What Are The Types Of Left
There are two types of left-sided heart failure: systolic heart failure and diastolic heart failure.
- Systolic heart failure: Also called reduced ejection fraction , it happens when the left ventricle cant contract forcefully. Less oxygen-rich blood gets pumped out to the body when you have systolic heart failure. Instead, it flows back into the organs, leading to fluid build-up in the lungs as well as swelling in certain parts of the body.
- Diastolic heart failure: Also referred to as preserved ejection fraction , this is when the heart muscle actually contracts normally but the ventricles are stiff or thick and dont relax, so the amount of blood pumped out to the body is reduced.
Ejection fraction is the term thats used to measure the amount of blood that pumps through the ventricles. A hearts normal ejection fraction is between 50 and 70 percent. A measurement of 40 percent or under is usually a sign of heart failure. Sometimes, people can have a normal ejection fraction reading and still have heart failure. An echocardiogram is the most common test used for measuring EF.
Diagnosis Of Heart Failure Of Acute Onset
|
Data from Ponikowski P, Voors AA, Anker SD, et al: 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology Developed with the special contribution of the Heart Failure Association of the ESC. European Heart Journal 37:2129-2200, 2016. doi: 10.1093/eurheartj/ehw128 |
Causes Of Heart Failure
Heart failure is often the result of a number of problems affecting the heart at the same time.
Conditions that can lead to heart failure include:
- coronary heart disease where the arteries that supply blood to the heart become clogged up with fatty substances , which may cause angina or a heart attack
- high blood pressure this can put extra strain on the heart, which over time can lead to heart failure
- conditions affecting the heart muscle
- heart rhythm problems , such as atrial fibrillation
- damage or other problems with the heart valves
- congenital heart disease birth defects that affect the normal workings of the heart
Sometimes obesity, anaemia, drinking too much alcohol, an overactive thyroid or high pressure in the lungs can also lead to heart failure.
Read Also: Can Kardia Detect Heart Attack
Pathophysiology Of Heart Failure
Kardiologie, Nephrologie/Hypertonie, Pneumologie, Internistische Intensivmedizin, Medizinische Klinik II, Klinikum Weiden, Weiden, Germany
Correspondence to:
Keywords: Heart failure pathophysiology HFpEF HFrEF treatment of heart failure
Submitted Feb 28, 2020. Accepted for publication May 28, 2020.
doi: 10.21037/cdt-20-302
Symptoms Of Heart Failure In Children
The following are the most common symptoms of heart failure. However, each child may experience symptoms differently. Symptoms may include:
-
Visible swelling of the legs, ankles, eyelids, face, and abdomen
-
Abnormally fast breathing
-
Falling asleep when feeding or becoming too tired to eat
-
Lack of appetite
-
Weight gain over a short period of time, even when the appetite is poor, typically due to fluid retention
-
Cough and congestion in the lungs
-
Sweating while feeding, playing, or exercising
-
Breathing difficulty with activity, especially while feeding, walking, or climbing stairs
-
Loss of muscle mass
-
Failure to gain weight
-
Change in skin temperature and color
The severity of the condition and symptoms depends on how much of the heart’s pumping capacity has been affected.
The symptoms of heart failure may resemble other conditions or medical problems. Always consult your child’s healthcare provider for a diagnosis.
Don’t Miss: How Does Exercise Affect Your Heart Rate
Treatments For Heart Failure
Treatment for heart failure usually aims to control the symptoms for as long as possible and slow down the progression of the condition.
How you’re treated will depend on what is causing your heart failure.
Common treatments include:
- lifestyle changes including eating a healthy diet, exercising regularly and stopping smoking
- medicine a range of medicines can help many people need to take 2 or 3 different types
- devices implanted in your chest these can help control your heart rhythm
- surgery such as a or a heart transplant
Treatment will usually be needed for life.
A cure may be possible when heart failure has a treatable cause. For example, if your heart valves are damaged, replacing or repairing them may cure the condition.
Anemia And Iron Deficiency
Anemia is common among patients with chronic heart failure and is frequently multifactorial. Anemia is associated with worse symptoms and outcomes in HF and so reversible causes should be sought and treated. Iron deficiency Iron Deficiency Anemia Iron deficiency is the most common cause of anemia and usually results from blood loss malabsorption, such as with celiac disease, is a much less common cause. Symptoms are usually nonspecific… read more is among the most common causes of anemia in HF, and iron replacement therapy should be considered once treatable causes such as blood loss have been excluded. Oral iron replacement is often less effective due to poor absorption and other reasons, thus intravenous iron replacement is preferred.
Also Check: What To Do In Case Of A Heart Attack
Outlook For Heart Failure
Heart failure is a serious long-term condition that will usually continue to get slowly worse over time.
It can severely limit the activities you’re able to do and is often eventually fatal.
But it’s very difficult to tell how the condition will progress on an individual basis.
It’s very unpredictable. Lots of people remain stable for many years, while in some cases it may get worse quickly.
Whats The Outlook For People With Right
For many people, the right combination of therapies and lifestyle changes can slow or stop the disease and improve symptoms. They can lead full, active lives.
About 1 in 10 American adults who live with heart failure have advanced heart failure. That means treatments arent working, and symptoms are getting worse. You may feel symptoms, such as shortness of breath, even when youre sitting. If you have advanced heart failure, talk with your care team about important care decisions and next steps.
You May Like: Is 85 Heart Rate Normal
Treatment Options For People With Acute Heart Failure
There is no cure for heart failure, but treatment can help improve your quality of life. Acute heart failure can have lasting effects on your body. Because of this, treatment is centered on managing symptoms and preventing future heart failure.
If you experience acute heart failure, youll likely stay in the hospital until youre in stable condition. During this time, you may need oxygen therapy. You might also need supplemental oxygen after you leave the hospital.
The cause of your acute heart failure will determine your treatment plan. In some cases, acute heart failure can be caused by undiagnosed chronic heart failure. Treatment for acute heart failure and chronic heart failure is often the same.
Treatment options for acute heart failure include medications, medical devices, and surgery.
Changes In Function And Expression Of Ion Channels And Contractile Proteins
Various processes involved in the conversion of an electrical stimulus to a mechanical response i.e., excitation contraction coupling are altered in human heart failure part of these alterations are expression and function of the ion channels or transporters , contractile proteins , intracellular calcium transport processes . Both, the calcium induced calcium release and the intracellular calcium handling is affected in heart failure leading to reduced contractility and prolonged relaxation . In consequence, in human heart failure the frequency-induced force generation is reduced or even absent i.e., negative force-frequency-relationship the intracellular free calcium concentration is enhanced and the Ca2+ sensitivity of the contractile proteins is increased . Following reduced ß-adrenoceptor response in heart failure phosphorylation of several Ca2+-handling proteins is reduced and Ca2+ affinity of contractile proteins is increased. Both mechanisms impair contraction and relaxation further. In addition, Na efflux via the NCX is affected as well leading to increased intracellular Na and reduced K. In consequence, the resting membrane potential is shifted to depolarization which acts proarrhythmogenic. The altered intracellular Ca2+ handling in human heart failure affect also mitochondria energy production and in consequence further deteriorate myocardial function .
Also Check: How To Get Heart Rate Down Fast
Tests For Acute Heart Failure
Your doctor will assess your medical history and perform a physical exam. Theyll listen to your heart and lungs with a stethoscope to detect any congestion or abnormal heart rhythms. Your doctor may also check for fluid buildup in your abdomen, legs, and the veins in your neck.
In addition, your doctor might request tests such as:
- Blood tests. These could include a BNP test, which measures a hormone related to heart failure.
- Electrocardiogram . During this test, your doctor will attach electrodes to your skin and record your hearts electrical activity.
- Stress test. This test measures your heart activity during physical exercise. Its not typically recommended if you already have signs and symptoms of heart failure.
Imaging tests that a doctor can use to help diagnose heart failure include:
- Chest X-ray. This test allows your doctor to better examine your heart and lungs.
- Echocardiogram. This test uses sound waves to form a live, moving image of your heart so your doctor can see which areas of your heart are affected.
- Angiogram. If your doctor thinks you may have a blocked artery, they will insert a thin tube into your groin or arm and into your coronary arteries. After injecting dye through a catheter, your doctor can see an image of your arteries.
When needed, other imaging tests can be used to look for underlying causes of heart failure:
Together, your physical exam and test results can help your doctor learn about the health of your heart.
Discuss An Exercise Plan And Get Started
Your doctor may advise you to treat exercise as part of your overall plan to manage heart failure. Talk to your doctor about the right level of exercise for you, and how you can get started. Depending on your condition, they may recommend a cardiac rehabilitation program.
For many people, a great exercise for getting started is simply walking. You can build up gradually, walking for longer periods of time and at a quicker pace as your fitness level improves. If youre finding moderate activity difficult, let your doctor know and see what they suggest.
Surprisingly, some programs might use high intensity interval training . This form of exercise alternates very intense cardio exercise with short breaks.
You May Like: Frequently, What Is The Earliest Symptom Of Left-sided Heart Failure
Left Ventricular Assist Device
A left ventricular assist device is a mechanical pump operated by a battery that’s implanted via open-heart surgery. There are different types, but they all have four parts, including:
Imaging And Other Tests
Other tests provide pictures of the heart and surrounding structures or show how well the heart is working:
- Electrocardiogram : An electrocardiogram test uses small sensors to measure heart rate , rhythm and electrical impulses.
- Chest X-ray: A chest X-ray is a picture of your lungs, heart and surrounding structures. It can show whether there is fluid in your lungs from heart failure, or if your heart muscle is enlarged.
- Echocardiogram : Echocardiography uses sound waves to create images of your heart. It can show how thick the heart muscle has become, as well as measure ejection fraction.
- MRI: MRI is an advanced imaging test that takes pictures of the heart and surrounding structures. It helps determine your heart function and size and whether there are any changes in the heart muscle. A cardiac MRI may help your doctors identify causes of heart failure.
Also Check: How Is Open Heart Surgery Performed
Manage Your Condition With An App
When you have heart failure, managing your condition and health can feel like a lot of work. A smartphone app can help you keep track of your medications, appointments, symptoms, and your state of mind. The Heart Failure Society of America has a free app called Heart Failure Storylines, and there are many others too.
A 2018 study reviewed 18 previous reports on mobile health apps for heart failure. The study authors noted a general trend that suggested the apps made a difference to people who used them. They also reported that the apps were cost-effective and promoted people being engaged in their own care.
Making heart-healthy food choices is an important aspect of managing heart failure. Your doctor may recommend that you see a dietitian to help you find a meal plan that works for you.
Two widely recommended diets for people living with heart failure are the
2017 review indicated that both diets, and especially the DASH plan, might be helpful for people with heart failure. The authors recommended further research on the Mediterranean diet, and noted that the DASH plan may provide benefits such as improved cardiac function.
If you dont want to stick to a specific diet, another option is to focus on making heart-healthy choices on a regular basis. The American Heart Association advises people to follow a couple key principles.
In general, youll want to focus on:
Heart Failure With Preserved Ejection Fraction Treatment
Diuretics are a mainstay of HFpEF treatment. For these medications to be helpful, however, you need to also make changes to your diet and overall lifestyle.
If you have HFpEF, your doctor will likely suggest you follow a treatment regimen that includes a combination of:
- Diet and lifestyle changes
- For some patients, a device to protect the heart from abnormal rhythms
Diet and Lifestyle Changes
If you have heart failure, the following lifestyle changes may help you manage your symptoms:
- Regular low-intensity aerobic exercise to strengthen the heart
- Cutting back on salt
- Limiting your alcohol consumption
- Quitting smoking
Reducing your salt intake is especially important. Too much salt in your diet can cause fluid retention. This will counteract the drugs that help relieve fluid accumulation.
The effectiveness of medication in the treatment of diastolic heart failure is inconclusive. Therefore, the best way to manage HFpEF is to treat its underlying cause, such as hypertension, diabetes, or coronary artery disease.
SGLT2 inhibitor medications are antidiabetic drugs that may be used to treat HFpEF in people with or without diabetes. In people with heart failure, taking this medication can help prevent heart failure episodes. Your doctor can determine whether you are able to use an SGLT2 inhibitor.
Management by Stage
The American College of Cardiology and the American Heart Association recommend that cardiologists manage heart failure by stage.
Read Also: What Is Heart Valve Disease
Coronary Angiography And Cardiac Catheterization
A coronary angiography and cardiac catheterization are two diagnostic procedures often used to identify problems with the heart. It is a surgical procedure that involves a small incision made into the groin, arm, or neck and into a large blood vessel. A catheter is fed through the blood vessel, via the incision, to the heart.
The coronary angiography portion of this procedure involves the administration of a contrast dye . After you are given the contrast dye, the healthcare provider can take X-rays, which allow them to watch where the dye goes and observe its flow through the blood vessels and heart. This is helpful in identifying any blockages.
Other things can be done through a cardiac catheterization. Biopsies of tissue can be taken, stents can be placed to open up blockages, and the pressure of blood flow through the heart can be measured.
These tests are invasive procedures and are usually able to be done on a same-day surgery basis. Depending on where your incision is made and what is done during the procedure, you may need to lay flat for a period of time following your cardiac catheterization. You should follow your practitioner’s or nurse’s instructions precisely during your recovery period.
How To Prevent Acute Heart Failure
Some risk factors, such as aging, cant be avoided. The key to preventing heart failure is to reduce the risk factors that you can control.
Many of the lifestyle measures recommended for heart failure recovery can also reduce or eliminate conditions that lead to heart failure. These conditions include high blood pressure and high cholesterol.
If youre at risk for heart failure, you should consider these measures to promote heart health:
- maintain a healthy weight, if overweight or obesity is a concern
- get regular physical activity
Also Check: What Is Ideal Resting Heart Rate
When To Get Medical Advice
See a GP if you experience persistent or gradually worsening symptoms of heart failure.
Call 999 for an ambulance or go to your nearest A& E department as soon as possible if you have sudden or very severe symptoms.
A number of tests can be used to help check how well your heart is working, including blood tests, an ECG and an echocardiogram.
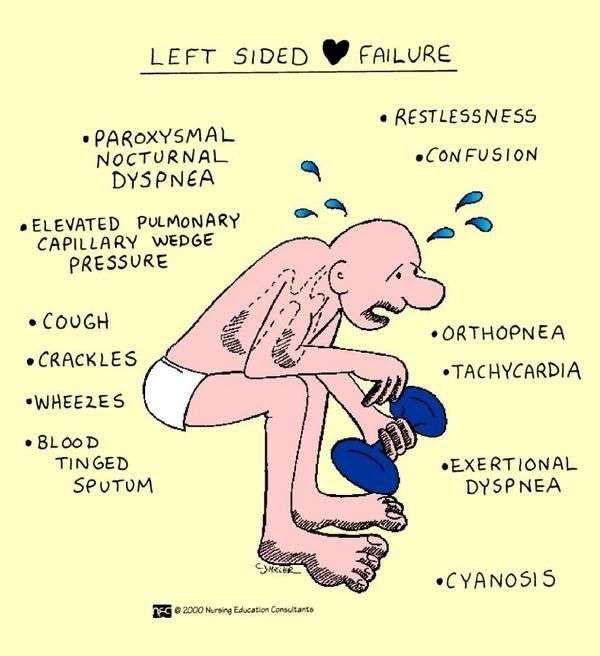
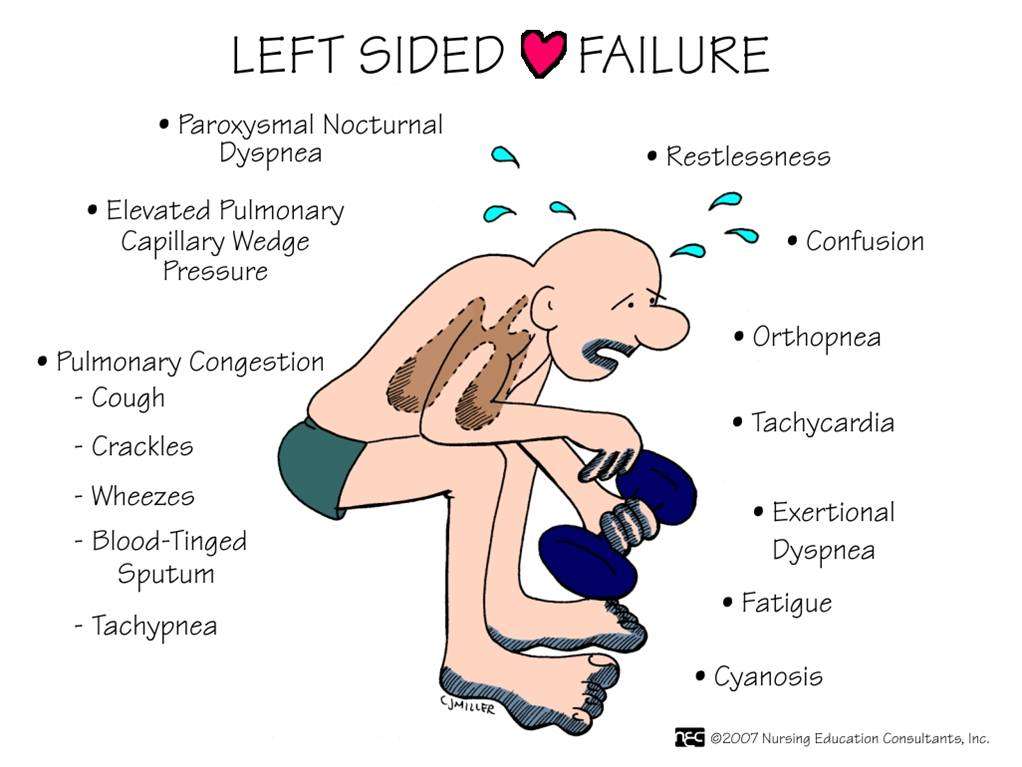
Recognizing Common Signs And Symptoms

Read Also: Heart Rate Sensor
