
- Clinical practice guidelines suggest their measurement is helpful for diagnosis or ruling out heart failure especially in the acute settings.
How Long Can An 85 Year Old Live With Heart Failure
In a recent study, it was reported that patients hospitalized with moderate systolic heart failure faced a median expected survival time of 2.4 years if they were aged 71 to 80 years and 1.4 years if they were aged 80 years or more. In patients with more advanced systolic dysfunction, life expectancy was even shorter.
Don’t Miss: What Is The Survival Rate Of Open Heart Surgery
Patient Teaching Regarding Captopril
Ensuring that the patient receives the best care possible, it is important that nurses provide them with information that would minimize the possibility of adverse effects occurring and facilitate the healing process. Patients with renal insufficiency or taking potassium sparing diuretics should refrain from taking this drug as it may cause hyperkalemia . Patient should be informed that the therapeutic effect of the drug may take several weeks to lower the blood pressure. The nurse will teach the patient when to report to them if they experience swelling in their face, lips and/or tongue. Additionally, the patient should be careful when rising from sitting/fowlers position. Lastly, the nurse should inform the patient that skipping or stopping the intake of their medication would cause blood pressure increases after stopping the administration of the drug also known as rebound hypertension.
Bnp Measurement Not Indicated With Nesiritide Therapy
Nesiritide is a synthetic BNP analogue therefore, the measurement of BNP is not indicated in patients who are receiving nesiritide. If BNP is used as a diagnostic marker to rule in heart failure, the level must be determined before nesiritide therapy is started.
In a study by Miller et al, levels of NT-proBNP and BNP decreased in patients with advanced heart failure after therapy with nesiritide, but the majority of the patients did not have biochemically significant decreases in these markers even with a clinical response. The investigators were unable to give a definitive reason for their results, and they indicated that nesiritide therapy should not be guided by the use of levels of both markers. Fitzgerald et al also found decreased levels of both natriuretic peptides following nesiritide therapy in patients with decompensated heart failure.
For more information, see the Medscape Drugs & Diseases article Natriuretic Peptides in Congestive Heart Failure.
Recommended Reading: Prevention For Heart Attack
Congestive Heart Failure Pathophysiology
Definition: According to Mayo Clinic Heart failure, sometimes known as congestive heart failure, occurs when your heart muscle doesnât pump blood as well as it should. Certain conditions, such as narrowed arteries in your heart or high blood pressure, gradually leave your heart too weak or stiff to fill and pump efficiently. Not all conditions that lead to heart failure can be reversed, but treatments can improve the signs and symptoms of heart failure and help you live longer. Lifestyle changes such as exercising, reducing salt in your diet, managing stress and losing weight can improve your quality of life. One way to prevent heart failure is to control conditions that cause heart failure, such as coronary artery disease, high blood pressure, diabetes or obesity.
Manifestations : Shortness of breath when you exert yourself or when you lie down Fatigue and weakness Swelling in your legs, ankles and feet Rapid or irregular heartbeat Reduced ability to exercise Persistent cough or wheezing with white or pink blood-tinged phlegm Increased need to urinate at night Swelling of your abdomen Sudden weight gain from fluid retention Lack of appetite and nausea Difficulty concentrating or decreased alertness Sudden, severe shortness of breath and coughing up pink, foamy mucus Chest pain if your heart failure is caused by a heart attack
Stages Of Heart Failure
When you’re diagnosed with heart failure, your doctor will usually be able to tell you what stage it is.
The stage describes how severe your heart failure is.
It’s usually given as a class from 1 to 4, with 1 being the least severe and 4 being the most severe:
- class 1 you don’t have any symptoms during normal physical activity
- class 2 you’re comfortable at rest, but normal physical activity triggers symptoms
- class 3 you’re comfortable at rest, but minor physical activity triggers symptoms
- class 4 you’re unable to carry out any physical activity without discomfort and may have symptoms even when resting
Knowing the stage of your heart failure will help your doctors decide which treatments they think are best for you.
Page last reviewed: 19 May 2022 Next review due: 19 May 2025
Recommended Reading: Why Did Mr Stone Develop Heart Failure
